Machine Learning Confirms Nonlinear Relationship between Severity of Peripheral Arterial Disease, Functional Limitation and Symptom Severity
Abstract
1. Introduction
2. Methods
2.1. Patient Inclusion Criteria
2.2. Strides Protocol
2.3. Data Analysis
3. Results
4. Discussion
4.1. Machine Learning
4.1.1. ML Versus Statistics
4.1.2. ML Ensemble
4.2. Clinical Significance
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| ML | machine learning |
| 6MWT | 6-minute walk test |
| PAD | peripheral arterial disease |
| CLI | critical limb ischemia |
| TBI | toe–brachial index |
| RF | random forest |
| NN | neural network |
| GLM | generalized linear model |
References
- Rozkovec, A.; Papouchado, M.; James, M.A.; Kendrick, A.H.; Clarke, L.M.; Rees, J.R. The relationship of symptoms to performance in paced patients with breathlessness. Eur. Heart J. 1989, 10, 63–69. [Google Scholar] [CrossRef] [PubMed]
- Criqui, M.H.; Fronek, A.; Barrett-Connor, E.; Klauber, M.R.; Gabriel, S.; Goodman, D. The prevalence of peripheral arterial disease in a defined population. Circulation 1985, 71, 510–515. [Google Scholar] [CrossRef] [PubMed]
- Vogt, M.T.; Wolfson, S.K.; Kuller, L.H. Lower extremity arterial disease and the aging process: A review. J. Clin. Epidemiol. 1992, 45, 529–542. [Google Scholar] [CrossRef]
- Cachovan, M. Body weight related treadmill ergometry vs. treadmill classification test for evaluation of intermittent claudication. VASA Suppl. 1992, 35, 162–163. [Google Scholar] [PubMed]
- Cachovan, M.; Rogatti, W.; Woltering, F.; Creutzig, A.; Diehm, C.; Heidrich, H.; Scheffler, P.; Cachovan, M. Randomized reliability study evaluating constant-load and graded-exercise treadmill test for intermittent claudication. Angiology 1999, 50, 193–200. [Google Scholar] [CrossRef] [PubMed]
- Cachovan, M.; Rogatti, W.; Creutzig, A.; Diehm, C.; Heidrich, H.; Scheffler, P.; Woltering, F. Treadmill testing for evaluation of claudication: Comparison of constant-load and graded-exercise tests. Eur. J. Vasc. Endovasc. Surg. 1997, 14, 238–243. [Google Scholar] [CrossRef][Green Version]
- Lipkin, D.P.; Scriven, A.J.; Crake, T.; Poole-Wilson, P.A. Six minute walking test for assessing exercise capacity in chronic heart failure. Br. Med. J. (Clin. Res. Ed.) 1986, 292, 653–655. [Google Scholar] [CrossRef] [PubMed]
- Guyatt, G.H.; Sullivan, M.J.; Thompson, P.J.; Fallen, E.L.; Pugsley, S.O.; Taylor, D.W.; Berman, L.B. The 6-minute walk: A new measure of exercise capacity in patients with chronic heart failure. Can. Med. Assoc. J. 1985, 132, 919–923. [Google Scholar] [PubMed]
- Bittner, V.; Weiner, D.H.; Yusuf, S.; Rogers, W.J.; McIntyre, K.M.; Bangdiwala, S.I.; Kronenberg, M.W.; Kostis, J.B.; Kohn, R.M.; Guillotte, M. Prediction of mortality and morbidity with a 6-minute walk test in patients with left ventricular dysfunction. SOLVD Investigators. JAMA 1993, 270, 1702–1707. [Google Scholar] [CrossRef] [PubMed]
- Langenfeld, H.; Schneider, B.; Grimm, W.; Beer, M.; Knoche, M.; Riegger, G.; Kochsiek, K. The six-minute walk—An adequate exercise test for pacemaker patients? Pacing Clin. Electrophysiol. 1990, 13, 1761–1765. [Google Scholar] [CrossRef] [PubMed]
- Anderson, K.L. The effect of chronic obstructive pulmonary disease on quality of life. Res. Nurs. Health 1995, 18, 547–556. [Google Scholar] [CrossRef] [PubMed]
- Rostagno, C.; Olivo, G.; Comeglio, M.; Boddi, V.; Banchelli, M.; Galanti, G.; Gensini, G.F. Prognostic value of 6-minute walk corridor test in patients with mild to moderate heart failure: Comparison with other methods of functional evaluation. Eur. J. Heart Fail. 2003, 5, 247–252. [Google Scholar] [CrossRef]
- Hirsch, C.H.; Fried, L.P.; Harris, T.; Fitzpatrick, A.; Enright, P.; Schulz, R. Cardiovascular Health Study Research Group Correlates of performance-based measures of muscle function in the elderly: The Cardiovascular Health Study. J. Gerontol. Ser. A Boil. Sci. Med. Sci. 1997, 52, M192–M200. [Google Scholar] [CrossRef]
- Montgomery, P.S.; Gardner, A.W. The clinical utility of a 6MWT in peripheral arterial occlusive disease patients. J. Am. Geriatr. Soc. 1998, 46, 706–711. [Google Scholar] [CrossRef]
- Morgan, M.B.; Crayford, T.; Murrin, B.; Fraser, S.C. Developing the Vascular Quality of Life Questionnaire: A new disease-specific quality of life measure for use in lower limb ischemia. J. Vasc. Surg. 2001, 33, 679–687. [Google Scholar] [CrossRef] [PubMed]
- Wickham, H. Tidy data. J. Stat. Softw. 2014, 59, 1–23. [Google Scholar] [CrossRef]
- Ali, A.S.; Baig, T.; Sadique, M.; Ali, M.; Qamar, A.U. Quantification of Soft Tissue Loss among Patients with Peripheral Arterial Disease. J. Vasc. Ultrasound 2016, 40, 20–23. [Google Scholar] [CrossRef]
- Norgren, L.; Hiatt, W.R.; Dormandy, J.A.; Nehler, M.R.; Harris, K.A.; Fowkes, F.G.R. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). J. Vasc. Surg. 2007, 45, 5–67. [Google Scholar] [CrossRef] [PubMed]
- Mills, J.L. Infrainguinal Bypass. In Vascular Surgery, 6th ed.; Rutherford, R.B., Ed.; Elsevier Saunders: New York, NY, USA, 2005; pp. 1154–1174. [Google Scholar]
- Gerhard-Herman, M.D.; Gornik, H.L.; Barrett, C.; Barshes, N.R.; Corriere, M.A.; Drachman, D.E.; Fleisher, L.A.; Fowkes, F.G.R.; Hamburg, N.M.; Kinlay, S.; et al. 2016 AHA/ACC Guideline on the Management of Patients With Lower Extremity Peripheral Artery Disease. J. Am. Coll. Cardiol. 2017, 69, e71–e126. [Google Scholar] [CrossRef] [PubMed]
- Allison, M.A.; Ho, E.; Denenberg, J.O.; Langer, R.D.; Newman, A.B.; Fabsitz, R.R.; Criqui, M.H. Ethnic-Specific Prevalence of Peripheral Arterial Disease in the United States. Am. J. Prev. Med. 2007, 32, 328–333. [Google Scholar] [CrossRef] [PubMed]
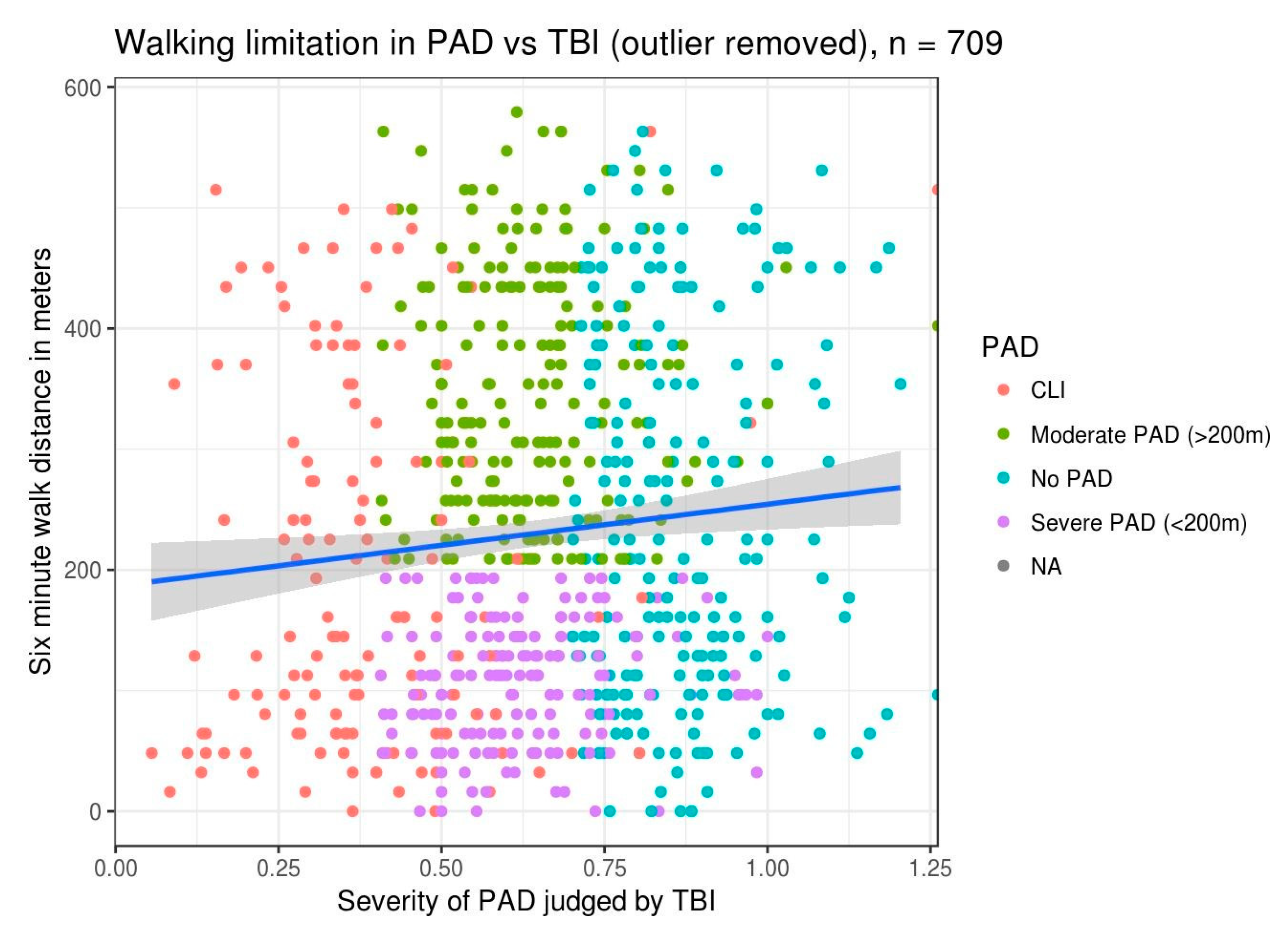


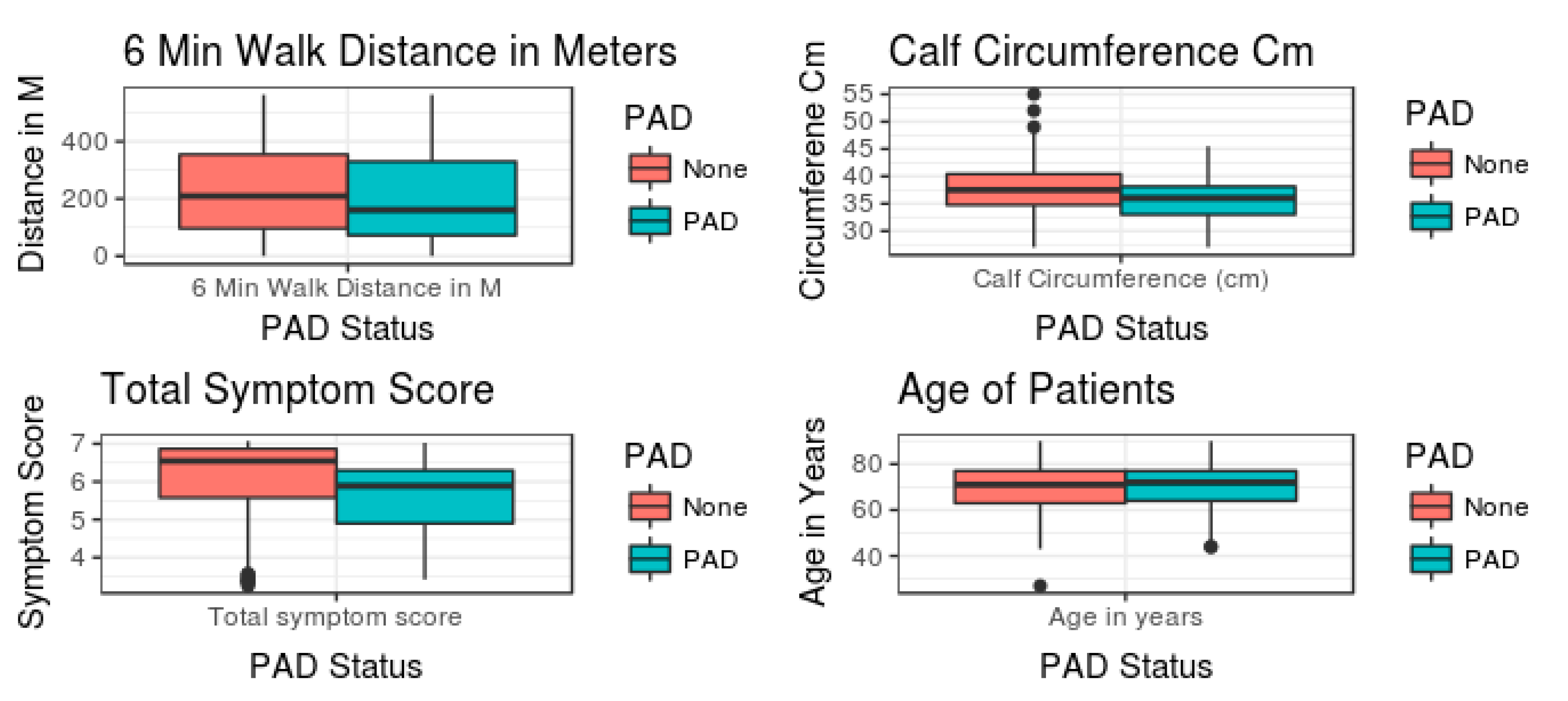

| Symptom Score (x) Categories with 6MWT | ||||
|---|---|---|---|---|
| <4 | <5 | <6 | 6–7 | |
| Sensitivity | 6.89% | 11.3% | 26.0% | 28.4% |
| Specificity | 90.5% | 96.6% | 91.6% | 63.6% |
| Positive Predictive Value (PPV) | 32.0% | 68.4% | 66.6% | 33.6% |
| Negative Predictive Value (NPV) | 60.0% | 62.9% | 65.8% | 57.8% |
| Statistics (Data Modeling) | Machine Learning (Algorithmic) | |
|---|---|---|
| Data Structure | Response variables = function (predictor variables, random noise, parameters) | Exact relationship between response variables and predictor variables is unknown |
| Model Validation | Uses goodness of fit and/or examines the residuals | Use predictive accuracy |
| Limitations | Mathematical model emulates nature’s model | A good predictive model may use features derived from variables thus a ‘black box’ |
| Machine Learning Model | ROC AUCs |
|---|---|
| Random forest 1 (rf1) | 0.69 |
| Random forest 2 (rf2) | 0.63 |
| Neural network (nn) | 0.63 |
| Generalized linear model (glm) | 0.68 |
| Recursive partitioning (rpart) | 0.64 |
| Ensemble = rf1 (1.30), rf2 (−1.70), nn (0.09), glm (−0.13), rpart (−0.70) | 0.687~0.69 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Qutrio Baloch, Z.; Raza, S.A.; Pathak, R.; Marone, L.; Ali, A. Machine Learning Confirms Nonlinear Relationship between Severity of Peripheral Arterial Disease, Functional Limitation and Symptom Severity. Diagnostics 2020, 10, 515. https://doi.org/10.3390/diagnostics10080515
Qutrio Baloch Z, Raza SA, Pathak R, Marone L, Ali A. Machine Learning Confirms Nonlinear Relationship between Severity of Peripheral Arterial Disease, Functional Limitation and Symptom Severity. Diagnostics. 2020; 10(8):515. https://doi.org/10.3390/diagnostics10080515
Chicago/Turabian StyleQutrio Baloch, Zulfiqar, Syed Ali Raza, Rahul Pathak, Luke Marone, and Abbas Ali. 2020. "Machine Learning Confirms Nonlinear Relationship between Severity of Peripheral Arterial Disease, Functional Limitation and Symptom Severity" Diagnostics 10, no. 8: 515. https://doi.org/10.3390/diagnostics10080515
APA StyleQutrio Baloch, Z., Raza, S. A., Pathak, R., Marone, L., & Ali, A. (2020). Machine Learning Confirms Nonlinear Relationship between Severity of Peripheral Arterial Disease, Functional Limitation and Symptom Severity. Diagnostics, 10(8), 515. https://doi.org/10.3390/diagnostics10080515





