Abstract
Casein phosphopeptide-amorphous calcium phosphate (CPP-ACP), potassium nitrate, and sodium monofluorophosphate are desensitizing agents that help in reducing teeth sensitivity. However, indecisive evidence exists regarding their efficacy. Therefore, this study was conducted to compare the desensitizing efficacy of casein phosphopeptide-amorphous calcium phosphate and potassium nitrate with sodium monofluorophosphate agents after in-office vital bleaching. A randomized controlled trial was conducted on 2011 patients. The patients were randomly and equally divided into the CPP-ACP group (group 1), potassium nitrate with sodium monofluorophosphate group (group 2), and placebo gel (group 3). The upper and lower anterior teeth including the first premolar were isolated with a rubber dam, then the bleaching agents were applied on the labial surface of all the teeth, followed by light activation for 15 min. The procedure was repeated 3 times with an interval of 5 min in-between. After carrying out the bleaching procedure, patients were given a desensitizing gel or placebo gel in unmarked syringes with an instruction to apply it every 12 h for up to 3 days. The intensity of pain was recorded using a discomfort interval scale (DIS). A decrease in pain was observed 24 h after the application of the desensitizing gel in groups 1 and 2. However, in group 3, the pain persisted, with 46 (69.69%) patients having moderate pain and 14 (21.21%) developing severe pain over time. A significant difference in discomfort level with time was noted in group 1 (p = 0.015) and group 2 (p = 0.036). However, no significant difference was found in group 3 (p = 0.085). It was concluded that both desensitizing agents performed exceptionally well in reducing teeth sensitivity.
1. Introduction
Vital tooth bleaching, including in-office bleaching and at-home bleaching, has been adopted as an effective and safe method for the esthetic treatment of stained teeth. Continuous advancements in bleaching products have made in-office bleaching more practical and predictable [1]. The most common side effect of in-office vital bleaching teeth is postoperative sensitivity [2]. Since bleaching occurs by the penetration of free radical ions into the enamel and dentin, it leaves behind micro-porosities that can lead to postoperative sensitivity; this is where desensitizing agents come into action. Several desensitizing agents are available with different mechanisms of action, for instance, some penetrate these micro-porosities and reduce the effects of sensitivity by occluding them, and others work by reducing the ability of nerve endings to block pain [3].
Casein phosphopeptide-amorphous calcium phosphate (CPP-ACP) is a biologically active material that is formed by the combination of casein phosphopeptide and calcium phosphate. CPP-ACP is derived from milk protein and contains phosphoseryl sequence, which helps in the stabilization of amorphous calcium phosphate [3]. The amorphous calcium phosphate plays a significant role in repairing tooth structure and reducing dentin hypersensitivity [4]. The combination of CPP-ACP provides desensitizing action through protein binding followed by continuous deposition of calcium and phosphate on exposed dentinal tubules [5]. CPP-ACP is reported to be effective in reducing sensitivity after teeth bleaching [6].
Potassium nitrate and sodium monofluorophosphate (PNSMP) is also a commonly used desensitizing agent in commercially available toothpaste. It has been in use for decades, and its role in reducing sensitivity is well established in the scientific literature [7,8]. Sodium monofluorophosphate reduces teeth sensitivity by blocking dentinal tubules through calcification. Potassium nitrate works by diffusing through the dentinal tubules to act on nerve endings and blocking the transmission of pulpal pain [8,9].
Nanjundasetty et al. compared the incidence and intensity of teeth sensitivity after in-office vital bleaching using CPP-ACP and PNSMP [10]. They reported that both desensitizing agents were equally effective in reducing teeth sensitivity. In another study by Singh et al., CPP-ACP was compared with sodium fluoride for reducing postoperative sensitivity after in-office vital tooth bleaching [11]. They reported a higher incidence and duration of tooth sensitivity in patients without the use of a desensitizer, compared with those exposed to the desensitizing agents.
In the light of the aforementioned literature, it has been observed that indecisive evidence exists regarding the efficacy of both desensitizing agents in reducing teeth sensitivity. Therefore, it was worthwhile to conduct a randomized clinical trial that compared the desensitizing efficacy of CPP-ACP and PNSMP after in-office vital bleaching.
2. Materials and Methods
A double-blinded randomized controlled trial was conducted at the department of operative dentistry and endodontics, Altamash Institute of Dental Medicine, for 11 months from 1 January 2020 to 1 December 2020. The study was previously approved by the Ethics Committee (protocol number: (AIDM/ERC/12/2019/01). The Helsinki Declarations’ ethical aspects were followed.
The sample size was calculated using the WHO sample size calculator, considering a mean discomfort score of 1.13 ± 1.08 of potassium nitrate and sodium monofluorophosphate, with a power of test 80. The confidence interval was set at 95% and 5% margin of error. The estimated sample size in each group was 67 participants [10].
A simple random sampling technique was used for the recruitment of participants in this study. Patients of both genders and aged between 18 to 45 years who required in-office vital bleaching in teeth with normal pulp response and no history of previous tooth sensitivity were included. Smokers, pregnant or lactating mothers, root canal-treated anterior teeth, anterior teeth with gingival recession or dentin exposure, active root carious lesion, and patients with known allergy to milk protein “casein” were excluded.
After obtaining informed consent, patients were randomly and equally divided into three groups by a certified dental hygienist using the lottery method: the CPP-ACP group (group 1), PNSMP group (group 2), and placebo gel group (group 3). To begin with, a cheek retractor was placed, and petroleum gel was applied on the exposed lip surface. Upper/lower anterior teeth including the first premolar were dried and isolated by a gingival barrier. After that, a thin layer of bleaching agent, 35% hydrogen peroxide (Fluorescent Express White, Vista Dental, USA) was applied on the labial surface of all isolated teeth, followed by light activation for 15 min. The procedure was performed 3 times for 8 min, as per manufacturer instructions. A certified dental hygienist was responsible for handing over the desensitizing or placebo gel in an unmarked (blinded) syringe to the patient with a written instruction to apply it immediately and every 12 h up to 36 h after the procedure.
A questionnaire designed to obtain information on any incident of pain after bleaching treatment was given to the patients. Patients were thoroughly educated about the questionnaire and were asked to mark the intensity of pain five minutes after the application of gel on a discomfort interval scale (DIS) [12], which was explained to the patients, and instructions were given to mark the score from 0 to 4 according to the intensity of pain experienced, such as 0: no pain, 1: mild pain, 2: moderate pain, 3: severe pain, and 4: intolerable pain.
Data were entered and analyzed using SPSS version 25. Mean and standard deviation was calculated for age and sensitivity score. Frequency and percentage were calculated for qualitative variables such as gender and efficacy. Efficacy of the desensitizing agent was compared in all groups by using an ANOVA test and post hoc Tukey’s test. Pearson correlation was applied to find an association of desensitizing agents with age. An independent t-test was applied to find gender disparity in discomfort level, keeping p ≤ 0.05 as significant.
3. Results
A total of 201 patients participated in this double-blind randomized controlled trial; patients were randomly and equally divided into three groups of 67 patients in each. There were three dropouts: one subject from each group. One subject from group 1 dropped out for an unknown reason and subjects from groups 2 and 3 dropped out due to severe sensitivity. The other 66 participants were available for the recall at 24 and 36 h of the study. Patients in group 1 applied CPP-ASP as the desensitizing agent, while group 2 used PNSMP, and group 3 applied placebo gel after in-office vital bleaching (Figure 1).
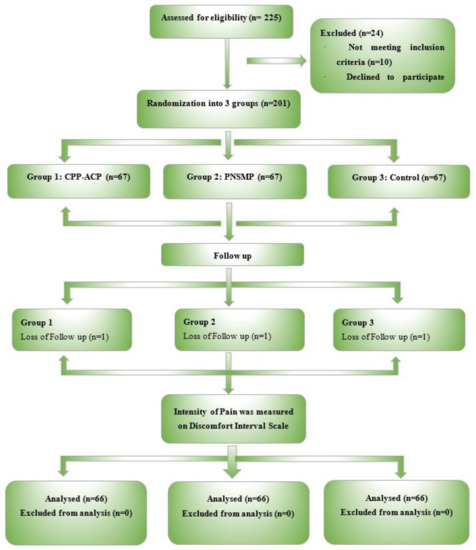
Figure 1.
CONSORT flow diagram of the study.
Overall, the mean age of participants who consented to participate in this study was calculated as 25.74 ± 5.155, with a standard error of ±0.445. This means that the average age for all participants who were part of this clinical trial was between 25 and 26 years of age. The gender distribution of patients showed equal representation (99 were males and were 99 females).
Furthermore, at the baseline, i.e., after bleaching but before the application of the desensitizing agent, it was observed that 54 (81.8%) of the total patients in group 1 experienced moderate pain, while 6 (9.09%) had severe pain, 4 (6.06%) showed mild pain, and 2 (3.03%) had no pain. In group 2, at the baseline 54 (81.81%) patients had moderate pain, 5 (7.57%) had mild pain, 4 (6.06%) had severe pain, and 3 (4.54%) had no pain at all. However, in group 3, 57 (86.36%) patients had moderate pain, 3 (4.54%) had mild pain, 3 (4.54%) had severe pain, and 3 (4.54%) no pain, as shown in Table 1.

Table 1.
Comparison within different groups before and after application of desensitizing agents.
The decrease in pain was observed 24 h after the application of the desensitizing gels in groups 1 and 2. Out of the total patients, it was observed that in group 1, 40 (60.60%) patients had mild pain, while 18 (27.27%) had no pain at all. In seven (10.60%) patients, the moderate amount of pain persisted, while one (1.51%) still had severe pain. Almost similar results were found in group 2 patients, where 41 (62.12%) patients had mild pain, while 19 (28.78%) had no pain at all, and in 6 (9.09%) patients the moderate level of pain persisted. In group 3, 46 (69.69%) patients had moderate pain and 14 (21.21%) developed severe pain, while 3 (4.54%) had mild pain, and 3 (4.54%) had no pain, as shown in Table 1.
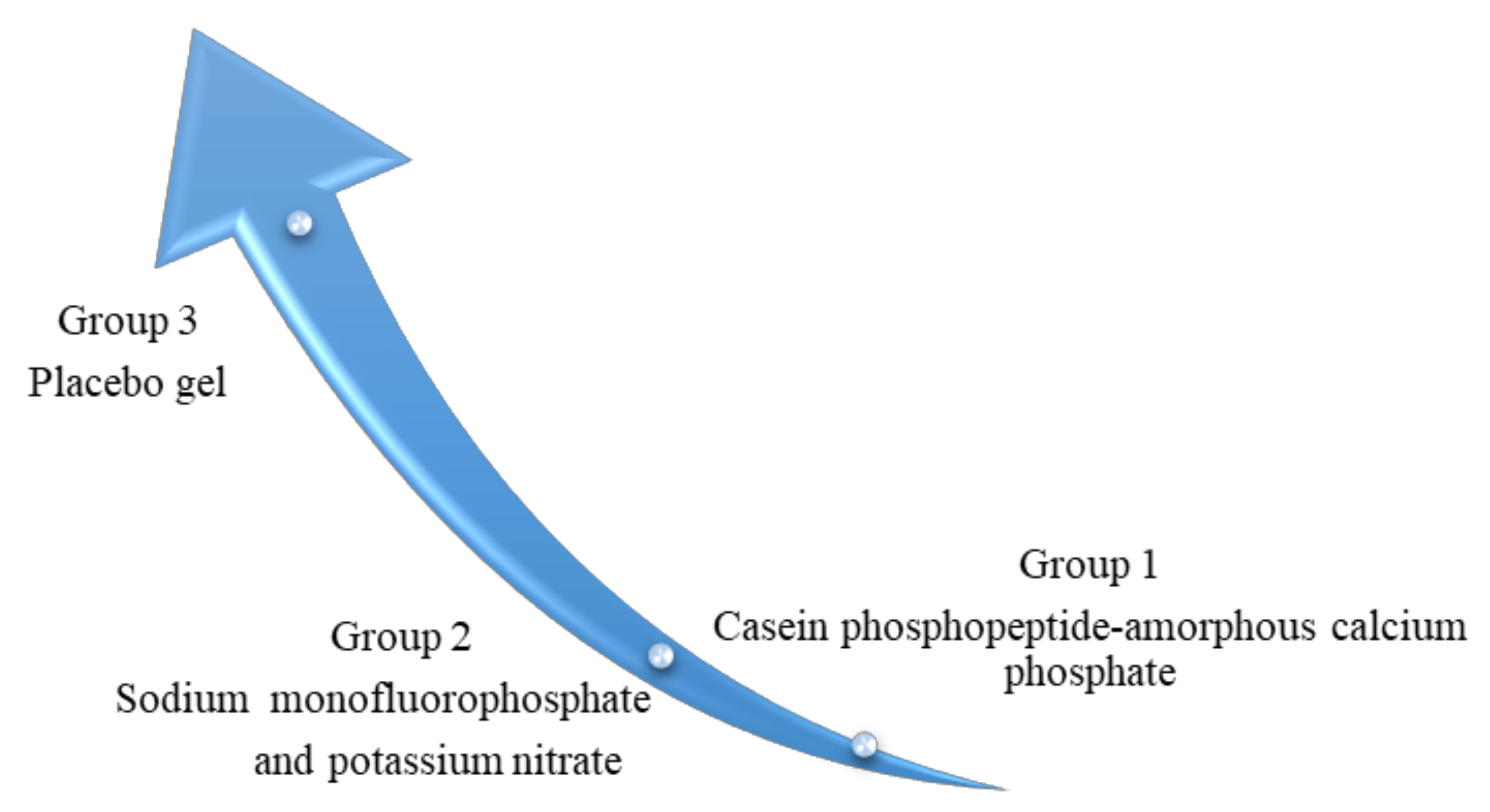
Lastly, after 36 h, the pain further decreased in group 1 and group 2 patients. In group 1, 57 (86.36%) patients were pain-free, followed by 7 who had only mild pain (10.60%) and 2 in which moderate pain persisted (3.03%). Meanwhile, in group 2, 57 patients (86.36%) were pain-free, followed by 8 patients (12.12%) who had only mild pain and only 1 who had moderate pain (1.51%). However, in group 3, 33 patients developed severe pain (48.48%) and 28 had moderate pain (42.42%), while 3 had mild pain (4.54%) and 3 had no pain (4.54%), as shown in Table 1. There was a significant difference in discomfort level with time within group 1 (p = 0.015) and group 2 (p = 0.036). However, no significant difference was found in group 3 (p = 0.085). The pain severity was worse in group 3 in comparison with groups 1 and 2, as illustrated in Figure 2.
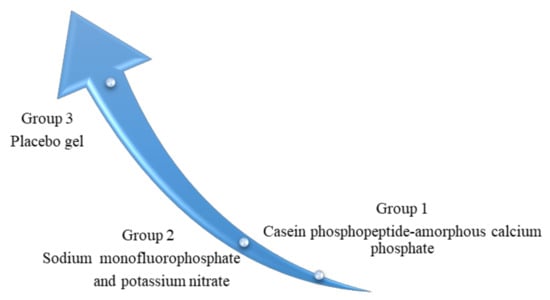
Figure 2.
Illustration of pain severity in study groups, the upward extension of arrowhead suggests an increase in pain intensity between experimental and control groups.
However, no significant difference (independent t-test; p = 0.391) was found between both sexes when desensitizing agents were applied on teeth, demonstrating that the postoperative discomfort was the same in both sexes. There, was a strong correlation (Pearson correlation pr = 0.75, p = 0.651) between age and desensitizing or pain reduction, post bleaching amongst the participants in this study, indicating that the level of discomfort was higher with increase in age and vice versa.
The majority of the participants from both groups experienced “mild pain” postoperatively in the first 24 h. In group 1, 30 females (88.23%) reported no or mild pain postoperatively after application of CPP-ASP; whereas only 3 females (8.82%) observed moderate pain, and 1 female developed severe pain (2.94%). Likewise, the majority of males in group 1 (29; 87.87%) noted no or mild pain, followed by 4 males who experienced moderate pain (12.12%).
Moreover, in group 2, 31 females observed no or mild pain (91.17%), followed by 3 patients (8.82%) who experienced moderate pain, whereas 30 males (90.90%) reported “no or mild pain”, and 3 reported moderate pain (9.09%).
Intergroup comparison revealed no significant difference in pain between the experimental groups at baseline and after 24 h and 36 h of desensitizing agents’ application, whereas a statistically significant difference was found between the experimental groups and the control group initially and after 24 to 36 h of bleaching application, showing higher incidence and greater intensity of sensitivity in the control group (Table 2).

Table 2.
Comparison of mean DIS score between the groups.
4. Discussion
The current study was conducted to compare the desensitizing efficacy of casein phosphopeptide-amorphous calcium phosphate and potassium nitrate with sodium monofluorophosphate after in-office vital bleaching. The results of the study show that both desensitizing gels (i.e., CPP-ASP and sodium monofluorophosphate) had a similar effect on reducing postoperative sensitivity after in-office vital teeth bleaching. The results of the current study are in agreement with the findings reported by Nanjundasetty et al. [10] and Gama et al. [13]. They reported a remarkable decrease in postoperative sensitivity following an in-office vital bleaching after using CPP-ASP. Moreover, Khoroushi et al. revealed that CPP-ACP can compensate for the loss of flexural strength of enamel and dentine that may occur during the bleaching [14]. The desensitizing effect of potassium nitrate (KNO3) has been established for decades, and it is a core component in various desensitizing toothpastes and mouthwashes. Peacock et al. have reported that the required concentration of K+ ions around the axons should be around 8 mM to 16 mM to achieve depolarization [15]. Potassium nitrate in combination with Na-monofluorophosphate has been claimed to significantly reduce postoperative sensitivity [7,8,9]. However, others observed no additional benefits of this combination on reduction in postoperative sensitivity [16].
Moreover, by stratifying gender and age, it became more evident that the postoperative pain experience was generally the same among participants from each gender and age group, although more females than males tend to seek bleaching treatment and more young people than older people tend to seek it rather. In this regard, stratification helped in reducing the risk of overestimating our results.
Furthermore, it can be seen in the results presented that the majority of the participants in either trial group only experienced “mild” to “moderate” postoperative pain in relation to the DIS. This shows that using either desensitizing agent significantly reduces postoperative pain irrespective of their mechanism of action.
Furthermore, if we consider the pricing of both of these products, it can be said that CPP-ACP is more expensive to purchase and use, whereas potassium nitrate with sodium monofluorophosphate is a more cost-effective option. However, this can be completely left to the discretion of the dental practitioner to choose either. Concerning our clinical study, statistical analysis has shown no evidence of either product being superior to the other one or vice versa.
Additionally, like every other study, this study also had its limitations. Although great care was taken to carefully explain to the participants how to complete the DIS, it can be said that there could have been errors on their part to correctly assess the severity of postoperative pain after in-office vital bleaching of teeth, which may have led to an overestimation of (DIS) pain scores. Moreover, the outliers may also have misjudged the severity of postoperative pain due to human error. Furthermore, due to limited resources, the sample size used in this study was not large enough to gauge more minor differences between the two products. Additionally, many other desensitizing products widely available in the market had to be left out of the study due to budget constraints.
5. Conclusions
This study concluded that both the desensitizing agents, i.e., casein phosphopeptide-amorphous calcium phosphate and potassium nitrate with sodium monofluorophosphate, were equally effective in eliminating postoperative discomfort after bleaching. It is up to the dental practitioners to take factors such as their cost of operations, material preferences, and clinical practice constraints into consideration before using either of the two products. This study intends to leave the decision of using either product to the sole discretion of the respective clinician when performing in-office vital teeth bleaching.
Author Contributions
Conceptualization, H.M.A., R.J., N.A. and M.S.A.; methodology, H.M.A., M.A.A., R.J., A.M. and S.B.; software, N.A., M.S.A. and A.K.N.; validation, A.M., R.J., M.K.A. and S.B.; formal analysis, H.M.A., N.A., M.S.A.; investigation, A.M.; resources, M.K.A., M.A.A. and R.J.; data curation, M.A.A., H.M.A. and A.K.N.; writing—original draft preparation, H.M.A., N.A., M.A.A., R.J. and A.M.; writing—review and editing, M.K.A., S.B., M.S.A. and A.K.N.; visualization, H.M.A., R.J.; supervision, R.J. and N.A.; project administration, H.M.A., R.J., M.A.A.; funding acquisition, M.K.A., S.B., A.K.N. and R.J. All authors have read and agreed to the published version of the manuscript.
Funding
The authors extend their appreciation to the Deanship of Scientific Research at Jouf University for funding this work through research grant no. (DSR-2021-01-0393).
Institutional Review Board Statement
The study was approved by the Institutional Review Board of Altamash Institute of Dental Medicine (AIDM/ERC/12/2019/01).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data included in the present study are available upon request from corresponding author.
Acknowledgments
The authors are grateful to the research and evaluation committee of Altamash Institute of Dental Medicine, King Faisal University and Jouf University, Kingdom of Saudi Arabia, for support and facilitation of this study. Additionally, part of the present research work was supported by Taif University Researchers Support project number (TURSP-2020/62), Taif University, P.O. Box-11099, Taif 21944, Saudi Arabia.
Conflicts of Interest
The authors declare no conflict of interest.
Abbreviations
| S. No | Abbreviation | Full Name/Description |
| 1. | CPP-ACP | Calcium phosphopeptide-amorphous calcium phosphate |
| 2. | PNSMP | Potassium nitrate with sodium monofluorophosphate |
| 3. | DIS | Discomfort interval scale |
References
- Wijetunga, C.L.; Otsuki, M.; Hiraishi, N.; Luong, M.N.; Tagami, J. Effect of pH of bleaching agent on tooth bleaching action in vitro. Dent. Mater. J. 2021, 40, 566–572. [Google Scholar] [CrossRef] [PubMed]
- Majeed, A.; Farooq, I.; Grobler, S.R.; Rossouw, R.J. Tooth-Bleaching: A Review of the Efficacy and Adverse Effects of Various Tooth Whitening Products. J. Coll. Physicians Surg. Pak. 2015, 25, 891–896. [Google Scholar] [PubMed]
- Alqahtani, M.Q. Tooth-bleaching procedures and their controversial effects: A literature review. Saudi Dent. J. 2014, 26, 33–46. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ma, X.; Lin, X.; Zhong, T.; Xie, F. Evaluation of the efficacy of casein phosphopeptide-amorphous calcium phosphate on remineralization of white spot lesions in vitro and clinical research: A systematic review and meta-analysis. BMC Oral Health 2019, 19, 295. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Walsh, L.J. The effects of GC Tooth Mousse on cervical dentinal sensitivity: A controlled clinical trial. Int. Dent. SA 2012, 12, 4–12. [Google Scholar]
- Yassin, O.; Milly, H. Effect of CPP-ACP on efficacy and postoperative sensitivity associated with at-home vital tooth bleaching using 20% carbamide peroxide. Clin. Oral Investig. 2019, 23, 1555–1559. [Google Scholar] [CrossRef] [PubMed]
- Waraaswapati, N.; Krongnawakul, D.; Jiraviboon, D.; Adulyanon, S.; Karimbux, N.; Pitiphat, W. The effect of a new toothpaste containing potassium nitrate and triclosan on gingival health, plaque formation and dentine hypersensitivity. J. Clin. Periodontol. 2005, 32, 53–58. [Google Scholar] [CrossRef] [PubMed]
- Low, S.B.; Allen, E.P.; Kontogiorgos, E.D. Reduction in dental hypersensitivity with nano-hydroxyapatite, potassium nitrate, sodium monoflurophosphate and antioxidants. Open Dent. J. 2015, 27, 92–97. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Orchardson, R.; Gillam, D.G. The Efficacy of Potassium Salts as Agents for Treating Dentin Hypersensitivity. J. Orofac. Pain 2000, 14, 9–19. [Google Scholar] [PubMed]
- Nanjundasetty, J.K.; Ashrafulla, M. Efficacy of desensitizing agents on postoperative sensitivity following an in-office vital tooth bleaching: A randomized controlled clinical trial. J. Conserv. Dent. 2016, 19, 207–211. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Singh, M.; Mahajan, P.; Monga, P.; Mahajan, S.; Singla, K.N. Comparative evaluation of effectiveness of sodium fluoride and casein phosphopetipde-amorphus calcium phosphate (CPP-ACP) in treating postoperative sensitivity associated with in-office vital tooth bleaching: A clinical study. Endodontology 2017, 29, 27–34. [Google Scholar]
- Yu, X.; Liang, B.; Jin, X.; Fu, B.; Hannig, M. Comparative in vivo study on the desensitizing efficacy of dentin desensitizers and one-bottle self-etching adhesives. Oper. Dent. 2010, 35, 279–286. [Google Scholar] [CrossRef] [PubMed]
- Cunha, A.G.; De Vasconcelos, A.A.; Borges, B.C.; Vitoriano Jde, O.; Alves-Junior, C.; Machado, C.T.; Dos Santos, A.J. Efficacy of in-office bleaching techniques combined with the application of a casein phosphopeptide-amorphous calcium phosphate paste at different moments and its influence on enamel surface properties. Microsc. Res. Tech. 2012, 75, 1019–1025. [Google Scholar] [CrossRef] [PubMed]
- Khoroushi, M.; Mazaheri, H.; Manoochehri, A. Effect of CPP-ACP application on flexural strength of bleached enamel and dentin complex. Oper. Dent. 2011, 36, 372–379. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Peacock, J.M.; Orchardson, R. Effects of potassium ions on action potential conduction in A- and C-fibers of rat spinal nerves. J. Dent. Res. 1995, 74, 634–641. [Google Scholar] [CrossRef] [PubMed]
- Tarique, N.; Awan, R.; Saleh, M.I. Vital tooth bleaching and management of post operative sensitivity: A clinical trial evaluating the efficacy of different desensitizing materials. Pak. J. Med. Health Sci. 2017, 11, 1564–1567. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).