Clinical Applicability of Ultrasound Shear Wave Elastography in Patients under Hypoglossal Nerve Stimulation Therapy
Abstract
:1. Introduction
2. Materials and Methods
3. Results
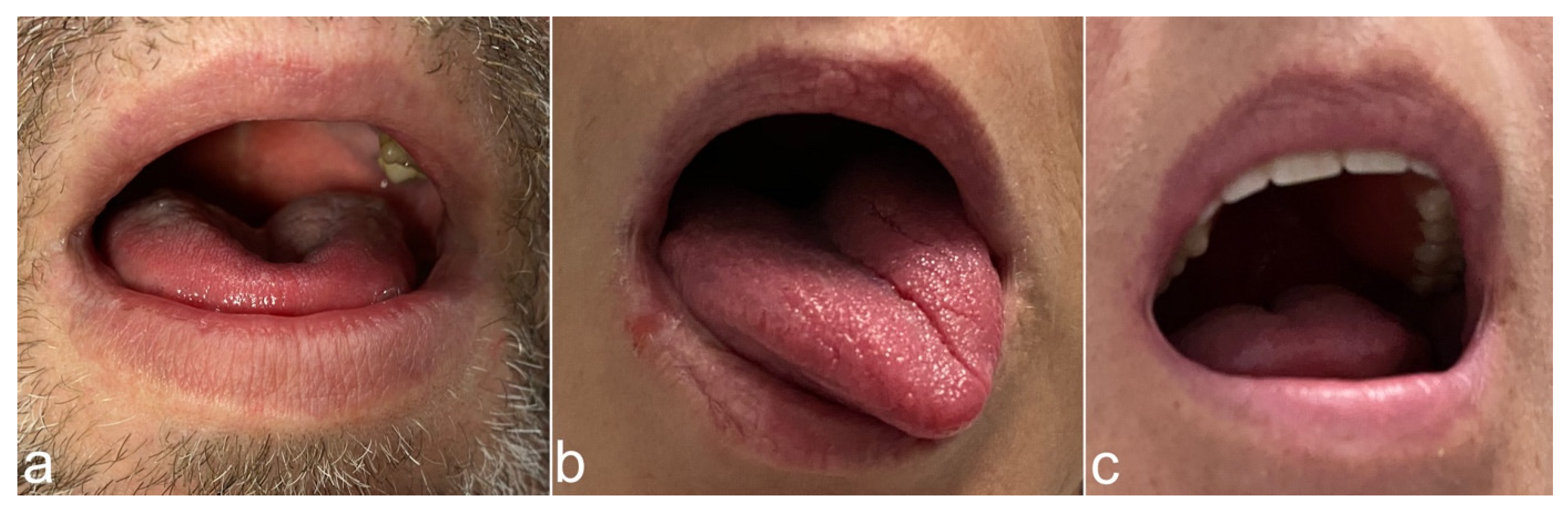
3.1. Clinical Results According to the Pattern of the Tongue Protrusion
3.2. US-SWE Results of Bilateral and Contralateral Tongue Protrusion Groups and Their Correlation to Clinical Outcome
- Bilateral protrusion: 5/9 patients with bilateral tongue protrusion were successfully treated (AHI < 15/h). No significant difference could be seen between the patients with and without therapy success in terms of absolute SWV (sGG, sGH, nGG and nGH) (see also Table 5). Patients with bilateral protrusion of the tongue under HNS therapy differed in clinical outcome with respect to the factor of increase in SWV in the genioglossus muscle (at the stimulator side (change factor SWV sGG wSTIMoSTIM, p = 0.032). Interestingly, a higher factor of SWV change in the ipsilateral GG muscle was measured in patients with treatment failure here. After adjusting the p-value with Bonferroni–Holm’s method, p-value did not reach significance value anymore (corr. p = 0.384). No further difference could be seen in this context with respect to the difference and increase in SWV values without and with stimulation regarding the other muscles (see also Table 5). Examination of SWV values (sGG, sGH, nGG, nGH under stimulation, increase factor of SWV) in relation to ESS, the absolute AHI values under therapy and the change of AHI under stimulation compared to baseline (change factor) revealed no significant correlation (see also Table 6).
- Protrusion to contralateral: 4/8 patients with tongue protrusion to the contralateral side were successfully treated (AHI < 15/h). A difference could only be seen between the patients with and without therapy success in terms of absolute SWV (sGG, sGH, nGG and nGH) at sGG without stimulation (2.08 (IQR 0.64) vs. 2.97 (IQR 0.51), p = 0.029). After adjusting the p-value with Bonferroni–Holm’s method p-value did not reach significance value anymore (corr. p = 0.348). Examination of SWV values (sGG, sGH, nGG, nGH under stimulation, increase factor of SWV) of the patients with tongue protrusion to the contralateral side in relation to ESS, the absolute AHI values under therapy and the change of AHI under stimulation compared to baseline (change factor) revealed also a correlation between SWV values at sGG without Stimulation to the current AHI under therapy (0.714; p = 0.047) and the change factor of the AHI (0.810; p = 0.015). After adjusting the p-value with Bonferroni–Holm’s method p-value did not reach significance value anymore (corr. p = 0.564 and corr. p = 0.18) (see also Table 5 and Table 7).
4. Discussion
- No general connection with the measured US-SWE values at the musculus GG and GH and the therapy outcome under HNS therapy can be found.
- There are indicators of a negative correlation between the AHI under therapy and the measured SWV of the musculus GH of the contralateral side during stimulation.
- The SWV of the genioglossus muscle of the stimulated side seem to differ in terms of clinical success parameters depending on the tongue movement pattern under stimulation.
5. Conclusions
- Contrary to expectations, the simple measurement of SWV of the genioglossi and geniohyoidei muscles under HNS therapy is not suitable for drawing conclusions about possible sleep medical therapy success.
- Measured SWV values at the GG and GH muscles do not allow for simple differentiation of the tongue movement pattern under therapy. In the future, neurophysiological studies of the tongue in combination of electromyography with US-SWE investigations could provide valuable insights in both directions.
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Gottlieb, D.J.; Punjabi, N.M. Diagnosis and Management of Obstructive Sleep Apnea: A Review. JAMA 2020, 323, 1380–1400. [Google Scholar] [CrossRef]
- Arens, P.; Hänsel, T.; Wang, Y. Hypoglossal Nerve Stimulation Therapy. Adv. Exp. Med. Biol. 2022, 1384, 351–372. [Google Scholar] [CrossRef]
- Strollo, P.J.; Soose, R.J.; Maurer, J.T.; de Vries, N.; Cornelius, J.; Froymovich, O.; Hanson, R.D.; Padhya, T.A.; Steward, D.L.; Gillespie, M.B.; et al. Upper-Airway Stimulation for Obstructive Sleep Apnea. N. Engl. J. Med. 2014, 370, 139–149. [Google Scholar] [CrossRef]
- Schwartz, A.R.; Jacobowitz, O.; Eisele, D.W.; Mickelson, S.A.; Miller, M.B.; Oliven, A.; Certal, V.; Hopp, M.L.; Winslow, D.H.; Huntley, T.C.; et al. Targeted Hypoglossal Nerve Stimulation for Patients with Obstructive Sleep Apnea: A Randomized Clinical Trial. JAMA Otolaryngol. Head. Neck Surg. 2023, 149, 512–520. [Google Scholar] [CrossRef]
- Eastwood, P.R.; Barnes, M.; MacKay, S.G.; Wheatley, J.R.; Hillman, D.R.; Nguyên, X.-L.; Lewis, R.; Campbell, M.C.; Pételle, B.; Walsh, J.H.; et al. Bilateral Hypoglossal Nerve Stimulation for Treatment of Adult Obstructive Sleep Apnea. Eur. Respir. J. 2019, 55, 1901320. [Google Scholar] [CrossRef]
- Mashaqi, S.; Patel, S.I.; Combs, D.; Estep, L.; Helmick, S.; Machamer, J.; Parthasarathy, S. The Hypoglossal Nerve Stimulation as a Novel Therapy for Treating Obstructive Sleep Apnea—A Literature Review. Int. J. Environ. Res. Public Health 2021, 18, 1642. [Google Scholar] [CrossRef]
- Bassiri Gharb, B.; Tadisina, K.K.; Rampazzo, A.; Hashem, A.M.; Elbey, H.; Kwiecien, G.J.; Doumit, G.; Drake, R.L.; Papay, F. Microsurgical Anatomy of the Terminal Hypoglossal Nerve Relevant for Neurostimulation in Obstructive Sleep Apnoea. Neuromodul. Technol. Neural Interface 2015, 18, 721–727. [Google Scholar] [CrossRef]
- Mu, L.; Sanders, I. Human Tongue Neuroanatomy: Nerve Supply and Motor Endplates. Clin. Anat. 2010, 23, 777–791. [Google Scholar] [CrossRef]
- Sanders, I.; Mu, L. A Three-Dimensional Atlas of Human Tongue Muscles. Anat. Rec. 2013, 296, 1102–1114. [Google Scholar] [CrossRef]
- Heiser, C.; Thaler, E.; Boon, M.; Soose, R.J.; Woodson, B.T. Updates of Operative Techniques for Upper Airway Stimulation. Laryngoscope 2016, 126, S12–S16. [Google Scholar] [CrossRef]
- Oliven, A.; O’Hearn, D.J.; Boudewyns, A.; Odeh, M.; De Backer, W.; van de Heyning, P.; Smith, P.L.; Eisele, D.W.; Allan, L.; Schneider, H.; et al. Upper Airway Response to Electrical Stimulation of the Genioglossus in Obstructive Sleep Apnea. J. Appl. Physiol. (1985) 2003, 95, 2023–2029. [Google Scholar] [CrossRef]
- Dotan, Y.; Golibroda, T.; Oliven, R.; Netzer, A.; Gaitini, L.; Toubi, A.; Oliven, A. Parameters Affecting Pharyngeal Response to Genioglossus Stimulation in Sleep Apnoea. Eur. Respir. J. 2011, 38, 338–347. [Google Scholar] [CrossRef]
- Fleury Curado, T.; Oliven, A.; Sennes, L.U.; Polotsky, V.Y.; Eisele, D.; Schwartz, A.R. Neurostimulation Treatment of OSA. Chest 2018, 154, 1435–1447. [Google Scholar]
- Heiser, C. Advanced Titration to Treat a Floppy Epiglottis in Selective Upper Airway Stimulation. Laryngoscope 2016, 126, S22–S24. [Google Scholar] [CrossRef]
- Gervasio, A.; D’Orta, G.; Mujahed, I.; Biasio, A. Sonographic Anatomy of the Neck: The Suprahyoid Region. J. Ultrasound 2011, 14, 130–135. [Google Scholar] [CrossRef]
- Arens, P.; Fischer, T.; Dommerich, S.; Olze, H.; Lerchbaumer, M.H. Ultrasound Shear Wave Elastography of the Tongue during Selective Hypoglossal Nerve Stimulation in Patients with Obstructive Sleep Apnea Syndrome. Ultrasound Med. Biol. 2021, 47, 2869–2879. [Google Scholar] [CrossRef]
- Chang, C.H.; Huang, C.C.; Wang, Y.H.; Chou, F.J.; Chen, J.W. Ultrasound Shear-Wave Elastography of the Tongue in Adults with Obstructive Sleep Apnea. Ultrasound Med. Biol. 2020, 46, 1658–1669. [Google Scholar] [CrossRef]
- Chu, C.A.; Chen, Y.J.; Chang, K.V.; Wu, W.T.; Özçakar, L. Reliability of Sonoelastography Measurement of Tongue Muscles and Its Application on Obstructive Sleep Apnea. Front. Physiol. 2021, 12, 654667. [Google Scholar] [CrossRef]
- Brown, E.C.; Cheng, S.; McKenzie, D.K.; Butler, J.E.; Gandevia, S.C.; Bilston, L.E. Tongue Stiffness Is Lower in Patients with Obstructive Sleep Apnea during Wakefulness Compared with Matched Control Subjects. Sleep 2015, 38, 537–544. [Google Scholar] [CrossRef]
- Ikidag, M.A.; Oksuzler, M. Utility of Tongue Root Acoustic Radiation Force Impulse Ultrasound Elastography in Determination of Obstructive Sleep Apnea Risk. Eurasian J. Med. Investig. 2022, 6, 424–428. [Google Scholar] [CrossRef]
- Heiser, C.; Vanderveken, O.M.; Edenharter, G.M.; Hofauer, B. Cross Motor Innervation of the Hypoglossal Nerve—A Pilot Study of Predictors for Successful Opening of the Soft Palate. Sleep Breath. 2020, 25, 425–431. [Google Scholar] [CrossRef]
- Thaler, E.; Schwab, R.; Maurer, J.; Soose, R.; Larsen, C.; Stevens, S.; Stevens, D.; Boon, M.; Huntley, C.; Doghramji, K.; et al. Results of the ADHERE Upper Airway Stimulation Registry and Predictors of Therapy Efficacy. Laryngoscope 2019, 130, 1333–1338. [Google Scholar] [CrossRef]
- Zinchuk, A.V.; Gentry, M.J.; Concato, J.; Yaggi, H.K. Phenotypes in Obstructive Sleep Apnea: A Definition, Examples and Evolution of Approaches. Sleep Med. Rev. 2017, 35, 113–123. [Google Scholar] [CrossRef]
- Maniaci, A.; Riela, P.M.; Iannella, G.; Lechien, J.R.; La Mantia, I.; De Vincentiis, M.; Cammaroto, G.; Calvo-Henriquez, C.; Di Luca, M.; Chiesa Estomba, C.; et al. Machine Learning Identification of Obstructive Sleep Apnea Severity through the Patient Clinical Features: A Retrospective Study. Life 2023, 13, 702. [Google Scholar] [CrossRef]
| All Patients (n = 18) | |
|---|---|
| Current ESS | 8 (IQR 12) |
| Baseline AHI (events/h) | 31.65 (IQR 25.1) |
| AHI under therapy (events/h) | 16.3 (IQR 20.03) |
| All Patients (n = 18) | |
|---|---|
| SWV Variable (Median (Unit), IQR) | Therapy Success AHI < 15/h (Yes vs. No) |
| SWV sGH oSTIM (2.11 m/s, IQR 0.57) | 2.12 (IQR 0.47) vs. 2.10 (IQR 0.69); p = 0.931 (corr. p ≥ 0.999) |
| SWV sGH wSTIM (2.53 m/s, IQR 1.5) | 2.67 (IQR 1.52) vs. 2.40 (IQR 1.53); p = 0.666 (corr. p ≥ 0.999) |
| DIFF SWV sGH wSTIM-oSTIM (0.45 m/s, IQR 1.89) | 0.48 (IQR 1.78) vs. 0.41 (IQR 1.84); p = 0.605 (corr. p ≥ 0.999) |
| SWV sGG oSTIM (2.50 m/s, IQR 0.96) | 2.32 (IQR 1.02) vs. 2.73 (IQR 1.05); p = 0.730 (corr. p ≥ 0.999) |
| SWV sGG wSTIM (4.78 m/s, IQR 1.32) | 4.98 (IQR 1.64) vs. 4.58 (IQR 1.05); p = 0.730 (corr. p ≥ 0.999) |
| DIFF SWV sGG wSTIM-oSTIM (2.16 m/s; IQR 1.39) | 1.99 (IQR 1.51) vs. 2.29 (IQR 1.36); p = 0.666 (corr. p ≥ 0.999) |
| SWV nGH oSTIM (2.03 m/s, IQR 0.73) | 2.15 (IQR 0.48) vs. 1.77 (IQR 0.82); p = 0.094 (corr. p ≥ 0.999) |
| SWV nGH wSTIM (1.69 m/s; IQR 0.48) | 2.02 (IQR 0.46) vs. 1.76 (IQR 0.46); p = 0.05 (corr. p = 0.75) |
| DIFF SWV nGH wSTIM-oSTIM (−0.16 m/s; IQR 0.53) | −0.15 (IQR 0.80) vs. −0.24 (IQR 0.51); p = 1.00 (corr. p ≥ 0.999) |
| SWV nGG oSTIM (2.48, IQR 0.62) | 2.44 (IQR 0.48) vs. 2.51 (IQR 0.78); p = 1.00 (corr. p ≥ 0.999) |
| SWV nGG wSTIM (2.21 m/s; 1.06) | 2.26 (IQR 1.96) vs. 1.86 (IQR 1.17); p = 0.190 (corr. p ≥ 0.999) |
| DIFF SWV nGG wSTIM-oSTIM (−0.43 m/s; IQR 1.16) | 0.11 (IQR 1.66) vs. −0.49 (IQR 1.59); p = 0.190 (corr. p ≥ 0.999) |
| Change Factor SWV sGH wSTIMoSTIM (1.24; IQR 0.81) | 1.27 (IQR 0.80) vs. 1.22 (IQR 0.90); p = 0.546 (corr. p ≥ 0.999) |
| Change Factor SWV sGG wSTIMoSTIM (1.82; IQR 0.64) | 1.76 (IQR 0.80) vs. 1.89 (IQR 0.80); p = 0.605 (corr. p ≥ 0.999) |
| Change Factor SWV nGH wSTIMoSTIM (0.93; IQR 0.25) | 0.94 (IQR 0.35) vs. 0.92 (IQR 0.27); p = 0.931 (corr. p ≥ 0.999) |
| Change Factor SWV nGG wSTIMoSTIM (0.82; IQR 0.51) | 1.04 (IQR 0.64) vs. 0.77 (IQR 0.57); p = 0.094 (corr. p ≥ 0.999) |
| All Patients (n = 18) | |||
|---|---|---|---|
| SWV Variable (Median (Unit), IQR) | Correlation to Current AHI under Therapy (16.3/h; IQR 20.03) | Correlation to Change Factor AHI (0.58; IQR 0.64) | Correlation to ESS (8; IQR 12) |
| SWV sGH oSTIM (2.11 m/s, IQR 0.57) | −0.40 (p = 0.874; corr. p ≥ 0.999) | 0.102 (p = 0.687; corr. p ≥ 0.999) | −0.350 (p = 0.155; corr. p ≥ 0.999) |
| SWV sGH wSTIM (2.53 m/s, IQR 1.5) | −0.234 (p = 0.349; corr. p ≥ 0.999) | −0.414 (p = 0.088; corr. p ≥ 0.999) | 0.121 (p = 0.631; corr. p ≥ 0.999) |
| DIFF SWV sGH wSTIM-oSTIM (0.45 m/s, IQR 1.89) | −0.174 (p = 0.489; corr. p ≥ 0.999) | −0.373 (p = 0.128; corr. p ≥ 0.999) | 0.262 (p = 0.293; corr. p ≥ 0.999) |
| SWV sGG oSTIM (2.50 m/s, IQR 0.96) | 0.104 (p = 0.681; corr. p ≥ 0.999) | 0.232 (p = 0.354; corr. p ≥ 0.999) | −0.252 (p = 0.313; corr. p ≥ 0.999) |
| SWV sGG wSTIM (4.78 m/s, IQR 1.32) | −0.092 (p = 0.717; corr. p ≥ 0.999) | −0.323 (p = 0.191; corr. p ≥ 0.999) | 0.111 (p = 0.661; corr. p ≥ 0.999) |
| DIFF SWV sGG wSTIM-oSTIM (2.16 m/s; IQR 1.39) | −0.074 (p = 0.769; corr. p ≥ 0.999) | −0.385 (p = 0.115; corr. p ≥ 0.999) | 0.290 (p = 0.244; corr. p ≥ 0.999) |
| SWV nGH oSTIM (2.03 m/s, IQR 0.73) | −0.469 (p = 0.050; corr. p = 0.7) | −0.343 (p = 0.164; corr. p ≥ 0.999) | −0.115 (p = 0.650; corr. p ≥ 0.999) |
| SWV nGH wSTIM (1.69 m/s; IQR 0.48) | −0.622 (p = 0.006; corr. p = 0.096) | −0.420 (p = 0.083; corr. p ≥ 0.913) | −0.291 (p = 0.241; corr. p ≥ 0.999) |
| DIFF SWV nGH wSTIM-oSTIM (−0.16 m/s; IQR 0.53) | −0.053 (p = 0.836; corr. p ≥ 0.999) | −0.083 (p = 0.880; corr. p ≥ 0.999) | −0.052 (p = 0.838; corr. p ≥ 0.999) |
| SWV nGG oSTIM (2.48 m/s, IQR 0.62) | −0.045 (p = 0.858; corr. p ≥ 0.999) | 0.035 (p = 0.890; corr. p ≥ 0.999) | 0.415 (p = 0.087; corr. p ≥ 0.999) |
| SWV nGG wSTIM (2.21 m/s; 1.06) | −0.426 (p = 0.078; corr. p ≥ 0.63) | −0.169 (p = 0.502; corr. p ≥ 0.999) | −0.052 (p = 0.838; corr. p ≥ 0.999) |
| DIFF SWV nGG wSTIM-oSTIM (−0.43 m/s; IQR 1.16) | −0.358 (p = 0.145; corr. p ≥ 0.999) | −0.170 (p = 0.499 corr. p ≥ 0.999) | −0.287 (p = 0.248; corr. p ≥ 0.999) |
| Change factor SWV sGH wSTIMoSTIM (1.24; IQR 0.81) | −0.191 (p = 0.448; corr. p ≥ 0.999) | −0.393 (p = 0.106 corr. p ≥ 0.999) | 0.285 (p = 0.251; corr. p ≥ 0.999) |
| Change factor SWV sGG wSTIMoSTIM (1.82; IQR 0.64) | −0.057 (p = 0.823; corr. p ≥ 0.999) | −0.323 (p = 0.191 corr. p ≥ 0.999) | 0.315 (p = 0.202; corr. p ≥ 0.999) |
| Change factor SWV nGH wSTIMoSTIM (0.93; IQR 0.25) | −0.077 (p = 0.760; corr. p ≥ 0.999) | 0.034 (p = 0.893 corr. p ≥ 0.999) | −0.074 (p = 0.77; corr. p ≥ 0.999)) |
| Change factor SWV nGG wSTIMoSTIM (0.82; IQR 0.51) | −0.484 (p = 0.042; corr. p ≥ 0.63) | −0.294 (p = 0.236 corr. p ≥ 0.999) | −0.315 (p = 0.202; corr. p ≥ 0.999) |
| Bilateral Tongue Protrusion (n = 9) | Contralateral Tongue Protrusion (n = 8) | ||
|---|---|---|---|
| ESS | 5 (IQR 5) | 14.5 (IQR 12) | p = 0.1 |
| Baseline AHI | 26.4/h (IQR 36.3) | 14.5 (IQR 12) | p = 0.773 |
| Current AHI under therapy | 14.5/h (IQR 13.05) | 15.1/h (IQR 31.43) | p = 0.847 |
| Change factor AHI | 0.7932 (IQR 0.54) | 0.5587 (IQR 0.81) | p = 0.7 |
| Therapy success AHI < 15/h | n = 5 | n = 4 | p = 0.824 |
| Therapy Success AHI < 15/h (Yes vs. No) (Mann–Whitney U Test) | ||
|---|---|---|
| Bilateral Tongue Protrusion (n = 9) | Contralateral Tongue Protrusion (n = 8) | |
| SWV sGH oSTIM (m/s) | 2.25 (IQR 0.63) vs. 2.26 (IQR 0.91); p = 1.000 (corr. p ≥ 0.999) | 2.05 (IQR 0.59) vs. 2.18 (IQR 0.52); p = 0.486 (corr. p ≥ 0.999) |
| SWV sGH wSTIM (m/s) | 2.26 (IQR 1.14) vs. 2.76 (IQR 1.95); p = 0.730 (corr. p ≥ 0.999) | 3.22 (IQR 1.08) vs. 2.42 (IQR 1.93); p = 0.343 (corr. p ≥ 0.999) |
| SWV sGG oSTIM (m/s) | 2.99 (IQR 0.88) vs. 2.40 (IQR 0.96); p = 0.286 (corr. p ≥ 0.999) | 2.08 (IQR 0.64) vs. 2.97 (IQR 0.51); p = 0.029 (corr. p = 0.348) |
| SWV sGG wSTIM (m/s) | 5.16 (IQR 1.95) vs. 4.52 (IQR 1.31); p = 1.000 (corr. p ≥ 0.999) | 4.53 (1.89) vs. 4.78 (IQR 1.47); p = 1.000 (corr. p ≥ 0.999) |
| SWV nGH oSTIM (m/s) | 2.15 (IQR 0.4) vs. 1.78 (IQR 1.03); p = 0.286 (corr. p ≥ 0.999) | 2.29 (IQR 0.58) vs. 1.68 (IQR 1.05); p = 0.343 (corr. p ≥ 0.999) |
| SWV nGH wSTIM (m/s) | 2.01 (IQR 0.66) vs. 1.96 (IQR 0.98); p = 0.413 (corr. p ≥ 0.999) | 2.12 (IQR 0.56) vs. 1.65 (IQR 0.32); p = 0.114 (corr. p ≥ 0.999) |
| SWV nGG oSTIM (m/s) | 2.44 (IQR 0.79) vs. 2.26 (IQR 1.81); p = 0.905 (corr. p ≥ 0.999) | 2.72 (IQR 0.36) vs. 2.56 (IQR 0.71); p = 0.686 (corr. p ≥ 0.999) |
| SWV nGG wSTIM (m/s) | 2.16 (IQR 2.45) vs. 2.31 (IQR 1.31); p = 0.730 (corr. p ≥ 0.999) | 2.39 (IQR 1.61) vs. 1.66 (IQR 0.99); p = 0.200 (corr. p ≥ 0.999) |
| Change Factor SWV sGH wSTIMoSTIM | 1.03 (IQR 0.56) vs. 1.17 (IQR 1.11); p = 1.000 (corr. p ≥ 0.999) | 1.62 (IQR 1.05) vs. 1.04 (IQR 1.12; p = 0.343 (corr. p ≥ 0.999) |
| Change Factor SWV sGG wSTIMoSTIM | 1.70 (IQR 0.27) vs. 1.98 (IQR 0.75); p = 0.032 (corr. p = 0.384) | 2.31 (IQR 1.50) vs. 1.63 (IQR 0.76); p = 0.343 (corr. p ≥ 0.999) |
| Change Factor SWV nGH wSTIMoSTIM | 0.93 (IQR 0.46) vs. 0.98 (IQR 0.27); p = 0.730 (corr. p ≥ 0.999) | 0.95 (IQR 0.41) vs. 0.91 (IQR 0.44); p = 0.886 (corr. p ≥ 0.999) |
| Change Factor SWV nGG wSTIMoSTIM | 1.23 (IQR 0.95) vs. 0.96 (IQR 0.63); p = 0.286 (corr. p ≥ 0.999) | 0.94 (IQR 0.57) vs. 0.68 (IQR 0.48); p = 0.343 (corr. p ≥ 0.999) |
| Bilateral Tongue Protrusion (n = 9) | |||
|---|---|---|---|
| Correlation with Current AHI under Therapy | Correlation with Change Factor AHI | Correlation with ESS | |
| SWV sGH oSTIM (m/s) | −0.150 (p = 0.700; corr. p ≥ 0.999) | −0.050 (p = 0.898; corr. p ≥ 0.999) | −0.017 (p = 0.965; corr. p ≥ 0.999) |
| SWV sGH wSTIM (m/s) | 0.017 (p = 0.966; corr. p ≥ 0.999) | −0.367 (p = 0.332; corr. p ≥ 0.999) | 0.051 (p = 0.897; corr. p ≥ 0.999) |
| SWV sGG oSTIM (m/s) | −0.633 (p = 0.067; corr. p ≥ 0.804) | −0.517 (p = 0.154; corr. p ≥ 0.999) | −0.475 (p = 0.197; corr. p ≥ 0.999) |
| SWV sGG wSTIM (m/s) | −0.217 (p = 0.576; corr. p ≥ 0.999) | −0.383 (p = 0.308; corr. p ≥ 0.999) | −0.085 (p = 0.828; corr. p ≥ 0.999) |
| SWV nGH oSTIM (m/s) | −0.502 (p = 0.168; corr. p ≥ 0.999) | −0.393 (p = 0.295; corr. p ≥ 0.999) | 0.043 (p = 0.913; corr. p ≥ 0.999) |
| SWV nGH wSTIM (m/s) | −0.517 (p = 0.154; corr. p ≥ 0.999) | −0.350 (p = 0.356; corr. p ≥ 0.999) | −0.271 (p = 0.480; corr. p ≥ 0.999) |
| SWV nGG oSTIM (m/s) | −0.192 (p = 0.620; corr. p ≥ 0.999) | 0.042 (p = 0.915; corr. p ≥ 0.999) | 0.366 (p = 0.333; corr. p ≥ 0.999) |
| SWV nGG wSTIM (m/s) | −0.418 (p = 0.262; corr. p ≥ 0.999) | 0.075 (p = 0.847; corr. p ≥ 0.999) | −0.289 (p = 0.450; corr. p ≥ 0.999) |
| Change Factor SWV sGH wSTIMoSTIM | 0.177 (p = 0.765; corr. p ≥ 0.999) | −0.250 (p = 0.516; corr. p ≥ 0.999) | 0.186 (p = 0.631; corr. p ≥ 0.999) |
| Change Factor SWV sGG wSTIMoSTIM | 0.550 (p = 0.125; corr. p ≥ 0.999) | 0.250 (p = 0.516; corr. p ≥ 0.999) | 0.220 (p = 0.569; corr. p ≥ 0.999) |
| Change Factor SWV nGH wSTIMoSTIM | 0.033 (p = 0.932; corr. p ≥ 0.999) | 0.267 (p = 0.488; corr. p ≥ 0.999) | −0.237 (p = 0.539; corr. p ≥ 0.999) |
| Change Factor SWV nGG wSTIMoSTIM | −0.533 (p = 0.139; corr. p ≥ 0.999) | −0.183 (p = 0.637; corr. p ≥ 0.999) | −0.593 (p = 0.092; corr. p ≥ 0.999) |
| Contralateral Tongue Protrusion (n = 8) | |||
|---|---|---|---|
| Correlation with Current AHI under Therapy | Correlation with Change Factor AHI | Correlation with ESS | |
| SWV sGH oSTIM (m/s) | 0.071 (p = 0.867; corr. p ≥ 0.999) | 0.357 (p = 0.385; corr. p ≥ 0.999) | −0.539 (p = 0.168; corr. p ≥ 0.999) |
| SWV sGH wSTIM (m/s) | −0.262 (p = 0.531; corr. p ≥ 0.999) | −0.452 (p = 0.260; corr. p ≥ 0.999) | 0.335 (p = 0.417; corr. p ≥ 0.999) |
| SWV sGG oSTIM (m/s) | 0.714 (p = 0.047; corr. p = 0.564) | 0.810 (p = 0.015; corr. p = 0.18) | −0.192 (p = 0.649; corr. p ≥ 0.999) |
| SWV sGG wSTIM (m/s) | 0.214 (p = 0.610; corr. p ≥ 0.999) | 0.048 (p = 0.911; corr. p ≥ 0.999) | 0.371 (p = 0.365; corr. p ≥ 0.999) |
| SWV nGH oSTIM (m/s) | −0.500 (p = 0.207; corr. p ≥ 0.999) | −0.214 (p = 0.610; corr. p ≥ 0.999) | −0.240 (p = 0.568; corr. p ≥ 0.999) |
| SWV nGH wSTIM (m/s) | −0.690 (p = 0.058; corr. p = 0.638) | −0.619 (p = 0.102; corr. p ≥ 0.999) | −0.287 (p = 0.490; corr. p ≥ 0.999) |
| SWV nGG oSTIM (m/s) | −0.190 (p = 0.651; corr. p ≥ 0.999) | 0.167 (p = 0.693; corr. p ≥ 0.999) | 0.048 (p = 0.910; corr. p ≥ 0.999) |
| SWV nGG wSTIM (m/s) | −0.381 (p = 0.352; corr. p ≥ 0.999) | −0.286 (p = 0.493; corr. p ≥ 0.999) | 0.156 (p = 0.713; corr. p ≥ 0.999) |
| Change Factor SWV sGH wSTIMoSTIM | −0.286 (p = 0.493; corr. p ≥ 0.999) | −0.476 (p = 0.233; corr. p ≥ 0.999) | 0.299 (p = 0.471; corr. p ≥ 0.999) |
| Change Factor SWV sGG wSTIMoSTIM | −0.310 (p = 0.456; corr. p ≥ 0.999) | −0.524 (p = 0.183; corr. p ≥ 0.999) | 0.287 (p = 0.490; corr. p ≥ 0.999) |
| Change Factor SWV nGH wSTIMoSTIM | 0.048 (p = 0.911; corr. p ≥ 0.999) | −0.214 (p = 0.610; corr. p ≥ 0.999) | 0.275 (p = 0.509; corr. p ≥ 0.999) |
| Change Factor SWV nGG wSTIMoSTIM | −0.310 (p = 0.456; corr. p ≥ 0.999) | −0.333 (p = 0.420; corr. p ≥ 0.999) | 0.132 (p = 0.756; corr. p ≥ 0.999) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Arens, P.; Fischer, T.; Fietze, I.; Penzel, T.; Dommerich, S.; Olze, H.; Lerchbaumer, M.H. Clinical Applicability of Ultrasound Shear Wave Elastography in Patients under Hypoglossal Nerve Stimulation Therapy. Diagnostics 2023, 13, 3493. https://doi.org/10.3390/diagnostics13233493
Arens P, Fischer T, Fietze I, Penzel T, Dommerich S, Olze H, Lerchbaumer MH. Clinical Applicability of Ultrasound Shear Wave Elastography in Patients under Hypoglossal Nerve Stimulation Therapy. Diagnostics. 2023; 13(23):3493. https://doi.org/10.3390/diagnostics13233493
Chicago/Turabian StyleArens, Philipp, Thomas Fischer, Ingo Fietze, Thomas Penzel, Steffen Dommerich, Heidi Olze, and Markus Herbert Lerchbaumer. 2023. "Clinical Applicability of Ultrasound Shear Wave Elastography in Patients under Hypoglossal Nerve Stimulation Therapy" Diagnostics 13, no. 23: 3493. https://doi.org/10.3390/diagnostics13233493
APA StyleArens, P., Fischer, T., Fietze, I., Penzel, T., Dommerich, S., Olze, H., & Lerchbaumer, M. H. (2023). Clinical Applicability of Ultrasound Shear Wave Elastography in Patients under Hypoglossal Nerve Stimulation Therapy. Diagnostics, 13(23), 3493. https://doi.org/10.3390/diagnostics13233493









