Abstract
Virtual reality (VR) demonstrates significant potential to improve rehabilitation outcomes for musculoskeletal conditions and associated chronic pain. However, the field faces notable challenges, including inconsistent terminology, a lack of specialized/comprehensive software solutions, and an overwhelming variety of hardware options, which can make it difficult for healthcare professionals without technical expertise to identify the most suitable tools for clinical use. This article explores the current state of VR in the rehabilitation of musculoskeletal conditions and chronic pain, focusing on terminology discrepancies, available hardware and software solutions, and key professional associations shaping the field. A review of the current state of terminology is essential to address inconsistencies that risk perpetuating misuse and to facilitate clearer communication. Building on this review, we propose a conceptual framework for understanding VR that aligns more closely with the capabilities of current VR technology. A comprehensive overview of VR hardware and software can assist healthcare professionals in selecting appropriate technologies for clinical practice, guide researchers in designing interventions, and inform developers on unmet needs in the field. Furthermore, understanding key professional associations provides valuable direction for those engaged in virtual rehabilitation, enabling them to access resources, foster collaboration, and stay informed about the latest advancements in the domain. This review addresses the significant confusion regarding the understanding of VR, particularly in relation to its classification based on levels of immersion. Accordingly, it proposes a framework that contributes to a standardized approach to understanding VR. Additionally, it highlights the lack of VR solutions tailored to the needs of patients with musculoskeletal conditions and associated chronic pain, emphasizing the necessity for further development in this area.
1. Introduction
Initially, virtual reality (VR) applications in healthcare predominantly focused on pain distraction during acute procedures, such as managing burn patients [1]. Its use for chronic pain received less attention, likely due to the persistent nature of chronic pain, making continuous VR use seem impractical [2]. This may explain why VR research for chronic pain lags behind its application for acute pain. Similarly, the development of VR for musculoskeletal rehabilitation has progressed more slowly compared to its adoption in neurological rehabilitation [3]. One potential reason is that VR was initially considered more suitable for neurological patients due to its ability to facilitate cortical reorganization and potentially restore motor function [4]. Although motor function improvement is also an important focus in musculoskeletal rehabilitation, the field often emphasizes goals such as enhancing range of motion, increasing muscle strength, and managing pain. At first glance, it may seem that these objectives would not significantly benefit from VR compared to traditional non-VR interventions, raising questions about its cost-effectiveness for widespread adoption in the musculoskeletal field. Accordingly, a recent scoping review identified financial costs as one of the barriers to the implementation of VR in healthcare [5]. However, it appears that in the field of chronic musculoskeletal conditions, VR may be cost-saving compared to non-VR interventions [6]. In addition, for patients with these conditions, the use of VR goes beyond mere distraction from immediate pain. Recovery success in patients with musculoskeletal pain, regardless of chronicity, can be hindered by various psychosocial factors [7,8,9,10,11,12,13], which can be addressed through VR. VR can benefit patients with kinesiophobia by providing distraction from fear, facilitating movement [14], or through gradual exposure to feared movements, enabling desensitization and reducing fear responses over time [15]. A fun, engaging, and interactive form of therapy is offered through VR, enhancing patient motivation for rehabilitation [16,17,18]. By enabling patients to develop skills for the self-regulation of pain through interactive and sensory-augmented experiences, such as controlling unpleasant virtual elements via biosensor feedback or practicing deep breathing techniques in gamified environments, it also serves as a tool to improve self-efficacy [19]. Additionally, it facilitates embodiment, allowing users to perceive the virtual body as their own [20,21]. Consequently, during and after VR interventions, users exhibit attitudes or behaviors aligned with the characteristics of the virtual avatar, a phenomenon known as the Proteus effect [22,23]. By leveraging embodiment in virtual avatars, VR can help address altered body image [24,25], which is often particularly pronounced in cases of chronic pain [26] and can contribute to dysfunctional pain-coping strategies, such as movement avoidance [27]. Furthermore, meta-analyses have increasingly highlighted the significant benefits of VR in managing musculoskeletal conditions and associated chronic pain [28,29,30,31,32,33,34,35,36], underscoring its potential as a valuable tool for integration into healthcare to effectively address these conditions.
However, likely due to the relatively recent expansion of VR research in healthcare, particularly in the rehabilitation of musculoskeletal conditions, the field faces notable challenges. These challenges include inconsistent terminology, a lack of specialized software solutions, and an overwhelming variety of hardware options, most of which are not primarily designed for healthcare use. Such factors can make it difficult for healthcare professionals without technical expertise to identify the most suitable tools for clinical practice. This article aims to explore the current state of VR in the rehabilitation of musculoskeletal conditions and associated chronic pain, focusing on terminology discrepancies, available hardware and software solutions, and key professional associations shaping the field. A review of the terminology is essential to address inconsistencies that risk perpetuating incorrect use and limiting the applicability of research findings. Building on this review, we aim to propose a conceptual framework for understanding VR that aligns more closely with the capabilities of current VR technology and aims to contribute to clearer communication. Furthermore, a comprehensive overview of VR hardware and software can assist healthcare professionals in selecting appropriate technologies for clinical practice, guide researchers in designing interventions, and inform developers on unmet needs in the field. Understanding the role of key professional associations also provides valuable direction for those engaged in virtual rehabilitation, enabling them to access resources, foster collaboration, and stay informed about the latest advancements in the domain.
2. Methods
This scoping review examines the current state of VR in musculoskeletal rehabilitation and associated chronic pain, focusing on terminology, VR technology (equipment), and relevant associations. Given the interdisciplinary nature of this topic, an exploratory approach was adopted to capture the breadth and depth of the field. To identify emerging trends and commercial applications, the data collection included gray literature, conference proceedings, and online resources, alongside peer-reviewed scientific articles. Unlike systematic reviews, which focus on answering specific, narrowly defined research questions and require a critical appraisal of included studies, scoping reviews are designed to map key concepts, identify gaps, and provide an overview of the existing literature. Since the aim of this review was to explore the breadth of research rather than assess study quality or effectiveness, a systematic review was not a feasible approach. This review was not prospectively registered, and as it does not involve empirical data collection from human participants or animals, ethical approval was not required.
2.1. Study Eligibility Criteria
To investigate existing research on VR terminology and examine how researchers in the field of musculoskeletal conditions conceptualize and define VR, we included studies that specifically focus on VR terminology, as well as review and original research articles that explore the use of either immersive or non-immersive VR for any musculoskeletal condition while explicitly providing a definition of VR. To examine the hardware and software used in studies on immersive VR for musculoskeletal conditions, we included research that investigates the application of immersive VR for any musculoskeletal condition and provides details on the VR equipment utilized. Additionally, to provide an overview of available commercial equipment, we conducted an online search and included VR hardware and software providers that appeared to offer solutions for immersive VR experiences suitable for musculoskeletal rehabilitation. Furthermore, we included associations and platforms dedicated to the use of VR in rehabilitation and medicine, highlighting key organizations involved in advancing VR applications in healthcare.
2.2. Information Sources and Search Strategy
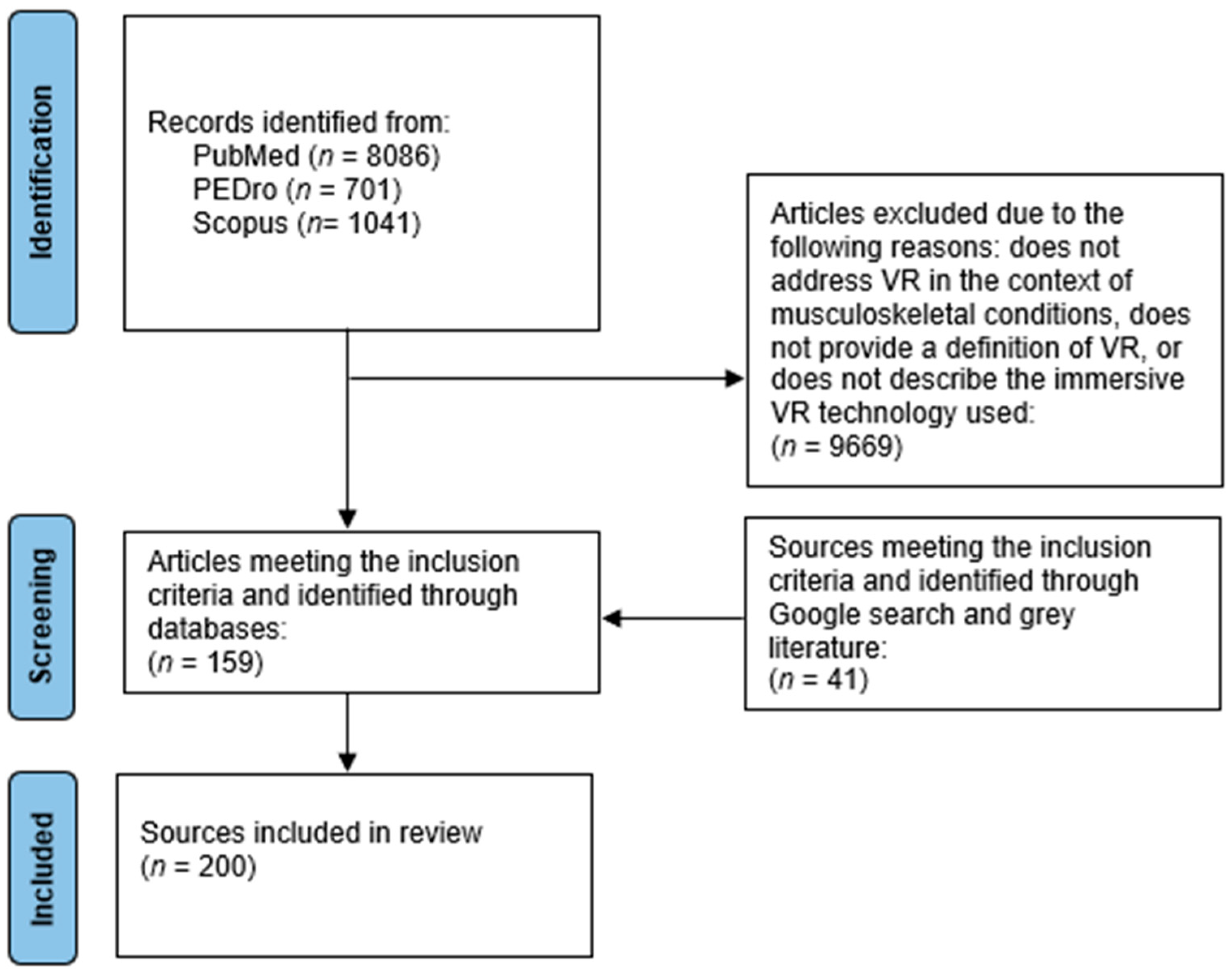
The search for articles was conducted in the PubMed, PEDro, and Scopus databases. Additionally, we performed a non-systematic search of the first five pages on Google Scholar. We used combinations of the following keywords in our article search.: “VR”, “virtual reality”, “virtual rehabilitation”, “virtual environment*”, “XR”, “extended reality”, “X-reality”, “cross reality”, “enhanced reality”, “mixed reality”, “MR”, “augmented reality”, “AR”, “immersive technology”, “immersive environment*”, “immersive technologies”, “terminology”, “definition*”, “terms”, “taxonomy”, “framework*”, “musculoskeletal”, “musculo-skeletal”, “orthopedic”, “orthopaedic“, “chronic pain”, “persistent pain”, “neck pain”, “back pain”, “knee”, “hip” “ankle”, “shoulder”, “elbow”, “tendinopathy”. Articles examining the use of VR for musculoskeletal conditions were also derived from data extraction conducted during the development of recent meta-analyses on the use of VR for musculoskeletal issues and associated chronic pain authored by the researchers [37,38]. Furthermore, we conducted a non-systematic search using the Google search engine to identify commercially available VR solutions (hardware and software). In addition to synonyms for VR and musculoskeletal conditions (outlined in beforementioned keywords), the following keywords were used when searching for commercially available VR solutions: HMD, head-mounted display, technology, hardware, software, tracker. Relevant information about VR technology was collected also by examining the websites of various VR companies listed on websites of associations such as XR4REHAB. These associations and organizations were identified through Google searches using keywords such as: organizations, networks, associations, societies, alongside the previously mentioned VR-related terms. Furthermore, some associations and VR technological solutions were introduced to the authors during international conferences on virtual rehabilitation, such as the «World Congress on Virtual Rehabilitation 2024» held in Amsterdam. The search process is presented in Figure 1.
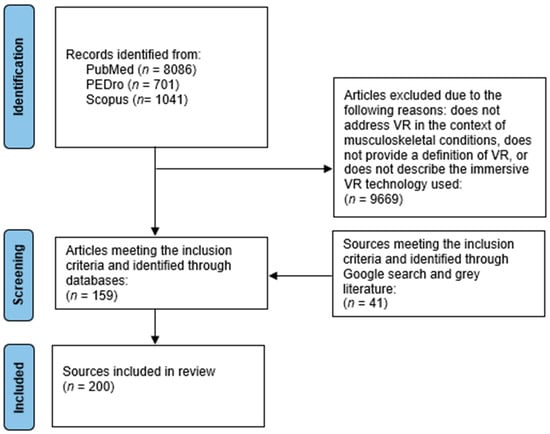
Figure 1.
Flowchart of the article search process [39].
2.3. Data Extraction and Analysis
A spreadsheet was created by both authors, and the data were extracted by M.O.Z. and checked by N.S. Data extracted included: (a) study design, (b) musculoskeletal condition studied, (c) VR definitions, (d) VR hardware, (e) VR software, (f) company name, (g) name of association, (h) field of activity of the association. In this study, all authors actively participated in discussions and reached a consensus on the final reporting of results. We employed a narrative synthesis approach to analyze and integrate the extracted data.
3. The Ambiguity of Virtual Reality Terminology in Healthcare and Beyond
Not only in the field of VR, but also within the broader spectrum of related technologies such as augmented reality (AR) and mixed reality (MR), a significant issue arises due to the lack of consensus on definitions and the meaning of terms. Numerous authors who have explored terminology in this area point to discrepancies in the use and interpretation of terms, leading to confusion among researchers, practitioners and users, with this inconsistency also evident in the use of VR in healthcare [40,41,42,43]. The lack of clarity is reflected not only in the scientific literature, but also in the definitions provided by various dictionaries [40,43]. It also extends to the marketing of these technologies, where professional news agencies have been observed describing the same product as an example of MR, AR, and VR, and instances have been noted where companies promote their immersive devices in ways inconsistent with common definitions, presenting them as something they are not [41,44]. In response to the confusion around definitions, some companies (such as Apple, Cupertino, CA, USA) strategically avoid specific terminology related to immersive technologies in their marketing and instead emphasize the use and capabilities of their technology [41,45].
The reasons for the lack of uniform terminology can be attributed to several factors. On one hand, the rapid development of technology means that new innovations are constantly emerging, often outpacing the adoption of updated definitions [41,43]. Some researchers suggest that this confusion arises from the exploration of VR-related concepts across diverse fields, where varying disciplinary perspectives lead to inconsistent applications of technology and thus inconsistent interpretations of the terms [41]. Cultural differences influencing the understanding of these terms and technology providers redefining terms to position their products more favorably, further contribute to the inconsistency [41,46].
The lack of uniformity in the definitions of VR is evident in the varying criteria used: some definitions rely primarily on the hardware employed (e.g., head-mounted displays, HMDs), others on the nature of the experience (e.g., the level of immersiveness), and some on the forms of interaction [41,43,47,48]. In the field of VR applications for healthcare conditions, definitions vary most significantly in how VR is characterized with respect to immersiveness. While some authors define VR as an “immersive experience” [47], “immersive 3D environment” [49] or 3D environment that differs from “watching an image on a typical computer or video display” [50], numerous studies in musculoskeletal rehabilitation report less immersive interventions. These interventions involve participants interacting with a digital environment viewed on a 2D computer screen, which is also referred to as a VR intervention [6,51,52,53,54]. Furthermore, numerous meta-analyses evaluating the effectiveness of VR include both interventions involving HMDs and 2D computer screens, such as Wii games. These analyses have been conducted in the context of low back and neck pain [32,55], rehabilitation of orthopedic ankle injuries [34], rehabilitation following total hip arthroplasty [56], and anterior cruciate ligament (ACL) injuries [29]. Notably, meta-analysis of ACL rehabilitation by Cortés-Pérez et al., (2024) [29] did not include any studies that examined immersive VR interventions using HMDs. This discrepancy indicates that VR in healthcare encompasses a broad spectrum of technologies and that VR remains a very broad term in this field. Such a broader understanding may also stem from some of the earliest definitions in rehabilitation from the 1990s, which did not limit VR to immersive systems but described it as including HMDs as well as other equipment such as monitors or large screens [57,58]. On the other hand, the inconsistency in reported definitions poses significant challenges. These inconsistencies limit the understanding and applicability of research findings, restrict researchers from identifying relevant studies, and create unrealistic expectations about the potential of these novel solutions [43,59].
3.1. Modern Definitions and Concepts of Virtual Reality and Related Technologies
The inconsistency in terminology surrounding VR and related technologies has led authors to propose modern definitions and concepts intended to align with current technological advancements and the use of VR systems. However, even up-to-date definitions lack uniformity, despite being published within a span of just one to two years [40,42,43]. This lack of consensus can even be seen in the definition of the appropriate umbrella term for VR and related technologies (the most frequently mentioned besides VR are AR and MR).
In the literature, the abbreviation “XR” is widely accepted as an umbrella term, but its interpretation varies. Some attribute XR to “extended reality” [60], others to “cross reality” [61], and some to “X-reality” [62], which is occasionally described as a variaton of “eXtended reality” [63,64]. Although it is widely agreed that XR encompasses VR, AR, and MR [65,66,67], the relationships between these technologies are often not clearly defined, except for MR, which is typically described as a blend of VR and AR [43].
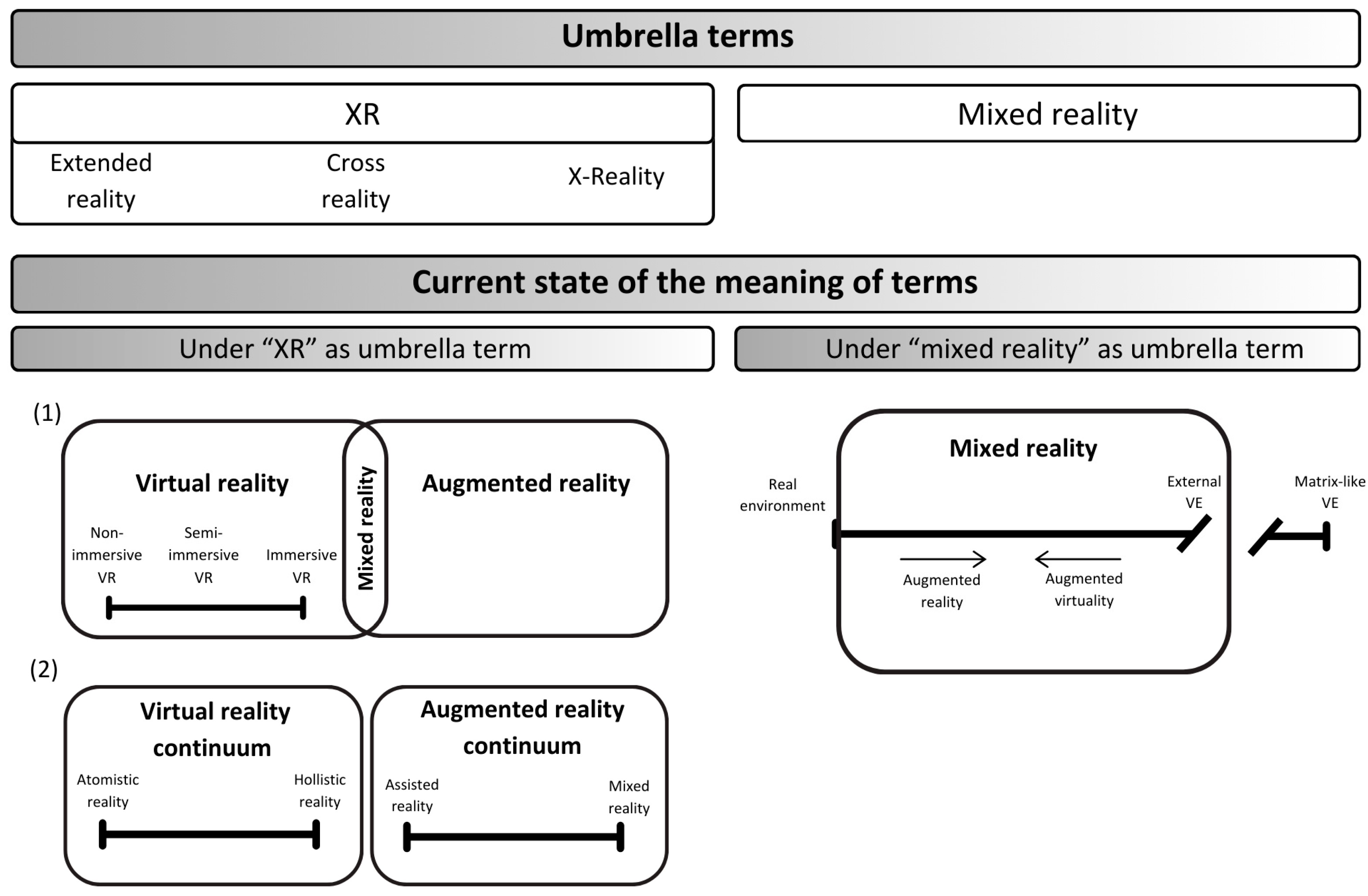
Recently, Rauschnabel et al., (2022) [40] raised concerns about the term “extended reality,” emphasizing that it fails to include VR, where the real environment is replaced rather than extended. As an alternative, the authors proposed “X-reality” as an umbrella term, with “X” functioning as a placeholder for any form of new reality. Within their framework, an AR continuum was introduced, extending from assisted reality, where virtual content appears clearly artificial, to MR, where the integration of virtual and real objects becomes seamless and indistinguishable. The concept also incorporates diminished reality, which ranges from the application of unrealistic overlays to the undetectable removal of real objects [40]. Additionally, they further outlined a VR continuum that spans from atomistic VR, prioritizing specific goals over user experience, to holistic VR, characterized by an immersive experience nearly indistinguishable from real-world interactions [40]. In contrast, Milgram and Kishino, (1994) [68] proposed the reality-virtuality continuum, anchored at one end by a purely real environment and at the other by a purely virtual environment. In their model, MR is defined as the umbrella term for environments that combine real and virtual elements, excluding fully virtual environments, which are positioned at the far right of the continuum. Critics, however, argue that the virtual environment endpoint, defined by Milgram and Kishino, (1994) [68] as “consisting solely of virtual objects” and “completely synthetic,” can be fully virtual only for extroceptive senses, but not for interoceptive ones [42]. Consequently, they propose that all VR experiences should be categorized under the umbrella term “mixed reality”, as they inherently blend virtual elements with real-world sensations (e.g., computer-generated stimuli combined with physical sensations such as gravity) [42]. Recently proposed frameworks and the present understanding of VR and related technologies are illustrated in Figure 2.
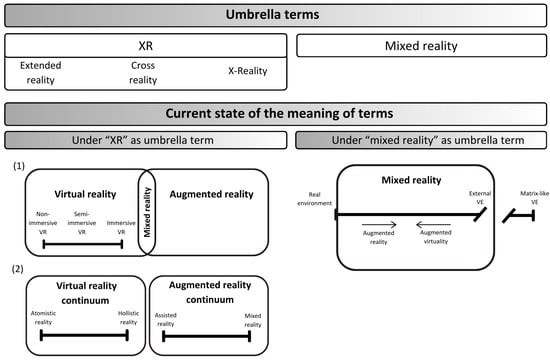
Figure 2.
The current state of umbrella terms with the most common understanding and contemporary proposals for the meaning of VR and related technologies. VR and related technologies, such as augmented reality (AR) and mixed reality (MR), are commonly grouped under the umbrella term XR. This abbreviation refers to “extended reality”, “cross reality”, or “X-reality”, with no significant difference in meaning between these terms. Under the umbrella of XR, VR and AR are the most frequently included components, with their combination forming MR (as shown in point 1 in Figure 2). In healthcare, this understanding of the relationships between VR, AR, and MR is the most widely accepted, where VR is further categorized based on the level of immersion, ranging from non-immersive to immersive VR. Recently, Rauschnabel et al., (2022) [40] distinguished VR and AR across two separate continua (see point 2 in Figure 2). According to their framework, VR spans from atomistic VR, which prioritizes specific goals over user experience, to holistic VR, characterized by immersive experiences that are indistinguishable from real-world interactions. In contrast, AR is described as ranging from assisted AR, where virtual objects are clearly artificial overlays on real-world objects, to MR, where the integration of virtual and real objects becomes indistinguishable. In contrast, Skrabez et al., (2021) [42] proposed “mixed reality” as the umbrella term, building upon and updating the framework introduced by Milgram and Kishino in 1994 [68]. According to their understanding, MR encompasses environments where real-world and virtual objects and stimuli are presented together within a single percept. MR environments where the real world is augmented with virtual content are referred to as AR, while environments where most content is virtual but there is some inclusion of real-world elements are termed augmented virtuality (AV). Under this interpretation, MR also encompasses VR, which they term an “external virtual environment (VE)” that includes only the stimulation of exteroceptive senses. At the far-right end of the continuum lies “Matrix-like VE”, which is excluded from MR (along with the purely real environment on the left end) and represents a simulation of both exteroceptive and interoceptive senses, a level of immersion that cannot be achieved in the real world.
In the field of healthcare, the term “XR” is widely used, with some researchers expanding its scope to include video games and related applications, in addition to VR, MR, and AR [60]. This further underscores the tendency of some researchers in this field to classify VR alongside 3D games displayed on a flat 2D screen. Accordingly, in their literature review, Abbas et al., (2023) [43] examined how the term VR is defined in the medical literature and proposed the following definition of VR: “VR is a three-dimensional computer-generated simulated environment, which attempts to replicate real-world or imaginary environments and interactions, thereby supporting work, education, recreation, and health”. Their definition was constructed to accommodate the current confusion in the field and to encompass the broad range of interpretations of what constitutes VR. Based on the up-to-date definition by Abbas et al., (2023) [43], any interaction with a 3D environment appears to qualify as VR, regardless of whether it is displayed on a 2D computer screen or through HMD. In contrast, modern definitions developed outside of healthcare, such as the one proposed by Rauschnabel et al., (2022) [40], limit VR to experiences where the user “does not see the physical environment and is, at least visually, sealed off from the physical environment”. This suggests that the understanding of VR in healthcare somewhat diverges from how VR is interpreted in other fields. One possible explanation for this discrepancy is the frequent use of various types of XR technologies in industry, particularly for training, simulations, and entertainment, where more immersive technologies often take center stage. In contrast, applications in healthcare tend to rely more on non-immersive approaches, such as Nintendo Wii games, a technology whose production in the industry ended in 2013. When it comes to immersive experiences, healthcare primarily utilizes immersive VR, while the use of MR and AR currently lags behind. This is likely due to the increasing accessibility of immersive VR, whereas MR and AR remain relatively recent developments.
3.2. Categorization of Virtual Reality in Healthcare: Subtypes Based on Levels of Immersion
In the field of healthcare, researchers often include a range of technologies under the VR term. These are typically categorized by the level of immersion, which is objective quality of VR and is associated with its technical aspect, such as the system’s ability to provide realistic feedback, facilitate general interaction, and enable the user to move and behave naturally within the virtual environment [69]. Within this context, VR in healthcare is commonly divided into three categories: non-immersive, semi-immersive, and (fully) immersive VR (see Figure 2).
Although studies uniformly describe the categorization of VR based on levels of immersion, there is inconsistency in how these terms are defined. For instance, non-immersive VR is commonly described as a virtual environment projected onto a 2D display screen [4,36,65,70,71]. Some authors state that such environments allow users to interact with it [36], while others do not mention interaction at all, instead defining non-immersive VR as the user observing or viewing computer-generated images of a virtual environment on a screen [4,70] or as a virtual environment “presented on a flat screen” [72]. This lack of clarity is problematic, as such definitions could classify activities where the user remains entirely passive (e.g., watching television) as non-immersive VR. Furthermore, the concept of a 2D screen requires more precise definition. Some virtual environments projected onto 2D screens that entirely surround the user and block their view of the real world—commonly referred to as VR caves—are classified as immersive VR by certain authors [40]. However, according to other definitions, VR caves could be classified as semi-immersive VR environments, which are described as environments that “integrate a large display screen for projecting the virtual environment” [36]. Based on the definition proposed by Wei et al., (2024) [36], the distinction between non-immersive and semi-immersive environments appears to hinge on the size of the display screen. However, it remains unclear where the threshold for screen size lies.
In the field of rehabilitation, non-immersive VR is often referred to as “exergames” or “active video games” which represents a combination of exercise and gaming [73]. This terminology likely arises because VR is frequently used in rehabilitation for exercise-based interventions. Additionally, exergames often rely on technologies such as Nintendo Wii, Xbox, and PlayStation, which many authors in healthcare classify as “non-immersive VR” [73,74]. It therefore seems that exergames are a subcategory of less immersive VR experiences that require patients to perform physical exercises. However, since some researchers state that exergames occur within less immersive environments [73,74], this raises the question of how to classify immersive VR experiences that also require patients to perform exercises. Alternatively, it may be necessary to revise the definition of exergaming to additionally include experiences involving immersive technology. Another term frequently used to describe VR interventions in healthcare is “serious games”. Serious games are defined as games designed with a purpose beyond entertainment and are utilized to promote users’ mental, physical, and social well-being [75]. It can be summarized that serious games represent a subcategory of VR, which can be further divided into exergames—a specific type of serious game focusing on exercise-based activities.
In the context of the treatment of musculoskeletal disorders and chronic pain, immersive VR appears to be predominantly limited to the use of HMDs. For example, immersive VR in this field is described as: “achieved through HMDs…” [36]; “involves the use of HMDs…” [70]; “involves utilizing an HMD” [4]; and “VR is considered immersive when an HMD is used” [76]. It seems that in addressing musculoskeletal issues, researchers primarily classify immersive VR as technology that engages vision, without incorporating other sensory modalities, such as touch, which could be facilitated by additional equipment like haptic technology. This may be due to the limited availability or high cost of such equipment, which makes its inclusion in studies less feasible. Another possible reason is that, particularly for patients with chronic pain who have a reduced capacity to process information, additional haptic technologies may not be used because some authors highlight the risk of information overload caused by excessive multisensory input [77]. Sensory overstimulation could result in negative outcomes such as increased stress, frustration, or even trigger kinesiophobia or catastrophizing in this population group [77].
In contrast to the approach in healthcare, which often categorizes VR based on the level of immersion, some authors from other fields argue that VR is inherently immersive and involves experiences where the physical environment is at least visually replaced [40]. These definitions exclude activities such as “looking at 3D content on a 2D screen and browsing through it with a mouse” [40]. Others contend that a fully immersive VR experience, where no real-world stimuli are perceived, does not exist. Such an experience, they argue, would only be possible in a Matrix-like VR scenario, where both interoceptive and exteroceptive senses are entirely stimulated by technology [42].
Furthermore, according to some definitions, non-immersive experiences classified as VR in healthcare might be more appropriately categorized as AR. For example, Milgram and Kishino, (1994) [68] define AR as “an environment that is primarily real but includes virtual elements”. Definitions which do not describe AR as an environment that overlaps or blends the virtual and real worlds, suggest that AR could also encompass situations where an individual perceives reality (e.g., themselves and the surrounding physical world) while simultaneously viewing a virtual world. This could include scenarios where an individual is positioned in front of a 2D computer screen, observing a virtual environment—commonly referred to as non-immersive environments in healthcare.
In summary, the lack of consensus on the definition of VR in the various application areas remains a problem. It can be said that the understanding of VR in the healthcare sector is somewhat different compared to other sectors. Although it appears that most researchers in healthcare categorize VR based on levels of immersion, notable discrepancies remain within the healthcare field itself, particularly regarding whether the observation of and/or interaction with 3D environments displayed on 2D computer screens should be classified as VR. Overall, the inconsistency in VR terminology highlights the need for researchers and practitioners to precisely define the equipment and methods they use [41]. While detailed descriptions of interventions are valuable, the need for such precision can increase the risk of errors—if an intervention is not thoroughly described, reliance may fall solely on (potentially inaccurate) terminology. Different interpretations of the same terms can lead to the inclusion of various types of interventions under a single label. For example, in the case of non-immersive VR, it is currently unclear whether such environments require interaction from the user or not. Uniformity in terminology would facilitate clearer communication within the field by reducing the need for highly detailed descriptions of the technology used and its intended purpose, ensuring a shared understanding of key concepts.
Supplementary Table S1 presents the definitions and descriptions of VR provided in studies investigating its application in the context of musculoskeletal conditions.
3.3. Rethinking the Meaning of Virtual Reality: A Proposed Framework
The terminology surrounding VR in healthcare is characterized by inconsistency and ambiguity, particularly regarding levels of immersion. While Abbas et al. (2023) [43] provided a comprehensive attempt to define VR terminology for healthcare applications, their approach primarily aimed to accommodate the existing confusion in the field, rather than resolve it by addressing the ambiguity surrounding terms like non-immersive, semi-immersive, and immersive VR. We believe there is significant confusion regarding what constitutes different levels of immersion in VR environments, particularly in defining non-immersive and semi-immersive VR. Meanwhile, current definitions of immersive VR are often limited solely to the use of HMD headsets, overlooking other modern technologies that stimulate additional exteroceptive senses (as presented in Section 3.2). Additionally, there also appears to be confusion about whether VR is understood as an immersive environment or as an environment that can encompass various levels of immersion. This lack of clarity underscores the need to develop a more refined framework specifically addressing the concept of immersion. To the best of our knowledge, our proposed framework is the first in the healthcare field to tackle this issue comprehensively. Our article serves as a starting point for establishing uniform terminology in this field, which appears to urgently require a standardized approach. We believe it will contribute to reducing ambiguity and facilitating clearer communication within the field. Our framework is not intended to prioritize immersive VR over non-immersive VR or to suggest that one is inherently more beneficial than the other. Instead, it seeks to address existing terminological inconsistencies and provide a standardized basis for understanding VR environments based on their technical characteristics.
Proposition 1:
VR begins when visual field is entirely occupied with virtual information.
In line with certain authors [40], we argue that VR experiences should be limited to so-called immersive VR experiences, where the individual cannot see the real world and is thus visually completely detached from it. According to this understanding, VR cave technologies would not fall under VR, as individuals using this technology can still see their own body and the physical surface they are standing on. The only technology currently capable of achieving such visual detachment from the real world are HMDs.
Proposition 2:
What is currently referred to as “non-immersive VR” should be distinguished from VR and excluded from the umbrella term encompassing VR and related technologies.
Non-immersive VR experiences, commonly categorized as virtual environments that individuals observe or interact with via computer screens, should not be considered part of VR or related technologies and should not fall under the XR umbrella (or mixed reality, which some propose as an umbrella term).
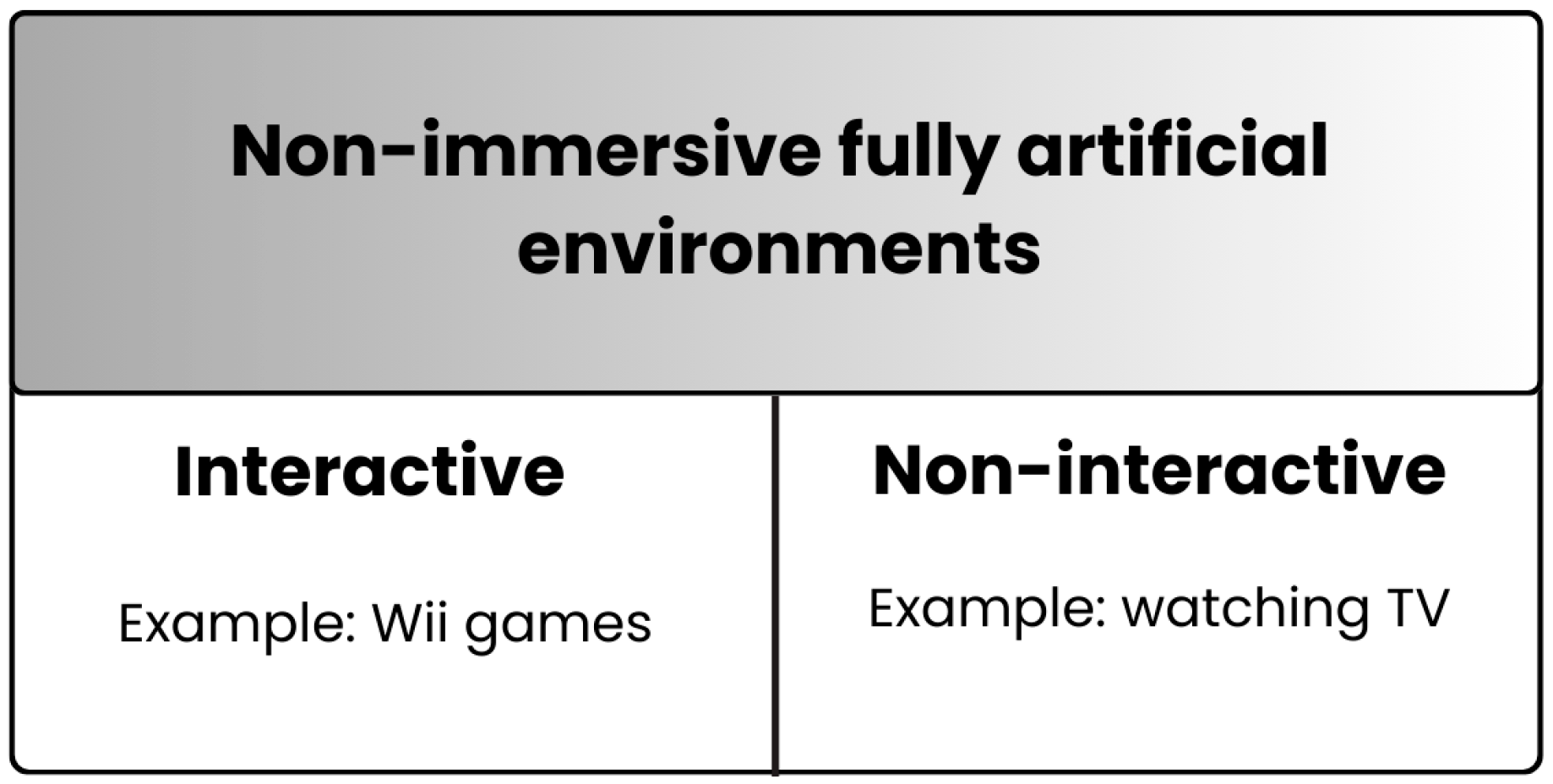
For VR in healthcare currently labeled as “non-immersive”, which typically involves the projection of artificial environments on a computer or television screen (e.g., Wii games) and does not allow for complete visual detachment from the real world, regardless of whether these environments are interactive or non-interactive, we propose the term “non-immersive fully artificial environments”. The term “non-immersive” distinctly separates these environments from VR, which, according to our proposal, begins only when an individual’s entire visual field is occupied by virtual information. Thus, VR can never truly be “non-immersive” (as it always involves at least visual immersion), making “non-immersive” a suitable term to differentiate these environments. The term “fully artificial” further clarifies the distinction from environments where virtual objects are integrated into the real world, a feature commonly included in definitions of AR or MR. Non-immersive fully artificial environments can still provide a certain degree of presence [78]. However, since the technology used in these environments does not allow for complete visual detachment from the real world, we categorize them as non-immersive environments.
We would like to emphasize that this distinction is not based on differences in the effectiveness of non-immersive and immersive environments. The separation of non-immersive environments is made based on the technological solutions these environments offer compared to immersive ones. As presented in the review article by Wilkinson et al., (2021) [69] immersion is described as “a more objective quality of VR” and “the technical qualities of a system”.
Furthermore, this distinction aligns with certain proposals from other authors in the field who also define VR as exclusively immersive environments [47,49,50]. This separation is not intended to discourage the use of non-immersive environments in healthcare but rather to establish a clear and standardized framework for understanding and categorizing VR technologies based on their technical characteristics.
Proposition 2 is illustrated in Figure 3.
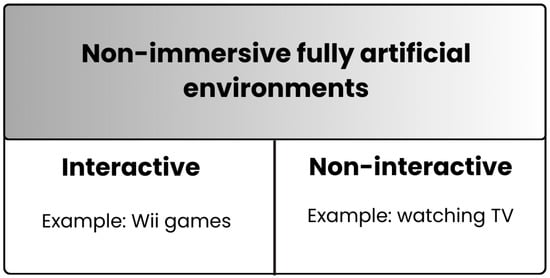
Figure 3.
Our proposal for naming environments currently defined as “non-immersive VR”. We propose that such environments be referred to as “non-immersive fully artificial environments”. Additionally, we propose “non-immersive fully artificial environments” should neither be classified as VR nor included under the XR umbrella (or mixed reality, which some propose as an umbrella term for VR and related technologies). “Non-immersive fully artificial environments” can be interactive (e.g., Wii games) or non-interactive (e.g., watching television). Typically, they are accessed through devices such as computers, televisions, or smartphones. According to the proposed term, so-called VR caves would also fall under “non-immersive fully artificial environments” (moreover, their name should no longer include the term VR).
Proposition 3:
VR should be divided into two continua of immersion depth based on exteroceptive and interoceptive system involvement.
The level of immersion in VR should be categorized based on the involvement of the exteroceptive system (i.e., sensory signals from outside the body) and the interoceptive system (i.e., sensory signals from inside the body). Such a classification has likely not been introduced previously due to the limited research on interoceptive system stimulation until recent years. However, evidence in this field is growing. For instance, Lernia et al., (2023) [79] demonstrated the ability to artificially manipulate interoceptive cortical signaling using a non-invasive stimulation technique called Sonoception. They showed that auditory synthetic stimulation (Sonoception) could prime insular activity (a key component of the interoceptive system that processes and integrates signals from within the body), either enhancing impulsivity or promoting inhibitory control, depending on the specific area of the insula targeted. Other interoceptive technologies are also emerging in research. These include methods that produce direct modulation of interoceptive signals, such as C-fiber stimulation [80,81], as well as tools that create illusions by providing individuals with false feedback about their physiological states [82]. To the best of our knowledge, no research in the healthcare field has yet combined VR with interoception stimulation. However, there are articles that discuss the integration of internal body stimulation with VR in the medical field [83], highlighting the need to reconceptualize certain previous frameworks that suggested interoception stimulation with modern technology was not possible [42].
Proposition 4:
Immersion should be categorized based on the number of stimulated senses and the quality of virtual stimulation.
We propose that the level of immersion should be categorized based on the number of senses stimulated and the quality of virtual stimulation. In the case of exteroception, it is possible to virtually stimulate all senses quantitatively, making this continuum continuous. In contrast, the immersion of the interoceptive system is inherently limited, as technology cannot fully simulate all interoceptive signals. A higher number of stimulated senses enhances immersion and, consequently, the sense of presence by increasing the feeling of “being there” [84]. This occurs because more attentional resources are allocated to the virtual world as the number of stimulated senses increases [84]. The level of immersion increases not only with the number of virtually stimulated senses but also with the quality of virtual stimulation. The better the quality of virtual stimuli (e.g., the visual appearance of objects, tracking quality, etc.), the greater the immersion. This, in turn, contributes to higher perceived realism and subsequently enhances the sense of presence [84].
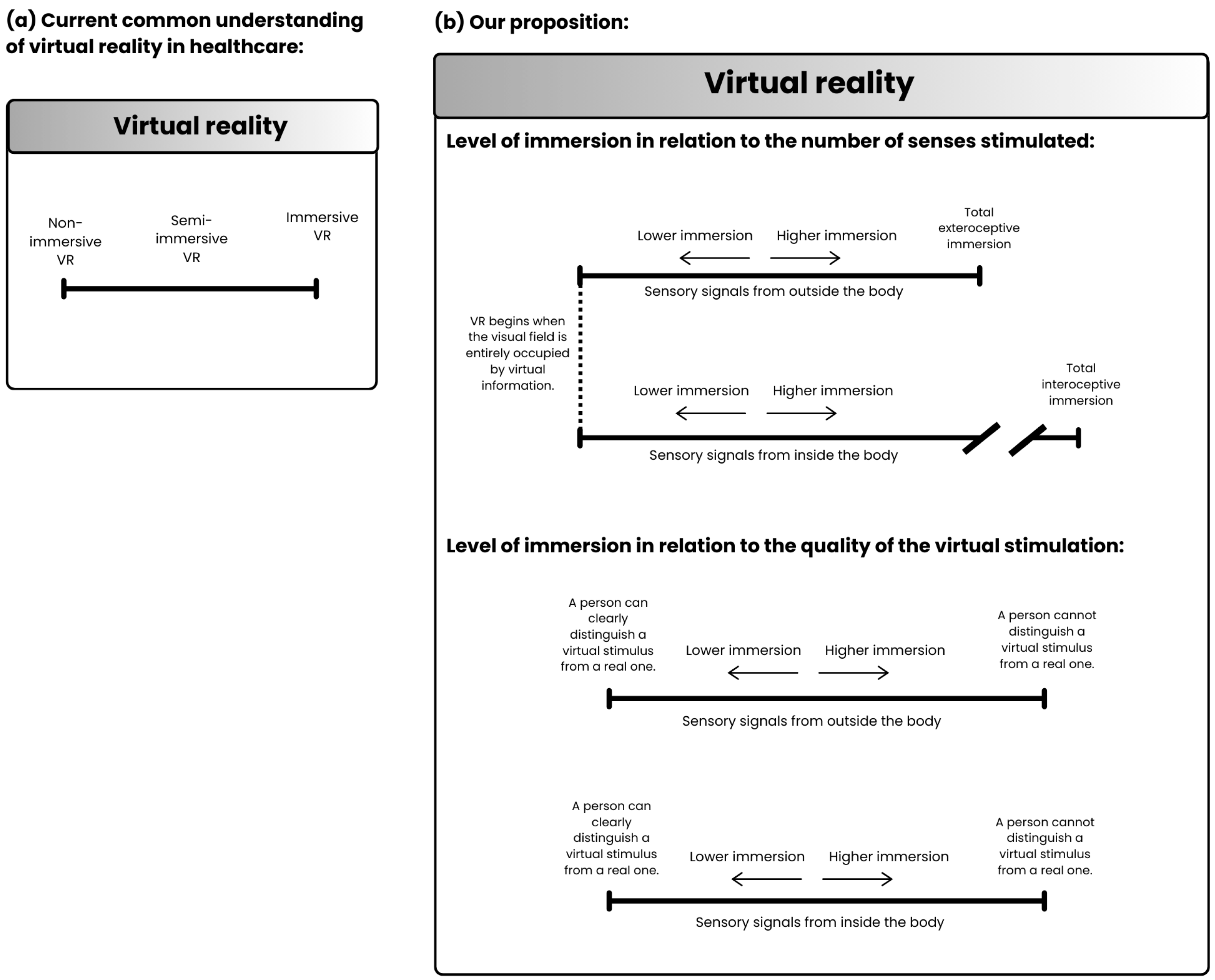
Figure 4 illustrates the proposed understanding of VR based on the level of immersion.
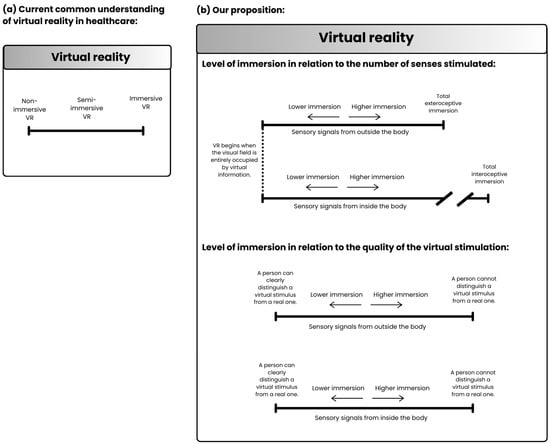
Figure 4.
(a) Representation of the most commonly mentioned categorization of VR based on immersion in healthcare. Currently, in healthcare, VR is classified on a single continuum of immersion depth, ranging from non-immersive VR (often involving systems such as Wii games) to immersive VR, typically associated with the use of HMDs. (b) Our proposed categorization of virtual reality based on immersion levels. We propose that the depth of immersion should be divided into two dimensions: the immersion depth of the exteroceptive and interoceptive systems. Additionally, immersion depth should also account for whether it is influenced by the number of senses stimulated or the quality of virtual stimulation.
4. Immersive Virtual Reality: Hardware and Software Perspectives
4.1. Overview of Immersive Virtual Reality Hardware
In healthcare, the most immersive experiences are often associated with the use of HMD devices. Therefore, this hardware overview will primarily focus on HMDs and accessories that can be utilized to enhance immersion.
The leading companies currently offering VR hardware for immersive experiences are primarily targeting entertainment, business applications and areas such as education and training [45,85,86,87,88]. Their focus is on providing devices that serve the general consumer and enterprise market, rather than specifically addressing the needs of patients. Nevertheless, researchers are increasingly using these companies’ hardware to perform therapeutic interventions with patients and support the treatment of various health conditions. It appears that Meta’s headset series are one of the most widely used immersive VR devices in chronic pain and musculoskeletal research. For example, VR headsets developed by Meta (formerly Oculus/Facebook Technologies) have been used in studies involving experimental groups of patients with various chronic pain conditions, including those with chronic low back pain [49,89,90,91,92], chronic neck pain [93,94], knee osteoarthritis [95] as well as participants experiencing different types of chronic pain across various body regions [96,97,98]. In studies conducted on patients with chronic pain, researchers have also used the Pico [99,100], HTC Vive [50,101,102,103], Samsung [96,104,105], and Vuzix [106] headsets. These companies typically offer a range of headset options rather than a single model, each tailored to different use needs and experiences [85,86,88]. Each VR headset varies across numerous specifications, significantly impacting the user experience. For instance, higher resolution per eye contributes to clearer and more detailed visuals, while refresh rate affects the smoothness and responsiveness of the display. The field of view (FOV), which represents the observable extent of the virtual environment influences the level of immersion. Headsets also differ in their ability to adjust interpupillary distance (IPD) to accommodate various users’ eye spacing. Weight and comfort of headsets are critical considerations, as heavier devices increase discomfort and pressure loads [107]. Battery performance is another important factor, varying between devices and determining their suitability for prolonged use without interruptions. Tracking capabilities also differ significantly, with some headsets supporting full-body, eye, face, or hand tracking through integrated sensors and cameras within the headset, meaning they can track body movements without the need for additional external sensors [85,88]. VR headsets can be categorized as either standalone or wired. Standalone models offer portability and freedom of movement due to integrated hardware, while wired headsets deliver higher performance but are limited by a direct connection to a PC [108].
Along with the purchase of VR headsets, companies often provide handheld controllers to facilitate interaction within the virtual environment. Additionally, a variety of optional accessories are available for separate purchase, enhancing the VR experience. For example, some devices provide optimized haptic feedback to the torso, enhancing tactile sensations during VR use [109]. For precise body tracking, accessories are available to monitor facial expressions and eye movement [110], hand tracking [111,112], tracking of orientation and rotation of the legs for control of locomotion [113] and even full body tracking [88,114,115]. Muscle-movement detectors such as FirstVR [116], feature optical sensors that detect arm and hand movements while providing vibration feedback. All-in-one solutions like the Tesla Suit integrate multiple functionalities, offering comprehensive body tracking with haptic feedback, motion capture, and biometric monitoring [117]. Some external sensors, require the installation of base stations to monitor sensor movements, a process known as outside-in tracking [118]. Others use built-in cameras for self-contained tracking, referred to as inside-out tracking, which provides greater mobility [88]. There are also products that enable motion tracking without the use of wearable sensors, utilizing motion-tracking cameras instead. Orbbec offers such solutions, like the Femto Bolt [119], which serves a similar purpose to the former Kinect. Some accessories are particularly useful in healthcare settings, such as facial interface with silicone facial pad, designed for easier sanitation [120], or UV-C disinfection cabinet for mobile headsets [121]. Limited physical space for VR use can be mitigated with devices like VR walkers, which enable locomotion within a confined area, allowing users to walk, run, or engage in movement-based actions without physically moving through the real-world environment [122]. Accessory compatibility varies—some are exclusive to headsets from the same manufacturer [114], while others are third-party compatible, functioning across multiple brands [123]. These various accessories allow users to tailor their VR setup to their specific needs, enhancing realism and interaction in virtual environments, whether for gaming, professional applications, or therapeutic use.
Currently, VR hardware appears to be fairly accessible for general consumers, with entry-level headsets available at relatively affordable prices. More affordable options include the DPVR P1 Personal for USD 198, Meta Quest 3S starting at approximately USD 300, HTC Vive Focus Plus at USD 450, Sony’s PlayStation VR2 at USD 550, and Steam’s Valve Index at USD 540, making these devices feasible options for many users interested in experiencing VR. However, the cost spectrum varies widely, with some mid- and high-tier models priced at thousands of euros. For instance, the Pimax Crystal series ranges from €860 to €1200, Lenovo’s ThinkReality VRX is offered at USD 1300, DPVR PRO-4K at USD 1099, VR TierOne’s at USD 1800, Apple’s Vison Pro at USD 3500, and HTC Vive’s Focus Vision and Focus 3 models are priced at USD 1000 and USD 1300, respectively. At the high end, Varjo stands out as an enterprise-grade option, with models such as the XR-4 starting around USD 5990 or XR-4 Focal Edition, starting at USD 9990. Unlike consumer-focused companies like Meta and Sony, which primarily target the entertainment sector, Varjo caters to professional fields, including healthcare, aerospace, marine and heavy industry, and government defense. Its key strength lies in its photorealistic image quality, making it exceptionally suited for developing VR environments that closely replicate real-world scenarios. This wide price range of immersive VR hardware allows VR to reach both casual users and those needing advanced, industry-specific features.

Table 1.
Overview of VR headsets and their specifications.

Table 2.
Overview of additional VR equipment and their functions.
4.2. Overview of Immersive Virtual Reality Software
The market for immersive VR software specifically tailored to musculoskeletal rehabilitation appears to be relatively underrepresented compared to offerings for neurological rehabilitation. This trend could be due to the higher research activity in the field of VR for neurorehabilitation, as a quick search in the PubMed database shows. Using a search string designed to capture VR applications for various neurological conditions (including terms such as: “VR”, “virtual reality”, “neuro*”, “stroke”, “Parkinson*”, “multiple sclerosis”, “brain injury”, “brain damage”, “CVA”, “cerebrovascular accident”, “spinal cord injury”, and “cerebral palsy”), number of the results are almost four times higher than those for musculoskeletal applications (the search string for the use of VR for musculoskeletal disorders included the following terms: “VR”, “virtual reality”, “musculoskeletal”, “orthopaedic”, “neck”, “back”, “knee”, “hip”, “ankle”, “shoulder”, “joint replacement”, “arthroplasty”). This discrepancy may reflect the growing interest in VR’s potential to support recovery in neurological patients, leaving musculoskeletal VR applications as a smaller, still developing field.
In the treatment of patients with musculoskeletal disorders and chronic pain, a variety of VR software is used in research, with the same software rarely appearing in more than one study. This variability could be attributed, at least in part, to the possibility that some of this research is funded by technology companies developing proprietary VR systems [82]. Both commercially available applications and custom-developed programs are used in these studies. Examples of commercially available software used in research include: RelieveVRx (initially named EaseVRx) by AppliedVR [49,124,125], guided meditation VR app by Cubicle Ninjas [50,95], Karuna Virtual Embodiment Training [102], the COOL! app by DeepStreamVR [126], VR TierOne [101], Ocean Rift and Gala 360 [93], Creed: Rise to Glory, The Avengers Powers Unite and The Climb [25]. These VR applications differ in the experiences and actions they require of users. Some software programs focus on meditation, education, and/or relaxation. RelieVRx, for example, is an immersive, multimodal, skills-based pain self-management program that incorporates evidence-based principles of cognitive behavioral therapy, mindfulness, and pain-neuroscience education. Other applications promote physical movement in a VR environment. Ocean Rift and Gala 360, for example, promote neck movement by engaging the user in observing marine animals, while Karuna Virtual Embodiment Training promotes physical movement in patients with upper-extremity chronic pain and is based on the principles of graded motor imagery. On the other hand, applications such as: Creed: Rise to Glory, The Avengers: Powers Unite, and The Climb, have been used in research to facilitate the embodiment of superhero-like avatars with the goal of improving body image dimensions such as perceptions of strength and vulnerability [25].
Studies indicate that using commercially available software can yield positive results in treating musculoskeletal conditions. For example, a study by Cetin et al., (2022) [93] demonstrated that, for patients with chronic neck pain, VR interventions using Ocean Rift and Gala 360 software were more effective than traditional motor control exercises in reducing joint position sense error, functional limitations, and increasing pain pressure thresholds. In another study, Garcia et al., (2021) [124] found that EaseVRx led to high user satisfaction and produced clinically meaningful reductions in average pain intensity and pain-related interference with activities, mood, and stress for patients with chronic low back pain when compared to a sham VR intervention. Similarly, Sarkar et al., (2022) [95] explored the effects of VR meditation using the Guided Meditation VR app by Cubicle Ninjas on knee osteoarthritis, showing significant moderate to large analgesic effects on knee pain intensity both during and post-VR, with some pain relief lasting into the following day.
To achieve specific research objectives, some studies design their own software programs. For example, in the study by Sarig Bahat et al., (2015) [106], the researchers developed a custom software for kinematic training tailored for patients with chronic neck pain. In another study, Stamm et al., (2022) [127] created an application called ViRST VR, designed for patients with chronic lower back pain, where participants perform interactive tasks on a virtual farm—such as rowing, turning on light bulbs, or sorting vegetables—to promote movement and engagement.
Since there is currently a limited availability of VR software on the market that addresses the specific needs of patients with diverse musculoskeletal disorders, some authors emphasize that caution is needed when adapting commercially available applications (particularly those originally developed for the entertainment industry) for use in patient care settings. Zhou et al., (2023) [77] argue that highly vivid and realistic virtual environments, which transmit substantial sensory information through visuals, sounds and touch can overwhelm the senses, particularly if designed as fast-paced, high-stimulation video games. Additionally, Zhou et al., (2023) [77] note that many video games are structured with levels that require completing tasks to advance. For chronic pain patients, prolonged immersion in VR environments designed as never-ending level-based games may counteract therapeutic goals, potentially overstimulating the brain rather than promoting the desired calming effects [77]. Other authors emphasize that commercially available VR games often promote nonspecific, and at times undesirable, movements, lack patient-specific customization options, and may lead to frustration for individuals with motor impairments [128].
The limitations of commercially available VR games also extend to their restricted utilization of specific VR mechanisms. Most off-the-shelf games are primarily applied in studies for purposes such as education, relaxation, distraction from pain and enhancing patient engagement. However, these applications fall short of achieving the more targeted therapeutic effects that VR has the potential to offer. For instance, when using VR for pain distraction during exercise, a common challenge is that many commercially available games promote only single-joint movements or repetitive actions. This limitation makes it difficult to replace a comprehensive exercise program with a single VR game that adequately supports the diverse range of movements necessary for individual patients. Consequently, VR can often supplement only a portion of the exercise regimen, with additional exercises needing to be performed outside the VR environment to ensure a complete therapeutic approach. Furthermore, VR technology allows for manipulation of somatosensory input, enabling therapists to display movements in the VR environment that a patient may be unable to perform in reality, or to adjust the perceived range of movement by making it appear understated or exaggerated, as demonstrated in studies with neck pain patients by Kragting et al., (2023) [14] and Harvie et al., (2020) [24]. Creating bodily illusions through VR can be especially beneficial in modifying patients’ movement, body or pain perceptions, offering therapeutic advantages for individuals with musculoskeletal conditions, particularly those with kinesiophobia, altered body perception or chronic pain [14,129,130]. However, we have not encountered any applications on the market that incorporate body illusions specifically for patients with musculoskeletal conditions or chronic pain. Although Mirage Lab offers tools for creating bodily illusions, these experiences are not fully immersive but rather fall within AR, primarily aimed at research purposes and focused on illusions for the hand, as described on their website [131]. Companies that market VR software for therapy and rehabilitation in chronic pain and musculoskeletal conditions tend to focus on VR for exercise interventions (e.g., cardio, range of motion improvement, strength training, or graded exposure therapy), with examples including, but not limited to, Corpus VR, XRHealth, SyncVRMedical, KineQuantum, Neuro Rehab VR, Dynamics VR, KarunaHOME and Virtualis. Others concentrate on pain education, such as XRHealth, Reality Health, Dynamics VR, RelieveVRx, KarunaHOME and Reducept, while some provide programs for meditation, relaxation, or stress management, including Neuro Rehab VR, Corpus VR, XRHealth, VRelax, RelieveVRx, and Dynamics VR. Some applications, such as RelieveVRx are designed to help patients develop the skill of shifting their focus away from pain.
It appears that there is still considerable opportunity for the VR software market in musculoskeletal rehabilitation to expand, as it is currently underrepresented and lacks comprehensive solutions tailored to specific health conditions. Therefore, it would be beneficial for future development efforts to focus on creating more specialized, integrated software solutions that address the unique therapeutic needs of musculoskeletal patients.
It is important to note that many companies offering software for patients, and advertising their programs as suitable for specific musculoskeletal conditions, often do not provide detailed information about the software content (e.g., the specific movements patients perform during use). Companies identified on the market typically offer demo versions of their software, but access to these demos generally requires contacting each company individually. This lack of detailed information from companies about their software content limits the ability to obtain a comprehensive overview of the market offerings. For the purpose of this market review, we did not reach out to each company individually to inquire about specific software details; instead, we relied on information available on company websites and descriptions provided in studies that utilize these programs. Consequently, there may be gaps in our overview, and certain relevant details might have been unintentionally overlooked.
Supplementary Table S2 provides an overview of the hardware and software utilized in studies investigating the application of immersive VR for musculoskeletal conditions.
5. Key Organizations Advancing Virtual Reality in Healthcare and Rehabilitation
In our exploration of VR associations within the healthcare and rehabilitation sector, XR4REHAB [132] and the International Society for Virtual Rehabilitation (ISVR) [133] emerge as leading organizations dedicated to advancing VR specifically in the fields of rehabilitation and physiotherapy. XR4REHAB focuses on optimizing rehabilitation protocols for patients and their therapists. Researchers and clinical personnel at XR4REHAB work together to create VR interventions that offer patients challenging experiences designed to improve rehabilitation protocols, speed up recovery, encourage adherence to treatment, and facilitate reintegration into daily life. Their goal is to stimulate the development of VR-based rehabilitation tools by uniting relevant stakeholders and facilitating knowledge exchange. Similarly, ISVR has a mission to encourage research, education, advocacy, and enhanced collaboration among researchers, clinicians, industry, and policymakers within the fields of virtual rehabilitation and tele-rehabilitation. ISVR aims to achieve its goals through scientific meetings, tutorials, publications, web postings, awards, sponsored pilot research, and various information exchange opportunities.
Other associations are also engaged in healthcare and therapeutic VR applications. The American Medical Extended Reality Association’s (AMXRA) [134] mission is to advance the science and practice of medical XR through advancing care delivery, scientific investigation, innovation, education, advocacy, and community. Similarly, the International Industry Society in Advanced Rehabilitation Technology (IISART) [135] is dedicated to advancing and promoting modern healthcare technology in rehabilitation for the benefit of patients and society. IISART represents the interests of developers, manufacturers, and marketers of medical devices and equipment, as well as healthcare providers in the fields of robotics, virtual rehabilitation, and therapeutic electrical stimulation. Additionally, the International Virtual Reality and Healthcare Association (IVRHA) [136] is a member-driven organization comprising entities throughout the healthcare ecosystem, including technology companies, teaching hospitals, universities, healthcare providers, and insurance companies. IVRHA’s mission is to facilitate and support the growth of VR in healthcare as this emerging platform impacts practitioners and patients alike.
Other organizations include healthcare within their scope but maintain a broader focus. EuroXR Association [137] is an umbrella organization that brings together individuals, national chapters, associations, large companies, small-to-medium enterprises, research institutions, universities, and laboratories, all with a strong interest in XR. The XR Association (XRA) [138] advocates for XR’s responsible development and adoption, representing the global XR ecosystem, from hardware manufacturers to enterprise solution providers. The VR/AR Association (VRARA) [139] facilitates collaboration between XR providers and end-users, supporting growth and innovation across various sectors, including healthcare, as seen through their events.
VR for Health [140] stands out as a unique content platform rather than a traditional association. This platform is dedicated to raising awareness about wellness and therapeutic VR applications, providing educational resources, curated videos, and articles that make it a valuable resource for patients and healthcare providers. Similarly, the Virtual Reality Society (VRS) [141] is a source of VR information, from comprehensive material for beginners, to interesting and deep discussions of VR’s problems, implications and applications. Additionally, Virtual Reality Marketing (VRM) [142] functions as a platform connecting brands with skilled XR creators.
6. Conclusions and Future Directions
In this article, we explored the challenges in VR terminology and the current state of hardware and software for immersive VR, particularly in the context of its application in musculoskeletal rehabilitation and chronic pain management. We identified considerable confusion in the terminology surrounding VR and related technologies, highlighting the need for authors to clearly define what they include under the term VR and how they interpret it in their studies. To contribute to a clearer understanding of VR, we proposed a framework categorizing VR immersion based on exteroceptive and interoceptive system involvement, as well as the quality and number of senses stimulated, aligning the concept of VR with modern technology. Additionally, we advocated for excluding “non-immersive VR” experiences from the VR category and proposed renaming them “non-immersive fully artificial environments”. While reviewing hardware and software, we identified a lack of solutions specifically tailored for healthcare, emphasizing the need for future development. Current software solutions often fail to leverage VR’s full potential mechanisms, such as its impact on kinesiophobia and body image through the use of body illusions or body-swapping techniques, highlighting the need for the development of additional software solutions in the field of musculoskeletal rehabilitation. Future research should prioritize providing detailed descriptions of the technologies and methods used, including clear indications of the type of equipment (e.g., HMD headsets or 2D screens), the nature of the environment (interactive or non-interactive) and the intended purpose of use. These details should ideally be included in the title or abstract of studies to enhance clarity and standardization. Efforts to achieve a consensus on VR terminology should continue, as a standardized approach would greatly benefit the consistency and comparability of future research. Furthermore, the development of VR technologies specifically designed for healthcare should be encouraged, addressing the current gap in solutions tailored to the needs of patients. Such advancements could enable more effective interventions targeting issues like kinesiophobia and altered body perception, which are critical in musculoskeletal rehabilitation and associated chronic pain. Finally, clinical implementation of these findings requires collaborative efforts between researchers, clinicians, and technology developers to ensure that VR systems are not only innovative but also practical, accessible, and aligned with the demands of modern healthcare. In addition to addressing these research and practical gaps, we also highlighted the contributions of key associations in advancing VR in healthcare. These organizations provide valuable resources, facilitate collaboration, and support the integration of VR technologies into clinical practice. By fostering partnerships and prioritizing healthcare-specific VR developments, the field can move closer to realizing the full potential of VR in improving outcomes for patients with musculoskeletal conditions and chronic pain.
Supplementary Materials
The following supporting information can be downloaded at https://www.mdpi.com/article/10.3390/app15052564/s1: Table S1: Definitions and descriptions of virtual reality in studies on musculoskeletal conditions. Table S2: Hardware and software used in studies on immersive virtual reality for musculoskeletal conditions [2,4,19,32,34,35,36,47,49,52,53,56,60,67,70,71,76,77,89,90,92,93,94,95,96,97,98,100,101,102,103,104,105,106,124,125,127,143,144,145,146,147,148,149,150,151,152,153,154,155,156,157,158,159,160,161,162,163,164,165,166,167,168,169,170,171,172,173,174,175,176,177,178,179,180,181,182,183,184,185,186,187,188,189,190,191,192,193,194,195,196,197,198,199,200,201,202,203,204,205,206,207,208,209,210,211,212,213,214,215,216,217,218,219,220,221,222,223].
Author Contributions
Conceptualization, M.O.Z. and N.Š.; investigation, M.O.Z.; resources, N.Š.; writing—original draft preparation, M.O.Z.; writing—review and editing, N.Š. and M.O.Z.; visualization, M.O.Z.; supervision, N.Š.; project administration, N.Š.; funding acquisition, N.Š. All authors have read and agreed to the published version of the manuscript.
Funding
This research was financially supported by the Slovenian Research and Innovation Agency (research program KINSPO—Kinesiology for the effectiveness and prevention of musculoskeletal injuries in sports (P5-0443) and grant number 58589 for junior researcher Manca Opara Zupančič).
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
No new data were generated for this paper (review).
Acknowledgments
The authors used AI tools (ChatGPT, version 4o, OpenAI, San Francisco, CA) to correct minor grammatical errors. The tool was not used to analyze the literature or draw insights from papers as part of the review process. After using this tool/service, the authors reviewed and edited the content as needed, and they take full responsibility for the content of the publication.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Hoffman, H.G.; Chambers, G.T.; Meyer, W.J.; Arceneaux, L.L.; Russell, W.J.; Seibel, E.J.; Richards, T.L.; Sharar, S.R.; Patterson, D.R. Virtual Reality as an Adjunctive Non-Pharmacologic Analgesic for Acute Burn Pain during Medical Procedures. Ann. Behav. Med. 2011, 41, 183–191. [Google Scholar] [CrossRef]
- Noble, T.; Boone, L.; El Helou, A. The Role of Virtual Reality as Adjunctive Therapy to Spinal Cord Stimulation in Chronic Pain: A Feasible Concept? Front. Pain Res. 2023, 4, 1094125. [Google Scholar] [CrossRef]
- Padilla-Castañeda, M.A.; Sotgiu, E.; Barsotti, M.; Frisoli, A.; Orsini, P.; Martiradonna, A.; Laddaga, C.; Bergamasco, M. An Orthopaedic Robotic-Assisted Rehabilitation Method of the Forearm in Virtual Reality Physiotherapy. J. Healthc. Eng. 2018, 2018, 7438609. [Google Scholar] [CrossRef] [PubMed]
- Chaplin, E.; Karatzios, C.; Benaim, C. Clinical Applications of Virtual Reality in Musculoskeletal Rehabilitation: A Scoping Review. Healthcare 2023, 11, 3178. [Google Scholar] [CrossRef] [PubMed]
- Kouijzer, M.M.T.E.; Kip, H.; Bouman, Y.H.A.; Kelders, S.M. Implementation of Virtual Reality in Healthcare: A Scoping Review on the Implementation Process of Virtual Reality in Various Healthcare Settings. Implement. Sci. Commun. 2023, 4, 67. [Google Scholar] [CrossRef] [PubMed]
- Fatoye, F.; Gebrye, T.; Mbada, C.E.; Fatoye, C.T.; Makinde, M.O.; Ayomide, S.; Ige, B. Cost Effectiveness of Virtual Reality Game Compared to Clinic Based McKenzie Extension Therapy for Chronic Non-Specific Low Back Pain. Br. J. Pain 2022, 16, 601–609. [Google Scholar] [CrossRef] [PubMed]
- Edwards, R.R.; Dworkin, R.H.; Sullivan, M.D.; Turk, D.C.; Wasan, A.D. The Role of Psychosocial Processes in the Development and Maintenance of Chronic Pain. J. Pain 2016, 17, T70–T92. [Google Scholar] [CrossRef]
- Filardo, G.; Roffi, A.; Merli, G.; Marcacci, T.; Ceroni, F.B.; Raboni, D.; Bortolotti, B.; De Pasqual, L.; Marcacci, M. Patient Kinesiophobia Affects Both Recovery Time and Final Outcome after Total Knee Arthroplasty. Knee Surg. Sports Traumatol. Arthrosc. 2016, 24, 3322–3328. [Google Scholar] [CrossRef]
- Chimenti, R.L.; Pacha, M.S.; Glass, N.A.; Frazier, M.; Bowles, A.O.; Valantine, A.D.; Archer, K.R.; Wilken, J.M. Elevated Kinesiophobia Is Associated with Reduced Recovery from Lower Extremity Musculoskeletal Injuries in Military and Civilian Cohorts. Phys. Ther. 2022, 102, pzab262. [Google Scholar] [CrossRef]
- Everhart, J.S.; Best, T.M.; Flanigan, D.C. Psychological Predictors of Anterior Cruciate Ligament Reconstruction Outcomes: A Systematic Review. Knee Surg. Sports Traumatol. Arthrosc. 2015, 23, 752–762. [Google Scholar] [CrossRef]
- La Touche, R.; Pardo-Montero, J.; Grande-Alonso, M.; Paris-Alemany, A.; Miñambres-Martín, D.; Nouvilas-Pallejà, E. Psychological, Pain, and Disability Factors Influencing the Perception of Improvement/Recovery from Physiotherapy in Patients with Chronic Musculoskeletal Pain: A Cross-Sectional Study. Healthcare 2023, 12, 12. [Google Scholar] [CrossRef] [PubMed]
- Farin, E.; Gramm, L.; Schmidt, E. The Patient–Physician Relationship in Patients with Chronic Low Back Pain as a Predictor of Outcomes after Rehabilitation. J. Behav. Med. 2013, 36, 246–258. [Google Scholar] [CrossRef] [PubMed]
- Moseley, G.L.; Flor, H. Targeting Cortical Representations in the Treatment of Chronic Pain. Neurorehabil. Neural Repair 2012, 26, 646–652. [Google Scholar] [CrossRef]
- Kragting, M.; Voogt, L.; Coppieters, M.W.; Pool-Goudzwaard, A.L. Visual Feedback Manipulation in Virtual Reality to Influence Pain-Free Range of Motion. Are People with Non-Specific Neck Pain Who Are Fearful of Movement More Susceptible? PLoS ONE 2023, 18, e0287907. [Google Scholar] [CrossRef] [PubMed]
- Coja, D.M.; Talaghir, L.G.; Georgescu, L.; Codreanu, C.M. Effectiveness of Virtual Reality in Reducing Kinesiophobia. A Systematic Review. Balneo PRM Res. J. 2023, 14, 629. [Google Scholar] [CrossRef]
- Malloy, K.M.; Milling, L.S. The Effectiveness of Virtual Reality Distraction for Pain Reduction: A Systematic Review. Clin. Psychol. Rev. 2010, 30, 1011–1018. [Google Scholar] [CrossRef]
- Kato, P.M. Video Games in Health Care: Closing the Gap. Rev. Gen. Psychol. 2010, 14, 113–121. [Google Scholar] [CrossRef]
- Zhang, C.; Yu, S. The Technology to Enhance Patient Motivation in Virtual Reality Rehabilitation: A Review. Games Health J. 2024, 13, 215–233. [Google Scholar] [CrossRef]
- Ahmadpour, N.; Randall, H.; Choksi, H.; Gao, A.; Vaughan, C.; Poronnik, P. Virtual Reality Interventions for Acute and Chronic Pain Management. Int. J. Biochem. Cell Biol. 2019, 114, 105568. [Google Scholar] [CrossRef]
- Maselli, A.; Slater, M. The Building Blocks of the Full Body Ownership Illusion. Front. Hum. Neurosci. 2013, 7, 83. [Google Scholar] [CrossRef]
- Lin, J.-H.T.; Wu, D.-Y.; Yang, J.-W. Exercising with a Six Pack in Virtual Reality: Examining the Proteus Effect of Avatar Body Shape and Sex on Self-Efficacy for Core-Muscle Exercise, Self-Concept of Body Shape, and Actual Physical Activity. Front. Psychol. 2021, 12, 693543. [Google Scholar] [CrossRef] [PubMed]
- Yee, N.; Bailenson, J. The Proteus Effect: The Effect of Transformed Self-Representation on Behavior. Hum. Commun. Res. 2007, 33, 271–290. [Google Scholar] [CrossRef]
- Yee, N.; Bailenson, J.N.; Ducheneaut, N. The Proteus Effect: Implications of Transformed Digital Self-Representation on Online and Offline Behavior. Commun. Res. 2009, 36, 285–312. [Google Scholar] [CrossRef]
- Harvie, D.S.; Rio, E.; Smith, R.T.; Olthof, N.; Coppieters, M.W. Virtual Reality Body Image Training for Chronic Low Back Pain: A Single Case Report. Front. Virtual Real. 2020, 1, 13. [Google Scholar] [CrossRef]
- Harvie, D.S.; Kelly, J.; Kluver, J.; Deen, M.; Spitzer, E.; Coppieters, M.W. A Randomized Controlled Pilot Study Examining Immediate Effects of Embodying a Virtual Reality Superhero in People with Chronic Low Back Pain. Disabil. Rehabil. Assist. Technol. 2024, 19, 851–858. [Google Scholar] [CrossRef]
- Senkowski, D.; Heinz, A. Chronic Pain and Distorted Body Image: Implications for Multisensory Feedback Interventions. Neurosci. Biobehav. Rev. 2016, 69, 252–259. [Google Scholar] [CrossRef]
- Sündermann, O.; Flink, I.; Linton, S.J. My Body Is Not Working Right: A Cognitive Behavioral Model of Body Image and Chronic Pain. Pain 2020, 161, 1136–1139. [Google Scholar] [CrossRef]
- Opara, M.; Kozinc, Ž. Which Muscles Exhibit Increased Stiffness in People with Chronic Neck Pain? A Systematic Review with Meta-Analysis. Front. Sports Act. Living 2023, 5, 1172514. [Google Scholar] [CrossRef]
- Cortés-Pérez, I.; Desdentado-Guillem, J.M.; Camacho-Delgado, M.S.; Del Rocío Ibancos-Losada, M.; Obrero-Gaitán, E.; Lomas-Vega, R. Virtual Reality-Based Therapy after Anterior Cruciate Ligament Injury Effectively Reduces Pain and Improves Knee Function, Movement Patterns, and Dynamic Balance: A Systematic Review and Meta-Analysis. Knee Surg. Sports Traumatol. Arthrosc. 2024. early view. [Google Scholar] [CrossRef]
- Su, S.; Wang, R.; Chen, Z.; Zhou, F.; Zhang, Y. The Effectiveness of Extended Reality on Relieving Pain after Total Knee Arthroplasty: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Arch. Orthop. Trauma Surg. 2024, 144, 3217–3226. [Google Scholar] [CrossRef]
- Kumar, V.; Vatkar, A.J.; Kataria, M.; Dhatt, S.S.; Baburaj, V. Virtual Reality Is Effective in the Management of Chronic Low Back Ache in Adults: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Eur. Spine J. 2024, 33, 474–480. [Google Scholar] [CrossRef]
- Li, R.; Li, Y.; Kong, Y.; Li, H.; Hu, D.; Fu, C.; Wei, Q. Virtual Reality-Based Training in Chronic Low Back Pain: Systematic Review and Meta-Analysis of Randomized Controlled Trials. J. Med. Internet Res. 2024, 26, e45406. [Google Scholar] [CrossRef] [PubMed]
- Ye, G.; Koh, R.G.L.; Jaiswal, K.; Soomal, H.; Kumbhare, D. The Use of Virtual Reality in the Rehabilitation of Chronic Nonspecific Neck Pain: A Systematic Review and Meta-Analysis. Clin. J. Pain 2023, 39, 491–500. [Google Scholar] [CrossRef] [PubMed]
- Elaraby, A.E.R.; Shahien, M.; Jahan, A.M.; Etoom, M.; Bekhet, A.H. The Efficacy of Virtual Reality Training in the Rehabilitation of Orthopedic Ankle Injuries: A Systematic Review and Meta-Analysis. Adv. Rehabil. Sci. Pract. 2023, 12, 11795727231151636. [Google Scholar] [CrossRef] [PubMed]
- García-Sánchez, M.; García-Robles, P.; Osuna-Pérez, M.C.; Lomas-Vega, R.; Obrero-Gaitán, E.; Cortés-Pérez, I. Effectiveness of Virtual Reality-Based Early Postoperative Rehabilitation after Total Knee Arthroplasty: A Systematic Review with Meta-Analysis of Randomized Controlled Trials. Appl. Sci. 2023, 13, 4597. [Google Scholar] [CrossRef]
- Wei, W.; Tang, H.; Luo, Y.; Yan, S.; Ji, Q.; Liu, Z.; Li, H.; Wu, F.; Yang, S.; Yang, X. Efficacy of Virtual Reality Exercise in Knee Osteoarthritis Rehabilitation: A Systematic Review and Meta-Analysis. Front. Physiol. 2024, 15, 1424815. [Google Scholar] [CrossRef]
- Opara, M.; Kozinc, Ž. Virtual Reality Training for Management of Chronic Neck Pain: A Systematic Review with Meta-Analysis. Eur. J. Physiother. 2024, 26, 135–147. [Google Scholar] [CrossRef]
- Opara, M.; Kozinc, Ž.; Ivezić, D.M. Effects of Virtual Reality on Pain, Disability and Kinesiophobia in Patients with Chronic Low Back Pain: A Systematic Review with Meta-Analysis. Physiother. Pract. Res. 2024, 45, 107–132. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. BMJ 2021, 372, n71. [Google Scholar] [CrossRef]
- Rauschnabel, P.A.; Felix, R.; Hinsch, C.; Shahab, H.; Alt, F. What Is XR? Towards a Framework for Augmented and Virtual Reality. Comput. Human Behav. 2022, 133, 107289. [Google Scholar] [CrossRef]
- Laato, S.; Xi, N.; Spors, V.; Thibault, M.; Hamari, J. Making Sense of Reality: A Mapping of Terminology Related to Virtual Reality, Augmented Reality, Mixed Reality, XR and the Metaverse. In Proceedings of the 57th Hawaii International Conference on System Sciences, Waikiki, HI, USA, 3–6 January 2024; pp. 6625–6634. [Google Scholar]
- Skarbez, R.; Smith, M.; Whitton, M.C. Revisiting Milgram and Kishino’s Reality-Virtuality Continuum. Front. Virtual Real. 2021, 2, 647997. [Google Scholar] [CrossRef]
- Abbas, J.R.; O’Connor, A.; Ganapathy, E.; Isba, R.; Payton, A.; McGrath, B.; Tolley, N.; Bruce, I.A. What Is Virtual Reality? A Healthcare-Focused Systematic Review of Definitions. Health Policy Technol. 2023, 12, 100741. [Google Scholar] [CrossRef]
- Fijačko, N.; Štiglic, G.; Gsaxner, C.; Chang, T.P.; Greif, R. Rethinking Realities: A Call for Accurate Terminology in EXtended Reality Studies. Resusc. Plus 2024, 17, 100558. [Google Scholar] [CrossRef]
- Apple Vision Pro. Available online: https://www.apple.com/apple-vision-pro/ (accessed on 10 December 2024).
- Kordyaka, B.; Park, S.; Krath, J.; Laato, S. Exploring the Relationship Between Offline Cultural Environments and Toxic Behavior Tendencies in Multiplayer Online Games. ACM Trans. Soc. Comput. 2023, 6, 1–20. [Google Scholar] [CrossRef]
- Gava, V.; Fialho, H.R.F.; Calixtre, L.B.; Barbosa, G.M.; Kamonseki, D.H. Effects of Gaming on Pain-Related Fear, Pain Catastrophizing, Anxiety, and Depression in Patients with Chronic Musculoskeletal Pain: A Systematic Review and Meta-Analysis. Games Health J. 2022, 11, 369–384. [Google Scholar] [CrossRef]
- Andreae, M.H. Virtual Reality in Rehabilitation. BMJ 1996, 312, 4–5. [Google Scholar] [CrossRef]
- Darnall, B.D.; Krishnamurthy, P.; Tsuei, J.; Minor, J.D. Self-Administered Skills-Based Virtual Reality Intervention for Chronic Pain: Randomized Controlled Pilot Study. JMIR Form. Res. 2020, 4, e17293. [Google Scholar] [CrossRef]
- Fu, H.; Garrett, B.; Tao, G.; Cordingley, E.; Ofoghi, Z.; Taverner, T.; Sun, C.; Cheung, T. Virtual Reality–Guided Meditation for Chronic Pain in Patients With Cancer: Exploratory Analysis of Electroencephalograph Activity. JMIR Biomed. Eng. 2021, 6, e26332. [Google Scholar] [CrossRef]
- Nambi, G.; Abdelbasset, W.K.; Alsubaie, S.F.; Saleh, A.K.; Verma, A.; Abdelaziz, M.A.; Alkathiry, A.A. Short-Term Psychological and Hormonal Effects of Virtual Reality Training on Chronic Low Back Pain in Soccer Players. J. Sport Rehabil. 2021, 30, 884–893. [Google Scholar] [CrossRef]
- Afzal, M.W.; Ahmad, A.; Mohseni Bandpei, M.A.; Gillani, S.A.; Hanif, A.; Sharif Waqas, M. Effects of Virtual Reality Exercises and Routine Physical Therapy on Pain Intensity and Functional Disability in Patients with Chronic Low Back Pain. J. Pak. Med. Assoc. 2022, 72, 413–417. [Google Scholar] [CrossRef]
- Rezaei, I.; Razeghi, M.; Ebrahimi, S.; Kayedi, S.; Rezaeian Zadeh, A. A Novel Virtual Reality Technique (Cervigame®) Compared to Conventional Proprioceptive Training to Treat Neck Pain: A Randomized Controlled Trial. J. Biomed. Phys. Eng. 2018, 9, 355–366. [Google Scholar] [CrossRef] [PubMed]
- Oliveira, L.K.R.; Marques, A.P.; Andrade, K.F.A.; de Assis, J.C.S.; Brito, A.L.; Souza, G.S.; Callegari, B. Virtual Reality in Improving Anticipatory Postural Adjustments to Step Initiation in Individuals with Knee Osteoarthritis: A Randomized Controlled Trial. Games Health J. 2024, 13, 100–108. [Google Scholar] [CrossRef] [PubMed]
- Henríquez-Jurado, J.M.; Osuna-Pérez, M.C.; García-López, H.; Lomas-Vega, R.; López-Ruiz, M.d.C.; Obrero-Gaitán, E.; Cortés-Pérez, I. Virtual Reality-Based Therapy for Chronic Low Back and Neck Pain: A Systematic Review with Meta-Analysis. EFORT Open Rev. 2024, 9, 685–699. [Google Scholar] [CrossRef] [PubMed]
- García-Sánchez, M.; Obrero-Gaitán, E.; Piñar-Lara, M.; Osuna-Pérez, M.C.; Díaz-Fernández, Á.; Cortés-Pérez, I. Early Rehabilitation Using Virtual Reality-Based Therapy Can Enhance Hip Function and Self-Perception of Improvement Following Total Hip Arthroplasty: A Systematic Review and Meta-Analysis. Geriatr. Nurs. 2024, 60, 593–601. [Google Scholar] [CrossRef]
- Myers, R.L.; Laenger, C.J. Virtual Reality in Rehabilitation. Disabil. Rehabil. 1998, 20, 111–112. [Google Scholar] [CrossRef]
- Wilson, P.N.; Foreman, N.; Stanton, D. Virtual Reality, Disability and Rehabilitation. Disabil. Rehabil. 1997, 19, 213–220. [Google Scholar] [CrossRef]
- Skarbez, R.; Smith, M.; Whitton, M. It Is Time to Let Go of “Virtual Reality”. Commun. ACM 2023, 66, 41–43. [Google Scholar] [CrossRef]
- Schuermans, J.; Van Hootegem, A.; Van den Bossche, M.; Van Gendt, M.; Witvrouw, E.; Wezenbeek, E. Extended Reality in Musculoskeletal Rehabilitation and Injury Prevention—A Systematic Review. Phys. Ther. Sport. 2022, 55, 229–240. [Google Scholar] [CrossRef]
- Ziker, C.; Truman, B.; Dodds, H. Cross Reality (XR): Challenges and Opportunities Across the Spectrum. In Innovative Learning Environments in STEM Higher Education; Springer: Cham, Switzerland, 2021; pp. 55–77. [Google Scholar]
- Yang, Y.; Keivanpour, S.; Imbeau, D. Integrating X-Reality and Lean into End-of-Life Aircraft Parts Disassembly Sequence Planning: A Critical Review and Research Agenda. Int. J. Adv. Manuf. Technol. 2023, 127, 2181–2210. [Google Scholar] [CrossRef]
- Gaballa, A.; Cavalcante, R.S.; Lamounier, E.; Soares, A.; Cabibihan, J.-J. Extended Reality “X-Reality” for Prosthesis Training of Upper-Limb Amputees: A Review on Current and Future Clinical Potential. IEEE Trans. Neural Syst. Rehabil. Eng. 2022, 30, 1652–1663. [Google Scholar] [CrossRef]
- Cheung, J.C.-W.; Cheung, D.S.K.; Ni, M.; Chen, K.-W.; Mao, Y.-J.; Feng, L.; Lam, W.-K.; Wong, D.W.-C.; Leung, A.K.-L. X-Reality for Phantom Limb Management for Amputees: A Systematic Review and Meta-Analysis. Eng. Regen. 2023, 4, 134–151. [Google Scholar] [CrossRef]
- Combalia, A.; Sanchez-Vives, M.V.; Donegan, T. Immersive Virtual Reality in Orthopaedics—A Narrative Review. Int. Orthop. 2024, 48, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Favre, J.; Cantaloube, A.; Jolles, B.M. Rehabilitation for Musculoskeletal Disorders: The Emergence of Serious Games and the Promise of Personalized Versions Using Artificial Intelligence. J. Clin. Med. 2023, 12, 5310. [Google Scholar] [CrossRef] [PubMed]
- Moreau, S.; Thérond, A.; Cerda, I.H.; Studer, K.; Pan, A.; Tharpe, J.; Crowther, J.E.; Abd-Elsayed, A.; Gilligan, C.; Tolba, R.; et al. Virtual Reality in Acute and Chronic Pain Medicine: An Updated Review. Curr. Pain Headache Rep. 2024, 28, 893–928. [Google Scholar] [CrossRef]
- Milgram, P.; Kishino, F. A Taxonomy of Mixed Reality Visual Displays. IEICE Trans. Inf. Syst. 1994, 12, 1321–1329. [Google Scholar]
- Wilkinson, M.; Brantley, S.; Feng, J. A Mini Review of Presence and Immersion in Virtual Reality. Proc. Human Factors Ergon. Soc. Annu. Meet. 2021, 65, 1099–1103. [Google Scholar] [CrossRef]
- Brady, N.; Dejaco, B.; Lewis, J.; McCreesh, K.; McVeigh, J.G. Physiotherapist Beliefs and Perspectives on Virtual Reality Supported Rehabilitation for the Management of Musculoskeletal Shoulder Pain: A Focus Group Study. PLoS ONE 2023, 18, e0284445. [Google Scholar] [CrossRef]
- Thuilier, E.; Carey, J.; Dempsey, M.; Dingliana, J.; Whelan, B.; Brennan, A. Virtual Rehabilitation for Patients with Osteoporosis or Other Musculoskeletal Disorders: A Systematic Review. Virtual Real. 2024, 28, 93. [Google Scholar] [CrossRef]
- Chirico, A.; Lucidi, F.; De Laurentiis, M.; Milanese, C.; Napoli, A.; Giordano, A. Virtual Reality in Health System: Beyond Entertainment. A Mini-Review on the Efficacy of VR During Cancer Treatment. J. Cell Physiol. 2016, 231, 275–287. [Google Scholar] [CrossRef]
- Manlapaz, D.G.; Sole, G.; Jayakaran, P.; Chapple, C.M. Exergaming to Improve Balance and Decrease the Risk of Falling in Adults with Knee Osteoarthritis: A Mixed-Methods Feasibility Study. Physiother. Theory Pract. 2022, 38, 2428–2440. [Google Scholar] [CrossRef]
- Mete, E.; Sari, Z. The Efficacy of Exergaming in Patients with Knee Osteoarthritis: A Randomized Controlled Clinical Trial. Physiother. Res. Int. 2022, 27, e1952. [Google Scholar] [CrossRef] [PubMed]
- Abd-Alrazaq, A.; Al-Jafar, E.; Alajlani, M.; Toro, C.; Alhuwail, D.; Ahmed, A.; Reagu, S.M.; Al-Shorbaji, N.; Househ, M. The Effectiveness of Serious Games for Alleviating Depression: Systematic Review and Meta-Analysis. JMIR Serious Games 2022, 10, e32331. [Google Scholar] [CrossRef] [PubMed]
- Hadjiat, Y.; Marchand, S. Virtual Reality and the Mediation of Acute and Chronic Pain in Adult and Pediatric Populations: Research Developments. Front. Pain Res. 2022, 3, 840921. [Google Scholar] [CrossRef]
- Zhou, S.; Gromala, D.; Wang, L. Ethical Challenges of Virtual Reality Technology Interventions for the Vulnerabilities of Patients With Chronic Pain: Exploration of Technician Responsibility. J. Med. Internet Res. 2023, 25, e49237. [Google Scholar] [CrossRef]
- Pallavicini, F.; Pepe, A.; Minissi, M.E. Gaming in Virtual Reality: What Changes in Terms of Usability, Emotional Response and Sense of Presence Compared to Non-Immersive Video Games? Simul. Gaming 2019, 50, 136–159. [Google Scholar] [CrossRef]
- Di Lernia, D.; Zaccaro, A.; Herman, A.M.; Villani, V.; Finotti, G.; Costantini, M.; Ferri, F.; Tsakiris, M.; Riva, G. Sonoception: Synthetic Auditory Stimulation of the Insula Alters Proxies of Interoceptive Processing at Behavioral and Cortical Levels. PsyArXiv Preprints 2023. [Google Scholar] [CrossRef]
- Di Lernia, D.; Lacerenza, M.; Ainley, V.; Riva, G. Altered Interoceptive Perception and the Effects of Interoceptive Analgesia in Musculoskeletal, Primary, and Neuropathic Chronic Pain Conditions. J. Pers. Med. 2020, 10, 201. [Google Scholar] [CrossRef]
- Björnsdotter, M.; Morrison, I.; Olausson, H. Feeling Good: On the Role of C Fiber Mediated Touch in Interoception. Exp. Brain Res. 2010, 207, 149–155. [Google Scholar] [CrossRef]
- Iodice, P.; Porciello, G.; Bufalari, I.; Barca, L.; Pezzulo, G. An Interoceptive Illusion of Effort Induced by False Heart-Rate Feedback. Proc. Natl. Acad. Sci. USA 2019, 116, 13897–13902. [Google Scholar] [CrossRef]
- Riva, G.; Wiederhold, B.K.; Mantovani, F. Neuroscience of Virtual Reality: From Virtual Exposure to Embodied Medicine. Cyberpsychol. Behav. Soc. Netw. 2019, 22, 82–96. [Google Scholar] [CrossRef]
- Weber, S.; Weibel, D.; Mast, F.W. How to Get There When You Are There Already? Defining Presence in Virtual Reality and the Importance of Perceived Realism. Front. Psychol. 2021, 12, 628298. [Google Scholar] [CrossRef] [PubMed]
- Meta Platforms. Available online: https://www.meta.com/ (accessed on 10 December 2024).
- PICO Interactive. Available online: https://www.picoxr.com/global (accessed on 10 December 2024).
- Varjo Technologies Oy. Available online: https://varjo.com/ (accessed on 10 December 2024).
- HTC Corporation. Available online: https://www.vive.com/eu/ (accessed on 10 December 2024).
- Groenveld, T.D.; Smits, M.L.M.; Knoop, J.; Kallewaard, J.W.; Staal, J.B.; de Vries, M.; van Goor, H. Effect of a Behavioral Therapy-Based Virtual Reality Application on Quality of Life in Chronic Low Back Pain. Clin. J. Pain 2023, 39, 278–285. [Google Scholar] [CrossRef] [PubMed]
- Brown, L.; DiCenso-Fleming, T.; Ensign, T.; Boyd, A.J.; Monaghan, G.; Binder, D.S. Chronic Pain Education Delivered with a Virtual Reality Headset in Outpatient Physical Therapy Clinics: A Multi-Site Exploratory Trial. Am. J. Transl. Res. 2023, 15, 3500–3510. [Google Scholar] [PubMed]
- Liikkanen, S.; Mäkinen, M.; Huttunen, T.; Sarapohja, T.; Stenfors, C.; Eccleston, C. Body Movement as a Biomarker for Use in Chronic Pain Rehabilitation: An Embedded Analysis of an RCT of a Virtual Reality Solution for Adults with Chronic Pain. Front. Pain Res. 2022, 3, 1085791. [Google Scholar] [CrossRef] [PubMed]
- Eccleston, C.; Fisher, E.; Liikkanen, S.; Sarapohja, T.; Stenfors, C.; Jääskeläinen, S.K.; Rice, A.S.C.; Mattila, L.; Blom, T.; Bratty, J.R. A Prospective, Double-Blind, Pilot, Randomized, Controlled Trial of an “Embodied” Virtual Reality Intervention for Adults with Low Back Pain. Pain 2022, 163, 1700–1715. [Google Scholar] [CrossRef]
- Cetin, H.; Kose, N.; Oge, H.K. Virtual Reality and Motor Control Exercises to Treat Chronic Neck Pain: A Randomized Controlled Trial. Musculoskelet. Sci. Pract. 2022, 62, 102636. [Google Scholar] [CrossRef]
- Sarig Bahat, H.; Croft, K.; Carter, C.; Hoddinott, A.; Sprecher, E.; Treleaven, J. Remote Kinematic Training for Patients with Chronic Neck Pain: A Randomised Controlled Trial. Eur. Spine J. 2018, 27, 1309–1323. [Google Scholar] [CrossRef]
- Sarkar, T.D.; Edwards, R.R.; Baker, N. The Feasibility and Effectiveness of Virtual Reality Meditation on Reducing Chronic Pain for Older Adults with Knee Osteoarthritis. Pain Pract. 2022, 22, 631–641. [Google Scholar] [CrossRef]
- Fowler, C.A.; Ballistrea, L.M.; Mazzone, K.E.; Martin, A.M.; Kaplan, H.; Kip, K.E.; Ralston, K.; Murphy, J.L.; Winkler, S.L. Virtual Reality as a Therapy Adjunct for Fear of Movement in Veterans With Chronic Pain: Single-Arm Feasibility Study. JMIR Form. Res. 2019, 3, e11266. [Google Scholar] [CrossRef]
- Garrett, B.; Taverner, T.; McDade, P. Virtual Reality as an Adjunct Home Therapy in Chronic Pain Management: An Exploratory Study. JMIR Med. Inform. 2017, 5, e11. [Google Scholar] [CrossRef]
- Brown, P.; Powell, W.; Dansey, N.; Al-Abbadey, M.; Stevens, B.; Powell, V. Virtual Reality as a Pain Distraction Modality for Experimentally Induced Pain in a Chronic Pain Population: An Exploratory Study. Cyberpsychol Behav. Soc. Netw. 2022, 25, 66–71. [Google Scholar] [CrossRef] [PubMed]
- Matthie, N.; Higgins, M.; Doorenbos, A.; Maddox, T.; Jenerette, C. Feasibility of In-Home Virtual Reality for Chronic Pain in Sickle Cell Disease. Pain Manag. Nurs. 2024, 25, 425–431. [Google Scholar] [CrossRef] [PubMed]
- Safy, O.; Rousseaux, F.; Faymonville, M.-E.; Libbrecht, D.; Fontaine, R.; Raaf, M.; Staquet, C.; Tasset, H.; Bonhomme, V.; Vanhaudenhuyse, A.; et al. Virtual Reality Hypnosis Prior to Radiofrequency Thermocoagulation for Patients with Chronic Pain: An Exploratory Clinical Trial. Front. Psychol. 2024, 15, 1331826. [Google Scholar] [CrossRef]
- Mazurek, J.; Cieślik, B.; Wrzeciono, A.; Gajda, R.; Szczepańska-Gieracha, J. Immersive Virtual Reality Therapy Is Supportive for Orthopedic Rehabilitation among the Elderly: A Randomized Controlled Trial. J. Clin. Med. 2023, 12, 7681. [Google Scholar] [CrossRef]
- Saby, A.; Alvarez, A.; Smolins, D.; Petros, J.; Nguyen, L.; Trujillo, M.; Aygün, O. Effects of Embodiment in Virtual Reality for Treatment of Chronic Pain: Pilot Open-Label Study. JMIR Form. Res. 2024, 8, e34162. [Google Scholar] [CrossRef]
- Yalfani, A.; Abedi, M.; Raeisi, Z. Effects of an 8-Week Virtual Reality Training Program on Pain, Fall Risk, and Quality of Life in Elderly Women with Chronic Low Back Pain: Double-Blind Randomized Clinical Trial. Games Health J. 2022, 11, 85–92. [Google Scholar] [CrossRef]
- Fuchs, L.; Kluska, A.; Novak, D.; Kosashvili, Y. The Influence of Early Virtual Reality Intervention on Pain, Anxiety, and Function Following Primary Total Knee Arthroplasty. Complement. Ther. Clin. Pract. 2022, 49, 101687. [Google Scholar] [CrossRef]
- Harvie, D.S.; Smith, R.T.; Moseley, G.L.; Meulders, A.; Michiels, B.; Sterling, M. Illusion-Enhanced Virtual Reality Exercise for Neck Pain. Clin. J. Pain 2020, 36, 101–109. [Google Scholar] [CrossRef]
- Sarig Bahat, H.; Takasaki, H.; Chen, X.; Bet-Or, Y.; Treleaven, J. Cervical Kinematic Training with and without Interactive VR Training for Chronic Neck Pain—A Randomized Clinical Trial. Man. Ther. 2015, 20, 68–78. [Google Scholar] [CrossRef]
- Yan, Y.; Chen, K.; Xie, Y.; Song, Y.; Liu, Y. The Effects of Weight on Comfort of Virtual Reality Devices. In Advances in Ergonomics in Design; Springer: Cham, Switzerland, 2019; pp. 239–248. [Google Scholar]
- Primax Innovation Inc. Available online: https://pimax.com/ (accessed on 10 December 2024).
- BHaptics Inc. Available online: https://www.bhaptics.com/tactsuit/ (accessed on 10 December 2024).
- HTC Corporation VIVE Full Face Tracker. Available online: https://www.vive.com/us/accessory/vive-full-face-tracker/ (accessed on 10 December 2024).
- MANUS Technology Group Metagloves Pro. Available online: https://www.manus-meta.com/products/metagloves-pro (accessed on 10 December 2024).
- HaptX Inc HaptX Gloves G1. Available online: https://haptx.com/gloves-g1/ (accessed on 10 December 2024).
- Mechatech Ltd. AGILEVR. Available online: https://www.mechatech.co.uk/agilevr (accessed on 10 December 2024).
- PICO Interactive PICO Motion Tracker. Available online: https://www.picoxr.com/global/products/pico-motion-tracker (accessed on 22 February 2025).
- Sony Electronics Inc Mobile Motion Capture for VR and 3D Contents Creation. Available online: https://electronics.sony.com/more/mocopi/all-mocopi/p/qmss1-uscx?srsltid=AfmBOoqRW7frPogXXWVl-ZFNG4s-oiSLNs8c7YI8OewzdIzged0TrYjq (accessed on 10 December 2024).
- Knoxlabs FirstVR - Muscle Displacement Controller. Available online: https://www.knoxlabs.com/products/firstvr-muscle-input-controller?srsltid=AfmBOopW335YC1EWb7D64W5_1QP2cxOmKmbzohjPIbVdnLarES042P4x (accessed on 10 December 2024).
- TESLASUIT TESLASUIT Dev Kit. Available online: https://teslasuit.io/products/teslasuit-4/ (accessed on 10 December 2024).
- HTC Corporation VIVE Tracker 3.0. Available online: https://www.vive.com/us/accessory/tracker3/ (accessed on 10 December 2024).
- Orbbec Inc Femto Bolt. Available online: https://www.orbbec.com/products/tof-camera/femto-bolt/ (accessed on 10 December 2024).
- Meta. Meta Quest 3S Breathable Facial Interface. Available online: https://www.meta.com/quest/accessories/quest-3s-breathable-facial-interface/?srsltid=AfmBOooPYEOcHGd0rxIzWlN8W1t3ISU_o25t4WT32pXS8lMFO3zG20-d (accessed on 10 December 2024).
- VR TierOne. UV-C Disinfection Cabinet for VR TierOne GO Headsets. Available online: https://vrtierone.com/products/uv-c-disinfection-cabinet-for-vr-tierone-go-headsets/ (accessed on 10 December 2024).
- Cyberith GmbH. Virtualizer ELITE 2. Available online: https://www.cyberith.com/virtualizer-elite/ (accessed on 10 December 2024).
- HTC Vive The VIVE Ultimate Tracker Is Now Third-Party Compatible! Available online: https://www.youtube.com/watch?v=3GXKXCTgNzI (accessed on 10 December 2024).
- Garcia, L.M.; Birckhead, B.J.; Krishnamurthy, P.; Sackman, J.; Mackey, I.G.; Louis, R.G.; Salmasi, V.; Maddox, T.; Darnall, B.D. An 8-Week Self-Administered At-Home Behavioral Skills-Based Virtual Reality Program for Chronic Low Back Pain: Double-Blind, Randomized, Placebo-Controlled Trial Conducted During COVID-19. J. Med. Internet Res. 2021, 23, e26292. [Google Scholar] [CrossRef]
- Dy, M.; Olazo, K.; Lyles, C.R.; Lisker, S.; Weinberg, J.; Lee, C.; Tarver, M.E.; Saha, A.; Kontson, K.; Araojo, R.; et al. Usability and Acceptability of Virtual Reality for Chronic Pain Management among Diverse Patients in a Safety-Net Setting: A Qualitative Analysis. JAMIA Open 2023, 6, ooad050. [Google Scholar] [CrossRef] [PubMed]
- Jones, T.; Moore, T.; Choo, J. The Impact of Virtual Reality on Chronic Pain. PLoS ONE 2016, 11, e0167523. [Google Scholar] [CrossRef] [PubMed]
- Stamm, O.; Dahms, R.; Reithinger, N.; Ruß, A.; Müller-Werdan, U. Virtual Reality Exergame for Supplementing Multimodal Pain Therapy in Older Adults with Chronic Back Pain: A Randomized Controlled Pilot Study. Virtual Real. 2022, 26, 1291–1305. [Google Scholar] [CrossRef] [PubMed]
- Krepkovich, E.; Kaur, M.; Mangum, L.C.; Saliba, S.; Lichter, M.; Olowin, A.; Richardson, N.; Hart, J. Feasibility of a Novel Video Game-Based Electromyography Biofeedback System in Patients With Knee Osteoarthritis. J. Sport Rehabil. 2022, 31, 937–942. [Google Scholar] [CrossRef]
- Stanton, T.R.; Gilpin, H.R.; Edwards, L.; Moseley, G.L.; Newport, R. Illusory Resizing of the Painful Knee Is Analgesic in Symptomatic Knee Osteoarthritis. PeerJ 2018, 6, e5206. [Google Scholar] [CrossRef]
- Lewis, J.S.; Newport, R.; Taylor, G.; Smith, M.; McCabe, C.S. Visual Illusions Modulate Body Perception Disturbance and Pain in Complex Regional Pain Syndrome: A Randomized Trial. Eur. J. Pain 2021, 25, 1551–1563. [Google Scholar] [CrossRef]
- MIRAGE Lab. About MIRAGE. Available online: https://miragemultisensoryillusions.wordpress.com/about/ (accessed on 10 December 2024).
- XR4REHAB. Available online: https://vr4rehab.org/ (accessed on 12 December 2024).
- International Society for Virtual Rehabilitation. Available online: https://isvr.org/ (accessed on 12 December 2024).
- The American Medical Extended Reality Association. Available online: https://amxra.org/ (accessed on 12 December 2024).
- International Industry Society in Advanced Rehabilitation Technology. Available online: https://iisart.org/ (accessed on 12 December 2024).
- International Virtual Reality Healthcare Association. Available online: https://ivrha.org/ (accessed on 12 December 2024).
- EuroXR Association. Available online: https://www.euroxr-association.org/ (accessed on 12 December 2024).
- XR Association. Available online: https://xra.org/ (accessed on 12 December 2024).
- The VR/AR Association. Available online: https://www.thevrara.com/ (accessed on 12 December 2024).
- VR for Health. Available online: https://vrforhealth.com/ (accessed on 12 December 2024).
- Virtual Reality Society. Available online: https://www.vrs.org.uk/ (accessed on 12 December 2024).
- Virtual Reality Marketing. Available online: https://go.virtualrealitymarketing.com/ (accessed on 12 December 2024).
- Lo, H.H.M.; Ng, M.; Fong, P.Y.H.; Lai, H.H.K.; Wang, B.; Wong, S.Y.; Sit, R.W.S. Examining the Feasibility, Acceptability, and Preliminary Efficacy of an Immersive Virtual Reality–Assisted Lower Limb Strength Training for Knee Osteoarthritis: Mixed Methods Pilot Randomized Controlled Trial. JMIR Serious Games 2024, 12, e52563. [Google Scholar] [CrossRef]
- Özlü, A.; Ünver, G.; Tuna, H.İ.; Menekşeoğlu, A.K. The Effect of a Virtual Reality-Mediated Gamified Rehabilitation Program on Pain, Disability, Function, and Balance in Knee Osteoarthritis: A Prospective Randomized Controlled Study. Games Health J. 2023, 12, 118–124. [Google Scholar] [CrossRef]
- Dod, V.; Phansopkar, P. Virtual Reality as Treatment Method for Knee Osteoarthritis—Short Review. J. Pharm. Negat. Results 2022, 2985–2988. [Google Scholar] [CrossRef]
- Barry, K.S.; Nimma, S.R.; Spaulding, A.C.; Wilke, B.K.; Torp, K.D.; Ledford, C.K. Perioperative Outcomes of Immersive Virtual Reality as Adjunct Anesthesia in Primary Total Hip and Knee Arthroplasty. Arthroplast. Today 2022, 18, 84–88. [Google Scholar] [CrossRef]
- Carella, M.; Beck, F.; Quoilin, C.; Azongmo, M.M.; Loheac, A.; Bonhomme, V.L.; Vanhaudenhuyse, A. Effect of Virtual Reality Hypnosis on Intraoperative Sedation Needs and Functional Recovery in Knee Arthroplasty: A Prospective Randomized Clinical Trial. Reg. Anesth. Pain Med. 2024, rapm-2023-105261. [Google Scholar] [CrossRef] [PubMed]
- Gür, O.; Başar, S. The Effect of Virtual Reality on Pain, Kinesiophobia and Function in Total Knee Arthroplasty Patients: A Randomized Controlled Trial. Knee 2023, 45, 187–197. [Google Scholar] [CrossRef] [PubMed]
- Hadamus, A.; Białoszewski, D.; Błażkiewicz, M.; Kowalska, A.J.; Urbaniak, E.; Wydra, K.T.; Wiaderna, K.; Boratyński, R.; Kobza, A.; Marczyński, W. Assessment of the Effectiveness of Rehabilitation after Total Knee Replacement Surgery Using Sample Entropy and Classical Measures of Body Balance. Entropy 2021, 23, 164. [Google Scholar] [CrossRef]
- Hong, S.; Lee, G. Effects of an Immersive Virtual Reality Environment on Muscle Strength, Proprioception, Balance, and Gait of a Middle-Aged Woman Who Had Total Knee Replacement: A Case Report. Am. J. Case Rep. 2019, 20, 1636–1642. [Google Scholar] [CrossRef]
- Pournajaf, S.; Goffredo, M.; Pellicciari, L.; Piscitelli, D.; Criscuolo, S.; Le Pera, D.; Damiani, C.; Franceschini, M. Effect of Balance Training Using Virtual Reality-Based Serious Games in Individuals with Total Knee Replacement: A Randomized Controlled Trial. Ann. Phys. Rehabil. Med. 2022, 65, 101609. [Google Scholar] [CrossRef]
- Su, C.-H. Developing and Evaluating Effectiveness of 3D Game-Based Rehabilitation System for Total Knee Replacement Rehabilitation Patients. Multimed. Tools Appl. 2016, 75, 10037–10057. [Google Scholar] [CrossRef]
- Gazendam, A.; Zhu, M.; Chang, Y.; Phillips, S.; Bhandari, M. Virtual Reality Rehabilitation Following Total Knee Arthroplasty: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Knee Surg. Sports Traumatol. Arthrosc. 2022, 30, 2548–2555. [Google Scholar] [CrossRef]
- Peng, L.; Zeng, Y.; Wu, Y.; Si, H.; Shen, B. Virtual Reality-Based Rehabilitation in Patients Following Total Knee Arthroplasty: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Chin. Med. J. 2022, 135, 153–163. [Google Scholar] [CrossRef]
- Su, S.; He, J.; Wang, R.; Chen, Z.; Zhou, F. The Effectiveness of Virtual Reality, Augmented Reality, and Mixed Reality Rehabilitation in Total Knee Arthroplasty: A Systematic Review and Meta-Analysis. J. Arthroplast. 2024, 39, 582–590.e4. [Google Scholar] [CrossRef]
- Su, S.; Wang, R.; Zhou, R.; Chen, Z.; Zhou, F. The Effectiveness of Virtual Reality, Augmented Reality, and Mixed Reality Training in Total Hip Arthroplasty: A Systematic Review and Meta-Analysis. J. Orthop. Surg. Res. 2023, 18, 121. [Google Scholar] [CrossRef]
- Araujo-Duran, J.; Kopac, O.; Montalvo Campana, M.; Bakal, O.; Sessler, D.I.; Hofstra, R.L.; Shah, K.; Turan, A.; Ayad, S. Virtual Reality Distraction for Reducing Acute Postoperative Pain After Hip Arthroplasty: A Randomized Trial. Anesth. Analg. 2023, 138, 751–759. [Google Scholar] [CrossRef] [PubMed]
- Berton, A.; Longo, U.G.; Candela, V.; Fioravanti, S.; Giannone, L.; Arcangeli, V.; Alciati, V.; Berton, C.; Facchinetti, G.; Marchetti, A.; et al. Virtual Reality, Augmented Reality, Gamification, and Telerehabilitation: Psychological Impact on Orthopedic Patients’ Rehabilitation. J. Clin. Med. 2020, 9, 2567. [Google Scholar] [CrossRef] [PubMed]
- Gumaa, M.; Rehan Youssef, A. Is Virtual Reality Effective in Orthopedic Rehabilitation? A Systematic Review and Meta-Analysis. Phys. Ther. 2019, 99, 1304–1325. [Google Scholar] [CrossRef] [PubMed]
- Jeyaraman, M.; Jeyaraman, N.; Ramasubramanian, S.; Shyam, A. Enhancing Orthopedic Rehabilitation: The Emergence and Impact of Virtual Reality Technology. J. Orthop. Case Rep. 2024, 14, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Kuroda, Y.; Young, M.; Shoman, H.; Punnoose, A.; Norrish, A.R.; Khanduja, V. Advanced Rehabilitation Technology in Orthopaedics—A Narrative Review. Int. Orthop. 2021, 45, 1933–1940. [Google Scholar] [CrossRef]
- Lal, H.; Mohanta, S.; Kumar, J.; Patralekh, M.K.; Lall, L.; Katariya, H.; Arya, R.K. Telemedicine-Rehabilitation and Virtual Reality in Orthopaedics and Sports Medicine. Indian J. Orthop. 2023, 57, 7–19. [Google Scholar] [CrossRef]
- Vuong, T.; Zhu, K.; Pastor, A. Virtual Reality as a Pain Control Adjunct in Orthopedics: A Narrative Review. Cureus 2024, 16, e66401. [Google Scholar] [CrossRef]
- Lin, H.-T.; Li, Y.-I.; Hu, W.-P.; Huang, C.-C.; Du, Y.-C. A Scoping Review of The Efficacy of Virtual Reality and Exergaming on Patients of Musculoskeletal System Disorder. J. Clin. Med. 2019, 8, 791. [Google Scholar] [CrossRef]
- Ditchburn, J.-L.; van Schaik, P.; Dixon, J.; MacSween, A.; Martin, D. The Effects of Exergaming on Pain, Postural Control, Technology Acceptance and Flow Experience in Older People with Chronic Musculoskeletal Pain: A Randomised Controlled Trial. BMC Sports Sci. Med. Rehabil. 2020, 12, 63. [Google Scholar] [CrossRef]
- Lo, H.H.M.; Zhu, M.; Zou, Z.; Wong, C.L.; Lo, S.H.S.; Chung, V.C.-H.; Wong, S.Y.-S.; Sit, R.W.S. Immersive and Nonimmersive Virtual Reality–Assisted Active Training in Chronic Musculoskeletal Pain: Systematic Review and Meta-Analysis. J. Med. Internet Res. 2024, 26, e48787. [Google Scholar] [CrossRef]
- Pretat, T.; Koller, C.; Hügle, T. Virtual Reality as a Treatment for Chronic Musculoskeletal Pain Syndromes. Jt. Bone Spine 2025, 92, 105769. [Google Scholar] [CrossRef]
- Borresen, A.; Wolfe, C.; Lin, C.-K.; Tian, Y.; Raghuraman, S.; Nahrstedt, K.; Prabhakaran, B.; Annaswamy, T. Usability of an Immersive Augmented Reality Based Telerehabilitation System with Haptics (ARTESH) for Synchronous Remote Musculoskeletal Examination. Int. J. Telerehabil. 2019, 11, 23–32. [Google Scholar] [CrossRef] [PubMed]
- Flórez Fonnegra, J.P.; Pino Prestan, A.C.; López, L.L.; Yepes, J.C.; Pérez, V.Z. Rehabilitation of Patients with Arthrogenic Muscular Inhibition in Pathologies of Knee Using Virtual Reality. Sensors 2023, 23, 9114. [Google Scholar] [CrossRef] [PubMed]
- Asadzadeh, A.; Salahzadeh, Z.; Samad-Soltani, T.; Rezaei-Hachesu, P. An Affordable and Immersive Virtual Reality-Based Exercise Therapy in Forward Head Posture. PLoS ONE 2024, 19, e0297863. [Google Scholar] [CrossRef] [PubMed]
- Yıldırım Şahan, T.; Aydoğan Arslan, S.; Demirci, C.; Oktaş, B.; Sertel, M. Comparison Of Short-Term Effects Of Virtual Reality and Short Foot Exercises in Pes Planus. Foot 2021, 47, 101778. [Google Scholar] [CrossRef] [PubMed]
- Shousha, T.M.; Abo-zaid, N.A.; Hamada, H.; Abdelhamid Abdelsamee, M.Y.; Behiry, M.A. Virtual Reality versus Biodex Training in Adolescents with Chronic Ankle Instability: A Randomized Controlled Trial. Arch. Med. Sci. 2021, 19, 1059. [Google Scholar] [CrossRef]
- Wang, E.F.; Jotwani, R. Virtual Reality Therapy for Myofascial Pain: Evolving towards an Evidence-Based Non-Pharmacologic Adjuvant Intervention. Interv. Pain Med. 2023, 2, 100181. [Google Scholar] [CrossRef]
- Carnevale, A.; Mannocchi, I.; Schena, E.; Carli, M.; Sassi, M.S.H.; Marino, M.; Longo, U.G. Performance Evaluation of an Immersive Virtual Reality Application for Rehabilitation after Arthroscopic Rotator Cuff Repair. Bioengineering 2023, 10, 1305. [Google Scholar] [CrossRef]
- Gsangaya, M.R.; Htwe, O.; Selvi Naicker, A.; Md Yusoff, B.A.H.; Mohammad, N.; Soh, E.Z.F.; Silvaraju, M. Comparison between the Effect of Immersive Virtual Reality Training versus Conventional Rehabilitation on Limb Loading and Functional Outcomes in Patients after Anterior Cruciate Ligament Reconstruction: A Prospective Randomized Controlled Trial. Asia Pac. J. Sports Med. Arthrosc. Rehabil. Technol. 2023, 34, 28–37. [Google Scholar] [CrossRef]
- Vogt, S.; Skjæret-Maroni, N.; Neuhaus, D.; Baumeister, J. Virtual Reality Interventions for Balance Prevention and Rehabilitation after Musculoskeletal Lower Limb Impairments in Young up to Middle-Aged Adults: A Comprehensive Review on Used Technology, Balance Outcome Measures and Observed Effects. Int. J. Med. Inform. 2019, 126, 46–58. [Google Scholar] [CrossRef]
- Emedoli, D.; Alemanno, F.; Iannaccone, S.; Houdayer, E.; Castellazzi, P.; Zangrillo, F.; Gasperotti, F.; Locatelli, M.; Tettamanti, A. Sensory-Motor Training with Virtual Reality as a Complementary Intervention to Manual Therapy for Persistent Non-Specific Neck Pain: A Randomized Controlled Trial. Eur. J. Phys. Rehabil. Med. 2024, 60, 680. [Google Scholar] [CrossRef] [PubMed]
- Tejera, D.; Beltran-Alacreu, H.; Cano-de-la-Cuerda, R.; Leon Hernández, J.V.; Martín-Pintado-Zugasti, A.; Calvo-Lobo, C.; Gil-Martínez, A.; Fernández-Carnero, J. Effects of Virtual Reality versus Exercise on Pain, Functional, Somatosensory and Psychosocial Outcomes in Patients with Non-Specific Chronic Neck Pain: A Randomized Clinical Trial. Int. J. Environ. Res. Public Health 2020, 17, 5950. [Google Scholar] [CrossRef] [PubMed]
- Hao, J.; He, Z.; Chen, Z.; Remis, A. Virtual Reality Training versus Conventional Rehabilitation for Chronic Neck Pain: A Systematic Review and Meta-analysis. PM&R 2024, 16, 1143–1153. [Google Scholar] [CrossRef]
- Orr, E.; Arbel, T.; Levy, M.; Sela, Y.; Weissberger, O.; Liran, O.; Lewis, J. Virtual Reality in the Management of Patients with Low Back and Neck Pain: A Retrospective Analysis of 82 People Treated Solely in the Metaverse. Arch. Physiother. 2023, 13, 11. [Google Scholar] [CrossRef]
- Ahern, M.M.; Dean, L.V.; Stoddard, C.C.; Agrawal, A.; Kim, K.; Cook, C.E.; Narciso Garcia, A. The Effectiveness of Virtual Reality in Patients with Spinal Pain: A Systematic Review and Meta-Analysis. Pain Pract. 2020, 20, 656–675. [Google Scholar] [CrossRef]
- Zhang, T.; Li, X.; Zhou, X.; Zhan, L.; Wu, F.; Huang, Z.; Sun, Y.; Feng, Y.; Du, Q. Virtual Reality Therapy for the Management of Chronic Spinal Pain: Systematic Review and Meta-Analysis. JMIR Serious Games 2024, 12, e50089. [Google Scholar] [CrossRef]
- Bordeleau, M.; Stamenkovic, A.; Tardif, P.-A.; Thomas, J. The Use of Virtual Reality in Back Pain Rehabilitation: A Systematic Review and Meta-Analysis. J. Pain 2022, 23, 175–195. [Google Scholar] [CrossRef]
- Slatman, S.; Ostelo, R.; van Goor, H.; Staal, J.B.; Knoop, J. Physiotherapy with Integrated Virtual Reality for Patients with Complex Chronic Low Back Pain: Protocol for a Pragmatic Cluster Randomized Controlled Trial (VARIETY Study). BMC Musculoskelet. Disord. 2023, 24, 132. [Google Scholar] [CrossRef]
- Slatman, S.; Groenveld, T.; Ostelo, R.; van Goor, H.; Staal, J.B.; Knoop, J. Development of a Multimodal, Personalized Intervention of Virtual Reality Integrated Within Physiotherapy for Patients with Complex Chronic Low-Back Pain. J. Med. Ext. Real. 2024, 1, 30–43. [Google Scholar] [CrossRef]
- Morone, G.; Papaioannou, F.; Alberti, A.; Ciancarelli, I.; Bonanno, M.; Calabrò, R.S. Efficacy of Sensor-Based Training Using Exergaming or Virtual Reality in Patients with Chronic Low Back Pain: A Systematic Review. Sensors 2024, 24, 6269. [Google Scholar] [CrossRef]
- Mortazavi, H. Virtual Reality: A Promising Non-Pharmacological Modality for Chronic Low Back Pain Management in Elderly. Korean J. Pain 2022, 35, 353–355. [Google Scholar] [CrossRef] [PubMed]
- Nagpal, A.S.; Raghunandan, A.; Tata, F.; Kibler, D.; McGeary, D. Virtual Reality in the Management of Chronic Low Back Pain: A Scoping Review. Front. Pain Res. 2022, 3, 856935. [Google Scholar] [CrossRef] [PubMed]
- Choi, T.; Heo, S.; Choi, W.; Lee, S. A Systematic Review and Meta-Analysis of the Effectiveness of Virtual Reality-Based Rehabilitation Therapy on Reducing the Degree of Pain Experienced by Individuals with Low Back Pain. Int. J. Environ. Res. Public Health 2023, 20, 3502. [Google Scholar] [CrossRef] [PubMed]
- Slatman, S.; Staal, J.B.; van Goor, H.; Ostelo, R.; Soer, R.; Knoop, J. Limited Use of Virtual Reality in Primary Care Physiotherapy for Patients with Chronic Pain. BMC Musculoskelet. Disord. 2024, 25, 168. [Google Scholar] [CrossRef]
- Guerra-Armas, J.; Flores-Cortes, M.; Pineda-Galan, C.; Luque-Suarez, A.; La Touche, R. Role of Immersive Virtual Reality in Motor Behaviour Decision-Making in Chronic Pain Patients. Brain Sci. 2023, 13, 617. [Google Scholar] [CrossRef]
- Austin, P.D. The Analgesic Effects of Virtual Reality for People with Chronic Pain: A Scoping Review. Pain Med. 2022, 23, 105–121. [Google Scholar] [CrossRef]
- Cerda, I.H.; Therond, A.; Moreau, S.; Studer, K.; Donjow, A.R.; Crowther, J.E.; Mazzolenis, M.E.; Lang, M.; Tolba, R.; Gilligan, C.; et al. Telehealth and Virtual Reality Technologies in Chronic Pain Management: A Narrative Review. Curr. Pain Headache Rep. 2024, 28, 83–94. [Google Scholar] [CrossRef]
- Chuan, A.; Zhou, J.J.; Hou, R.M.; Stevens, C.J.; Bogdanovych, A. Virtual Reality for Acute and Chronic Pain Management in Adult Patients: A Narrative Review. Anaesthesia 2021, 76, 695–704. [Google Scholar] [CrossRef]
- Goldsmith, E.; Anthony, M.; Landsteiner, A.; Ullman, K.; Kalinowski, C.; Zerzan, N.; Ewart, D.; Rich, T.; Miller, W.; Calvert, C.; et al. Extended Reality Interventions for Chronic Pain: A Systematic Review; Department of Veterans Affairs: Washington, DC, USA, 2024.
- Goudman, L.; Jansen, J.; Billot, M.; Vets, N.; De Smedt, A.; Roulaud, M.; Rigoard, P.; Moens, M. Virtual Reality Applications in Chronic Pain Management: Systematic Review and Meta-Analysis. JMIR Serious Games 2022, 10, e34402. [Google Scholar] [CrossRef]
- Grassini, S. Virtual Reality Assisted Non-Pharmacological Treatments in Chronic Pain Management: A Systematic Review and Quantitative Meta-Analysis. Int. J. Environ. Res. Public Health 2022, 19, 4071. [Google Scholar] [CrossRef]
- Matthie, N.S.; Giordano, N.A.; Jenerette, C.M.; Magwood, G.S.; Leslie, S.L.; Northey, E.E.; Webster, C.I.; Sil, S. Use And Efficacy Of Virtual, Augmented, Or Mixed Reality Technology For Chronic Pain: A Systematic Review. Pain Manag. 2022, 12, 859–878. [Google Scholar] [CrossRef] [PubMed]
- McGhee, W.R.G.; Doherty, C.J.; Graham-Wisener, L.; Fallis, R.; Stone, C.; Axiaq, A.; Dempster, M. Immersive Virtual Reality and Psychological Well-Being in Adult Chronic Physical Illness: Systematic Review. BMJ Support. Palliat. Care 2024, 14, 14–24. [Google Scholar] [CrossRef] [PubMed]
- O’Connor, S.; Mayne, A.; Hood, B. Virtual Reality-Based Mindfulness for Chronic Pain Management: A Scoping Review. Pain Manag. Nurs. 2022, 23, 359–369. [Google Scholar] [CrossRef]
- Shahrbanian, S.; Ma, X.; Korner-Bitensky, N.; Simmonds, M.J. Scientific Evidence for the Effectiveness of Virtual Reality for Pain Reduction in Adults with Acute or Chronic Pain. Stud. Health Technol. Inform. 2009, 144, 40–43. [Google Scholar]
- Skidmore, N.; Ryan, C.; Mankelow, J.; Bradford, C.; Graham, A.; Martin, D. Exploring the Potential of Virtual Reality for the Self-Management of Chronic Pain: A Scoping Review of Its Use to Address Health Literacy. Musculoskelet. Sci. Pract. 2024, 72, 102962. [Google Scholar] [CrossRef]
- Smith, A.; Wyles, K.J.; Hernandez, S.M.; Clarke, S.; Schofield, P.; Hughes, S.W. Harnessing the Therapeutic Effects of Nature for Chronic Pain: A Role for Immersive Virtual Reality? A Narrative Review. Eur. J. Pain 2025, 29, e4727. [Google Scholar] [CrossRef]
- Trost, Z.; Zielke, M.; Guck, A.; Nowlin, L.; Zakhidov, D.; France, C.R.; Keefe, F. The Promise and Challenge of Virtual Gaming Technologies for Chronic Pain: The Case of Graded Exposure for Low Back Pain. Pain Manag. 2015, 5, 197–206. [Google Scholar] [CrossRef]
- Wong, K.P.; Tse, M.M.Y.; Qin, J. Effectiveness of Virtual Reality-Based Interventions for Managing Chronic Pain on Pain Reduction, Anxiety, Depression and Mood: A Systematic Review. Healthcare 2022, 10, 2047. [Google Scholar] [CrossRef]
- Jin, C.; Feng, Y.; Ni, Y.; Shan, Z. Virtual Reality Intervention in Postoperative Rehabilitation after Total Knee Arthroplasty: A Prospective and Randomized Controlled Clinical Trial. Int. J. Clin. Exp. Med. 2018, 11, 6119–6124. [Google Scholar]
- Peuchot, H.; Khakha, R.; Riera, V.; Ollivier, M.; Argenson, J.-N. Intraoperative Virtual Reality Distraction in TKA under Spinal Anesthesia: A Preliminary Study. Arch. Orthop. Trauma Surg. 2021, 141, 2323–2328. [Google Scholar] [CrossRef]
- Prabhu, V.G.; Stanley, L.; Morgan, R. A Biofeedback Enhanced Adaptive Virtual Reality Environment for Managing Surgical Pain and Anxiety. Int. J. Semant. Comput. 2020, 14, 375–393. [Google Scholar] [CrossRef]
- Yoon, S.; Son, H. Effects of full immersion virtual reality training on balance and knee function in total knee replacement patients: A randomized controlled study. J. Mech. Med. Biol. 2020, 20, 2040007. [Google Scholar] [CrossRef]
- Sarig Bahat, H.; Hadar, D.; Treleaven, J. Predictors for Positive Response to Home Kinematic Training in Chronic Neck Pain. J. Manip. Physiol. Ther. 2020, 43, 779–790. [Google Scholar] [CrossRef] [PubMed]
- Cioeta, M.; Pournajaf, S.; Goffredo, M.; Giovannico, G.; Franceschini, M. Improving Adherence to a Home Rehabilitation Plan for Chronic Neck Pain through Immersive Virtual Reality: A Case Report. J. Clin. Med. 2023, 12, 1926. [Google Scholar] [CrossRef]
- Glavare, M.; Stålnacke, B.-M.; Häger, C.K.; Löfgren, M. Virtual Reality Exercises in an Interdisciplinary Rehabilitation Programme for Persons with Chronic Neck Pain: A Feasibility Study. J. Rehabil. Med. Clin. Commun. 2021, 4, 1000067. [Google Scholar] [CrossRef]
- Nusser, M.; Knapp, S.; Kramer, M.; Krischak, G. Effects of Virtual Reality-Based Neck-Specific Sensorimotor Training in Patients with Chronic Neck Pain: A Randomized Controlled Pilot Trial. J. Rehabil. Med. 2021, 53, jrm00151. [Google Scholar] [CrossRef]
- Zauderer, J.; Lefèvre-Colau, M.-M.; Davoine, É.; Hocquart, M.; Rannou, F.; Roby-Brami, A.; Nguyen, C.; Roren, A. Exercise Therapy Program Using Immersive Virtual Reality for People with Non-Specific Chronic Neck Pain: A 3-Month Retrospective Open Pilot and Feasibility Study. Ann. Phys. Rehabil. Med. 2022, 65, 101527. [Google Scholar] [CrossRef]
- Rose-Dulcina, K.; Dubessy, M.; Armand, S.; Genevay, S. Understanding the Flexion-Relaxation Phenomenon in Non-Specific Chronic Low Back Pain Patients Throught Immersive Virtual Reality Feedback Approach. Sci. Rep. 2024, 14, 15936. [Google Scholar] [CrossRef]
- MacIntyre, E.; Sigerseth, M.; Larsen, T.F.; Fersum, K.V.; Meulders, M.; Meulders, A.; Michiels, B.; Braithwaite, F.A.; Stanton, T.R. Get Your Head in the Game: A Replicated Single-Case Experimental Design Evaluating the Effect of a Novel Virtual Reality Intervention in People with Chronic Low Back Pain. J. Pain 2023, 24, 1449–1464. [Google Scholar] [CrossRef]
- McConnell, R.; Lane, E.; Webb, G.; LaPeze, D.; Grillo, H.; Fritz, J. A Multicenter Feasibility Randomized Controlled Trial Using a Virtual Reality Application of Pain Neuroscience Education for Adults with Chronic Low Back Pain. Ann. Med. 2024, 56, 2311846. [Google Scholar] [CrossRef]
- de Vries, F.S.; van Dongen, R.T.M.; Bertens, D. Pain Education and Pain Management Skills in Virtual Reality in the Treatment of Chronic Low Back Pain: A Multiple Baseline Single-Case Experimental Design. Behav. Res. Ther. 2023, 162, 104257. [Google Scholar] [CrossRef] [PubMed]
- Kawanishi, K.; Nakamoto, M.; Mityashita, T.; Ogita, S.; Kudo, S. Seated Virtual Reality-Guided Exercise Improved Gait in a Patient with Trunk Dysfunction Due to Hip Fracture: A Single-Case Design Study. Cureus 2024, 16, e62433. [Google Scholar] [CrossRef] [PubMed]
- Reilly, C.A.; Greeley, A.B.; Jevsevar, D.S.; Gitajn, I.L. Virtual Reality-Based Physical Therapy for Patients with Lower Extremity Injuries: Feasibility and Acceptability. OTA Int. 2021, 4, e132. [Google Scholar] [CrossRef] [PubMed]
- Elser, A.; Kopkow, C.; Schäfer, A.G. Implementation of a Virtual Reality Intervention in Outpatient Physiotherapy for Chronic Pain: Protocol for a Pilot Implementation Study. JMIR Res. Protoc. 2024, 13, e58089. [Google Scholar] [CrossRef]
- Tuck, N.; Pollard, C.; Good, C.; Williams, C.; Lewis, G.; Hames, M.; Aamir, T.; Bean, D. Active Virtual Reality for Chronic Primary Pain: Mixed Methods Randomized Pilot Study. JMIR Form. Res. 2022, 6, e38366. [Google Scholar] [CrossRef]
- Wiederhold, B.K.; Gao, K.; Sulea, C.; Wiederhold, M.D. Virtual Reality as a Distraction Technique in Chronic Pain Patients. Cyberpsychol. Behav. Soc. Netw. 2014, 17, 346–352. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).