Pulmonary Ultrasonography in Systemic Sclerosis-Induced Interstitial Lung Disease—A Systematic Review and Meta-Analysis
Abstract
:1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Literature Selection
- Study design: clinical trials, randomized controlled trials, cohort studies, or observational studies;
- Studies assessing the presence of interstitial lung disease using lung ultrasound examination compared to HRCT in SSc patients;
- Studies including human participants over 18 years old;
- Studies available online and in English;
- Studies with appropriate data availability.
- Study design: letters, editorials, comments, meeting abstracts, case reports, review, systematic review, or meta-analysis;
- Studies not assessing the presence of interstitial lung disease using lung ultrasound examination compared to HRCT in SSc patients;
- Studies including patients with other conditions with impact on pulmonary tissue or connective tissue;
- Studies with no appropriate data availability or no differentiation of SSc patients among other participants;
- Studies not including human participants over 18 years old;
- Studies unavailable online or in English.
2.3. Data Extraction
2.4. Outcome Measures
2.5. Quality Assessment
2.6. Statistical Analysis
3. Results
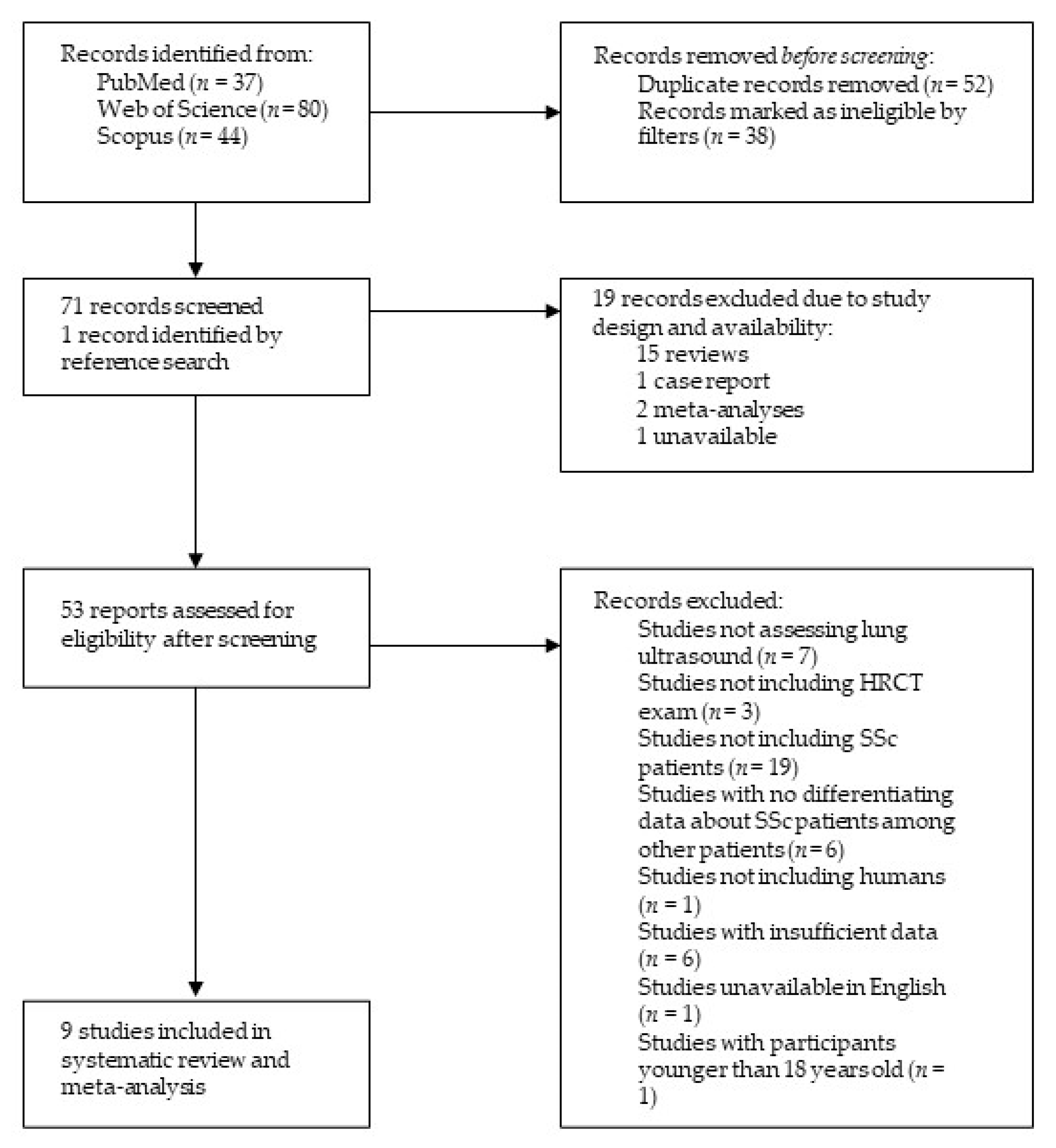
3.1. Literature Search Results
3.2. Characteristics of the Included Studies
3.3. Risk-of-Bias and Quality Assessment
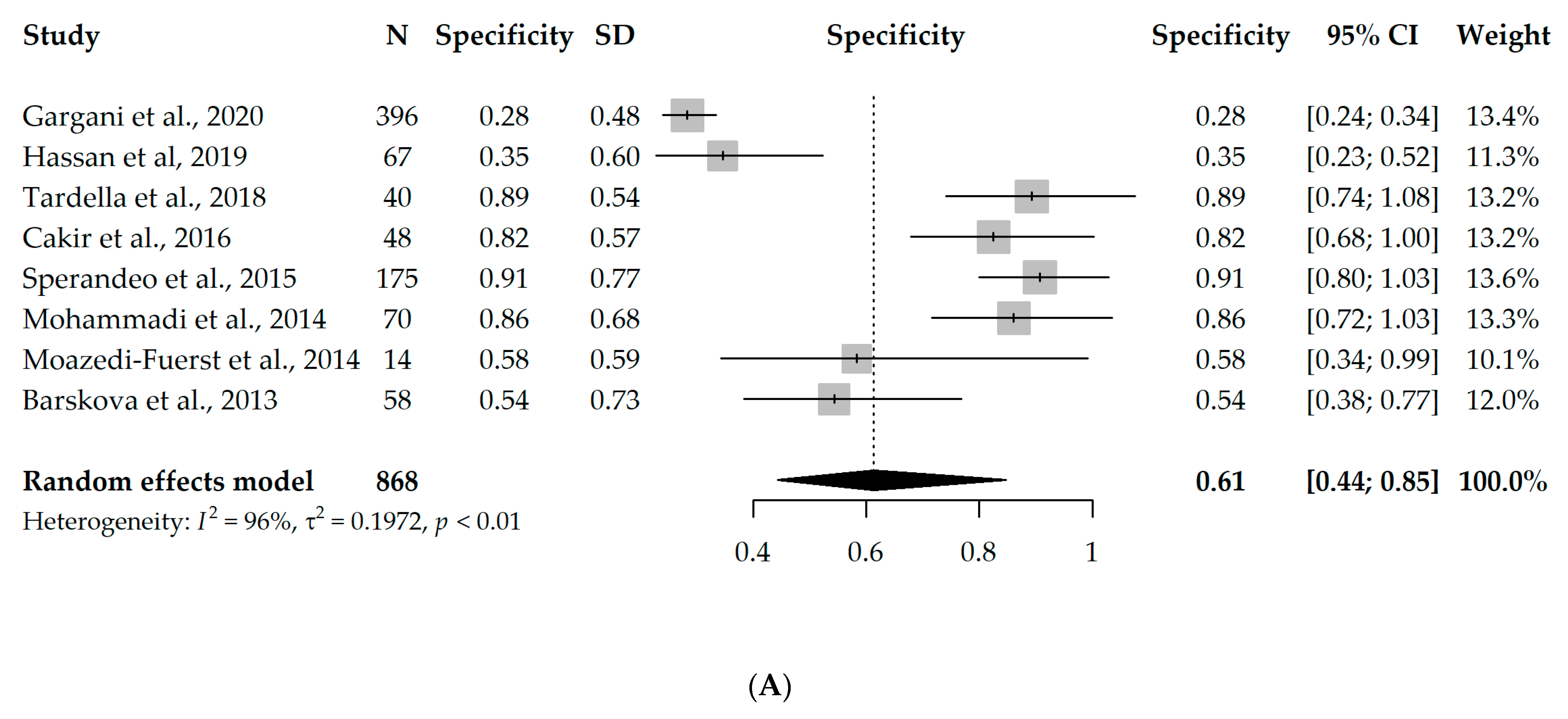
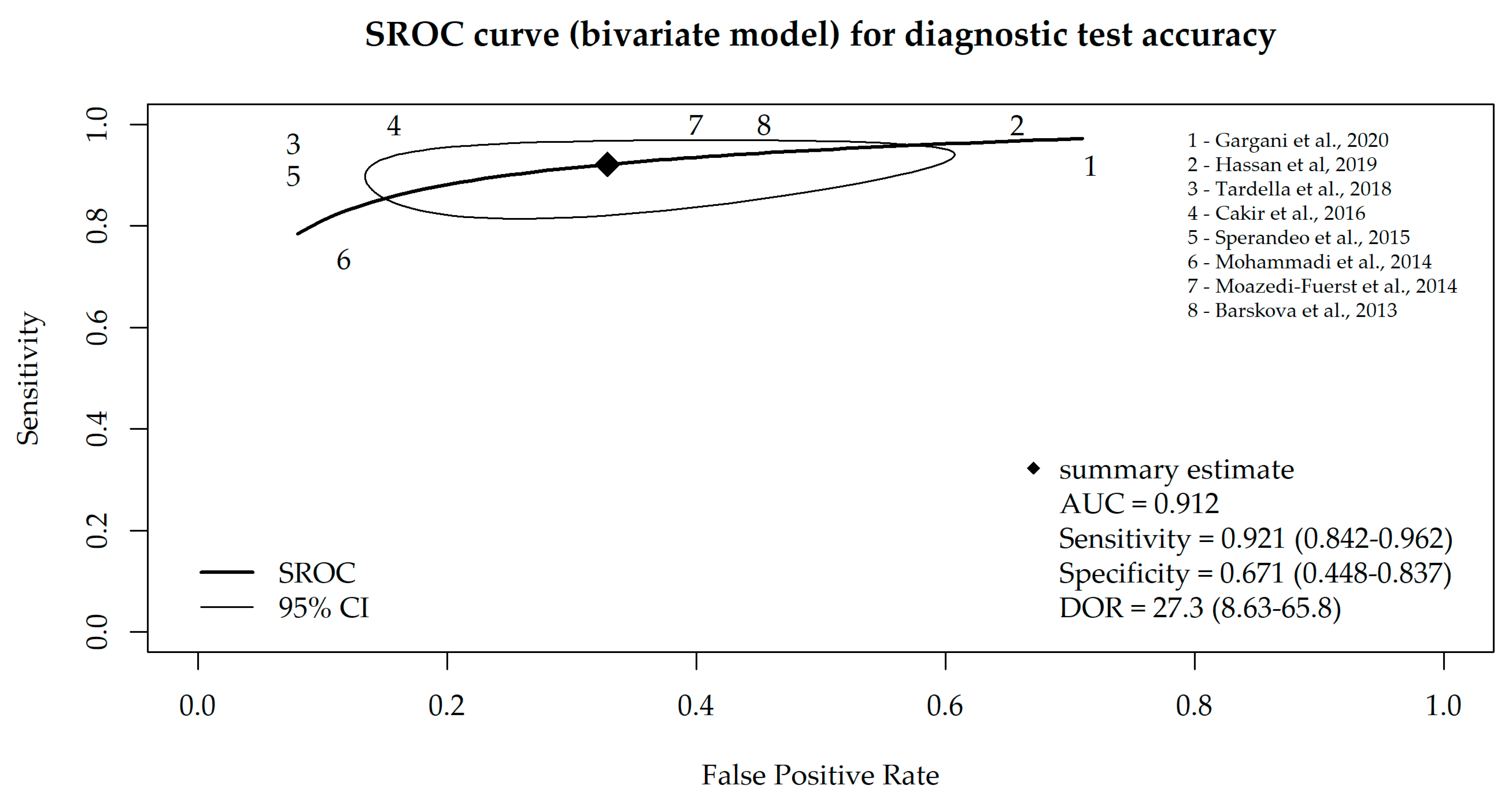
3.4. Meta-Analysis of LUS Assessment and B-Line Analysis
3.5. Meta-Analysis of the Number of LIS Points Examined
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Denton, C.P.; Khanna, D. Systemic sclerosis. Lancet 2017, 390, 1685–1699. [Google Scholar] [CrossRef] [PubMed]
- Perelas, A.; Silver, R.M.; Arrossi, A.V.; Highland, K.B. Systemic sclerosis-associated interstitial lung disease. Lancet Respir. Med. 2020, 8, 304–320. [Google Scholar] [CrossRef]
- Scallan, C.J.; Collins, B.F.; Raghu, G. Systemic sclerosis-associated interstitial lung disease. Curr. Opin. Pulm. Med. 2020, 26, 487–495. [Google Scholar] [CrossRef]
- Warrick, J.H.; Bhalla, M.; Schabel, S.I.; Silver, R.M. High resolution computed tomography in early scleroderma lung disease. J. Rheumatol. 1991, 18, 1520–1528. [Google Scholar]
- Hoffmann-Vold, A.-M.; Maher, T.M.; Philpot, E.E.; Ashrafzadeh, A.; Barake, R.; Barsotti, S.; Bruni, C.; Carducci, P.; Carreira, P.E.; Castellví, I.; et al. The identification and management of interstitial lung disease in systemic sclerosis: Evidence-based European consensus statements. Lancet Rheumatol. 2020, 2, E71–E83. [Google Scholar] [CrossRef]
- Ruaro, B.; Baratella, E.; Confalonieri, P.; Wade, B.; Marrocchio, C.; Geri, P.; Busca, A.; Pozzan, R.; Andrisano, A.G.; Cova, M.A.; et al. High-resolution computed tomography: Lights and shadows in improving care for SSC-ILD patients. Diagnostics 2021, 11, 1960. [Google Scholar] [CrossRef]
- Ruaro, B.; Baratella, E.; Confalonieri, P.; Confalonieri, M.; Vassallo, F.G.; Wade, B.; Geri, P.; Pozzan, R.; Caforio, G.; Marrocchio, C.; et al. High-resolution computed tomography and lung ultrasound in patients with systemic sclerosis: Which One to choose? Diagnostics 2021, 11, 2293. [Google Scholar] [CrossRef]
- Bruni, C.; Mattolini, L.; Tofani, L.; Gargani, L.; Landini, N.; Roma, N.; Lepri, G.; Orlandi, M.; Guiducci, S.; Bellando-Randone, S.; et al. Lung Ultrasound B-lines in the evaluation of the extent of interstitial lung disease in systemic sclerosis. Diagnostics 2022, 12, 1696. [Google Scholar] [CrossRef]
- Song, G.; Bae, S.C.; Lee, Y.H. Diagnostic accuracy of lung ultrasound for interstitial lung disease in patients with connective tissue diseases: A meta-analysis. Clin. Exp. Rheumatol. 2016, 34, 11–16. [Google Scholar] [PubMed]
- Xie, H.Q.; Zhang, W.W.; Sun, D.S.; Chen, X.M.; Yuan, S.F.; Gong, Z.H.; Liu, L. A simplified lung ultrasound for the diagnosis of interstitial lung disease in connective tissue disease: A meta-analysis. Arthritis Res. Ther. 2019, 21, 93. [Google Scholar] [CrossRef] [PubMed]
- McInnes, M.D.; Moher, D.; Thombs, B.D.; McGrath, T.A.; Bossuyt, P.M.; Clifford, T.; Cohen, J.F.; Deeks, J.J.; Gatsonis, C.; Hooft, L.; et al. Preferred reporting items for a systematic review and meta-analysis of Diagnostic Test Accuracy Studies. JAMA 2018, 319, 388. [Google Scholar] [CrossRef] [PubMed]
- Whiting, P.F. Quadas-2: A revised tool for the quality assessment of Diagnostic Accuracy Studies. Ann. Intern. Med. 2011, 155, 529. [Google Scholar] [CrossRef] [PubMed]
- R Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2020; Available online: https://www.R-Project.Org/ (accessed on 24 April 2020).
- Balduzzi, S.; Rücker, G.; Schwarzer, G. How to perform a meta-analysis with R: A practical tutorial. Evid.-Based Ment. Health 2019, 22, 153–160. [Google Scholar] [CrossRef]
- Philipp Doebler with contributions from Bernardo Sousa-Pinto. Mada: Meta-Analysis of Diagnostic Accuracy. 2022. Available online: https://CRAN.R-project.org/package=mada (accessed on 10 January 2023).
- Fairchild, R.; Chung, M.; Yang, D.; Sharpless, L.; Li, S.; Chung, L. Development and assessment of novel lung ultrasound interpretation criteria for the detection of interstitial lung disease in systemic sclerosis. Arthritis Care Res. 2021, 73, 1338–1342. [Google Scholar] [CrossRef]
- Gargani, L.; Bruni, C.; Romei, C.; Frumento, P.; Moreo, A.; Agoston, G.; Guiducci, S.; Bellando-Randone, S.; Lepri, G.; Belloli, L.; et al. Prognostic value of Lung Ultrasound B-lines in systemic sclerosis. Chest 2020, 158, 1515–1525. [Google Scholar] [CrossRef] [PubMed]
- Hassan, R.I.; Lubertino, L.I.; Barth, M.A.; Quaglia, M.F.; Montoya, S.F.; Kerzberg, E.; Binda, M. Del Lung ultrasound as a screening method for interstitial lung disease in patients with systemic sclerosis. JCR J. Clin. Rheumatol. 2019, 25, 304–307. [Google Scholar] [CrossRef]
- Tardella, M.; Di Carlo, M.; Carotti, M.; Filippucci, E.; Grassi, W.; Salaffi, F. Ultrasound B-lines in the evaluation of interstitial lung disease in patients with systemic sclerosis. Medicine 2018, 97, e0566. [Google Scholar] [CrossRef]
- Çakır Edis, E. Effectiveness of thoracic ultrasonography in the evaluation of the severity of pulmonary involvement in patients with systemic sclerosis. Arch. Rheumatol. 2016, 31, 364–370. [Google Scholar] [CrossRef]
- Sperandeo, M.; De Cata, A.; Molinaro, F.; Trovato, F.M.; Catalano, D.; Simeone, A.; Varriale, A.; Martines, G.F.; Trovato, G. Ultrasound signs of pulmonary fibrosis in systemic sclerosis as timely indicators for chest computed tomography. Scand. J. Rheumatol. 2015, 44, 389–398. [Google Scholar] [CrossRef]
- Mohammadi, A. Comparison of a new, modified lung ultrasonography technique with high-resolution CT in the diagnosis of the alveolo-interstitial syndrome of systemic scleroderma. Med. Ultrason. 2014, 16, 27–31. [Google Scholar] [CrossRef]
- Moazedi-Fuerst, F.C.; Kielhauser, S.; Brickmann, K.; Tripolt, N.; Meilinger, M.; Lufti, A.; Graninger, W. Sonographic assessment of interstitial lung disease in patients with rheumatoid arthritis, systemic sclerosis and systemic lupus erythematosus. Clin. Exp. Rheumatol. 2015, 33, S87–S91. [Google Scholar]
- Barskova, T.; Gargani, L.; Guiducci, S.; Randone, S.B.; Bruni, C.; Carnesecchi, G.; Conforti, M.L.; Porta, F.; Pignone, A.; Caramella, D.; et al. Lung ultrasound for the screening of interstitial lung disease in very early systemic sclerosis. Ann. Rheum. Dis. 2012, 72, 390–395. [Google Scholar] [CrossRef]
- Soldati, G. Sonographic findings in pulmonary diseases. Radiol. Med. 2006, 111, 507–515. [Google Scholar] [CrossRef]
- Tardella, M.; Gutierrez, M.; Salaffi, F.; Carotti, M.; Ariani, A.; Bertolazzi, C.; Filippucci, E.; Grassi, W. Ultrasound in the assessment of pulmonary fibrosis in connective tissue disorders: Correlation with high-resolution computed tomography. J. Rheumatol. 2012, 39, 1641–1647. [Google Scholar] [CrossRef]
- Sperandeo, M.; Rotondo, A.; Guglielmi, G.; Catalano, D.; Feragalli, B.; Trovato, G.M. Transthoracic ultrasound in the assessment of pleural and pulmonary diseases: Use and limitations. La. Radiol. Med. 2014, 119, 729–740. [Google Scholar] [CrossRef]
- Vicente-Rabaneda, E.F.; Bong, D.A.; Busquets-Pérez, N.; Moller, I. Ultrasound evaluation of interstitial lung disease in rheumatoid arthritis and autoimmune diseases. Eur. J. Rheumatol. 2022. [Google Scholar] [CrossRef]
- Mongodi, S.; De Luca, D.; Colombo, A.; Stella, A.; Santangelo, E.; Corradi, F.; Gargani, L.; Rovida, S.; Volpicelli, G.; Bouhemad, B.; et al. Quantitative Lung Ultrasound: Technical Aspects and Clinical Applications. Anesthesiology 2021, 134, 949–965. [Google Scholar] [CrossRef]
- Yan, J.-H.; Pan, L.; Gao, Y.-B.; Cui, G.-H.; Wang, Y.-H. Utility of lung ultrasound to identify interstitial lung disease. Medicine 2021, 100, e25217. [Google Scholar] [CrossRef]
- Man, M.A.; Dantes, E.; Domokos Hancu, B.; Bondor, C.I.; Ruscovan, A.; Parau, A.; Motoc, N.S.; Marc, M. Correlation between transthoracic lung ultrasound score and HRCT features in patients with interstitial lung diseases. J. Clin. Med. 2019, 8, 1199. [Google Scholar] [CrossRef]
- Gargani, L.; Romei, C.; Bruni, C.; Lepri, G.; El-Aoufy, K.; Orlandi, M.; D’Errico, L.; Bandini, G.; D’Angelo, G.; Guiducci, S.; et al. Lung Ultrasound B-lines in systemic sclerosis: Cut-off values and methodological indications for interstitial lung disease screening. Rheumatology 2022, 61, SI56–SI64. [Google Scholar] [CrossRef]
- Wang, Y.K.; Gargani, L.; Barskova, T.; Furst, D.E.; Cerinic, M.M. Usefulness of lung ultrasound B-lines in connective tissue disease-associated interstitial lung disease: A literature review. Arthritis Res. Ther. 2017, 19, 206. [Google Scholar] [CrossRef] [PubMed]

| Author and Year | Country | Sample Size (Total/Male/Female) | Age (Years) | Disease Duration (Years) | QUADAS-2 (Risk of Bias) |
|---|---|---|---|---|---|
| Fairchild et al., 2021 [16] | USA | 20/NA/NA | NA | NA | Low |
| Gargani et al., 2020 [17] | Italy | 396/31/365 | 55 (44–66) * | 4 (1–9) * | Moderate |
| Hassan et al., 2019 [18] | Argentina | 67/4/63 | 53 ± 13 ** | NA | Low |
| Tardella et al., 2018 [19] | Italy | 40/6/34 | 56.4 ± 13.42 ** | 6.5 ± 6.79 ** | Low |
| Çakır et al., 2016 [20] | Turkey | 48/2/46 | 50.8 ± 11.9 ** | NA | Moderate |
| Sperandeo et al., 2015 [21] | Italy | 175/9/166 | 46.46 ± 15.33 ** | NA | Low |
| Mohammadi et al., 2014 [22] | USA | 70/8/62 | 50.29 ± 9.7 ** | 7.33 ± 6.93 ** | Moderate |
| Moazedi-Fuerst et al., 2014 [23] | Austria | 14/NA/NA | NA | NA | Moderate |
| Barskova et al., 2013 [24] | Italy | 58/4/54 | 51 ± 14 ** | NA | Low |
| Author and Year | Number of LIS Points Assessed | LUS Criterion Used | Cut-Off Values (Total B-Lines) | Probe | TP | FP | TN | FN |
|---|---|---|---|---|---|---|---|---|
| Fairchild et al., 2021 [16] | 14 | Pleural thickening and granularity, pleural irregularity | NA | Medium-frequency linear probe | 11 | 1 | 8 | 0 |
| Gargani et al., 2020 [17] | 58 | B-lines | ≥5 | 2.5–3.5 MHz cardiac-sector transducers | 46 | 248 | 98 | 4 |
| Hassan et al., 2019 [18] | 72 | B-lines | ≥5 | Convex transducer of 3.5 MHz | 29 | 25 | 13 | 0 |
| Tardella et al., 2018 [19] | 14 | B-lines | >10 | 4–13 MHz broadband linear transducer | 26 | 1 | 12 | 1 |
| Çakır et al., 2016 [20] | 14 | B-lines | >5 | 5 to 10 MHz linear probe | 29 | 3 | 16 | 0 |
| Sperandeo et al., 2015 [21] | All | B-lines | >3 | 3.5–5-MHz convex probe | 134 | 2 | 24 | 15 |
| Mohammadi et al., 2014 [22] | 10 | B-lines | >5 | Broadband linear multifrequency transducer of 7–10 MHz | 39 | 2 | 15 | 14 |
| Moazedi-Fuerst et al., 2014 [23] | All | B-lines | >2 | 3.5 MHz convex transducer | 9 | 2 | 3 | 0 |
| Barskova et al., 2013 [24] | 72 | B-lines | >5 | 2.5–3.5 MHz cardiac sector transducer | 36 | 10 | 12 | 0 |
| Univariate Model | Bivariate Model | ||
|---|---|---|---|
| Diagnostic Accuracy (95% CI) | I2 (p-Value) | Diagnostic Accuracy (95% CI) | |
| Category of Four Studies Evaluating the Lower Number of Examined LIS Points (Below 15) | |||
| Specificity | 0.86 (0.78–0.95) | 0% (0.95) | 0.853 (0.74–0.922) |
| Sensitivity | 0.91 (0.80–1.03) | 74% (<0.01) | 0.916 (0.713–0.98) |
| DOR | 97.49 (29.67–320.38) | 100% (<0.001) | 88.7 (12.7–315) |
| AUC | / | 0.867 | |
| Category of Three Studies Evaluating the Medium Number of Examined LIS Points (Between 15 and 72) | |||
| Specificity | 0.37 (0.25–0.55) | 82% (<0.01) | 0.37 (0.246–0.513) |
| Sensitivity | 0.97 (0.93–1.01) | 15% (0.31) | 0.965 (0.856–0.992) |
| DOR | 22.40 (3.86–129.79) | 100% (<0.01) | 27.5 (2.15–125) |
| AUC | / | 0.686 | |
| Category of Two Studies That Examined All LIS Points | |||
| Specificity | 0.79 (0.52–1.18) | 60% (0.11) | 0.797 (0.364–0.964) |
| Sensitivity | 0.90 (0.86–0.95) | 0% (0.54) | 0.921 (0.826–0.966) |
| DOR | 47.64 (15.25–148.80) | 100% (<0.01) | 61.1 (10.2–204) |
| AUC | / | 0.934 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Radić, M.; Đogaš, H.; Gelemanović, A.; Jurić Petričević, S.; Škopljanac, I.; Radić, J. Pulmonary Ultrasonography in Systemic Sclerosis-Induced Interstitial Lung Disease—A Systematic Review and Meta-Analysis. Diagnostics 2023, 13, 1429. https://doi.org/10.3390/diagnostics13081429
Radić M, Đogaš H, Gelemanović A, Jurić Petričević S, Škopljanac I, Radić J. Pulmonary Ultrasonography in Systemic Sclerosis-Induced Interstitial Lung Disease—A Systematic Review and Meta-Analysis. Diagnostics. 2023; 13(8):1429. https://doi.org/10.3390/diagnostics13081429
Chicago/Turabian StyleRadić, Mislav, Hana Đogaš, Andrea Gelemanović, Slavica Jurić Petričević, Ivan Škopljanac, and Josipa Radić. 2023. "Pulmonary Ultrasonography in Systemic Sclerosis-Induced Interstitial Lung Disease—A Systematic Review and Meta-Analysis" Diagnostics 13, no. 8: 1429. https://doi.org/10.3390/diagnostics13081429





