Impact of Smoking Cessation and Charlson Comorbidity Index on Influenza Vaccination Efficacy in COPD Patients
Abstract
1. Introduction
2. Method
2.1. Charlson Comorbidity Index (CCI)
2.2. Influenza Vaccine
2.3. Smoking Cessation
2.4. Statistical Analysis
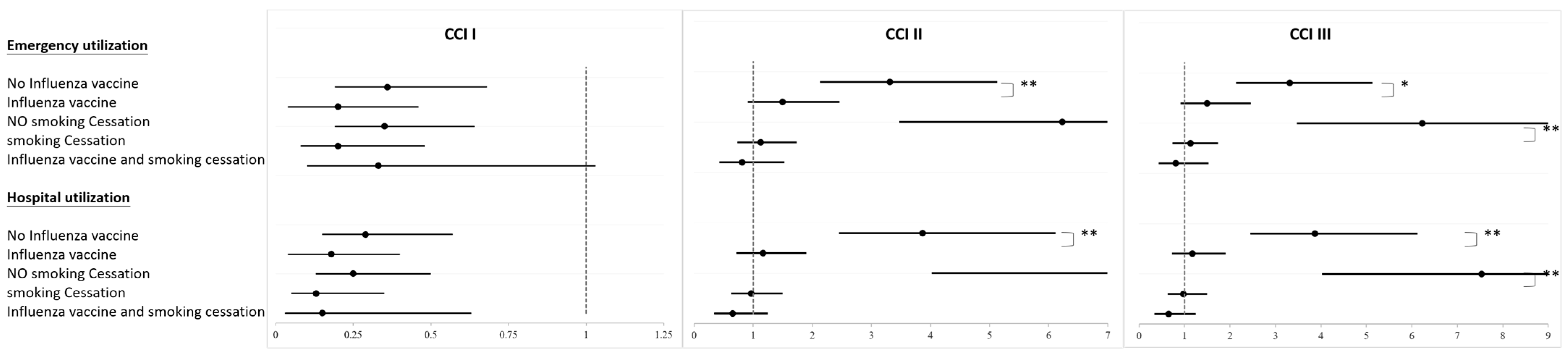
3. Results
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| COPD | Chronic Obstructive Pulmonary Disease |
| CCI | Charlson Comorbidity Index |
References
- Global Strategy for the Diagnosis, Management and Prevention of COPD. In Proceedings of the Global Initiative for Chronic Obstructive Lung Disease (Updated 2024). Available online: https://goldcopd.org/2024-gold-report/ (accessed on 20 April 2024).
- World Health Organization. Chronic Obstructive Pulmonary Disease. Available online: https://www.who.int/news-room/fact-sheets/detail/chronic-obstructive-pulmonary-disease-(copd) (accessed on 16 March 2023).
- Barnes, P.J. Inflammatory mechanisms in patients with chronic obstructive pulmonary disease. J. Allergy Clin. Immunol. 2016, 138, 16–27. [Google Scholar] [CrossRef] [PubMed]
- Mathers, C.D.; Loncar, D. Projections of global mortality and burden of disease from 2002 to 2030. PLoS Med. 2006, 3, e442. [Google Scholar] [CrossRef] [PubMed]
- Wesseling, G. Occasional review: Influenza in COPD: Pathogenesis, prevention, and treatment. Int. J. Chronic Obstr. Pulm. Dis. 2007, 2, 5–10. [Google Scholar] [CrossRef] [PubMed]
- Schauer, U.; Hoffjan, S.; Bittscheidt, J.; Köchling, A.; Hemmis, S.; Bongartz, S.; Stephan, V. RSV bronchiolitis and risk of wheeze and allergic sensitisation in the first year of life. Eur. Respir. J. 2002, 20, 1277–1283. [Google Scholar] [CrossRef] [PubMed]
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C.R. A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. J. Chronic Dis. 1987, 40, 373–383. [Google Scholar] [CrossRef] [PubMed]
- Schols, A.; Buurman, W.A.; Van den Brekel, A.S.; Dentener, M.A.; Wouters, E. Evidence for a relation between metabolic derangements and increased levels of inflammatory mediators in a subgroup of patients with chronic obstructive pulmonary disease. Thorax 1996, 51, 819–824. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Greenlund, K.J.; VanFrank, B.; Xu, F.; Lu, H.; Croft, J.B. Smoking cessation among US adult smokers with and without chronic obstructive pulmonary disease, 2018. Am. J. Prev. Med. 2022, 62, 492–502. [Google Scholar] [CrossRef] [PubMed]
- Trinkmann, F.; Saur, J.; Borggrefe, M.; Akin, I. Cardiovascular comorbidities in chronic obstructive pulmonary disease (COPD)—Current considerations for clinical practice. J. Clin. Med. 2019, 8, 69. [Google Scholar] [CrossRef] [PubMed]
- Godtfredsen, N.S.; Lam, T.H.; Hansel, T.T.; Leon, M.; Gray, N.; Dresler, C.; Burns, D.; Prescott, E.; Vestbo, J. COPD-related morbidity and mortality after smoking cessation: Status of the evidence. Eur. Respir. J. 2008, 32, 844–853. [Google Scholar] [CrossRef] [PubMed]
- Schikowski, T.; Sugiri, D.; Ranft, U.; Gehring, U.; Heinrich, J.; Wichmann, H.-E.; Krämer, U. Long-term air pollution exposure and living close to busy roads are associated with COPD in women. Respir. Res. 2005, 6, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Charlson, M.E.; Carrozzino, D.; Guidi, J.; Patierno, C. Charlson comorbidity index: A critical review of clinimetric properties. Psychother. Psychosom. 2022, 91, 8–35. [Google Scholar] [CrossRef] [PubMed]
- Poland, G.A.; Ovsyannikova, I.G.; Kennedy, R.B. Personalized vaccinology: A review. Vaccine 2018, 36, 5350–5357. [Google Scholar] [CrossRef] [PubMed]
- Qaseem, A.; Wilt, T.J.; Weinberger, S.E.; Hanania, N.A.; Criner, G.; van der Molen, T.; Marciniuk, D.D.; Denberg, T.; Schunemann, H.; Wedzicha, W.; et al. Diagnosis and management of stable chronic obstructive pulmonary disease: A clinical practice guideline update from the American College of Physicians, American College of Chest Physicians, American Thoracic Society, and European Respiratory Society. Ann. Intern. Med. 2011, 155, 179–191. [Google Scholar] [CrossRef] [PubMed]
- de Miguel Díez, J.; Morgan, J.C.; Garrido, P.C.; Barrera, V.H.; Rodríguez, P.R.; Maestu, L.P.; de Miguel, A.G.; García, R.J. Hospitalizations from pandemic influenza (pH1N1) infections among patients with COPD in Spain. Eur Respir. Soc. 2012, 65, 95–98. [Google Scholar] [CrossRef] [PubMed]
- Charlson, M.; Szatrowski, T.P.; Peterson, J.; Gold, J. Validation of a combined comorbidity index. J. Clin. Epidemiol. 1994, 47, 1245–1251. [Google Scholar] [CrossRef] [PubMed]
- Rehman, A.U.; Shah, S.; Abbas, G.; Harun, S.N.; Shakeel, S.; Hussain, R.; Hassali, M.A.A.; Rasool, M.F. Assessment of risk factors responsible for rapid deterioration of lung function over a period of one year in patients with chronic obstructive pulmonary disease. Sci. Rep. 2021, 11, 13578. [Google Scholar] [CrossRef] [PubMed]
- Bekkat-Berkani, R.; Wilkinson, T.; Buchy, P.; Dos Santos, G.; Stefanidis, D.; Devaster, J.-M.; Meyer, N. Seasonal influenza vaccination in patients with COPD: A systematic literature review. BMC Pulm. Med. 2017, 17, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Gershon, A.S.; Chung, H.; Porter, J.; Campitelli, M.A.; Buchan, S.A.; Schwartz, K.L.; Crowcroft, N.S.; Campigotto, A.; Gubbay, J.B.; Karnauchow, T. Influenza vaccine effectiveness in preventing hospitalizations in older patients with chronic obstructive pulmonary disease. J. Infect. Dis. 2020, 221, 42–52. [Google Scholar] [CrossRef] [PubMed]
- Pezzuto, A.; Stellato, M.; Catania, G.; Mazzara, C.; Tonini, S.; Caricato, M.; Crucitti, P.; Tonini, G. Short-term benefit of smoking cessation along with glycopirronium on lung function and respiratory symptoms in mild COPD patients: A retrospective study. J. Breath Res. 2018, 12, 046007. [Google Scholar] [CrossRef] [PubMed]


| Variables (N = 357) | Total | CCI I | CCI II | CCI III | p Value |
|---|---|---|---|---|---|
| Number | 90 (25.21%) | 90 (25.21%) | 177 (49.58%) | ||
| Age (SD) | 71.69 (8.45) | 71.03 (10.04) | 70.57 (9.63) | 0.233 | |
| Gender | 0.067 | ||||
| women | 27 (7.56%) | 2 (2.22%) | 7 (7.78%) | 18 (10.17%) | |
| man | 330 (92.44%) | 88 (97.78%) | 83 (92.22%) | 159 (89.83%) | |
| Influenza vaccination | 0.348 | ||||
| Yes | 213 (59.66%) | 49 (54.44%) | 52 (57.78%) | 112 (63.28%) | |
| No | 144 (40.34%) | 41 (45.56%) | 38 (42.22%) | 65 (36.72%) | |
| Smoking Cessation | 0.036 | ||||
| Yes | 185 (51.82%) | 54 (60%) | 37 (40.11%) | 94 (53.11%) | |
| No | 172 (48.18%) | 36 (40%) | 53 (58.89%) | 83 (46.89%) |
| Emergency Visits | Coef | 95%CI | p Value |
| Age | −0.02 | −0.05~−0.002 | 0.06 |
| Gender | 0.29 | −0.64~1.22 | 0.61 |
| Influenza vaccine | −0.86 | −1.36~−0.36 | 0.00 ** |
| Smoking cessation | −1.25 | −1.74~−0.76 | 0.00 ** |
| CCI I (Ref.) | |||
| CCI II | 1.24 | 0.56~1.94 | 0.00 ** |
| CCI III | 1.76 | 1.15~2.37 | 0.00 ** |
| Hospitalization Frequencies | Coef | 95%CI | p Value |
| Age | −0.01 | −0.02~−0.001 | 0.06 |
| gender | −0.68 | −1.11~−0.21 | 0.07 |
| Influenza vaccine | −0.59 | −0.82~−0.36 | 0.00 ** |
| Smoking cessation | −0.69 | −0.92~−0.46 | 0.00 ** |
| CCI I (Ref.) | |||
| CCI II | 0.54 | 0.23~0.86 | 0.00 ** |
| CCI III | 0.90 | 0.62~1.18 | 0.00 ** |
| Hospital Length of Stay | Coef | 95%CI | p Value |
| Age | 0.06 | −0.07~0.19 | 0.9 |
| gender | −4.39 | −9.04~0.26 | 0.06 |
| Influenza vaccine | −5.57 | −8.07~−3.08 | 0.00 ** |
| Smoking cessation | −3.15 | −5.64~−0.65 | 0.013 * |
| CCI I (Ref.) | |||
| CCI II | 2.28 | −1.16~5.72 | 0.193 |
| CCI III | 4.91 | 1.86~7.95 | 0.00 * |
| CCI I (N = 90) | CCI II (N = 90) | CCI III (N = 117) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Influenza vaccine | NO | Yes | p value | NO | Yes | p value | NO | Yes | p value |
| emergency visits mean ± SD | 0.52 (1.04) | 0.45 (0.91) | 0.338 | 1.85 (2.53) | 0.57 (1.15) | 0.000 | 2.43 (3.19) | 1.41 (1.86) | 0.000 |
| Hospitalization frequencies mean ± SD | 0. 39 (0.80) | 0.36 (0.79) | 0.926 | 1.16 (1.25) | 0.25 (0.51) | 0.000 | 1.47 (1.67) | 0.78 (1.06) | 0.001 |
| Hospital length of stay mean ± SD | 3.84 (10.98) | 1.60 (3.52) | 0.000 | 6.67 (11.51) | 2.22 (4.95) | 0.000 | 10.54 (15.29) | 5.48 (10.03) | 0.000 |
| Smoking Cessation | NO | Yes | p value | NO | Yes | p value | NO | Yes | p value |
| emergency visits mean ± SD | 0.46 (0.95) | 0.39 (1.05) | 0.500 | 2.11 (3.13) | 1.10 (1.54) | 0.000 | 3.26 (3.39) | 1.34 (1.90) | 0.000 |
| Hospitalization frequencies mean ± SD | 0.33 (0.78) | 0.20 (0.58) | 0.061 | 1.05 (1.41) | 0.60 (0.86) | 0.001 | 1.91 (1.49) | 0.78 (1.00) | 0.000 |
| Hospital length of stay mean ± SD | 3.20 (10.69) | 1.89 (6.79) | 0.005 | 7.95 (14.98) | 3.11 (5.49) | 0.000 | 11.45 (13.51) | 7.23 (14.36) | 0.572 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chang, H.-C.; Liu, S.-F. Impact of Smoking Cessation and Charlson Comorbidity Index on Influenza Vaccination Efficacy in COPD Patients. Microorganisms 2024, 12, 1437. https://doi.org/10.3390/microorganisms12071437
Chang H-C, Liu S-F. Impact of Smoking Cessation and Charlson Comorbidity Index on Influenza Vaccination Efficacy in COPD Patients. Microorganisms. 2024; 12(7):1437. https://doi.org/10.3390/microorganisms12071437
Chicago/Turabian StyleChang, Hui-Chuan, and Shih-Feng Liu. 2024. "Impact of Smoking Cessation and Charlson Comorbidity Index on Influenza Vaccination Efficacy in COPD Patients" Microorganisms 12, no. 7: 1437. https://doi.org/10.3390/microorganisms12071437
APA StyleChang, H.-C., & Liu, S.-F. (2024). Impact of Smoking Cessation and Charlson Comorbidity Index on Influenza Vaccination Efficacy in COPD Patients. Microorganisms, 12(7), 1437. https://doi.org/10.3390/microorganisms12071437






