Abstract
There is growing evidence to support change in the rehabilitation strategy of patellofemoral pain syndrome (PFPS) from traditional quadriceps strengthening exercises to inclusion of hip musculature strengthening in individuals with PFPS. Several studies have evaluated effects of quadriceps and hip musculature strengthening on PFPS with varying outcomes on pain and function. This systematic review and meta-analysis aims to synthesize outcomes of pain and function post-intervention and at follow-up to determine whether outcomes vary depending on the exercise strategy in both the short and long term. Electronic databases including MEDLINE, EMBASE, CINAHL, Web of Science, PubMed, Pedro database, Proquest, Science direct, and EBscoHost databases were searched for randomized control trials published between 1st of January 2005 and 31st of June 2015, comparing the outcomes of pain and function following quadriceps strengthening and hip musculature strengthening exercises in patients with PFPS. Two independent reviewers assessed each paper for inclusion and quality. Means and SDs were extracted from each included study to allow effect size calculations and comparison of results. Six randomized control trials met the inclusion criteria. Limited to moderate evidence indicates that hip abductor strengthening was associated with significantly lower pain post-intervention (SMD −0.88, −1.28 to −0.47 95% CI), and at 12 months (SMD −3.10, −3.71 to −2.50 95% CI) with large effect sizes (greater than 0.80) compared to quadriceps strengthening. Our findings suggest that incorporating hip musculature strengthening in management of PFPS tailored to individual ability will improve short-term and long-term outcomes of rehabilitation. Further research evaluating the effects of quadriceps and hip abductors strengthening focusing on reduction in anterior knee pain and improvement in function in management of PFPS is needed.
1. Introduction
Patello-femoral pain syndrome (PFPS) is one of the most diagnosed knee pain syndromes in paediatric physical therapy or orthopaedic outpatient clinics [1,2,3] and is thus implicated as the primary cause of knee pain in clinical settings in up to 40% of cases [4,5]. PFPS is prevalent in active young adults with a noticeable peak of prevalence in young, active adolescents between the ages of 12 and 17 years with double the annual incidence in women compared to men [1,2,3].
Diagnosis and treatment of PFPS poses a challenge in clinical practice, as its exact aetiology is unknown. However, PFPS describes anterior knee pain resulting from several intrinsic factors including increased Q-angle in the weight-bearing position, genu valgus, tibia internal rotation, patellar mal-alignment, muscular imbalance around the hip and knee joints, and over-activity [6]. Thus, diagnosis of PFPS requires exclusion of other conditions including intra-articular pathologic abnormality, plica syndromes, Osgood-Schlatter disease, neuromas, and other rare causes [6,7].
Conservative management options, which have been suggested for PFPS, include quadriceps strengthening, stretching, bracing, and patella taping although no specific intervention has been reported to be most effective in management of PFPS [8,9,10]. Quadriceps strengthening in the management of PFPS has been the focus of clinical interventions to correct patella tracking, alignment, and motion seen in PFPS thus reducing resultant increased patellar joint pressure and pain [8,10]. However, abnormal hip motion in both frontal and transverse planes due to weak hip muscles occurs in PFPS further influencing pain, knee kinematics, and function [9]. Poor eccentric hip abductors and external rotator muscle strength causes a resultant femoral adduction and medial rotation during weight-bearing activities, causing a lateral patellar tracking as the femur medially rotates beneath the patella, resulting in patellar mal-alignment [10,11].
Studies have reported that when compared to healthy controls, persons with PFPS show deficits in hip abductor, extensor, and external rotator muscle strength [12,13]. A deficit in hip abductor strength deficit compared with healthy controls of up to 14% has been reported in persons with PFP syndrome, resulting in impaired medial–lateral postural stability with diminished quantitative balance performance difference of up to 39%–45% [14]. This strength deficit plays huge biomechanical significance as seen in diminished single leg stance performance with following fatiguing of the hip abductor muscles [15] and also a reported correlation between balance performance and hip muscle abductor strength in adults [16]. The gluteus medius is an important muscle in controlling frontal-plane motion in a far reaching movement of the arm compared to ankle evertors and invertors, and as such play a significant role in maintaining normal posture in response to medial-lateral perturbations on the body [17].
The primary goals in management of PFPS, either surgical or conservative management, are the reduction in intensity of anterior knee pain, and restoration of patient optimal function (aspects of interaction between a person’s health status and their contextual factors either environmental and personal factors) [8,13]. Evaluation of pain intensity and function pre and post intervention, provides a means of determining whether goals of conservative management of PFPS are achieved and serve as a means of assessing severity of patient symptoms at different time points during the course of management [8].
Although several studies have focused on the effects of both quadriceps strengthening and hip abductor strengthening on pain, hip muscle function and functional activities in PFPS reported mixed and inconclusive results.
Therefore, this meta-analysis was aimed to:
- Determine differences in patient-reported anterior knee pain intensity in management of PFPS following quadriceps strengthening or hip abductor strengthening programs in management of PFPS.
- Determine differences in function following quadriceps strengthening or hip abductor strengthening programs in management of PFPS.
2. Materials and Methods
2.1. Type of Participants
Studies were included if they reported having both male and female participants aged 15 to 40 years with a diagnosis of PFPS by medical and radiographic examination.
2.2. Types of Studies
Studies selection was limited to randomized control trial studies to reflect the highest level of clinical research quality. All studies reported pre and post intervention data of outcomes of anterior knee pain intensity and function following quadriceps strengthening and hip abductor strengthening programs in management of PFPS.
2.3. Type of Interventions
The interventions under consideration were quadriceps strengthening alone or hip abductor and external rotator strengthening programme in management of PFPS.
2.4. Outcome Measurements
Outcome measures used in selected studies in this review to evaluate pain and function included:
- Function—Evaluated with outcome measures including lower extremity function score (LEFS), Western Ontario and McMaster Universities Arthritis Index (WOMAC), or anterior knee pain score (AKPS), which have all been consistently used in research to assess function of the lower extremity pre and post intervention in management of PFPS [8].
- Pain as measured with outcome measures including the visual analogue scale or numerical pain rating scale (0/10) which have both been consistently used in research to assess anterior knee pain intensity pre and post intervention, in management of PFPS [3,8].
Validity and Reliability of Outcome Measures
Reliability for the LEFS and AKPS has been reported to be R = 0.98 and R = 0.95 in subjects with PFPS [18]. Reliability and validity of outcome measures of pain selected for this study, including the visual analogue scale (VAS) and numerical pain rating scale (NPRS) have been described in literature.
The VAS and the NPRS compared to other pain rating tools has a better responsiveness compared to other rating tools with an inter-rater reliability of ICC = 0.76 and 0.84 respectively [3,8].
2.5. Electronic Search
An electronic online search was conducted using a systematic search strategy to identify relevant articles in electronic databases including MEDLINE, EMBASE, CINAHL, Web of Science, PubMed, Pedro database, Proquest, Science direct, and EBscoHost for studies published in English between 2008 and May 2015 to reflect current research knowledge. Key word combinations used included: patellofemoral pain syndrome, anterior knee pain, function, hip, muscle strengthening, and muscle endurance. The electronic data search was limited to randomized control trial studies only to reflect the highest level of clinical research quality included in this review. In addition, a manual searching of the references of all articles selected for the review and bibliographies of relevant texts and journals was conducted. Depositories of unpublished research were not perused and although the authors agree this may potentially lead to publication bias [19], it is impossible to exhaustively peruse all unpublished work on effects of strength training interventions associated with PFPS from all authors and institutions around the world related to this research area.
2.6. Inclusion and Exclusion Criteria
Inclusion Criteria—Studies with
- Participants aged 15–40 years.
- Comparison of pre and post intervention outcomes following quadriceps strengthening or hip abductor strengthening programs in management of PFPS including anterior knee pain and patient reported function.
- Incidence of PFPS of at-least four weeks onset. Participants had to report anterior, retro, or peri-patellar pain during at least two or three of the following provocative activities: squatting, kneeling, prolonged sitting, ascending or descending stairs, running, hopping, jumping, palpation or compression of medial or lateral patella facet, and isometric quadriceps contraction.
- Studies published between 1st of January 2005 and 31st of June 2015.
Exclusion criteria
- ○
- Studies were excluded if they reported inclusion of participants with a previous history of knee surgeries, lower limb pathology, or dysfunctions including knee/patellar osteoarthritis, bursitis, meniscal injuries and knee collateral or cruciate ligament injuries, or other pathological diseases of the knee joint.
2.7. Study Selection
Two reviewers independently performed the process of study selection based on the title and the abstract. Articles not excluded by both reviewers were assessed in full-text and disagreement regarding inclusion was resolved by consensus.
Quality Rating of Selected Studies
For studies meeting inclusion criteria, the PEDRO scale was used to appraise their methodological quality. It has a fair inter-rater agreement for individual domains and substantial agreement for the final grade in contrast to similar rating tools (ICC = 0.56–0.68) [19]. This was independently applied by two reviewers, with discrepancies resolved during a consensus meeting.
2.8. Data Abstraction
Data relating to study design, participants, PFPS definitions, and protocol for exercise intervention (frequency, intensity, type, and time) were extracted from all studies. The mean differences of pre and post intervention for anterior knee pain using the Visual Analogue Scale/Numerical Pain rating Scale were determined. Similarly, pre and post intervention mean differences of outcome measures of function of the lower extremity using the Anterior Knee Pain Scale (AKPS), Lower Extremity Function Scale (LEFS) and WOMAC (The Western Ontario and McMaster Universities Arthritis Index) questionnaires between subjects with PFPS in both quadriceps strengthening group and hip abductor and external rotator groups were extracted. If data were missing, information was requested from the authors to allow effect size (ES) calculations.
2.9. Data Analysis
The Cochrane review statistical program Revman 5.3 was used for statistical data analysis of effect size, heterogeneity, and Standard Error of Effect size estimate. Data were pooled for pain with the VAS and where studies evaluated lower extremity function, results were pooled using functional outcome measures for the lower extremity function variable. Calculated individual or pooled ES were categorised as small (=0.59), medium (0.60–1.19) or large (=1.20). The level of statistical heterogeneity for pooled data was established using the Chi2 and I2 statistics (with heterogeneity defined as p < 0.05). Thus, the summary measure of treatment effect was the between-groups difference in mean levels of post intervention pain reduction and increase in function, expressed as a standardised mean difference (SMD) using Hedges’ (adjusted) g, which includes a correction term for sample size bias [20] Statistical heterogeneity was assessed by the I2 test, which describes the percentage of variability among effect estimates beyond that expected by chance. Heterogeneity can be considered as unlikely to be important for I2 values up to 40%. In the absence of statistical heterogeneity (I2 less than or equal to 40%), individual effect sizes were combined statistically using the inverse variance random-effects method, which assumes that true effects are normally distributed [21]. Levels of evidence definitions employed in this study were as recommended by van Tulder et al. [22].
3. Results
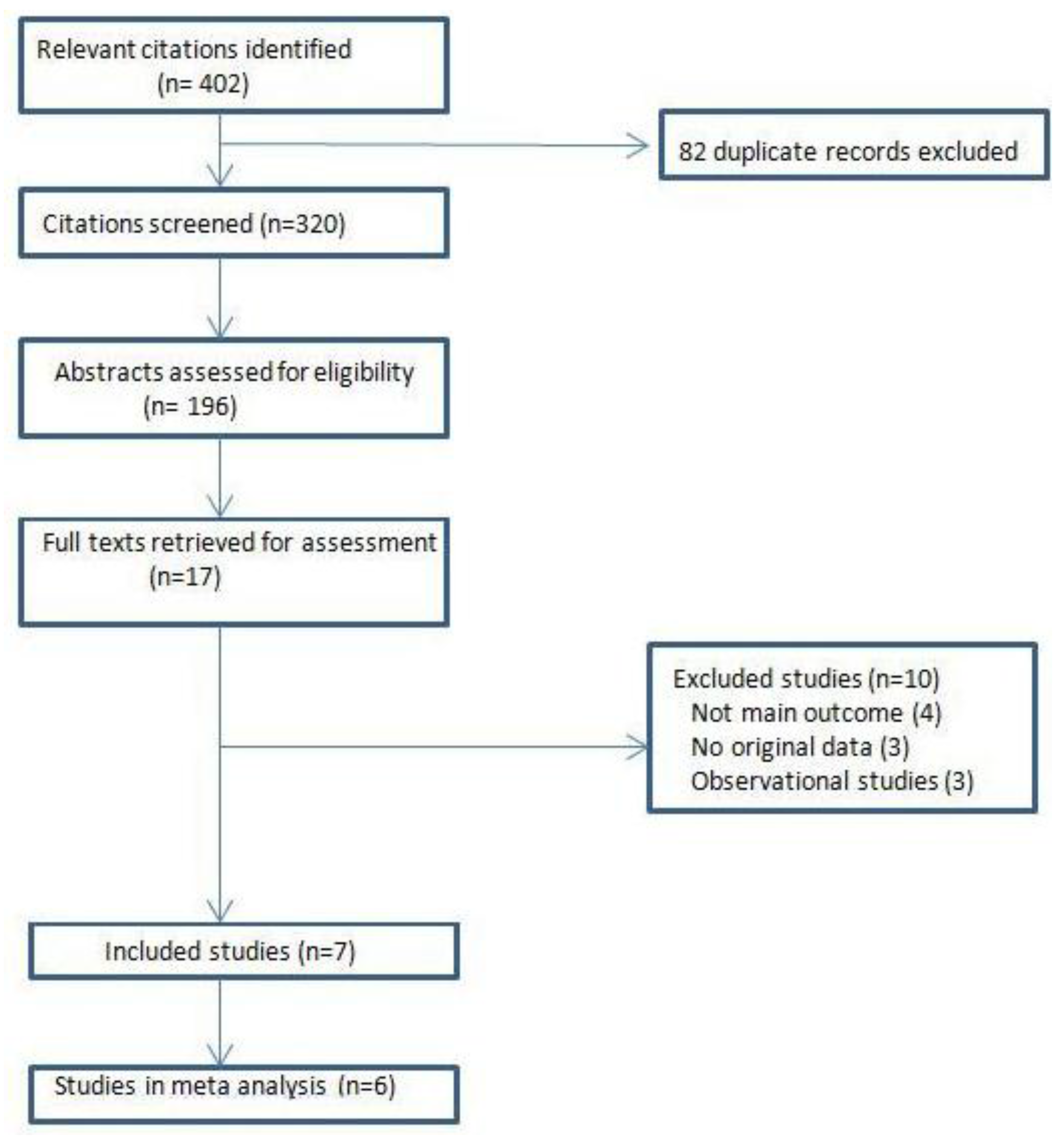
The literature search produced a total of 402 studies. Six randomized control trials met the inclusion and exclusion criteria for this review. Manual search of literature sources did not produce any additional study. The search strategy is itemized in Figure 1 below.

Figure 1.
Flow chart showing search strategy.
Figure 1.
Flow chart showing search strategy.
3.1. Study Characteristics
A total of six randomized controlled trials met the inclusion and exclusion criteria and were included in the review. All six studies [23,24,25,26,27,28] evaluated anterior knee pain intensity (VAS/NPRS 0/10) as a pre and post intervention outcome measure. A total of four studies examined function using the functional assessment tools AKPS [25,26], LEFS [25,26,28] and WOMAC [27]. All six studies randomized a total of 214 participants (89.7% female), with sample size ranging from 14 to 54 subjects. The mean age of studies populations ranged from 16 to over 40 years. Participant eligibility was determined by clinician diagnosis of PFPS of at least four weeks onset, and a fulfilment of an inclusion and exclusion criteria as itemized in Table 1. Interventions typically involved exercising for three 30-45 min sessions per week for 4-8 weeks, a range of 12–24 sessions per trial [23,24,25,26,27,28].

Table 1.
Description of Methods and characteristics of included studies with quality ratings score.
| Author | Study Population/Group Allocation | Inclusion/Exclusion Criteria | Follow up/Monitoring | Intervention Description | Pre and Post-Operative Measurements | Randomisation Process | Pedro Score (0/10) |
|---|---|---|---|---|---|---|---|
| Nagakawa et al. 2008 [23] RCT | 14 subjects (4 male; 10 females); QUADSG (7) HABLG (7) | Inclusion—Clinically diagnosed with PFP; anterior knee pain; insidious onset of pain unrelated to a traumatic incident and persistent for at least four weeks; presence of pain on palpation of the patellar facets. Exclusion—Intra-articular pathologic conditions; cruciate or collateral ligament involvement; tenderness over patellar tendon, iliotibial band, or pes anserinus tendon; patellar apprehension; Osgood-Schlatter or Sinding-Larsen-Johansson syndromes; hip or lumbar referred pain; a history of patellar dislocation; knee effusion; or previous patellofemoral joint surgery. | No follow-up period | Duration—5 sessions/week for 6 weeks, 1 supervised and 4 unsupervised weekly session. QUADSG—
HABSG—Same as QUADSG with addition of
| Pain—Worst and usual pain; Pain during stair ascending and descending (VAS) | Sealed envelope, blinded assessors, single blinded | 9 |
| Razeghi et al. 2010 [24] RCT | 32 females; mean age 22.62 ± 2.67 years (18–30); QUADSG (16) HABLG (16) | Inclusion—Clinically diagnosed with PFP; anterior knee pain; insidious onset of pain unrelated to a traumatic incident of at least four weeks onset; pain during patellar orthopaedic test or facet tenderness. Exclusion—Intra-articular pathologic conditions; cruciate or collateral ligament involvement; tenderness over iliotibial band, patella or pes anserinus tendon; patellar apprehension; Osgood-Schlatter or Sinding-Larsen-Johansson syndromes; hip or lumbar referred pain; a history of patellar dislocation; Pregnancy; history of being on a steroidal or nonsteroidal medication in last 6 months | No follow-up | Duration—4-week treatment program, supervised. QUADSG—Strengthening exercise in the control group focused only on the quadriceps muscle. The treatment program consisted of progressive resistive exercises for the hip muscles and terminal and 90° to 50° resistive knee extension and mini squat for the quadriceps. The Mc Queen progressive resistive technique was applied to increase exercise resistance. HABSG—Exercise intervention not properly described. | Usual pain measured with VAS | Random allocation | 5 |
| Fukuda et al. 2010 [25] RCT | 70 females; mean age 25 years (20–40); QUADSG (22); HABSG (23) Control group (25) | Inclusion—History of anterior knee pain of more than 3 months onset; reported pain in 2 or more daily activities; sedentary for at least the past 6 months. Exclusion—Pregnant or had any neurological disorders; hip, knee, or ankle injuries; low back or sacroiliac joint pain; rheumatoid arthritis; used corticosteroids or anti-inflammatory drugs; a heart condition that prohibited performing the exercises; or previous surgery involving the lower extremities. | No follow up | Duration—3 sessions per week for 4 weeks, totalling 12 sessions, supervised. QUADSG—
| Pain during stair ascending and descending (NPRS); Lower extremity function with LEFS and AKPS | Random allocation using opaque and sealed envelopes containing the names of the groups | 8 |
| Fukuda et al. 2012 [26] RCT | 54 females; mean age 23 years QUADSG (26); HABSG (28) | Inclusion—History of anterior knee pain of more than 3 months onset; reported pain in 2 or more daily activities; sedentary for at least the past 6 months. Exclusion—Pregnant or had any neurological disorders; hip, knee, or ankle injuries; low back or sacroiliac joint pain; rheumatoid arthritis; used corticosteroids or anti-inflammatory drugs; a heart condition that prohibited performing the exercises; or previous surgery involving the lower extremities. | 1 year | Duration—3 sessions per week for 4 weeks, totalling 12 sessions, supervised exercise sessions QUADSG—
| Pain during stair ascending and descending (NPRS); Lower extremity function with LEFS and AKPS | Random allocation using opaque and sealed envelopes containing the names of the groups | 8 |
| Khayambashis et al. 2014 [27] RCT | 36 (18 male; 18 female); mean age 27.3 ± 7 years (19–35 years); QUADSG (18) HABSG (18) | Inclusion—Unilateral or bilateral PFP diagnosed by a physician. Exclusion—Ligamentous laxity; meniscal injury; pes anserine bursitis; iliotibial band syndrome; patella tendinitis; or a history of patella dislocation, patella fracture, knee surgery or symptoms that had been present for ≤6 months. | 6 months | Duration—3 sessions/week for 8 weeks totalling 24 sessions; 3 sets, 20–25 reps/set, supervised exercise sessions. QUADSG—
| Usual pain (VAS); Lower extremity function (WOMAC). | Controlled clinical trial | 5 |
| Doldak et al. 2011 [28] RCT | 33 females; aged 16–35 years; QUADSG (16) HABSG (17) | Inclusion—Clinically diagnosed with PFP; anterior knee pain; insidious onset of pain unrelated to a traumatic incident of at least four weeks onset; pain during patellar orthopaedic test or facet tenderness. Exclusion—Symptoms present for less than one month; self-reported other knee pathology; history of knee surgery within the last year; a self-reported history of patella dislocations or subluxations; and other concurrent significant injury affecting the lower extremity. | No follow up | Duration—8 weeks, 3 sessions per week. 1 supervised, 2 unsupervised at home (3 sets/10 reps). 1st rehabilitation phase—4 weeks HABSG—
| Usual pain (VAS), Lower extremity function with LEFS. | Participants were randomly assigned to a hip strengthening program (hip group) or a quadriceps strengthening program (quad group) for 4 weeks. | 6 |
In three of the six studies, [23,25,26] the hip abductor strengthening group (HABSG) performed both hip abductor, external rotator, and quadriceps muscle strengthening exercises, while the quadriceps strengthening group (QUADSG) performed quadriceps muscle strengthening exercises alone. In the other three studies [24,27,28], the hip abductor strengthening group performed hip abductor and external rotator strengthening exercises alone, while subjects in the quadriceps strengthening group performed quadriceps strengthening exercises alone.
In four studies, all subjects performed stretching exercises as part of their exercise intervention sessions in both hip abductor strengthening groups and quadriceps strengthening groups [23,24,25,28], while stretching was not performed in the other two trials [26,27]. In two studies, all weekly exercise sessions were performed in a rehabilitation setting and supervised by the investigator [24,25,26,27] while in the other two of the studies [23,28], one out of five session weekly sessions [23] and one out of three weekly sessions [28] were supervised in the clinic by the investigator while all other sessions were performed by the subject at home unsupervised (Table 1). Only two of the six studies [26,27] reported a post-intervention follow-up period (6 and 12 months respectively).
3.2. Effect of Hip Abductor and Quadriceps Strengthening Exercise on Anterior Knee Pain
Post Intervention: The point estimate of effect size for each study indicated a greater reduction in PFPS amongst subjects in the hip abductor and external rotator muscle strengthening group compared with subjects in the quadriceps muscle strengthening groups post intervention (Figure 2). In four out of six trials [23,24,26,27] the post intervention difference in intensity of anterior knee pain was statistically significant between both groups (p < 0.05). One study reported non-statistically significant differences in post intervention usual pain [28] and in ascending pain post intervention [25]. In the presence of statistical heterogeneity (I2 greater or equal to 40%), individual effect sizes could not be combined statistically using the inverse variance random-effects method, which assumes that true effects are not normally distributed. Synthesis of data showed evidence of high statistical heterogeneity (I2 = 78%, p < 0.05), and therefore effect size estimates from the three subgroups (usual pain, pain during ascending stairs, and descending stairs) could not be pooled (Figure 2).
However, from results of analysis of overall pain, focusing on usual pain as a subgroup of overall pain, analysis of estimates of effect sizes of usual pain intensity from four studies [23,24,27,28] indicated that there is moderate evidence showing that the hip abductor strengthening group compared to the quadriceps strengthening alone in management of PFPS resulted in more significant reduction in usual pain (I2 = 28%, p = 0.24) with a medium pooled ES (SMD −0.88, −1.28 to −0.47 95% CI) (Figure 2).
Six months follow up: In the presence of statistical heterogeneity (I2 = 67%), effect size estimates could not be pooled statistically. However, sub group analysis of inverse variance random effects showed an increase in effect size at six months follow-up from post-intervention levels between both groups in usual pain intensity (−0.87 to −1.43), during stair ascending (SMD −1.12 to −2.65 95% CI), and stair descending (SMD −1.09 to −2.50 95% CI) (Figure 3).
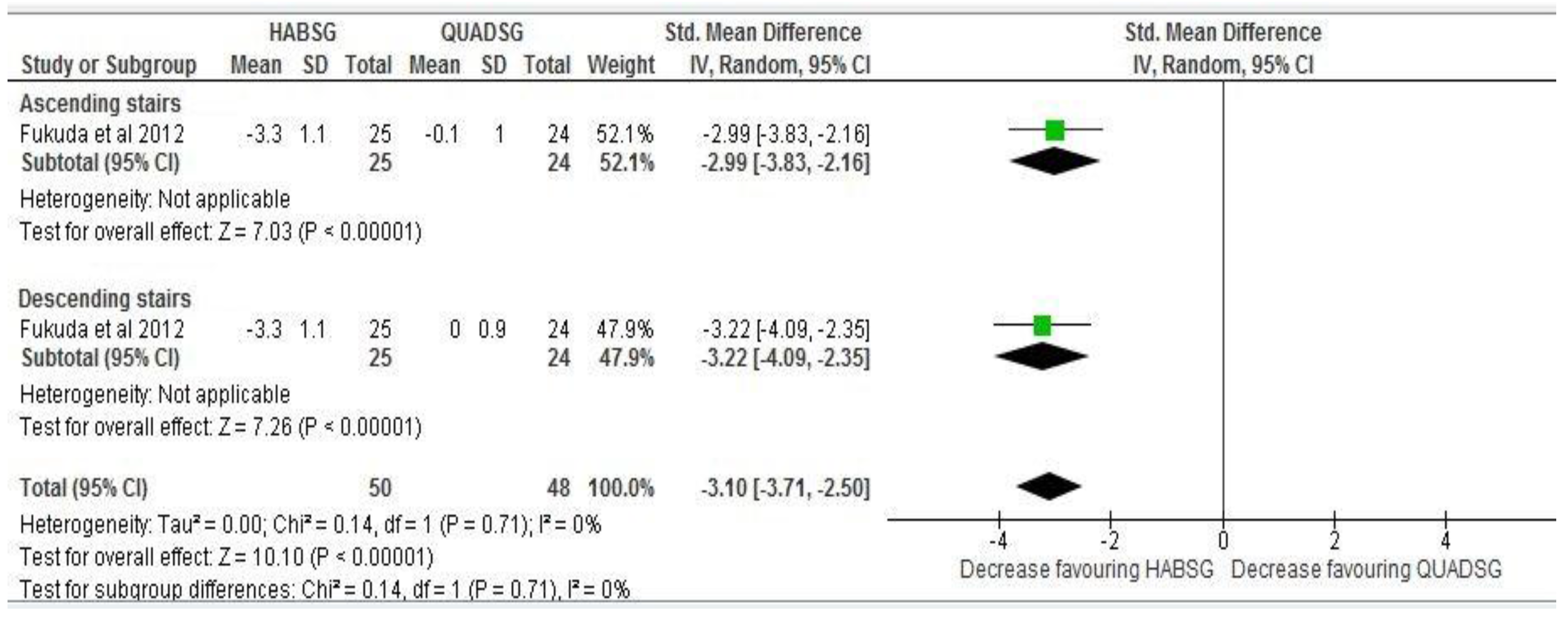
Twelve months follow up: In the absence of statistical heterogeneity (I2 = 0%, p = 0.07), synthesis of data at 12 months follow up from one high quality study [26] shows limited evidence for significant differences in pain reduction between both the hip abductor strengthening group and the quadriceps strengthening group at six months follow-up with no evidence of statistical heterogeneity among the pooled estimates and a large pooled effect size (SMD −3.10, −3.71 to −2.50 95% CI) (Figure 4). However, sub group analysis of inverse variance random effects showed a more significant increase in effect size estimates at 12 months follow-up between both groups in pain intensity during stair ascending (SMD −2.65 to −2.99 95% CI) and stair descending (SMD −2.50 to −3.22 95% CI) (Figure 4).

Figure 2.
Post intervention: Effect size comparison and estimate of anterior knee pain intensity measured a 10 point visual analogue scale (VAS) and numerical pain rating scale (NPRS) (0/10) in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
Figure 2.
Post intervention: Effect size comparison and estimate of anterior knee pain intensity measured a 10 point visual analogue scale (VAS) and numerical pain rating scale (NPRS) (0/10) in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
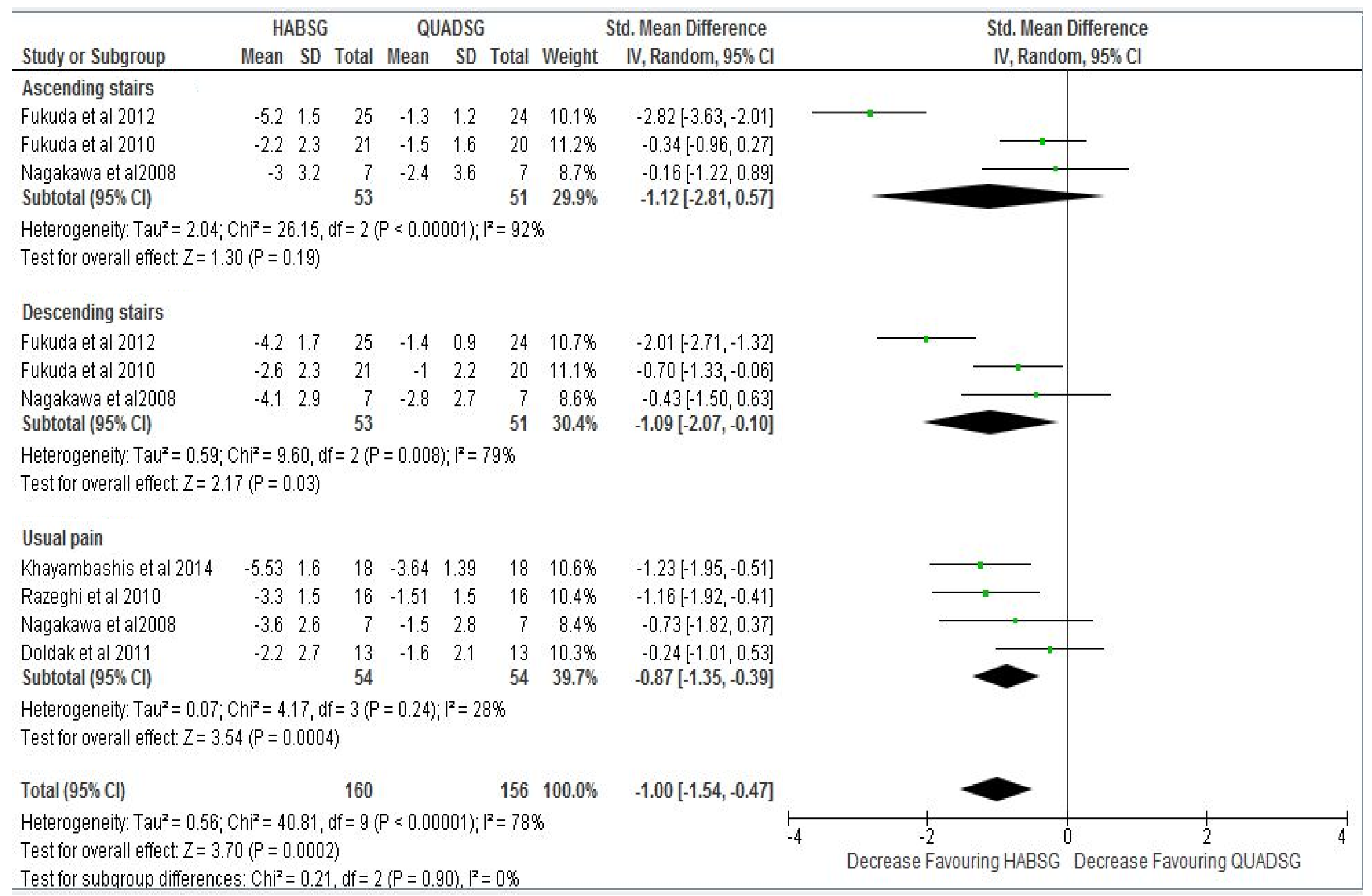

Figure 3.
At six months follow-up: Effect size comparison and estimate of anterior knee pain intensity measured with a 10 point visual analogue scale/NPRS (0/10) in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
Figure 3.
At six months follow-up: Effect size comparison and estimate of anterior knee pain intensity measured with a 10 point visual analogue scale/NPRS (0/10) in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
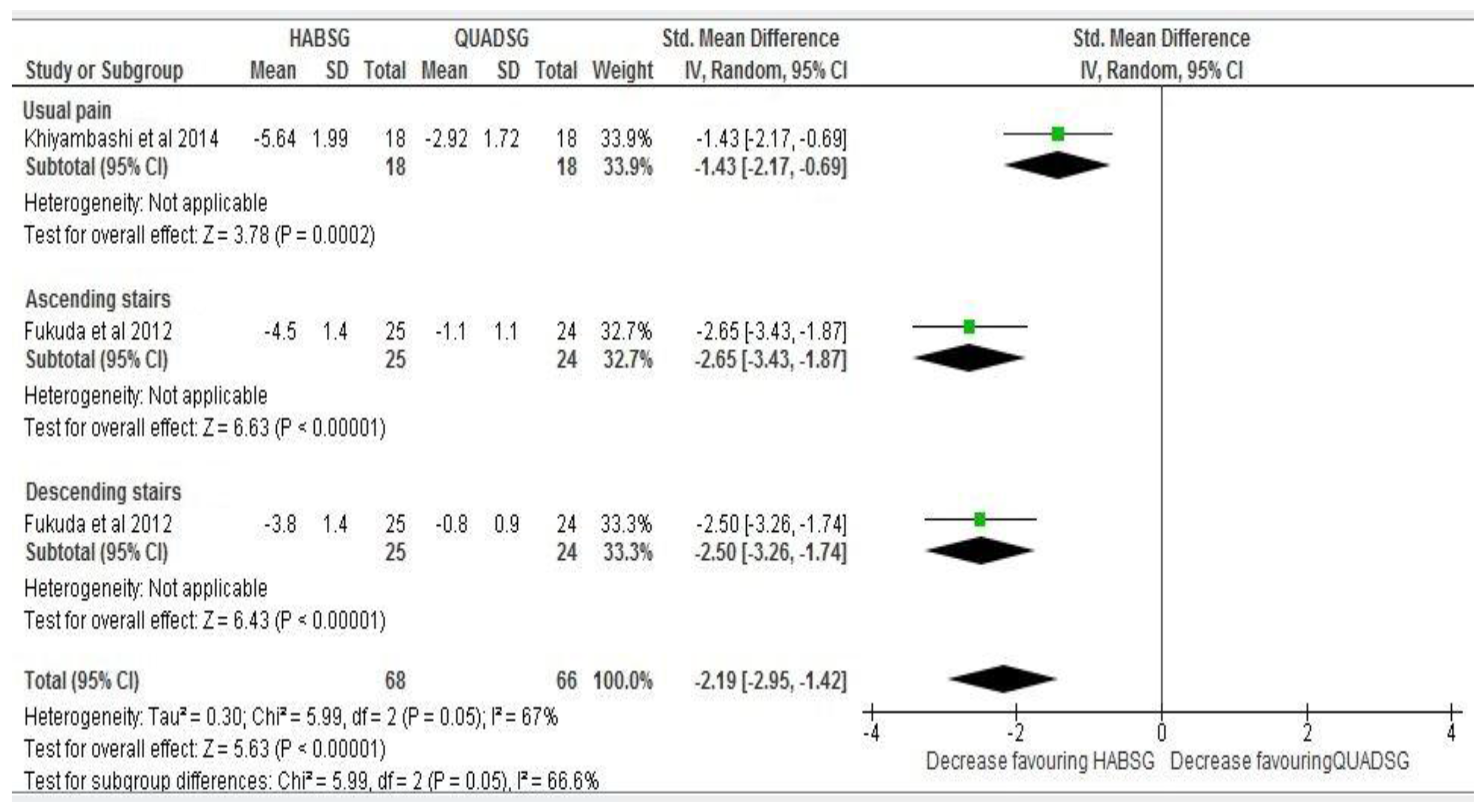

Figure 4.
At 12 months follow-up: Effect size comparison and estimate of anterior knee pain intensity measured with a 10 point VAS/NPRS (0/10) in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
Figure 4.
At 12 months follow-up: Effect size comparison and estimate of anterior knee pain intensity measured with a 10 point VAS/NPRS (0/10) in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
3.3. Effect of Hip Abductor and Quadriceps Strengthening Exercise on Function
Post intervention: Four trials evaluated function pre and post intervention. The point estimate of effect size of each study [25,26,27] excluding Doldak et al. [28] indicated a greater increase in function amongst subjects in the hip abductor strengthening group compared with subjects in the quadriceps muscle strengthening group. Contrastingly, Doldak et al. [28] showed a point estimate of effect size indicating a greater increase in function post-intervention in the quadriceps strengthening group compared to the hip abductor strengthening group (Figure 5). In two out of four studies [26,27] the post intervention differences in increased function between both groups were statistically significant and non-significant in the other two studies [25,28] (p < 0.05) (Figure 5). Synthesis of data showed evidence of high statistical heterogeneity (I2 = 87%, p < 0.05), and therefore effect sizes from the three subgroups (LEFS, AKPS and WOMAC) could not be pooled for further analysis.

Figure 5.
Post intervention: Effect size comparison of estimates of Function in subjects with Patellofemoral pain in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
Figure 5.
Post intervention: Effect size comparison of estimates of Function in subjects with Patellofemoral pain in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
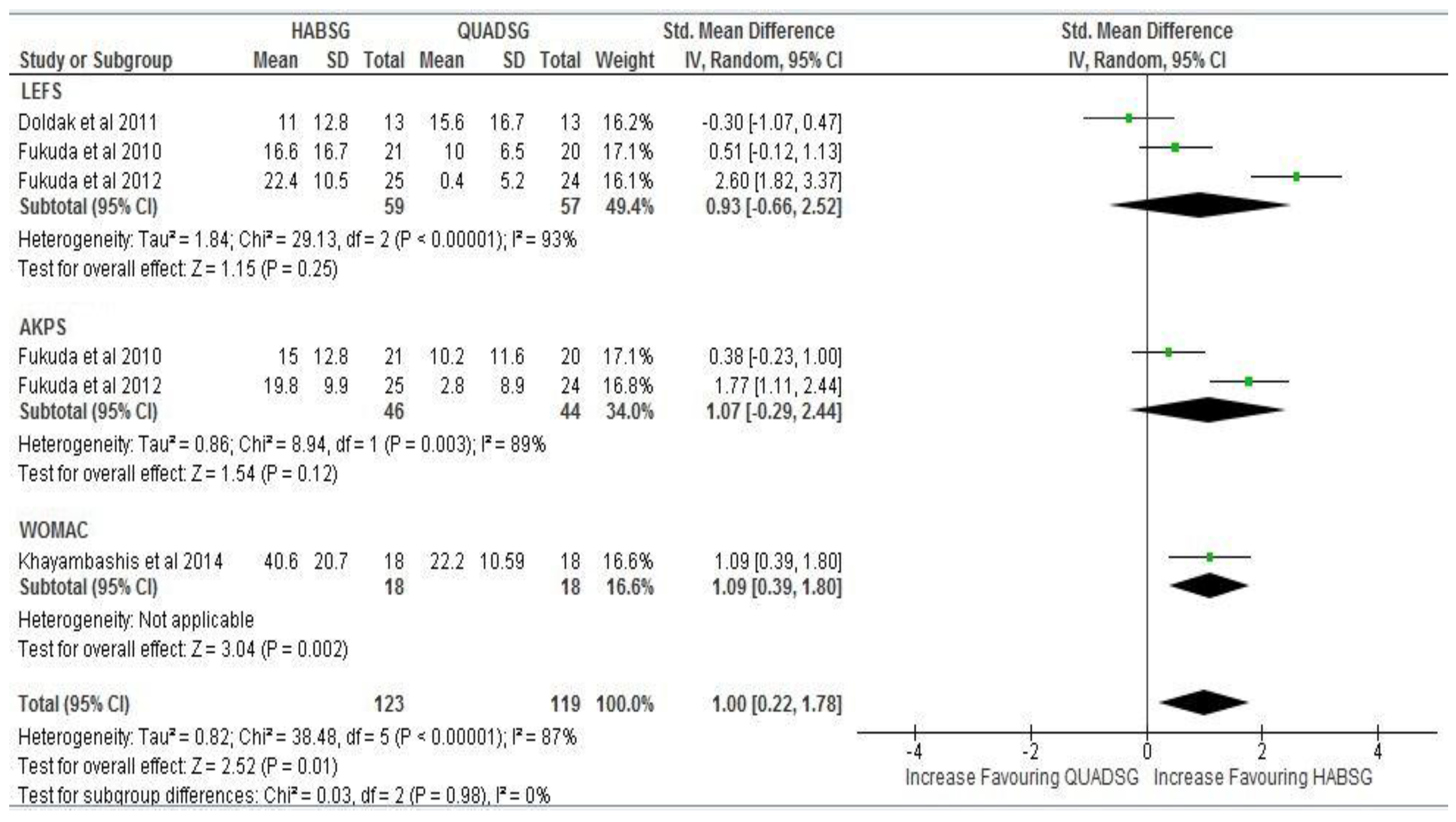
Six months follow up: Due to high statistical heterogeneity (I2 = 66%, p = 0.05) individual effect sizes could not be combined statistically assuming that true effects are not normally distributed. Therefore, ES estimates from the three subgroups (LEFS, AKPS and WOMAC) could not be pooled (Figure 6). However, sub group analysis showed a more significant increase in effect size estimates (SMD) of function at six months follow-up from post-intervention levels between both groups in LEFS (SMD 0.99 to 2.49 95% CI); AKPS (SMD 1.07 to 1.86 95% CI); WOMAC (SMD 1.09 to 1.20 95% CI) (Figure 6).

Figure 6.
At six months follow-up: Effect size comparison of estimates of Function in subjects with patellofemoral pain in both Hip strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
Figure 6.
At six months follow-up: Effect size comparison of estimates of Function in subjects with patellofemoral pain in both Hip strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
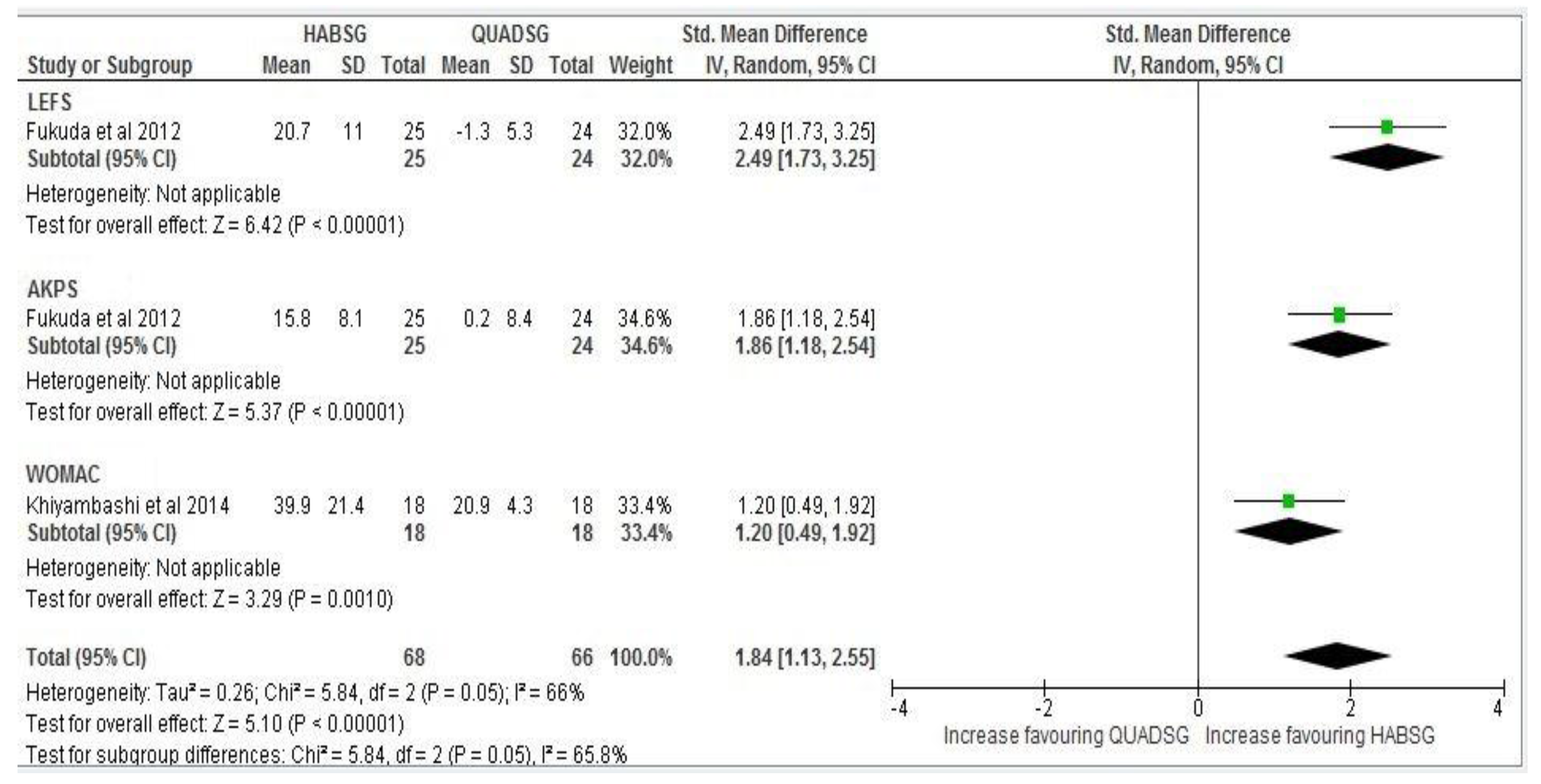
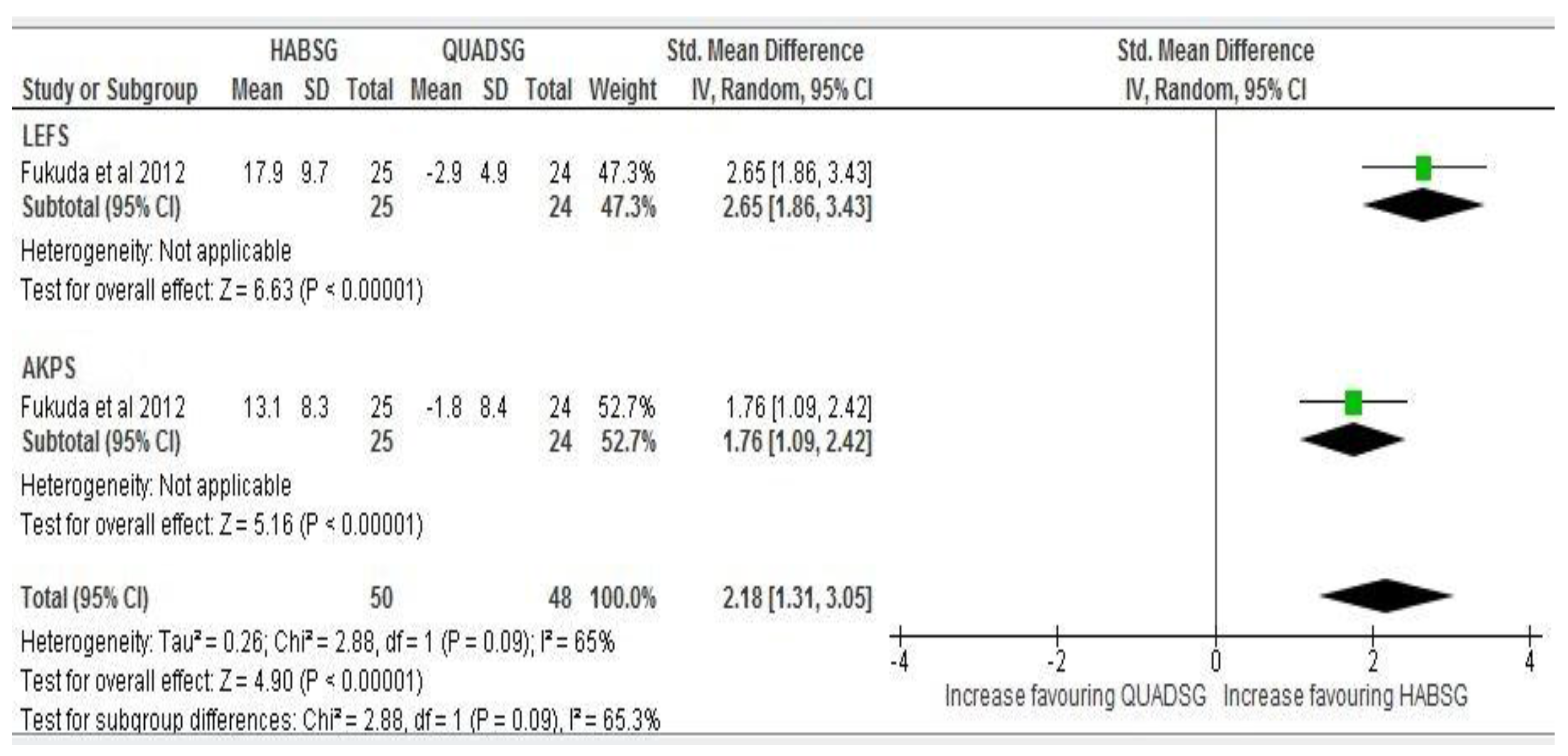
Twelve months follow up: Due to high statistical heterogeneity (I2 = 65%, p = 0.05) individual effect sizes could not be combined, assuming that true effects are not normally distributed. Results from only one high quality study [26] showed a more significant increase in effect size estimates of function at from six to 12 months follow-up levels between both groups in LEFS (SMD 2.49 to 2.65 95% CI) and a slight decrease in AKPS (SMD 1.86 to 1.76 95% CI) (Figure 7).

Figure 7.
At 12 months follow-up: Effect size comparison and estimate of Function in subjects with patellofemoral pain in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
Figure 7.
At 12 months follow-up: Effect size comparison and estimate of Function in subjects with patellofemoral pain in both Hip abductor strengthening group (HABSG) and Quadriceps strengthening group (QUADSG).
4. Discussion
The aim of this meta-analysis was to compare effects of hip abductor strengthening and quadriceps strengthening in management of PFPS. Results from individual studies indicated significant differences in usual pain intensity post intervention, and pain and function at six and 12 months follow-up with large effect sizes. However, these post intervention differences were not consistent in their level of statistical significances across all studies and tasks with high statistical heterogeneity of data during synthesis. While attempting to identify methodological differences to explain this disparate finding, one possible explanation could be because PFPS diagnosis is based on a group of symptoms and not a specific test. And although inclusion and exclusion criteria were similar, they differed between studies with some variability in terms of localization, onset of pain and pre-intervention level of function of subjects meeting eligibility criteria for inclusion across studies. In two studies [23,28] onset of PFPS as an inclusion criteria of participants was minimum of four weeks onset of PFPS while the four remaining studies [24,25,26,27] reported an inclusion criteria of a minimum of six months onset of PFPS (Table 1).
Due to high level of statistical heterogeneity, outcomes of overall pain post-intervention and at six months follow-up and function post intervention and at six months and 12 months follow-up were not pooled. Thus, individual effect sizes could not be combined statistically using the inverse variance random-effects method, assuming that true effects were not normally distributed across studies.
4.1. Anterior Knee Pain
Post intervention, effect sizes were medium-to-strong, indicating that the hip strengthening group demonstrated greater improvements in usual pain post intervention (Figure 2) and overall pain at 12 months follow-up (Figure 4) compared with the quadriceps strengthening group. Moderate evidence indicates that usual pain was significantly reduced in the hip abductor strengthening group compared to the quadriceps strengthening group with a moderate effect size (SMD −0.88, −1.28 to −0.47 95% CI) immediately post-intervention (analysis of a total of 108 subjects). While hip abductor strengthening exercises and quadriceps strengthening exercises reduced usual pain intensity post-intervention, there was a significant difference in the magnitude of this post-intervention usual pain reduction between both groups, with far greater pain reduction in the hip abductor strengthening groups.
At 12 months follow-up for overall pain, analysis of data (a total of 49 subjects) showed a large pooled effect size (SMD −3.10, −3.71 to −2.50 95% CI). This increased effect size estimate compared to post intervention effect sizes between both groups may be explained as a consequence of a gradual increase in overall pain post-intervention in the quadriceps strengthening group. Low evidence indicates an increased reduction in overall pain in the hip abductor strengthening group compared to the quadriceps strengthening group at 12 months follow up.
4.2. Function
Results show that the hip abductor strengthening groups showed a greater increase in function post-intervention and at six and 12 months follow-up compared to the quadriceps strengthening groups according to point estimates of effect sizes across subgroups for LEFS, AKPS [25,26,28] and WOMAC [27]. However, the magnitude of effect sizes of function between both groups became more significant at six and 12 months follow-up compared to post intervention estimates. This may be explained to be as a result of a noticeable steady decline in function in the quadriceps strengthening groups compared to the hip abductor strengthening group from post intervention levels, widening the point estimates of effect size between groups in the long term as seen from the results. Overall estimates of function could not be pooled due to heterogeneity of effect size estimates across studies. Although individual studies report increased function post intervention, no evidence exists due to statistical heterogeneity of outcomes reported.
A recently published study by Regelski et al. (2015) [29] reported similar outcomes post intervention and at follow-up by interpreting pooled effect sizes of individual studies post-intervention and at follow-up where applicable. However, they did not provide a clear interpretation of data as they did not perform further analysis with pooling and synthesis of data with recommendations made from effect sizes from individual studies.
4.3. Exercise Interventions
Changes in lower limb kinetics and kinematics occur in PFPS with weakness of hip muscles, a clinical finding in PFPS, associated with changes in hip and knee joint kinematics in PFPS [8,9,10]. Incorporating hip musculature strengthening (abductors and external rotator) into rehabilitation programs in management of PFPS may increase patient function and reduce severity of PFPS symptoms [23]. Amongst included trials, there were similarities in hip strengthening and quadriceps protocols with regards to exercise frequency: three sessions weekly for four weeks [24,25,26,28]. Two studies, Khayambashi et al. [27] and Nakagawa et al. [23] required patients to perform exercises three times per week for eight weeks and five times per week for six weeks, respectively. However, the types of exercises performed varied across studies. Apart from the study by Razeghi et al. [24] where exercise protocol was not properly described, five studies incorporated stretching of the hamstrings, quadriceps, and triceps surae as part of the PFPS protocols and used side-lying hip abduction in the hip strengthening protocol [23,25,26,27,28].
Standing hip abduction exercise was performed in three studies [25,26,28] while three studies [25,26,27] progressed hip abduction exercises in side-lying and standing by incorporating use of an elastic band. Four studies performed strengthening of the hip external rotation in sitting with or without the use of an elastic band [25,26,27,28]. Dolak et al. [28] and Nakagawa et al. [23] combined hip abduction and external rotation in side-lying to strengthen both abductors and external rotators. With reference to exercise types, Nakagawa et al. [23] used isometric exercises while the other five studies used isotonic exercises.
While there is no evidence of effects of different quadriceps strengthening and hip abductor strengthening exercise protocols influencing rehabilitation outcomes in management of PFPS, there is a possibility that this may have contributed to the high heterogeneity of pooled data across studies included in this review.
4.4. Strengths and Limitations and Recommendations
Strengths of this study include synthesis of homogenous data only where data are assumed to reflect similar effects across studies and are normally distributed. Therefore, this review not only provides data crucial to healthcare decision-making, such as uptake of hip strengthening exercise in rehabilitation strategies for PFPS, but data that are derived from trials conducted under conditions that most closely match the context of usual healthcare practice.
Limitations of this review include inclusion of a small number of studies as only the six included RCTs met the inclusion criteria. Additionally, as a result of the high heterogeneity of pooled data (I2 greater or equal to 40%), further analysis of pooled data for overall pain post-intervention and function post-intervention and at follow-up could not be made. Future studies should systematically homogenize participant’s eligibility criteria for selection of patients with PFPS to improve the quality research and consistency of outcomes in management of PFPS. While methodological quality across all studies was moderate to high with the Pedro scale, only one of the studies stated that the assessors responsible for collecting baseline and post-intervention outcomes were blinded to group assignment. Heterogeneity of reported outcomes in research on PFPS is too large to allow a clinically and scientifically sound meta-analysis of data. Better designed studies should be conducted considering limitations of currently existing studies.
In addition, valid and reliable scales, responsive to PFPS specifically, like the anterior knee pain scale (AKPS) (also known as the Kujula scale) was used by only two of the included studies [25,26]. The systematic use of the AKPS in studies on PFPS could allow optimal comparability between participants. PFPS is a multifactorial and complex condition and it is evident that the target population is often heterogeneous and thus could be separated in subgroups. Also, similarities and variances in exercise protocols provide a strong basis to incorporate a standardised exercise protocol and regimen for hip abductor or quadriceps strengthening exercises in conservative management of PFPS to aid future research into this condition.
5. Conclusions
Although results indicate that quadriceps strengthening may also reduce intensity of usual pain post-intervention, for greater significant post-intervention and clinically beneficial long-term outcomes, hip strengthening should be the preferred treatment approach for management of PFPS. However, there is currently low to moderate quality evidence to support this recommendation. Future studies should seek development of eligibility criteria/PFPS subject checklists for inclusion of subjects into studies on PFPS, and also take into consideration limitations of current studies so as to minimize, to the barest minimum, heterogeneity of outcomes from studies on PFPS.
Acknowledgments
The authors wish to acknowledge the authors of studies included in this review and authors who provided requested original data. We also acknowledge the staff at the Outpatient clinic, University of Potsdam.
Author Contributions
Adebisi Bisi-Balogun was tasked with preparation and finalisation of manuscript; statistical data analysis and interpretation of the results. Both authors conducted the electronic search process; quality ratings of the methodological process of included studies; data abstraction and revision of manuscript.
Conflicts of Interest
The author declares no conflicts of interest.
References
- Boling, M.; Padua, D.; Marshall, S.; Guskiewicz, K.; Pyne, S.; Beutler, A. Gender differences in the incidence and prevalence of patellofemoral pain syndrome. Scand. J. Med. Sci. Sports 2010, 20, c723–c730. [Google Scholar] [CrossRef] [PubMed]
- Blond, L.; Hansen, L. Patellofemoral pain syndrome in athletes: A 5.7-year retrospective follow-up study of 250 athletes. Acta Orthop. Belg. 1998, 644, 393–400. [Google Scholar]
- Callaghan, M.J.; Selfe, J. Has the incidence or prevalence of patellofemoral pain in the general population in the United Kingdom been properly evaluated? Phys. Ther. Sport 2007, 81, 37–43. [Google Scholar] [CrossRef]
- Wood, L.; Muller, S.; Peat, G. The epidemiology of patellofemoral disorders in adulthood: A review of routine general practice morbidity. Prim. Health Care Res. Dev. 2011, 122, 157–164. [Google Scholar] [CrossRef] [PubMed]
- Witvrouw, E.; Callaghan, M.J.; Stefanik, J.J.; Noehren, B.; Bazett-Jones, D.M.; Willson, J.D.; Earl-Boehm, J.E.; Davis, I.S.; Powers, C.M.; McConnell, J.; et al. Patellofemoral pain: Consensus statement from the 3rd International Patellofemoral Pain Research Retreat held in Vancouver, 2013. Br. J. Sports Med. 2014, 48, 411–414. [Google Scholar] [CrossRef] [PubMed]
- Thomee, R.; Augustsson, J.; Karlsson, J. Patellofemoral pain syndrome: A review of current issues. Sports Med. 1999, 284, 245–262. [Google Scholar] [CrossRef]
- Lankhorst, N.E.; Bierma-Zeinstra, S.; van Middelkoop, M. Factors associated with patellofemoral pain syndrome: A systematic review. Br. J. Sports Med. 2013, 47, 193–206. [Google Scholar] [CrossRef] [PubMed]
- Rothermich, M.; Glaviano, N.; Li, J.; Hart, J. Patellofemoral Pain Epidemiology, Pathophysiology, and Treatment Options. Clin. Sports Med. 2015, 34, 313–327. [Google Scholar] [CrossRef] [PubMed]
- Mascal, C.L.; Landel, R.; Powers, C. Management of patellofemoral pain targeting hip, pelvis, and trunk muscle function: 2 case reports. J. Orthop. Sports Phys. Ther. 2003, 33, 647–660. [Google Scholar] [CrossRef] [PubMed]
- Powers, C.M.; Ward, S.R.; Fredericson, M.; Guillet, M.; Shellock, F.G. Patellofemoral kinematics during weight-bearing and non-weight-bearing knee extension in persons with lateral subluxation of the patella: A preliminary study. J. Orthop. Sports Phys. Ther. 2003, 33, 677–685. [Google Scholar] [CrossRef] [PubMed]
- Ferber, R.; Davis, I.M.; Williams, D.S., III. Gender differences in lower extremity mechanics during running. Clin. Biomech. 2003, 18, 350–357. [Google Scholar] [CrossRef]
- Bolgla, L.A.; Malone, T.R.; Umberger, B.R.; Uhl, T.L. Hip strength and hip and knee kinematics during stair descent in females with and without patellofemoral pain syndrome. J. Orthop. Sports Phys. Ther. 2008, 381, 12–18. [Google Scholar] [CrossRef] [PubMed]
- Cichanowski, H.R.; Schmitt, J.S.; Johnson, R.J.; Niemuth, P.E. Hip strength in collegiate female athletes with patellofemoral pain. Med. Sci. Sports Exerc. 2007, 398, 1227–1232. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.; Souza, R.; Powers, C. The influence of hip abductor muscle performance on dynamic postural stability in females with patellofemoral pain. Gait Posture 2012, 36, 425–429. [Google Scholar] [CrossRef] [PubMed]
- Gribble, P.A.; Hertel, J. Effect of hip and ankle muscle fatigue on unipedal postural control. J. Electromyogr. Kinesiol. 2004, 146, 641–646. [Google Scholar] [CrossRef] [PubMed]
- Chang, S.H.; Mercer, V.S.; Giuliani, C.A.; Sloane, P.D. Relationship between hip abductor rate of force development and mediolateral stability in older adults. Arch. Phys. Med. Rehabil. 2005, 869, 1843–1850. [Google Scholar] [CrossRef] [PubMed]
- Winter, D.A.; Prince, F.; Frank, J.S.; Powell, C.; Zabjek, K.F. Unified theory regarding A/P and M/L balance in quiet stance. J. Neurophysiol. 1996, 756, 2334–2343. [Google Scholar]
- Watson, C.J.; Propps, M.; Ratner, J.; Zeigler, D.L.; Horton, P.; Smith, S.S. Reliability and responsiveness of the lower extremity functional scale and the anterior knee pain scale in patients withanterior knee pain. J. Orthop. Sports Phys. Ther. 2005, 35, 136–146. [Google Scholar] [CrossRef] [PubMed]
- Maher, C.; Sherrington, C.; Herbert, R.D.; Moseley, A.M.; Elkins, M. Reliability of the PEDro Scale for Rating Quality of Randomized Controlled Trials. Phys. Ther. 2003, 838, 713–721. [Google Scholar]
- Higgins, J.P.T.; Green, S. Cochrane Handbook for Systematic Reviews of Interventions (V5.0.2); The Cochrane Collaboration: London, UK, 2009. [Google Scholar]
- Hedges, L.V.; Vevea, J.L. Fixed and random effects models in meta-analysis. Psychol. Methods 1998, 3, 486–504. [Google Scholar] [CrossRef]
- Van Tulder, M.; Furlan, A.; Bombardier, C.; Bouter, L.; Editorial Board of the Cochrane Collaboration Back Review Group. Updated method guidelines for systematic reviews in the Cochrane collaboration back review group. Spine 2003, 28, 1290–1299. [Google Scholar] [CrossRef] [PubMed]
- Nakagawa, T.; Batista Muniz, T.; Marche, R.; Menezes Reiff, R.; Serra, F. The effect of additional strengthening of hip abductor and lateral rotator muscles in patellofemoral pain syndrome: A randomized controlled pilot study. Clin. Rehabil. 2008, 22, 1051–1060. [Google Scholar] [CrossRef] [PubMed]
- Razeghi, M.; Etemadi, Y.; Taghizadeh, Sh.; Ghaem, H. Could Hip and Knee Muscle Strengthening Alter the Pain Intensity in Patellofemoral Pain Syndrome? Iran. Red Crescent Med. J. IRCMJ 2010, 122, 104–110. [Google Scholar]
- Fukuda, T.; Rossetto, F.; Magalhães, E.; Fernandes Bryk, F.; Lucareli, P.R.; Carvalho, N. Short-Term Effects of Hip Abductors and Lateral Rotators Strengthening in Females with Patellofemoral Pain Syndrome: A Randomized Controlled Clinical Trial. J. Orthop. Sports Phys. Ther. 2010, 40, 736–740. [Google Scholar] [CrossRef] [PubMed]
- Fukuda, T.; Pagotti Melo, W.; Zaffalon, B.; Rossetto, F.; Magalhães, E.; Fernandes Bryk, F.; Martin, R. Hip Posterolateral Musculature Strengthening in Sedentary Women with Patellofemoral Pain Syndrome: A Randomized Controlled Clinical Trial with 1-Year Follow-up. J. Orthop. Sports Phys. Ther. 2012, 42, 823–830. [Google Scholar] [CrossRef] [PubMed]
- Khayambashi, K.; Fallah, A.; Movahed, A.; Bagwell, J.; Power, C. Posterolateral Hip Muscle Strengthening Versus Quadriceps Strengthening for Patellofemoral Pain: A Comparative Control Trial. Arch. Phys. Med. Rehabil. 2014, 95, 900–907. [Google Scholar] [CrossRef] [PubMed]
- Dolak, D.; Silkman, C.; Mckeon, M.J.; Hosey, R.; Lattermann, C.; Uhl, T. Hip Strengthening Prior to Functional Exercises Reduces Pain Sooner than Quadriceps Strengthening in Females with Patellofemoral Pain Syndrome: A Randomized Clinical Trial. J. Orthop. Sports Phys. Ther. 2011, 418, 23–32. [Google Scholar] [CrossRef] [PubMed]
- Regelski, C.; Ford, B.; Hoch, M. Hip Strengthening Compared with Quadriceps Strengthening in Conservative Treatment of Patients with Patellofemoral Pain: A Critically Appraised Topic. Int. J. Athl. Ther. Train. 2015, 20, 4–12. [Google Scholar] [CrossRef]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
