Sequential Ultrasound Assessment of Peri-Articular Soft Tissue in Adhesive Capsulitis of the Shoulder: Correlations with Clinical Impairments—Sequential Ultrasound in Adhesive Capsulitis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Baseline Demographics and Clinical Assessments
2.3. Clinical Management
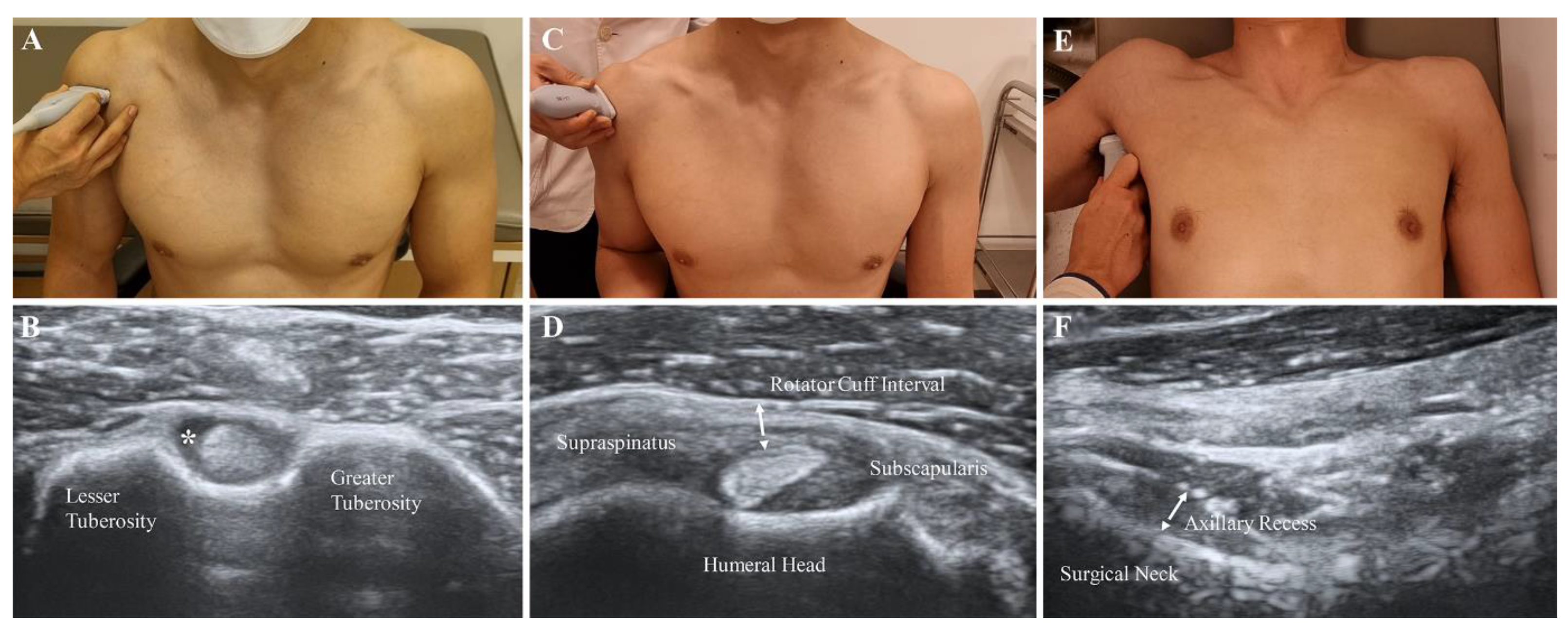
2.4. Ultrasound Parameters
2.5. Effusion of the LHBT
2.6. RI Thickness and Hypervascularity
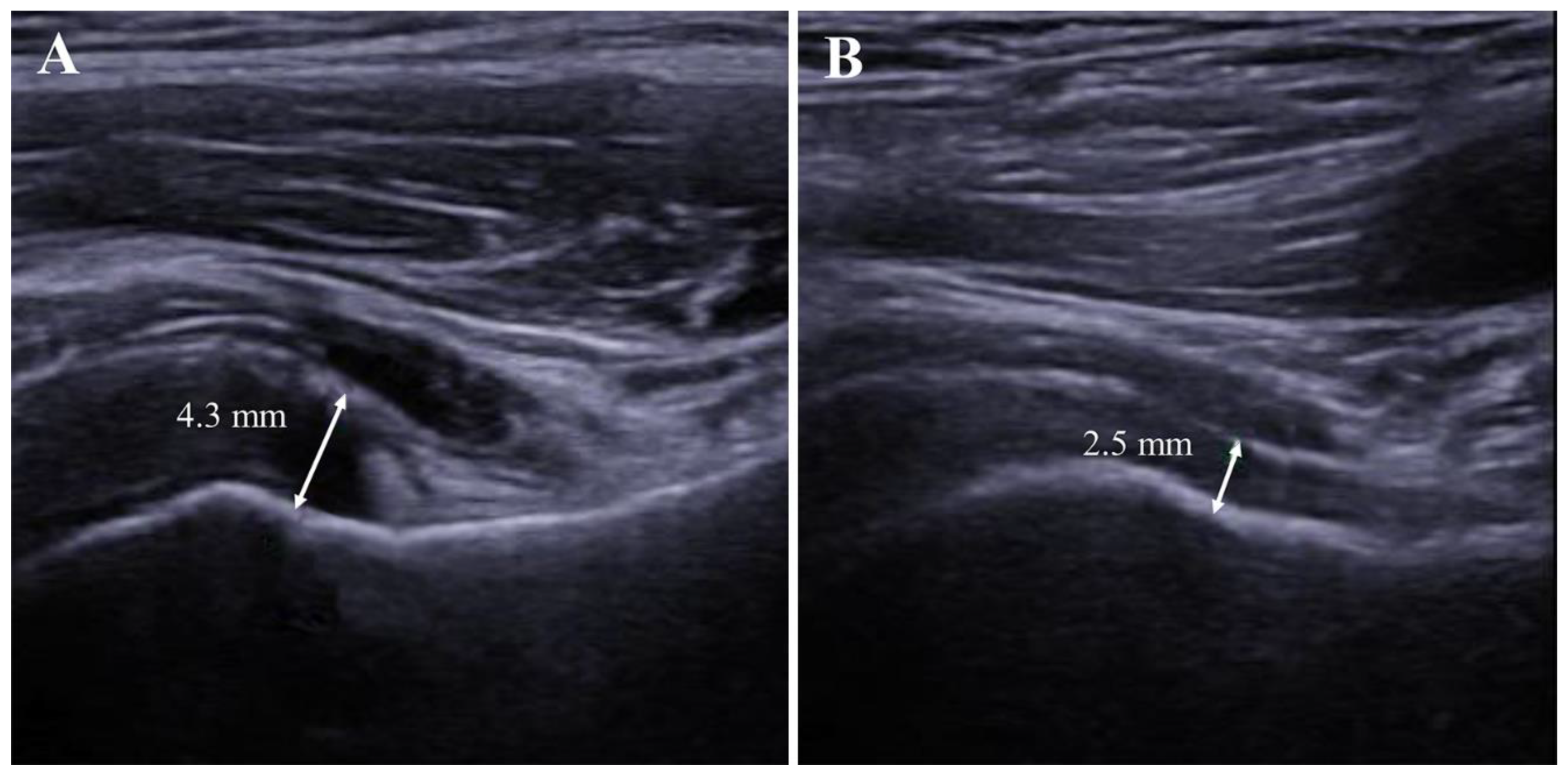
2.7. AR Thickness
2.8. Statistical Analysis
3. Results
3.1. Patient Characteristics
3.2. Initial Values and Sequential Changes of Ultrasound Parameters
3.3. Sequential Changes in Clinical Impairments
3.4. Correlations between UItrasound Parameters and Clinical Variables
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
References
- Fields, B.K.K.; Skalski, M.R.; Patel, D.B.; White, E.A.; Tomasian, A.; Gross, J.S.; Matcuk, G.R. Adhesive capsulitis: Review of imaging findings, pathophysiology, clinical presentation, and treatment options. Skelet. Radiol. 2019, 48, 1171–1184. [Google Scholar] [CrossRef] [PubMed]
- Woertler, K. Rotator interval. Semin. Musculoskelet. Radiol. 2015, 19, 243–253. [Google Scholar] [CrossRef] [PubMed]
- Passanante, G.J.; Skalski, M.R.; Patel, D.B.; White, E.A.; Schein, A.J.; Gottsegen, C.J.; Matcuk, G.R. Inferior glenohumeral ligament (IGHL) complex: Anatomy, injuries, imaging features, and treatment options. Emerg. Radiol. 2016, 24, 65–71. [Google Scholar] [CrossRef]
- Do, J.G.; Hwang, J.T.; Yoon, K.J.; Lee, Y.T. Correlation of Ultrasound Findings With Clinical Stages and Impairment in Adhesive Capsulitis of the Shoulder. Orthop. J. Sports Med. 2021, 9, 23259671211003675. [Google Scholar] [CrossRef]
- Park, G.-Y. Role of Ultrasonography in Diagnosis and Treatment of Frozen Shoulder. J. Rheum. Dis. 2019, 26. [Google Scholar] [CrossRef]
- Tandon, A.; Dewan, S.; Bhatt, S.; Jain, A.K.; Kumari, R. Sonography in diagnosis of adhesive capsulitis of the shoulder: A case–control study. J. Ultrasound 2017, 20, 227–236. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.-H.; Kim, D.H. Correlations between clinical features and MRI findings in early adhesive capsulitis of the shoulder: A retrospective observational study. BMC Musculoskelet. Disord. 2020, 21, 1–9. [Google Scholar] [CrossRef]
- Stella, S.M.; Gualtierotti, R.; Ciampi, B.; Trentanni, C.; Sconfienza, L.M.; Del Chiaro, A.; Pacini, P.; Miccoli, M.; Galletti, S. Ultrasound Features of Adhesive Capsulitis. Rheumatol. Ther. 2022, 9, 481–495. [Google Scholar] [CrossRef]
- Cheng, X.; Zhang, Z.; Xuanyan, G.; Li, T.; Li, J.; Yin, L.; Lu, M. Adhesive Capsulitis of the Shoulder: Evaluation With US-Arthrography Using a Sonographic Contrast Agent. Sci. Rep. 2017, 7, 5551. [Google Scholar] [CrossRef]
- Kim, D.H.; Cho, C.-H.; Sung, D.H. Ultrasound measurements of axillary recess capsule thickness in unilateral frozen shoulder: Study of correlation with MRI measurements. Skelet. Radiol. 2018, 47, 1491–1497. [Google Scholar] [CrossRef]
- Michelin, P.; Delarue, Y.; Duparc, F.; Dacher, J.N. Thickening of the inferior glenohumeral capsule: An ultrasound sign for shoulder capsular contracture. Eur. Radiol. 2013, 23, 2802–2806. [Google Scholar] [CrossRef] [PubMed]
- Hartrick, C.T.; Kovan, J.P.; Shapiro, S. The numeric rating scale for clinical pain measurement: A ratio measure? Pain Pract. 2003, 3, 310–316. [Google Scholar] [CrossRef]
- Kelley, M.J.; Shaffer, M.A.; Kuhn, J.E.; Michener, L.A.; Seitz, A.L.; Uhl, T.L.; Godges, J.J.; McClure, P.W. Shoulder pain and mo-bility deficits: Adhesive capsulitis. J. Orthop. Sports Phys. Ther. 2013, 43, A1–A31. [Google Scholar] [CrossRef] [PubMed]
- Fama, G.; Tagliapietra, J.; Belluzzi, E.; Pozzuoli, A.; Biz, C.; Ruggieri, P. Mid-Term Outcomes after Arthroscopic “Tear Comple-tion Repair” of Partial Thickness Rotator Cuff Tears. Medicina 2021, 57, 74. [Google Scholar] [CrossRef] [PubMed]
- Shaffer, B.; Tibone, J.E.; Kerlan, R.K. Frozen shoulder. A long-term follow-up. J. Bone Jt. Surg. Am. 1992, 74, 738–746. [Google Scholar] [CrossRef] [PubMed]
- Roach, K.E.; Budiman-Mak, E.; Songsiridej, N.; Lertratanakul, Y. Development of a Shoulder Pain and Disability Index. Arthritis Care Res. 1991, 4, 143–149. [Google Scholar] [CrossRef]
- Tamborrini, G.; Moller, I.; Bong, D.; Miguel, M.; Marx, C.; Muller, A.M.; Muller-Gerbl, M. The Rotator Interval—A Link Be-tween Anatomy and Ultrasound. Ultrasound Int. Open 2017, 3, E107–E116. [Google Scholar]
- Bakdash, J.Z.; Marusich, L.R. Repeated Measures Correlation. Front. Psychol. 2017, 8, 456. [Google Scholar] [CrossRef]
- Park, G.Y.; Park, J.H.; Kwon, D.R.; Kwon, D.G.; Park, J. Do the Findings of Magnetic Resonance Imaging, Arthrography, and Ultrasonography Reflect Clinical Impairment in Patients With Idiopathic Adhesive Capsulitis of the Shoulder? Arch. Phys. Med. Rehabil. 2017, 98, 1995–2001. [Google Scholar] [CrossRef]
- Song, K.D.; Kwon, J.W.; Yoon, Y.C.; Choi, S.-H. Indirect MR Arthrographic Findings of Adhesive Capsulitis. Am. J. Roentgenol. 2011, 197, W1105–W1109. [Google Scholar] [CrossRef]
- Lee, J.C.; Sykes, C.; Saifuddin, A.; Connell, D. Adhesive capsulitis: Sonographic changes in the rotator cuff interval with ar-throscopic correlation. Skeletal Radiol. 2005, 34, 522–527. [Google Scholar] [CrossRef]
- Walmsley, S.; Osmotherly, P.G.; Walker, C.J.; Rivett, D.A. Power Doppler ultrasonography in the early diagnosis of prima-ry/idiopathic adhesive capsulitis: An exploratory study. J. Manipulative Physiol. Ther. 2013, 36, 428–435. [Google Scholar] [CrossRef]
- Park, I.; Lee, H.J.; Kim, S.E.; Bae, S.H.; Lee, K.Y.; Park, K.S.; Kim, Y.S. Evaluation of the Effusion within Biceps Long Head Ten-don Sheath Using Ultrasonography. Clin. Orthop. Surg. 2015, 7, 351–358. [Google Scholar] [CrossRef]
- Kanazawa, K.; Hagiwara, Y.; Sekiguchi, T.; Suzuki, K.; Koide, M.; Ando, A.; Yabe, Y. Correlations between Capsular Changes and ROM Restriction in Frozen Shoulder Evaluated by Plain MRI and MR Arthrography. Open Orthop. J. 2018, 12, 396–404. [Google Scholar] [CrossRef]
- Park, S.; Lee, D.-H.; Yoon, S.-H.; Lee, H.Y.; Kwack, K.-S. Evaluation of Adhesive Capsulitis of the Shoulder With Fat-Suppressed T2-Weighted MRI: Association Between Clinical Features and MRI Findings. Am. J. Roentgenol. 2016, 207, 135–141. [Google Scholar] [CrossRef]
- Vastamäki, H.; Kettunen, J.; Vastamäki, M. The Natural History of Idiopathic Frozen Shoulder: A 2- to 27-year Followup Study. Clin. Orthop. Relat. Res. 2011, 470, 1133–1143. [Google Scholar] [CrossRef]
- Hand, C.; Clipsham, K.; Rees, J.L.; Carr, A.J. Long-term outcome of frozen shoulder. J. Shoulder Elb. Surg. 2008, 17, 231–236. [Google Scholar] [CrossRef]
- Bunker, T.D.; Anthony, P.P. The pathology of frozen shoulder. A Dupuytren-like disease. J. Bone Jt. Surg. Br. 1995, 77, 677–683. [Google Scholar] [CrossRef]
- Rodeo, S.A.; Hannafin, J.A.; Tom, J.; Warren, R.F.; Wickiewicz, T.L. Immunolocalization of cytokines and their receptors in adhesive capsulitis of the shoulder. J. Orthop. Res. 1997, 15, 427–436. [Google Scholar] [CrossRef]
- Lho, Y.-M.; Ha, E.; Cho, C.-H.; Song, K.S.; Min, B.-W.; Bae, K.-C.; Lee, K.-J.; Hwang, I.; Park, H.-B. Inflammatory cytokines are overexpressed in the subacromial bursa of frozen shoulder. J. Shoulder Elb. Surg. 2012, 22, 666–672. [Google Scholar] [CrossRef]
- Lubis, A.M.T.; Lubis, V.K. Matrix metalloproteinase, tissue inhibitor of metalloproteinase and transforming growth factor-beta 1 in frozen shoulder, and their changes as response to intensive stretching and supervised neglect exercise. J. Orthop. Sci. 2013, 18, 519–527. [Google Scholar] [CrossRef]


| Total (n= 56) | |
|---|---|
| Age, year | 53.1 ± 7.7 |
| Female, n (%) | 49 (87.5%) |
| DM, n (%) | 4 (7.1%) |
| Dominant side affected, n (%) | 32 (57.1%) |
| Corticosteroid injection | 41 (73.2%) |
| BMI (kg/m2) | 17.2 ± 3.3 |
| NRS (pain at resting) | 1.9 ± 2.1 |
| NRS (pain at activity) | 5.8 ± 2.0 |
| SPADI, pain (%) | 40.7 ± 20.3 |
| SPADI, disability (%) | 46.7 ± 17.4 |
| SPADI, total (%) | 43.0 ± 17.3 |
| FE, deg | 124.5 ± 18.1 |
| Abduction, deg | 87.2 ± 16.7 |
| IR, deg | 34.0 ± 16.4 |
| ER, deg | 33.0 ± 14.1 |
| n = 56 | Affected | Unaffected | p-Value |
|---|---|---|---|
| AR thickness, mm | 4.6 ± 1.6 | 2.5 ± 0.7 | <0.001 * |
| RI thickness, mm | 2.0 ± 0.6 | 1.7 ± 0.5 | 0.026 * |
| LHBT effusion | 20 (35.7%) | 3 (5.4%) | <0.001 * |
| Hypervascularity of RI | 1 (1.8%) | 0 (0%) | 1.000 |
| Initial | 1-Month | 3-Month | 6-Month | |
|---|---|---|---|---|
| NRS, pain (resting) | 1.9 ± 2.1 | 0.3 ± 0.7 * | 0.2 ± 0.5 | 0.1 ± 0.4 |
| NRS, pain (activity) | 5.8 ± 2.0 | 1.9 ± 1.1 * | 0.8 ± 1.1 † | 0.6 ± 0.9 |
| SPADI, pain (%) | 46.7 ± 17.4 | 17.3 ± 10.7 * | 10.1 ± 8.1 † | 7.2 ± 7.0 |
| SPADI, disability (%) | 40.7 ± 20.3 | 13.3 ± 10.3 * | 5.4 ± 5.4 † | 3.2 ± 5.6 ‡ |
| SPADI, total (%) | 43.0 ± 17.3 | 14.8 ± 9.1 * | 7.3 ± 5.6 † | 4.8 ± 5.9 ‡ |
| FE, deg | 124.5 ± 18.1 | 152.7 ± 13.6 * | 168.1 ± 10.6 † | 172.1 ± 11.6 ‡ |
| Abduction, deg | 87.2 ± 16.7 | 119.9 ± 17.8 * | 151.2 ± 24.3 † | 162.6 ± 22.3 ‡ |
| IR, deg | 34.0 ± 16.4 | 51.8 ± 14.1 * | 61.2 ± 11.9 † | 62.0 ± 11.2 |
| ER, deg | 33.0 ± 14.1 | 57.3 ± 15.3 * | 72.1 ± 15.7 † | 76.0 ± 15.2 |
| ART | ART Ratio | RIT | RIT Ratio | |
|---|---|---|---|---|
| NRS, pain (resting) | R: 0.363 | R: 0.376 | R: 0.241 | R: 0.406 |
| p < 0.001 | p < 0.001 | p = 0.003 | p < 0.001 | |
| NRS, pain (activity) | R: 0.557 | R: 0.539 | R: 0.359 | R: 0.391 |
| p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | |
| SPADI pain (%) | R: 0.580 | R: 0.578 | R: 0.351 | R: 0.450 |
| p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | |
| SPADI, disability (%) | R: 0.540 | R: 0.577 | R: 0.330 | R: 0.467 |
| p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | |
| SPADI total (%) | R: 0.569 | R: 0.591 | R: 0.346 | R: 0.471 |
| p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | |
| FE | R: −0.584 | R: −0.594 | R: −0.333 | R: −0.389 |
| p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | |
| AB | R: −0.566 | R: −0.554 | R: −0.318 | R: −0.330 |
| p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 | |
| IR | R: −0.436 | R: −0.434 | R: −0.228 | R: −0.278 |
| p < 0.001 | p < 0.001 | p = 0.005 | p < 0.001 | |
| ER | R: −0.571 | R: −0.538 | R: −0.340 | R: −0.339 |
| p < 0.001 | p < 0.001 | p < 0.001 | p < 0.001 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lee, B.C.; Yeo, S.M.; Do, J.G.; Hwang, J.H. Sequential Ultrasound Assessment of Peri-Articular Soft Tissue in Adhesive Capsulitis of the Shoulder: Correlations with Clinical Impairments—Sequential Ultrasound in Adhesive Capsulitis. Diagnostics 2022, 12, 2231. https://doi.org/10.3390/diagnostics12092231
Lee BC, Yeo SM, Do JG, Hwang JH. Sequential Ultrasound Assessment of Peri-Articular Soft Tissue in Adhesive Capsulitis of the Shoulder: Correlations with Clinical Impairments—Sequential Ultrasound in Adhesive Capsulitis. Diagnostics. 2022; 12(9):2231. https://doi.org/10.3390/diagnostics12092231
Chicago/Turabian StyleLee, Byung Chan, Seung Mi Yeo, Jong Geol Do, and Ji Hye Hwang. 2022. "Sequential Ultrasound Assessment of Peri-Articular Soft Tissue in Adhesive Capsulitis of the Shoulder: Correlations with Clinical Impairments—Sequential Ultrasound in Adhesive Capsulitis" Diagnostics 12, no. 9: 2231. https://doi.org/10.3390/diagnostics12092231






