Abstract
Background: Blood vessels have the Windkessel effect and are involved in blood circulation. The breakdown of this mechanism is also involved in the pathogenesis of heart failure (HF); however, the relationship between vascular dysfunction and HF prognosis is not fully understood. Methods: We evaluated 214 patients hospitalized for HF at our institution who underwent a cardio–ankle vascular index (CAVI), which evaluates vascular function, between January 2012 and July 2018. To investigate factors (including CAVI) associated with major adverse cardiac events (MACE) during 1 year after patients with HF were discharged, we evaluated clinical profiles, blood tests, chest X-P, 12-lead electrocardiography, and transthoracic echocardiographic findings. MACE was defined as cardiovascular death or readmission for HF. Results: The severity of HF between the MACE and non-MACE was not significantly different. Previous HF and chronic kidney disease were significantly more common in the MACE group. CAVI and % mean atrial pressure in the MACE group were statistically higher than those in the non-MACE group. The cardiac shadow as shown by chest X-P and left ventricular size in the MACE group were significantly bigger, and HF preserved ejection fraction (EF) (EF > 50%) was significantly more common in the MACE group. In multivariate analysis, CAVI was an independent predictive factor for the occurrence of MACE (model 1; hazard ratio (HR): 1.33, 95% confidence interval (CI): 1.05–1.68, p = 0.018; model 2; HR: 1.31, 95% CI: 1.07–1.60, p = 0.009). Conclusions: Because high CAVI is associated with poor prognosis of HF, these patients require more careful treatment.
1. Introduction
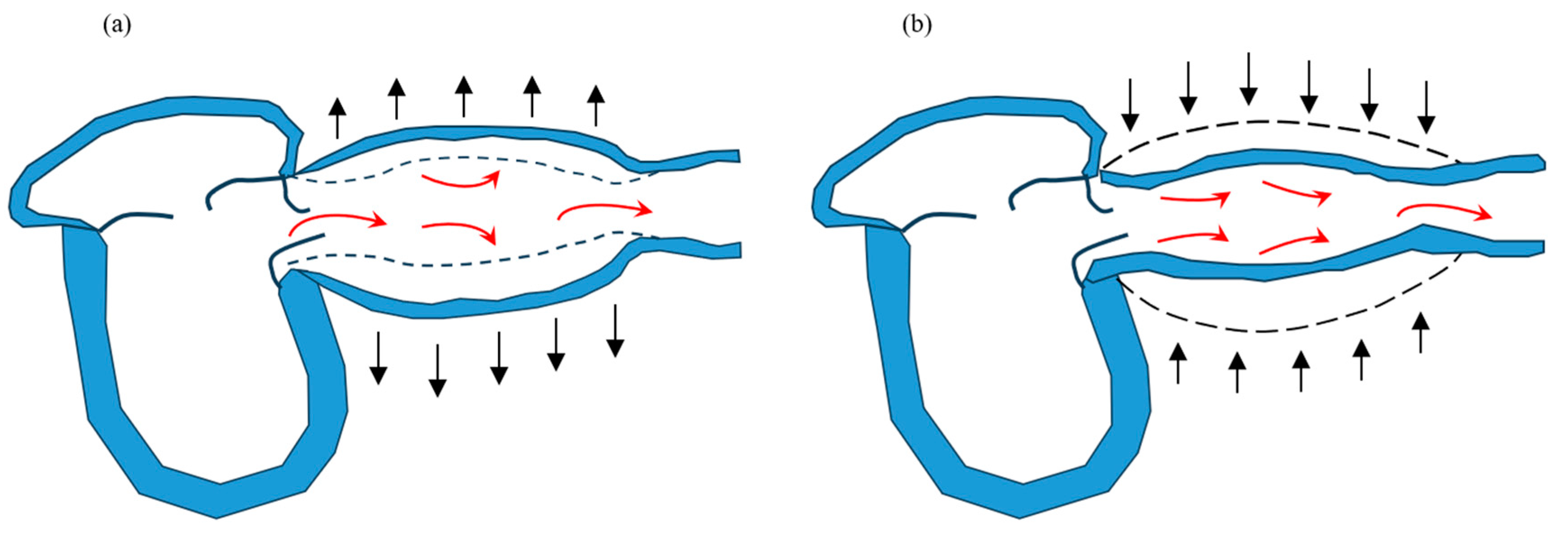
In Japan, the number of patients with heart failure (HF) is estimated to increase by approximately 1.3 million by 2030 [1]. The United States has approximately 6.7 million patients with HF; thus, HF is a worldwide problem [2]. Additionally, HF has high mortality and re-hospitalization rates, resulting in a poor long-term prognosis. Although HF treatment advances yearly, the mortality and re-hospitalization rates have not decreased over time in Japan [3]. Therefore, early prognostic assessment and timely appropriate treatment are important. Previous studies reported that the number of hospitalizations for HF, total bilirubin (T-Bil), improved contractility, and other factors were associated with poor prognosis [4,5,6]. By contrast, vascular function is also important in HF. Usually, during left ventricular systole, approximately 40% of the blood ejected from the left ventricle is stored in the arteries, and the remaining 60% flows to the periphery [7]. During left ventricular diastole, the stored blood (40%) flows to the periphery. This mechanism is called the Windkessel effect, and vascular dysfunction contributes to HF by the breakdown of the Windkessel effect (Figure 1). When the Windkessel effect collapses, the increase in afterload caused by the elevated systolic blood pressure (BP) exacerbates HF. However, the relationship between vascular dysfunction and the prognosis of HF is not fully understood. Therefore, we evaluated how each factor, including vascular function assessment, affected the 1-year prognosis after patients with HR were discharged.
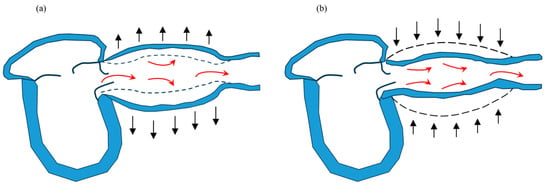
Figure 1.
The Windkessel effect. During cardiac systole, approximately 60% of the blood ejected from the left ventricle pools in blood vessels (a), and during cardiac diastole, the pooled blood returns to the periphery (b).
2. Materials and Methods
The present study was a single-center retrospective observational study in accordance with the Declaration of Helsinki (patients’ medical records were accessed for data collection). The study was approved by the Ethics Committee of Toho University Omori Medical Center (approval number: M21292_M18271_17318). The details of the study in opt-out format were posted on the website of our institution and our department (Department of Cardiovascular Medicine) and this acted as a waiver of informed consent from study participants. The subjects of the study were given the opportunity to decline to be enrolled.
2.1. Study Participants
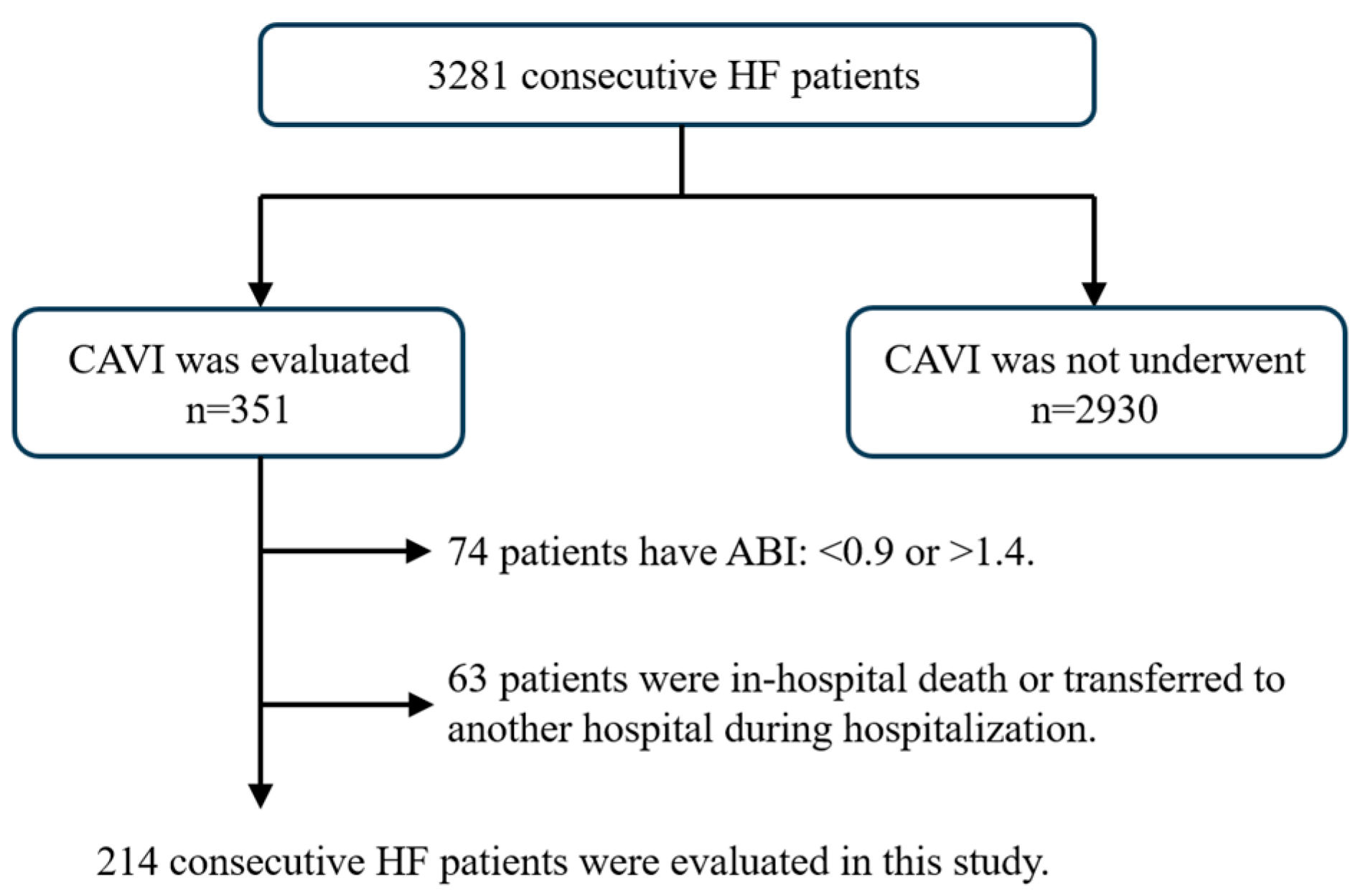
Figure 2 shows the subject flow chart of the present study. We evaluated 3281 consecutive patients hospitalized for HF at our institution between January 2012 and July 2018. HF was diagnosed based on the Framingham criteria or the guidelines of the American Heart Association or the European Society of Cardiology [8,9]. We investigated vascular function using CAVI and excluded patients whose ankle–brachial index (ABI) was <0.9 or >1.4. We also excluded patients with in-hospital death and those who transferred to another hospital and who could not be followed up for 1 year. The final cohort consisted of 214 patients.
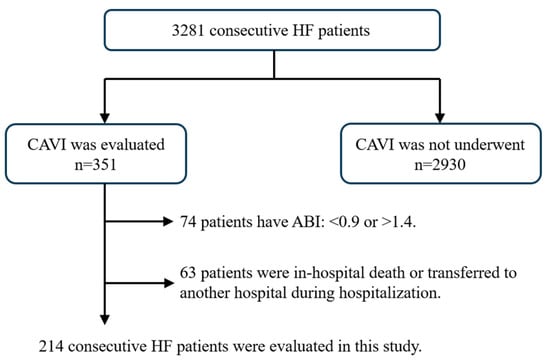
Figure 2.
Selection of study populations. This flow chart illustrates the selection method of the present study’s participants. Overall, 214 consecutive heart failure patients were analyzed.
2.2. Study Outcomes
The present study primarily aimed to investigate the factors (including CAVI) related to 1-year major adverse cardiac events (MACE) after patients with HF were discharged. MACE was defined as cardiovascular death or re-hospitalization with HF. We compared each factor (including CAVI) between the MACE and non-MACE groups. Multivariate analysis using the factors with statistically significant differences between the two groups was also performed. Furthermore, we created a receiver operating characteristic (ROC) curve of CAVI for predicting 1-year prognosis of HF, and a Kaplan–Meier curve was created using these values. Kaplan–Meier curves were also created for cardiovascular death or re-hospitalization with HF.
2.3. Patient Clinical Profiles
We investigated HF symptoms (New York Heart Association (NYHA) classification), length of hospital stay, and medications related to HF treatment at discharge. We evaluated the medications used for HF, such as beta-blockers (BBs), renin–angiotensin–aldosterone system inhibitors (RAS-Is), mineral corticoid receptor antagonists (MRAs), cardioprotective medications (BB, RAS-I, and MRA), and loop diuretics. Because the use of sodium glucose cotransporter (SGLT) 2 inhibitors had not been approved at the time of the study, we used triple therapy for cardioprotective therapy. Angiotensin-converting enzyme inhibitors or angiotensin II type 1a receptor blockers were considered as RAS-Is. Additionally, medical history and underlying heart disease were evaluated. We investigated hypertension (HT), diabetes mellitus, previous HF, and chronic kidney disease (CKD). Previous HF was defined as a history of previous hospitalization for HF. Underlying heart disease was classified into ischemic cardiomyopathy (ICM), hypertensive heart disease (HHD), valvular heart disease (VHD), tachycardia-induced cardiomyopathy (TIC), dilated cardiomyopathy (DCM), and others (including hypertrophic cardiomyopathy). Body mass index (BMI) was calculated using BMI = weight (kg)/height2 (m2), and we also evaluated physical features, such as age, sex, height, weight, and BMI.
2.4. BP and CAVI
We measured systolic and diastolic BP using an aneroid sphygmomanometer on admission and discharge [10]. The patients were divided into clinical scenario classifications (CS) of HF based on systolic BP at admission [11]. We calculated pulse pressure (PP) and mean BP using the following formula: PP = systolic BP − diastolic BP, mean BP, diastolic BP + PP/3. A nurse measured BPs during hospitalization three or more times (at 6:00, 10:00, 18:00, and other times). In-hospital BPV was evaluated using systolic BP (measured ≥ 8) for 3 days before discharge when the condition was stable. We calculated the coefficient of variation (CV) and standard deviation (SD) of systolic BP to evaluate in-hospital BP variability [12,13]. We defined CV as the within-patient SD divided by systolic BP. Heart rate (HR) was evaluated using standard 12-lead electrocardiography in the supine position on admission.
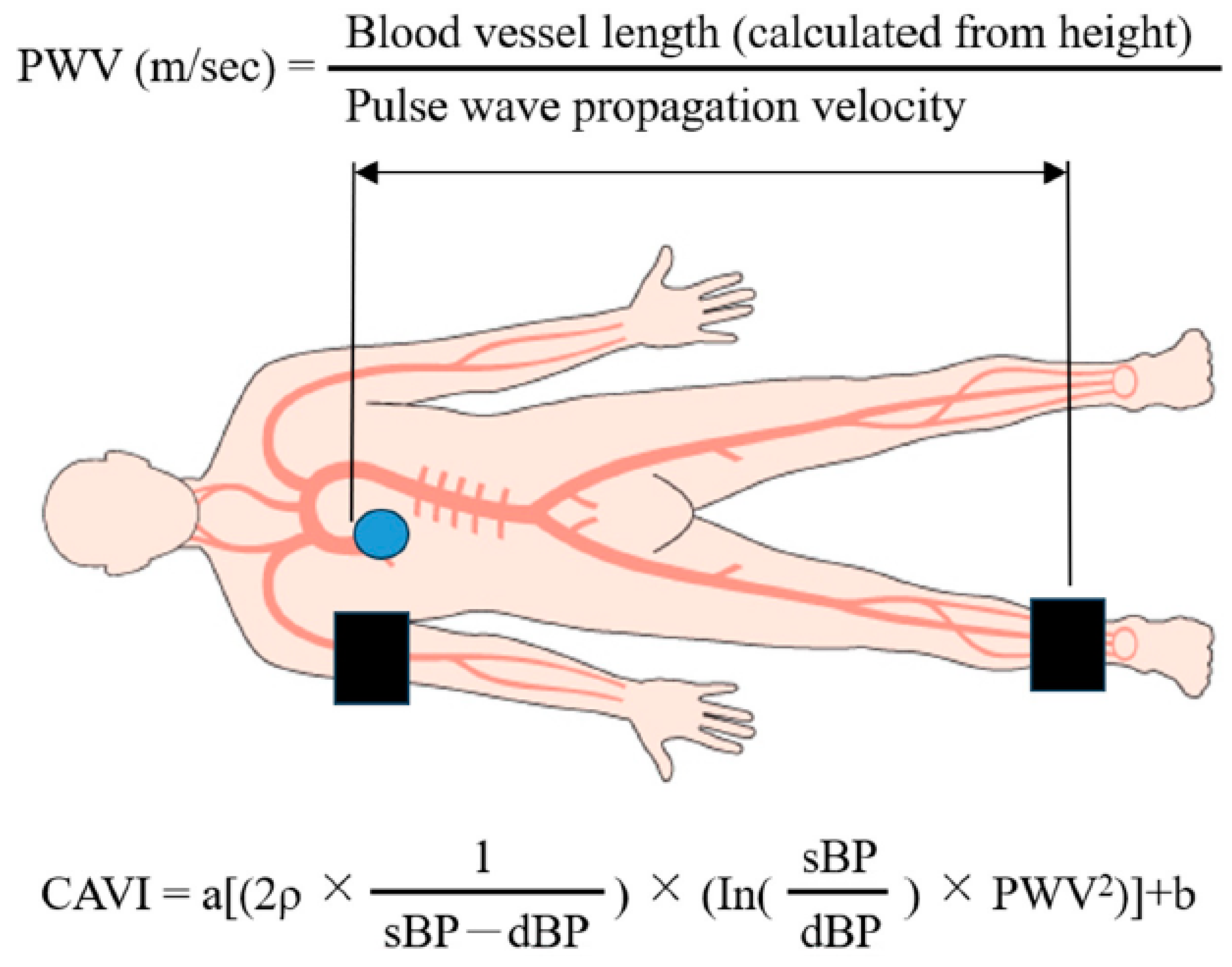
We measured ABI/CAVI using a VaSera VS-1500E (Fukuda Denshi Company, Ltd., Tokyo, Japan) after 12 h of fasting in the morning following HF improvement, which was defined as a general condition suitable for discharge. Pulse wave velocity (PWV) was calculated using the time taken for the pulse wave to travel from the aortic valve to the ankle [14]. Using PWV, the CAVI was calculated as follows: CAVI = a[(2ρ × 1/(sBP − dBP)) × (In(sBP/dBP) × PWV2)] + b, where ρ is blood density, and a and b are constants to match aortic PWV (Figure 3). The right and left CAVI mean values were measured, as well as upstroke time and % mean atrial pressure (% MAP).
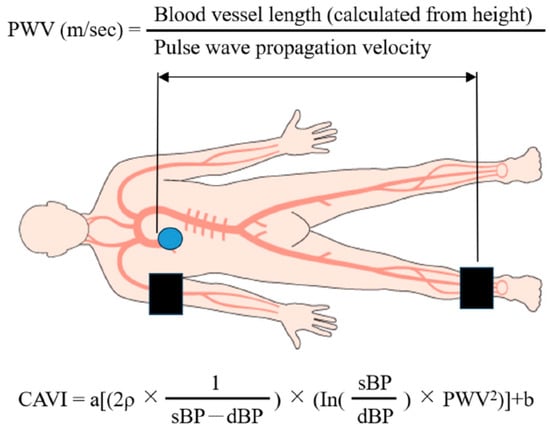
Figure 3.
Graphic illustration of the CAVI measurement method.
2.5. Other Clinical Examinations
Liver function (aspartate aminotransferase, alanine aminotransferase, and lactate dehydrogenase), renal function (JSNeGFR, blood urea nitrogen, and creatinine), hemoglobin (Hb), hematocrit, electrolytes (sodium and potassium), and brain natriuretic peptide (BNP) at admission were evaluated from laboratory examinations. Using the Japanese Society of Nephrology criteria, the JSNeGFR was calculated as JSNeGFR = 194 × Cr − 1.094 × age − 0.287 for men and 194 × Cr − 1.094 × age − 0.287 × 0.739 for women [15].
Two physicians blinded to the study evaluated the chest X-ray at admission to determine the cardiothoracic ratio (CTR). The CTR was calculated from the maximal cardiac and intrathoracic diameters.
We analyzed cardiac size, wall thickness, and left ventricle systolic function (ejection fraction: EF) from the transthoracic echocardiography performed by two physicians blinded to the present study. Cardiac size was measured using the left atrial dimension and left ventricular end-diastolic/-systolic dimensions, and interventricular septal and posterior left ventricular wall thicknesses at end-diastole were evaluated as wall thickness. We calculated the EF using either the modified Simpson method (apical two- or four-chamber view) or the Teichholz method (parasternal long-axis view) [16]. We also assessed the proportion of patients with HF reduced EF (HFrEF), HF mid-range EF (HFmrEF) and HF preserved EF (HFpEF). The Japan Circulation Society defines each type of HF as follows; HFrEF: EF ≦ 40%, HFmrEF: 40–50%, HFpEF: EF > 50%. [17].
2.6. Statistical Analysis
Data are presented as means ± SD. The unpaired Student’s t-test was used to compare the two groups. In all cases, differences with p value of <0.05 were considered statistically significant. We conducted multivariate analysis on factors that were found to be significant when compared between the two groups. Furthermore, the ROC curve was analyzed to determine an appropriate cutoff value of CAVI for predicting MACE. We used EZR (Saitama Medical Center, Jichi Medical University, Saitama, Japan), which is a graphical user interface for R (version 2.13.0, The R Foundation for Statistical Computing, Vienna, Austria) to conduct statistical analyses [18].
3. Results
3.1. Patient Backgrounds, Underlying Heart Disease, and HF Medications
Table 1 shows the patient characteristics of both groups. Compared with the non-MACE group, the MACE group was older, had a lower proportion of men, and had a smaller body size. Previous HF and CKD were also significantly more common in the MACE group.

Table 1.
Patient characteristics and medication at discharge in the MACE and non-MACE groups.
In the non-MACE group, underlying heart diseases were ICM (37 patients, 23.6%), HHD (42 patients, 26.8%), VHD (37 patients, 23.6%), TIC (15 patients, 9.6%), DCM (16 patients, 10.2%), and others (10 patients, 6.4%). The MACE group diseases comprised ICM (12 patients, 21.1%), HHD (9 patients, 15.8%), VHD (18 patients, 31.6%), TIC (5 patients, 8.8%), DCM (7 patients, 12.3%), and others (6 patients, 10.5%). The MACE and non-MACE groups had several cases of VHD and HHD, respectively.
The introduction rate of cardioprotective medications, including BB, RAS-I, and MRA, as well as loop diuretics and their dosage, showed no differences.
3.2. Differences in HF Condition, and Cardiac and Renal Functions
HF severity using NYHA and BNP were not significantly different between the two groups (Table 1 and Table 2). The pathological condition of HF expressed with CS also showed no differences. Table 2 shows the results of blood examinations. BUN and JSNeGFR were significantly different between the two groups, with worse renal function in the MACE group. Although Hb showed no difference, hematocrit was significantly lower in the MACE group than in the non-MACE group.

Table 2.
Laboratory and chest X-P findings in the MACE and non-MACE groups.
In the non-MACE group, the cardiac shadow using chest X-P was significantly smaller (Table 2), and the size of the left ventricle using transthoracic echocardiography was also significantly smaller (Table 3). Left ventricular systolic function evaluated by EF was similar in both groups; however, HFpEF (EF > 50%) was significantly more common in the MACE group (Table 3).

Table 3.
Transthoracic echocardiac findings in the MACE and non-MACE groups.
3.3. BP Evaluation and CAVI
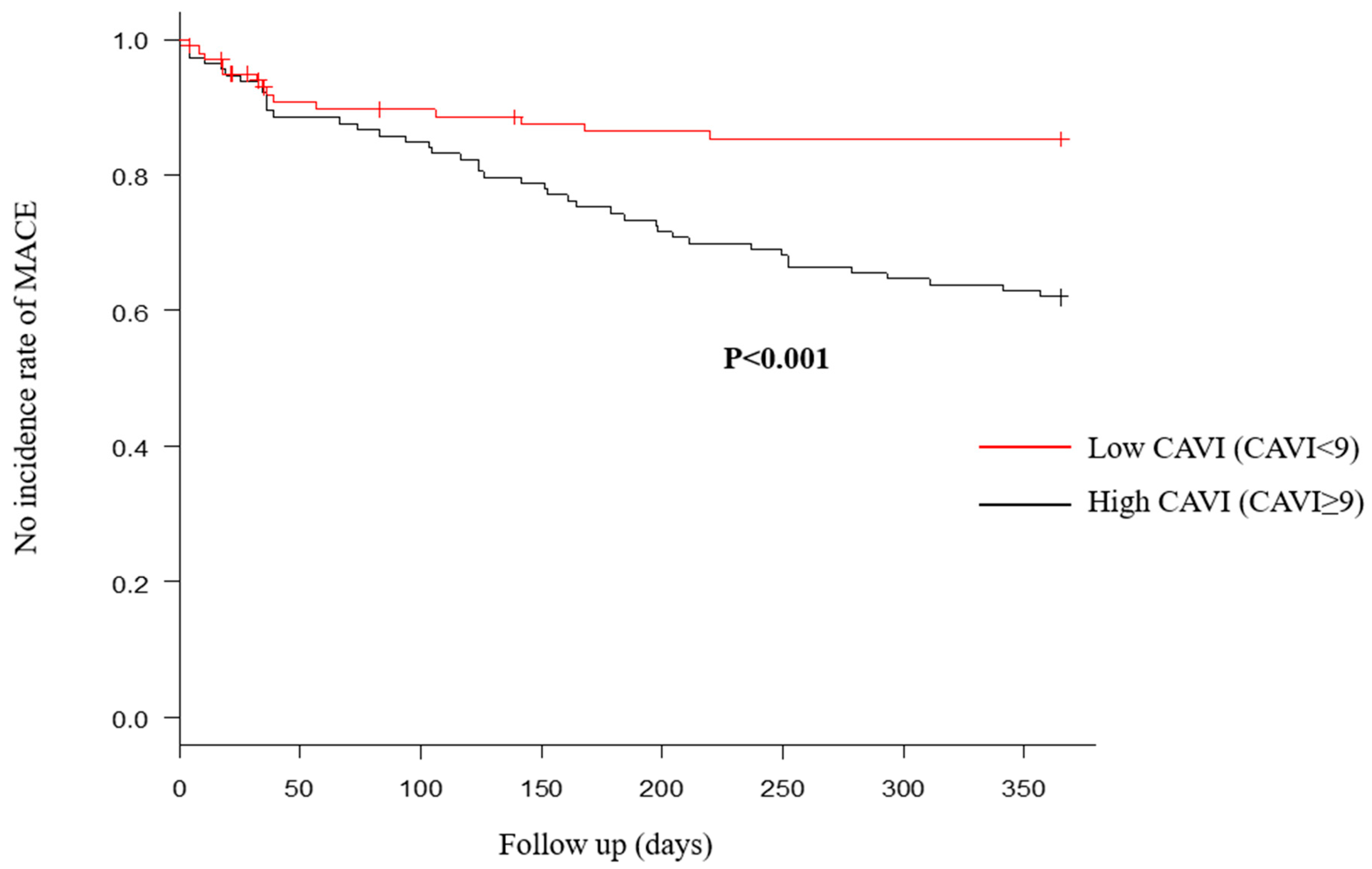
Table 4 shows ABI/CAVI results and BP assessment at admission. Systolic and diastolic BPs were not significantly different between the two groups, which was similar to the findings for mean BP and PP results. In addition, BP variability also showed no differences. By contrast, CAVI and % MAP were significantly different between the two groups. In particular, CAVI can independently predict MACE, even after adjusting for other factors (Table 5). The cutoff value of CAVI for predicting the composite endpoint was 9.0 from the ROC curve (sensitivity, 0.554; specificity, 0.754; area under the curve, 0.66; 95% confidence interval, 0.581–0.739). When comparing Kaplan−Meier curves between two groups using this value, the high CAVI group had significantly more MACE (Figure 4). Although re-hospitalization with HF was significantly different, cardiovascular mortality showed no significant difference (Figure 5).

Table 4.
CAVI and % MAP findings in the MACE and non-MACE groups.

Table 5.
Multivariate analysis for prediction of MACE.
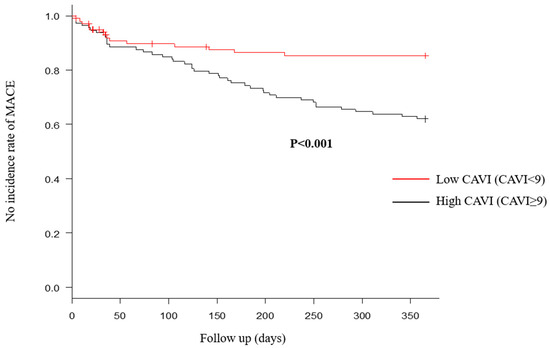
Figure 4.
Major adverse cardiac events (MACE) within 1 year after discharge were compared between high and low cardio–ankle brachial index (CAVI) groups. Number of MACE within 1 year after discharge in the high CAVI group was significantly more, compared with the low CAVI group.
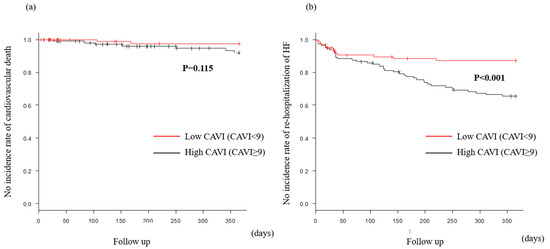
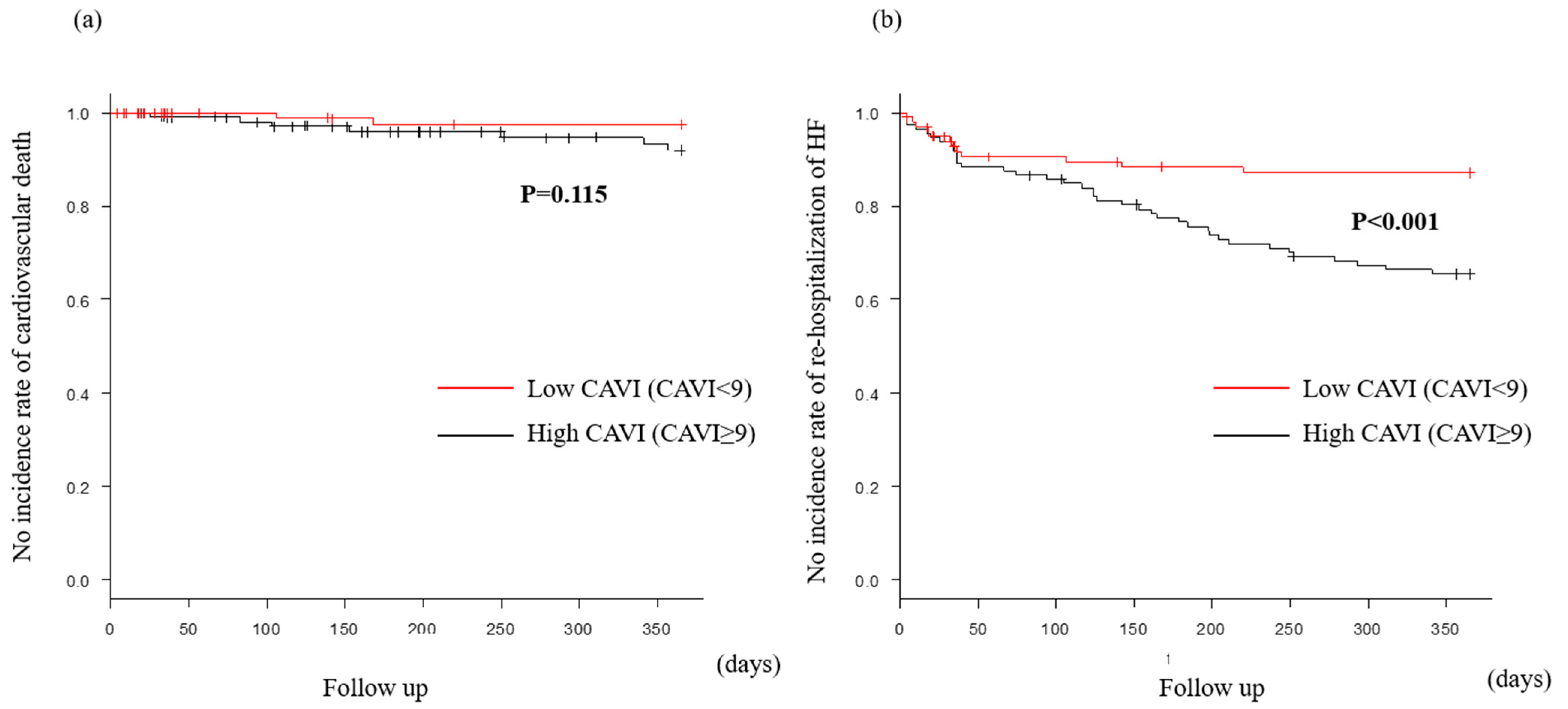
Figure 5.
MACE within 1 year after discharge in the preserved CAVI group. Cardiovascular death (a) was similar in both groups. However, rehospitalization of heart failure (b) in the high CAVI group was significantly more, compared with the low CAVI group.
4. Discussion
4.1. Main Findings
In the present study, previous HF, CKD, cardiac morphology (cardiac size and function), CAVI, and % MAP were associated with the occurrence of MACE. Most factors were reported as being associated with HF prognosis in previous studies. In particular, CAVI was an independent predictive factor for the occurrence of MACE. When divided into two groups based on CAVI, MACE occurred significantly more in the high CAVI group. In terms of MACE components, re-hospitalization with HF was significantly different, but cardiovascular death rates were not different.
4.2. Re-Hospitalization with HF and Prognosis
The greater the number of previous hospitalizations for HF, the worse the in-hospital mortality rate and poor prognosis 1 year after discharge [4,19]. In the past 9 years of longitudinal studies, the prognosis (mortality and/or re-hospitalization with HF) of patients with HF has not improved [3]. Re-hospitalization rates have not improved over time, and re-hospitalization with HF needs to be reduced first [20]. Factors leading to re-hospitalization with HF in Japan include increased salt intake, poor medication compliance, and arrhythmia. Approximately half of these factors can be addressed through patient self-management, and forms of self-management can reduce cardiovascular events by approximately 40% [21]. This study found that although all-cause mortality did not show differences, the risk of re-hospitalization with HF was reduced by approximately 50%. This result is consistent with the prediction that thorough self-management will reduce re-hospitalization with HF by approximately 50%. Although cardiovascular mortality was not different in the present study, re-hospitalization with HF was significantly reduced in the low CAVI group. The high CAVI group is a high-risk group for frequent re-hospitalization with HF, and stricter management, including thorough self-management, is important for these patients. Their prognosis could be improved by reducing re-hospitalization with HF.
4.3. Vascular Insufficiency and HF
HF is classified into HFrEF, HFmrEF, and HFpEF, based on left ventricular contractility [16]. Many treatments have been established for HFrEF, including cardioprotective medications, such as the fantastic four [22]. By contrast, the only cardioprotective treatment effective for HFpEF is sodium glucose cotransporter 2 (SGLT2) inhibitors, and medications are chosen based on individual pathological condition for HFmrEF. SGLT2 inhibitors are effective therapeutic medications for many pathological conditions, including reducing mortality in HF, recovered EF, and CKD [23,24]. Their mechanism may include effects on sympathetic nerve activity and cardiac energy metabolism [25,26]; however, this has not been established. As HFpEF includes various pathological conditions, only SGLT2 inhibitors with various actions are considered effective. The influence of vascular function contributes to the difference in treatment for the three types of HF (HFrEF, HFmrEF, and HFpEF) [27]. A decrease in the Windkessel effect causes an increase in systolic BP, which raises left ventricular afterload. This causes left ventricular hypertrophy, leading to left ventricular diastolic dysfunction by increasing cardiac work and oxygen demand [28]. Conversely, impaired coronary artery perfusion caused by a decrease in diastolic BP induces left ventricular systolic dysfunction due to decreased myocardial oxygen supply. Furthermore, vascular insufficiency results in coronary artery perfusion disorders via coronary arteriosclerosis. However, although some previous studies have reported an association between CAVI and HFpEF, which primarily involves diastolic dysfunction [29], there are few reports on all pathologies of HF. In the present study, we demonstrated that high CAVI was associated with a worsened prognosis in all cases of HF, and that vascular insufficiency is present in all pathologies of HF. Elevated PWV, which is used to calculate CAVI, was linked to prognosis in HFrEF without peripheral artery disease [30]. It has also been reported that CAVI can help predict hospitalization for worsening HF in patients with chronic HF [31]. Moreover, CAVI has also been linked to BNP [32], and BNP-related left ventricular filling pressure has been linked to CAVI [33]. Increased oxidative stress in failing hearts is linked to a poor prognosis [34], and CAVI is also thought to reflect oxidative stress [35]. Therefore, reduced oxidative stress could be responsible for these results. The current study was retrospective and oxidative stress and inflammatory markers could not be measured; therefore, a large-scale prospective study is required to confirm these hypotheses.
4.4. Evaluation of Vascular Function
Vascular insufficiency is a combination of vascular endothelial dysfunction, smooth muscle dysfunction, and metabolic dysfunction. Pathophysiological features range from asymptomatic early-stage vascular dysfunction to advanced atherosclerosis with some clinical symptoms. CAVI, PWV, flow-mediated vasodilation (FMD), and reactive hyperemia peripheral arterial tonometry (RH-PAT) are some of the methods used for evaluation [36]. FMD and RH-PAT can assess vascular endothelial function, whereas PWV can be roughly classified into two types based on the measurement site. This includes the carotid artery–femoral artery (cf) PWV and brachial–ankle (ba) PWV. The former mainly measures elastic arteries, and the latter focuses on muscular arteries. Heart–ankle (ha) PWV is used for CAVI measurement, but the target blood vessels are similar to baPWV. Like CAVI, haPWV has been linked to cardiovascular events [37], but it is heavily dependent on BP. However, unlike haPWV, CAVI is a BP independent index [14]. Although only CAVI was assessed in this retrospective study, there was no difference in BP between the MACE and non-MACE groups, and PWV may have produced similar results to CAVI. Furthermore, increased oxidative stress has been shown to cause vascular endothelial dysfunction, and a link between FMD or RH-PAT and oxidative stress has been reported [38,39]. Furthermore, it is believed that vascular endothelial damage may be linked to HF via oxidative stress, but this was not investigated in this retrospective study, and more research is needed.
4.5. Study Limitations
The present study was a single-center, retrospective study, which was limited by the small number of patients with HF whose vascular function was evaluated. The evaluation of CAVI in patients not suspected of having arteriosclerotic disease is not clinically useful, and it is also excluded from medical treatment covered by insurance. Therefore, we only evaluated the vascular function of patients who were suspected of having atherosclerotic disease. In the present study, the attending physician decided whether CAVI should be measured. Additionally, the extracted data may be limited because of the retrospective nature of the present study. Therefore, we were unable to evaluate patients’ quality of life, living environment, and nursing care. These potential limitations can undermine the strength of the study’s conclusions. Further clinical prospective studies in larger consecutive populations should be conducted to confirm our results.
5. Conclusions
As high CAVI is associated with poor prognosis of HF, these patients require more careful treatment.
Author Contributions
S.K. contributed to the study concept and the acquisition of the data. All authors reviewed the raw data and contributed to the analysis and interpretation. S.K. drafted the manuscript and S.H., S.D., Y.M. and T.I. revised it. All authors have read and agreed to the published version of the manuscript.
Funding
The present study received no external funding.
Institutional Review Board Statement
The present study was approved by the Ethics Committee of Toho University Omori Medical Center (approval number: M21292_M18271_17318, 5 March 2024), and was conducted in accordance with the Declaration of Helsinki.
Informed Consent Statement
The details of the study in opt-out format were posted on the website of our institution and our department (Department of Cardiovascular Medicine) and this acted as a waiver of informed consent from study participants. The subjects of the study were given the opportunity to decline to be enrolled.
Data Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Acknowledgments
We would like to thank all the members who contributed to this study.
Conflicts of Interest
The authors declare no conflicts of interest for the present study.
References
- Okura, Y.; Ramadan, M.M.; Ohno, Y.; Mitsuma, W.; Tanaka, K.; Ito, M.; Suzuki, K.; Tanabe, N.; Kodama, M.; Aizawa, Y. Impending epidemic: Future projection of heart failure in Japan to the year 2055. Circ. J. 2008, 72, 489–491. [Google Scholar] [CrossRef] [PubMed]
- Benjamin, E.J.; Virani, S.S.; Callaway, C.W.; Chamberlain, A.M.; Chang, A.R.; Cheng, S.; Chiuve, S.E.; Cushman, M.; Delling, F.N.; Deo, R.; et al. American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. Circulation 2018, 137, e67–e492. [Google Scholar] [PubMed]
- Shiraishi, Y.; Kohsaka, S.; Sato, N.; Takano, T.; Kitai, T.; Yoshikawa, T.; Matsue, Y.; Ross, J.S.; Chen, J.; Lin, Z.; et al. 9-Year trend in the management of acute heart failure in Japan: A report from the national consortium of acute heart failure registries. J. Am. Heart Assoc. 2018, 7, e008687. [Google Scholar] [CrossRef] [PubMed]
- Su, K.; Kato, T.; Toyofuku, M.; Morimoto, T.; Yaku, H.; Inuzuka, Y.; Tamaki, Y.; Ozasa, N.; Yamamoto, E.; Yoshikawa, Y.; et al. KCHF Registry Investigators. Association of Previous Hospitalization for Heart Failure With Increased Mortality in Patients Hospitalized for Acute Decompensated Heart Failure. Circ. Rep. 2019, 1, 517–524. [Google Scholar] [CrossRef]
- Shinagawa, H.; Inomata, T.; Koitabashi, T.; Nakano, H.; Takeuchi, I.; Naruke, T.; Ohsaka, T.; Nishii, M.; Takehana, H.; Izumi, T. Prognostic significance of increased serum bilirubin levels coincident with cardiac decompensation in chronic heart failure. Circ. J. 2008, 72, 364–369. [Google Scholar] [CrossRef] [PubMed]
- Pereira, J.; Chaves, V.; Tavares, S.; Albuquerque, I.; Gomes, C.; Guiomar, V.; Monteiro, A.; Ferreira, I.; Lourenço, P.; Bettencourt, P. Systolic function recovery in Heart Failure: Frequency, prognostic impact and predictors. Int. J. Cardiol. 2020, 300, 172–177. [Google Scholar] [CrossRef] [PubMed]
- Mei, C.C.; Zhang, J.; Jing, H.X. Fluid mechanics of Windkessel effect. Med. Biol. Eng. Comput. 2018, 56, 1357–1366. [Google Scholar] [CrossRef] [PubMed]
- Heidenreich, P.A.; Bozkurt, B.; Aguilar, D.; Allen, L.A.; Byun, J.J.; Colvin, M.M.; Deswal, A.; Drazner, M.H.; Dunlay, S.M.; Evers, L.R.; et al. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation 2022, 145, e895–e1032. [Google Scholar] [CrossRef] [PubMed]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Böhm, M.; Burri, H.; Butler, J.; Čelutkienė, J.; Chioncel, O.; et al. ESC Scientific Document Group. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef]
- Umemura, S.; Arima, H.; Arima, S.; Asayama, K.; Dohi, Y.; Hirooka, Y.; Horio, T.; Hoshide, S.; Ikeda, S.; Ishimitsu, T.; et al. The Japanese Society of Hypertension Guideline for the Management of Hypertension (JSH2019). Hypertens. Res. 2019, 42, 1235–1481. [Google Scholar]
- Mebazaa, A.; Gheorghiade, M.; Piña, I.L.; Harjola, V.-P.; Hollenberg, S.M.; Follath, F.; Rhodes, A.; Plaisance, P.; Roland, E.; Nieminen, M.; et al. Practical recommendations for prehospital and early in-hospital management of patients presenting with acute heart failure syndromes. Crit. Care Med. 2008, 36, S129–S139. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, M.; Saito, Y.; Kitahara, H.; Saito, K.; Takahara, M.; Himi, T.; Kobayashi, Y. Impact of in-hospital blood pressure variability on clinical outcomes in patients with symptomatic peripheral arterial disease. Hypertens. Res. 2021, 44, 1002–1008. [Google Scholar] [CrossRef] [PubMed]
- Saito, K.; Saito, Y.; Kitahara, H.; Nakayama, T.; Fujimoto, Y.; Kobayashi, Y. In-Hospital Blood Pressure Variability: A Novel Prognostic Marker of Renal Function Decline and Cardiovascular Events in Patients with Coronary Artery Disease. Kidney Blood Press Res. 2020, 45, 748–757. [Google Scholar] [CrossRef] [PubMed]
- Shirai, K.; Utino, J.; Otsuka, K.; Takata, M. A novel blood pressure-independent arterial wall stiffness parameter; cardio-ankle vascular index (CAVI). J. Atheroscler. Thromb. 2006, 13, 101–107. [Google Scholar] [CrossRef] [PubMed]
- Matsuo, S.; Imai, E.; Horio, M.; Yasuda, Y.; Tomita, K.; Nitta, K.; Yamagata, K.; Tomino, Y.; Yokoyama, H.; Hishida, A. Collaborators developing the Japanese equation for estimated GFR. Revised equations for estimated GFR from serum creatinine in Japan. Am. J. Kidney Dis. 2009, 53, 982–992. [Google Scholar] [CrossRef] [PubMed]
- Tsutsui, H.; Ide, T.; Ito, H.; Kihara, Y.; Kinugawa, K.; Kinugawa, S.; Makaya, M.; Murohara, T.; Node, K.; Saito, Y.; et al. Japanese Circulation Society and the Japanese Heart Failure Society Joint Working Group. JCS/JHFS 2021 Guideline Focused Update on Diagnosis and Treatment of Acute and Chronic Heart Failure. Circ. J. Off. J. Jpn. Circ. Soc. 2021, 85, 2252–2291. [Google Scholar]
- Schiller, N.B.; Shah, P.M.; Crawford, M.; DeMaria, A.; Devereux, R.; Feigenbaum, H.; Gutgesell, H.; Reichek, N.; Sahn, D.; Schnittger, I.; et al. Recommendations for quantitation of the left ventricle by two-dimensional echocardiography. J. Am. Soc. Echocardiogr. 1989, 2, 358–367. [Google Scholar] [CrossRef] [PubMed]
- Kanda, Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transpl. 2013, 48, 452–458. [Google Scholar] [CrossRef] [PubMed]
- Kaneko, H.; Itoh, H.; Yotsumoto, H.; Kiriyama, H.; Kamon, T.; Fujiu, K.; Morita, K.; Michihata, N.; Jo, T.; Morita, H.; et al. Association between the number of hospital admissions and in-hospital outcomes in patients with failure. Hypertens. Res. 2020, 43, 1385–1391. [Google Scholar] [CrossRef] [PubMed]
- Tsuchihashi, M.; Tsutsui, H.; Kodama, K.; Kasagi, F.; Takeshita, A. Clinical characteristics and prognosis of hospitalized patients with congestive heart failure--a study in Fukuoka, Japan. Jpn. Circ. J. 2000, 64, 953–959. [Google Scholar] [CrossRef]
- Nakane, E.; Kato, T.; Tanaka, N.; Kuriyama, T.; Kimura, K.; Nishiwaki, S.; Hamaguchi, T.; Morita, Y.; Yamaji, Y.; Haruna, Y.; et al. Association of the induction of a self-care management system with 1-year outcomes in patients hospitalized for heart failure. J. Cardiol. 2020, 77, 48–56. [Google Scholar] [CrossRef]
- Bauersachs, J. Heart failure drug treatment: The fantastic four. Eur. Heart J. 2021, 42, 681–683. [Google Scholar] [CrossRef]
- Vardeny, O.; Desai, A.S.; Jhund, P.S.; Fang, J.C.; Claggett, B.; de Boer, R.A.; Hernandez, A.F.; Inzucchi, S.E.; Kosiborod, M.N.; Lam, C.S.P.; et al. Dapagliflozin and Mode of Death in Heart Failure With Improved Ejection Fraction: A Post Hoc Analysis of the DELIVER Trial. JAMA Cardiol. 2024, 9, 283–289. [Google Scholar] [CrossRef]
- Heerspink, H.J.L.; Sjöström, C.D.; Jongs, N.; Chertow, G.M.; Kosiborod, M.; Hou, F.F.; McMurray, J.J.V.; Rossing, P.; Correa-Rotter, R.; Kurlyandskaya, R.; et al. DAPA-CKD Trial Committees and Investigators. Effects of dapagliflozin on mortality in patients with chronic kidney disease: A pre-specified analysis from the DAPA-CKD randomized controlled trial. Eur. Heart J. 2021, 42, 1216–1227. [Google Scholar] [CrossRef]
- Kiuchi, S.; Hisatake, S.; Kabuki, T.; Fujii, T.; Oka, T.; Dobashi, S.; Hashimoto, H.; Ikeda, T. Long-term use of ipragliflozin improved cardiac sympathetic nerve activity in a patient with heart failure: A case report. Drug Discov. Ther. 2018, 12, 51–54. [Google Scholar] [CrossRef]
- Xie, Y.; Wei, Y.; Li, D.; Pu, J.; Ding, H.; Zhang, X. Mechanisms of SGLT2 Inhibitors in Heart Failure and Their Clinical Value. J. Cardiovasc. Pharmacol. 2023, 81, 4–14. [Google Scholar] [CrossRef]
- Kiuchi, S.; Ikeda, T. Management of hypertension associated with cardiovascular failure. J. Cardiol. 2021, 79, 698–702. [Google Scholar] [CrossRef] [PubMed]
- Namba, T.; Masaki, N.; Takase, B.; Adachi, T. Arterial Stiffness Assessed by Cardio-Ankle Vascular Index. Int. J. Mol. Sci. 2019, 20, 3664. [Google Scholar] [CrossRef] [PubMed]
- Takagi, K.; Ishihara, S.; Kenji, N.; Iha, H.; Kobayashi, N.; Ito, Y.; Nohara, T.; Ohkuma, S.; Mitsuishi, T.; Ishizuka, A.; et al. Clinical significance of arterial stiffness as a factor for hospitalization of heart failure with preserved left ventricular ejection fraction: A retrospective matched case-control study. J. Cardiol. 2020, 76, 171–176. [Google Scholar] [CrossRef] [PubMed]
- Takae, M.; Yamamoto, E.; Oike, F.; Nishihara, T.; Fujisue, K.; Sueta, D.; Usuku, H.; Takashio, S.; Sakamoto, K.; Kaikita, K.; et al. Clinical Significance of Brachial-Ankle Pulse Wave in Patients With Heart Failure With Reduced Left Ventricular Ejection Fraction. Am. J. Hypertens. 2019, 32, 657–667. [Google Scholar] [CrossRef]
- Hitsumoto, T. Efficacy of the Reactive Oxygen Metabolism Test as a Predictor of Initial Heart Failure Hospitalization in Elderly Patients With Chronic Heart Failure. Cardiol. Res. 2018, 9, 153–160. [Google Scholar] [CrossRef]
- Masugata, H.; Senda, S.; Inukai, M.; Murao, K.; Himoto, T.; Hosomi, N.; Murakami, K.; Noma, T.; Kohno, M.; Okada, H.; et al. Association of cardio-ankle vascular index with brain natriuretic peptide levels in hypertension. J. Atheroscler. Thromb. 2012, 19, 255–262. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Masugata, H.; Senda, S.; Goda, F.; Yamagami, A.; Okuyama, H.; Kohno, T.; Hosomi, N.; Yukiiri, K.; Noma, T.; Kiyomoto, H.; et al. Tissue Doppler echocardiography for predicting arterial stiffness assessed by cardio-ankle vascular index. Tohoku J. Exp. Med. 2009, 217, 139–146. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Shibata, A.; Izumiya, Y.; Yamaguchi, Y.; Kitada, R.; Iwata, S.; Ehara, S.; Izumi, Y.; Hanatani, A.; Yoshiyama, M. Increased oxidative stress during exercise predicts poor prognosis in patients with acute decompensated heart failure. ESC Heart Fail. 2021, 8, 3885–3893. [Google Scholar] [CrossRef]
- Masugata, H.; Senda, S.; Murao, K.; Inukai, M.; Himoto, T.; Hosomi, N.; Okada, H.; Goda, F. Association between urinary 8-hydroxydeoxyguanosine, an indicator of oxidative stress, and the cardio-ankle vascular index in hypertensive patients. J. Atheroscler. Thromb. 2012, 19, 747–755. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Tanaka, A.; Tomiyama, H.; Maruhashi, T.; Matsuzawa, Y.; Miyoshi, T.; Kabutoya, T.; Kario, K.; Sugiyama, S.; Munakata, M.; Ito, H.; et al. hysiological Diagnostic Criteria for Vascular Failure. Hypertension 2018, 72, 1060–1071. [Google Scholar] [CrossRef] [PubMed]
- Tanaka, H.; Munakata, M.; Kawano, Y.; Ohishi, M.; Shoji, T.; Sugawara, J.; Tomiyama, H.; Yamashina, A.; Yasuda, H.; Sawayama, T.; et al. Comparison between carotid-femoral and brachial-ankle pulse wave velocity as measures of arterial stiffness. J. Hypertens. 2009, 27, 2022–2027. [Google Scholar] [CrossRef]
- Gurovich, A.N.; Avery, J.C.; Holtgrieve, N.B.; Braith, R.W. Flow-mediated dilation is associated with endothelial oxidative stress in human venous endothelial cells. Vasc. Med. 2014, 19, 251–256. [Google Scholar] [CrossRef]
- Kato, M.; Masuda, T.; Ogano, M.; Hotta, K.; Takagi, H.; Tanaka, S.; Kamada, Y.; Akiyama, A.; Kamekawa, D.; Shimizu, R.; et al. Stretching Exercises Improve Vascular Endothelial Dysfunction Through Attenuation of Oxidative Stress in Chronic Heart Failure Patients With an Implantable Cardioverter Defibrillator. J. Cardiopulm. Rehabilitation Prev. 2017, 37, 130–138. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).