Relationship between Changes in Myocardial F-18 Fluorodeoxyglucose Uptake and Radiation Dose after Adjuvant Three-Dimensional Conformal Radiotherapy in Patients with Breast Cancer
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
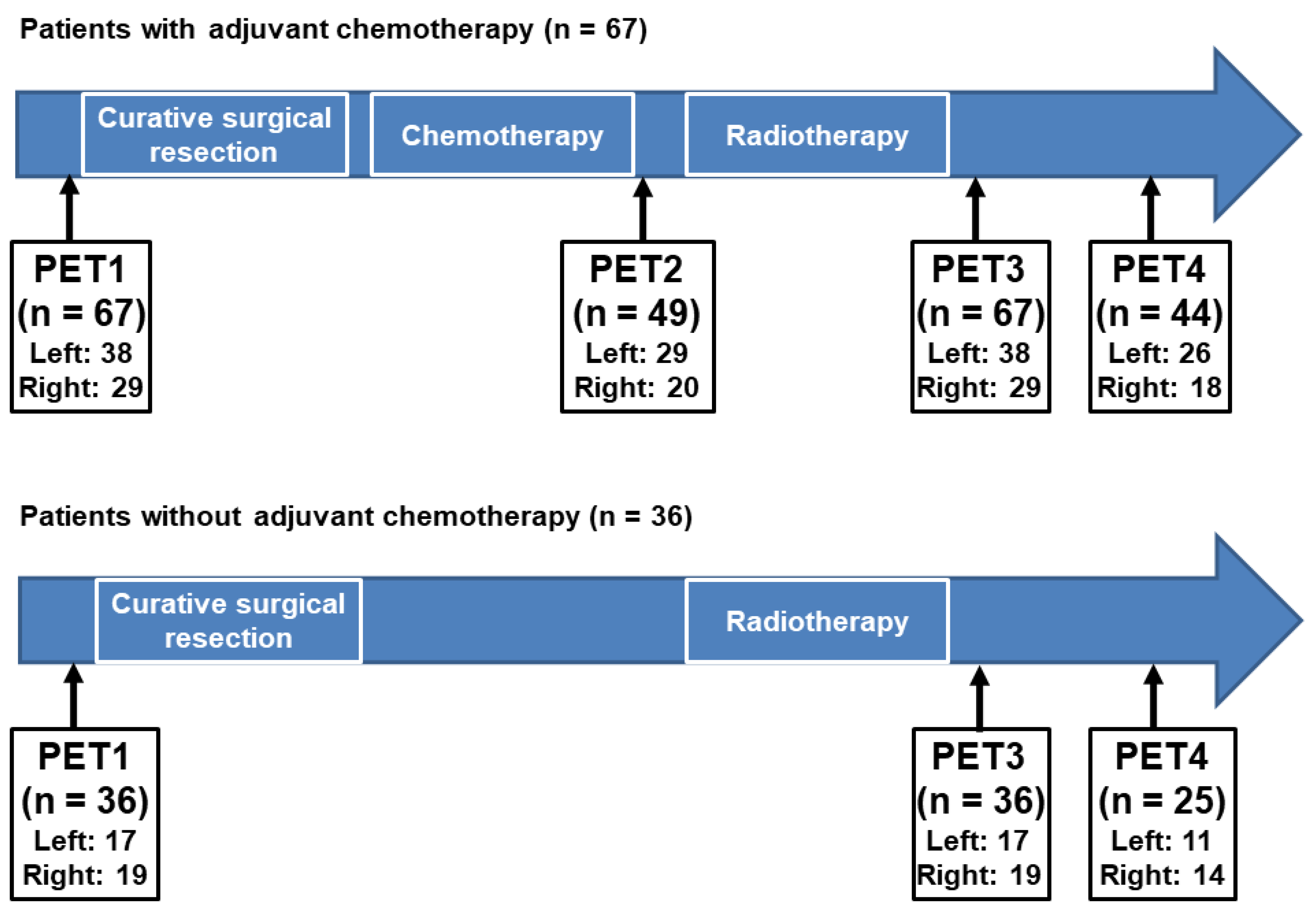
2.2. Diagnostic Work-Up and Follow-Up Courses
2.3. FDG PET/CT
2.4. Adjuvant RT
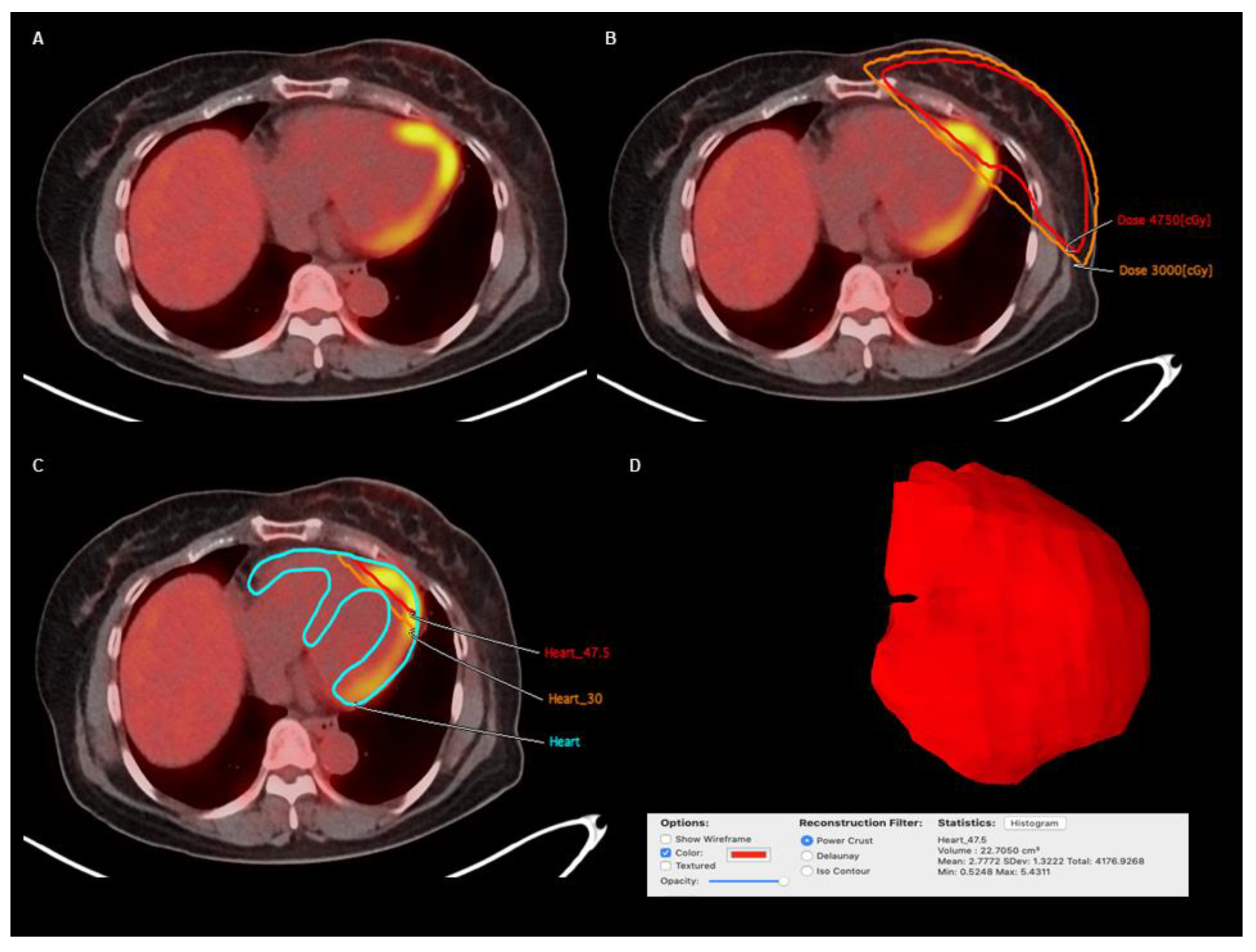
2.5. Image Analysis
2.6. Statistical Analysis
3. Results
3.1. Patient Characteristics
3.2. Comparison of Myocardial FDG Uptake between Left and Right Breast Cancers
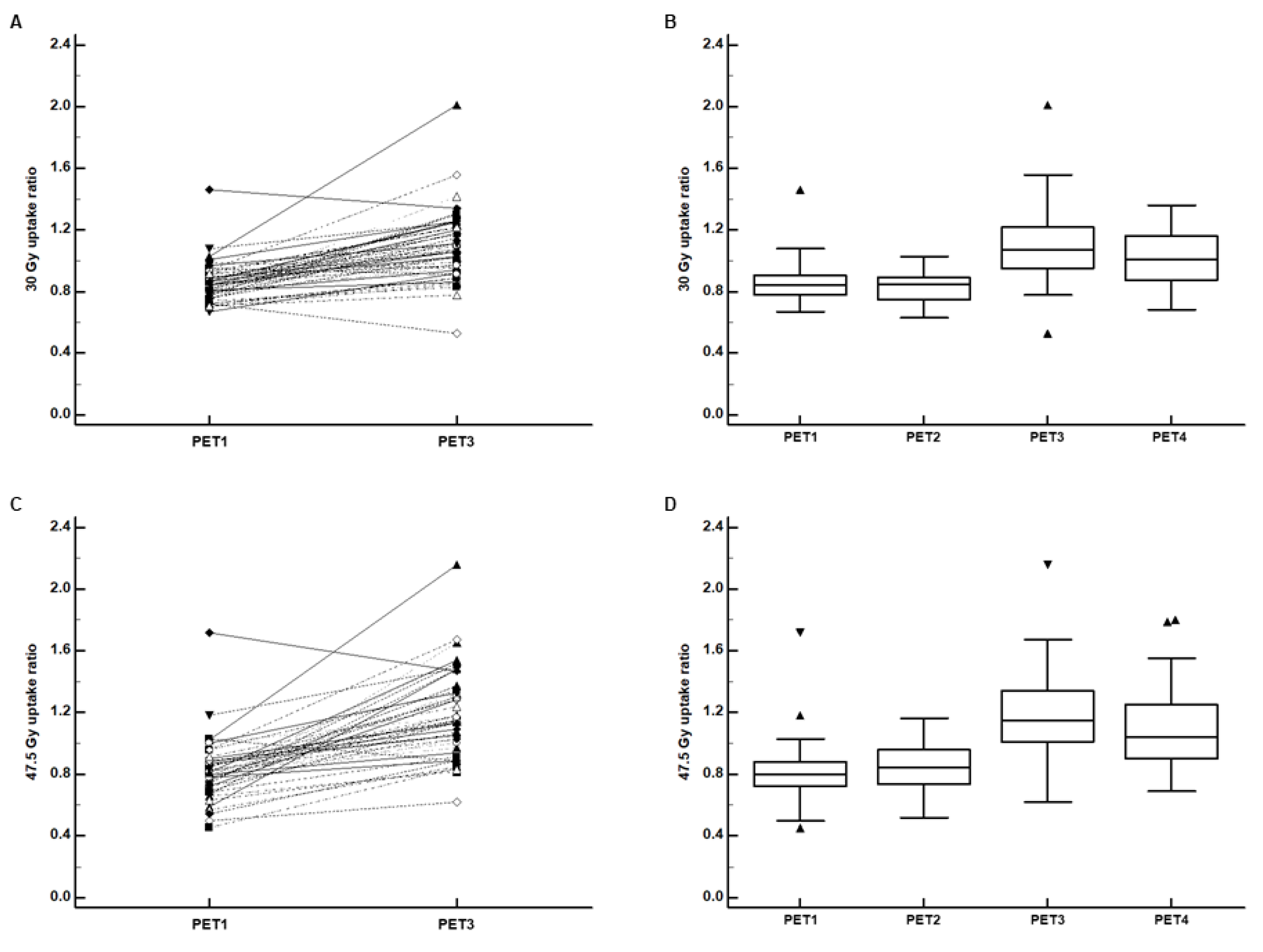
3.3. Comparison of the Irradiated Myocardium-to-Non-Irradiated Myocardium Uptake Ratios between PET Scans
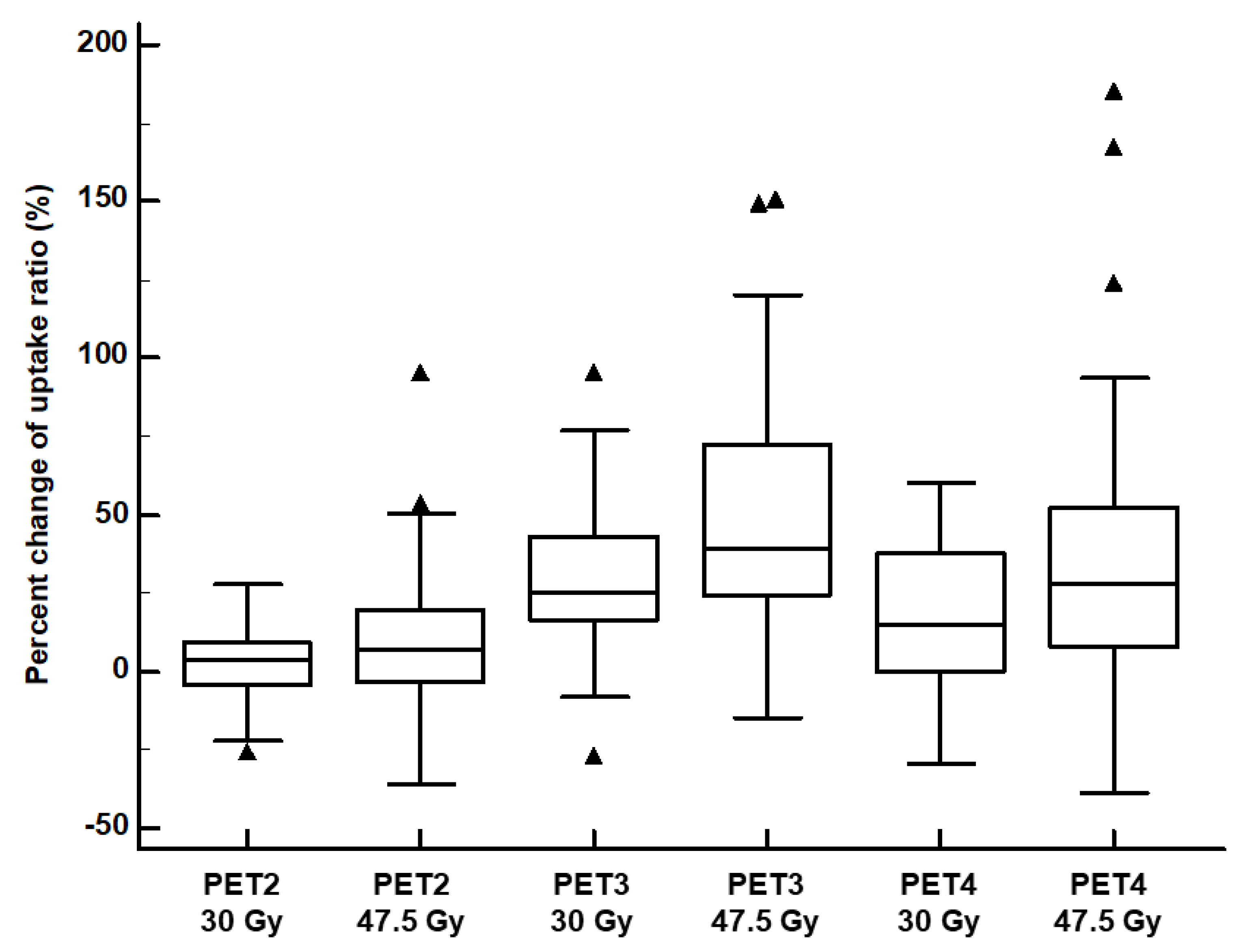
3.4. Comparison of FDG Uptake between the 30 Gy and 47.5 Gy Irradiated Myocardium
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Castaneda, S.A.; Strasser, J. Updates in the treatment of breast cancer with radiotherapy. Surg. Oncol. Clin. N. Am. 2017, 26, 371–382. [Google Scholar] [CrossRef]
- Recht, A.; Comen, E.A.; Fine, R.E.; Fleming, G.F.; Hardenbergh, P.H.; Ho, A.Y.; Hudis, C.A.; Hwang, E.S.; Kirshner, J.J.; Morrow, M.; et al. Postmastectomy radiotherapy: An American Society of Clinical Oncology, American Society for Radiation Oncology, and Society of Surgical Oncology focused guideline update. J. Clin. Oncol. 2016, 34, 4431–4442. [Google Scholar] [CrossRef]
- Darby, S.; McGale, P.; Correa, C.; Taylor, C.; Arriagada, R.; Clarke, M.; Cutter, D.; Davies, C.; Ewertz, M.; Godwin, J.; et al. Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: Meta-analysis of individual patient data for 10,801 women in 17 randomised trials. Lancet 2011, 378, 1707–1716. [Google Scholar] [CrossRef]
- Wennstig, A.K.; Garmo, H.; Isacsson, U.; Gagliardi, G.; Rintela, N.; Lagerqvist, B.; Holmberg, L.; Blomqvist, C.; Sund, M.; Nilsson, G. The relationship between radiation doses to coronary arteries and location of coronary stenosis requiring intervention in breast cancer survivors. Radiat. Oncol. 2019, 14, 40. [Google Scholar] [CrossRef] [PubMed]
- Taylor, C.W.; Povall, J.M.; McGale, P.; Nisbet, A.; Dodwell, D.; Smith, J.T.; Darby, S.C. Cardiac dose from tangential breast cancer radiotherapy in the year 2006. Int. J. Radiat. Oncol. Biol. Phys. 2008, 72, 501–507. [Google Scholar] [CrossRef] [PubMed]
- Harris, E.E.; Correa, C.; Hwang, W.T.; Liao, J.; Litt, H.I.; Ferrari, V.A.; Solin, L.J. Late cardiac mortality and morbidity in early-stage breast cancer patients after breast-conservation treatment. J. Clin. Oncol. 2006, 24, 4100–4106. [Google Scholar] [CrossRef]
- Bouillon, K.; Haddy, N.; Delaloge, S.; Garbay, J.R.; Garsi, J.P.; Brindel, P.; Mousannif, A.; Le, M.G.; Labbe, M.; Arriagada, R.; et al. Long-term cardiovascular mortality after radiotherapy for breast cancer. J. Am. Coll. Cardiol. 2011, 57, 445–452. [Google Scholar] [CrossRef] [PubMed]
- Darby, S.C.; Ewertz, M.; McGale, P.; Bennet, A.M.; Blom-Goldman, U.; Bronnum, D.; Correa, C.; Cutter, D.; Gagliardi, G.; Gigante, B.; et al. Risk of ischemic heart disease in women after radiotherapy for breast cancer. N. Engl. J. Med. 2013, 368, 987–998. [Google Scholar] [CrossRef] [PubMed]
- Skytta, T.; Tuohinen, S.; Boman, E.; Virtanen, V.; Raatikainen, P.; Kellokumpu-Lehtinen, P.L. Troponin T-release associates with cardiac radiation doses during adjuvant left-sided breast cancer radiotherapy. Radiat. Oncol. 2015, 10, 141. [Google Scholar] [CrossRef]
- Shah, C.; Badiyan, S.; Berry, S.; Khan, A.J.; Goyal, S.; Schulte, K.; Nanavati, A.; Lynch, M.; Vicini, F.A. Cardiac dose sparing and avoidance techniques in breast cancer radiotherapy. Radiother. Oncol. 2014, 112, 9–16. [Google Scholar] [CrossRef]
- Caresia Aroztegui, A.P.; Garcia Vicente, A.M.; Alvarez Ruiz, S.; Delgado Bolton, R.C.; Orcajo Rincon, J.; Garcia Garzon, J.R.; de Arcocha Torres, M.; Garcia-Velloso, M.J. 18F-FDG PET/CT in breast cancer: Evidence-based recommendations in initial staging. Tumour. Biol. 2017, 39, 1010428317728285. [Google Scholar] [CrossRef]
- Hildebrandt, M.G.; Lauridsen, J.F.; Vogsen, M.; Holm, J.; Vilstrup, M.H.; Braad, P.E.; Gerke, O.; Thomassen, M.; Ewertz, M.; Hoilund-Carlsen, P.F. FDG-PET/CT for response monitoring in metastatic breast cancer: Today, tomorrow, and beyond. Cancers (Basel) 2019, 11, 1190. [Google Scholar] [CrossRef]
- Lee, J.W.; Lee, S.M. Radiomics in oncological PET/CT: Clinical applications. Nucl. Med. Mol. Imaging 2018, 52, 170–189. [Google Scholar] [CrossRef]
- Lee, J.W.; Kim, S.Y.; Lee, H.J.; Han, S.W.; Lee, J.E.; Lee, S.M. Prognostic significance of CT-attenuation of tumor-adjacent breast adipose tissue in breast cancer patients with surgical resection. Cancers (Basel) 2019, 11, 1135. [Google Scholar] [CrossRef]
- Lee, J.W.; Lee, S.M.; Chung, Y.A. Prognostic value of CT attenuation and FDG uptake of adipose tissue in patients with pancreatic adenocarcinoma. Clin. Radiol. 2018, 73, 1056.e1–1056.e10. [Google Scholar] [CrossRef]
- Lee, J.W.; Ban, M.J.; Park, J.H.; Lee, S.M. Effect of F-18 fluorodeoxyglucose uptake by bone marrow on the prognosis of head and neck squamous cell carcinoma. J. Clin. Med. 2019, 8, 1169. [Google Scholar] [CrossRef]
- Dou, K.F.; Gao, X.J.; Xie, B.Q.; Li, Y.; He, Z.X.; Yang, M.F. Dual-time-point myocardial (18)F-FDG imaging in the detection of coronary artery disease. BMC Cardiovasc. Disord. 2017, 17, 120. [Google Scholar] [CrossRef]
- Atterton-Evans, V.; Turner, J.; Vivanti, A.; Robertson, T. Variances of dietary preparation for suppression of physiological (18)F-FDG myocardial uptake in the presence of cardiac sarcoidosis: A systematic review. J. Nucl. Cardiol. 2018, 1–9. [Google Scholar] [CrossRef]
- Inglese, E.; Leva, L.; Matheoud, R.; Sacchetti, G.; Secco, C.; Gandolfo, P.; Brambilla, M.; Sambuceti, G. Spatial and temporal heterogeneity of regional myocardial uptake in patients without heart disease under fasting conditions on repeated whole-body 18F-FDG PET/CT. J. Nucl. Med. 2007, 48, 1662–1669. [Google Scholar] [CrossRef]
- Evans, J.D.; Gomez, D.R.; Chang, J.Y.; Gladish, G.W.; Erasmus, J.J.; Rebueno, N.; Banchs, J.; Komaki, R.; Welsh, J.W. Cardiac (1)(8)F-fluorodeoxyglucose uptake on positron emission tomography after thoracic stereotactic body radiation therapy. Radiother. Oncol. 2013, 109, 82–88. [Google Scholar] [CrossRef]
- Jingu, K.; Kaneta, T.; Nemoto, K.; Ichinose, A.; Oikawa, M.; Takai, Y.; Ogawa, Y.; Nakata, E.; Sakayauchi, T.; Takai, K.; et al. The utility of 18F-fluorodeoxyglucose positron emission tomography for early diagnosis of radiation-induced myocardial damage. Int. J. Radiat. Oncol. Biol. Phys. 2006, 66, 845–851. [Google Scholar] [CrossRef]
- Stewart, F.A.; Hoving, S.; Russell, N.S. Vascular damage as an underlying mechanism of cardiac and cerebral toxicity in irradiated cancer patients. Radiat. Res. 2010, 174, 865–869. [Google Scholar] [CrossRef]
- Konski, A.; Li, T.; Christensen, M.; Cheng, J.D.; Yu, J.Q.; Crawford, K.; Haluszka, O.; Tokar, J.; Scott, W.; Meropol, N.J.; et al. Symptomatic cardiac toxicity is predicted by dosimetric and patient factors rather than changes in 18F-FDG PET determination of myocardial activity after chemoradiotherapy for esophageal cancer. Radiother. Oncol. 2012, 104, 72–77. [Google Scholar] [CrossRef]
- Ishida, Y.; Sakanaka, K.; Itasaka, S.; Nakamoto, Y.; Togashi, K.; Mizowaki, T.; Hiraoka, M. Effect of long fasting on myocardial accumulation in 18F-fluorodeoxyglucose positron emission tomography after chemoradiotherapy for esophageal carcinoma. J. Radiat. Res. 2018, 59, 182–189. [Google Scholar] [CrossRef]
- Unal, K.; Unlu, M.; Akdemir, O.; Akmansu, M. 18F-FDG PET/CT findings of radiotherapy-related myocardial changes in patients with thoracic malignancies. Nucl. Med. Commun. 2013, 34, 855–859. [Google Scholar] [CrossRef]
- Duane, F.; Aznar, M.C.; Bartlett, F.; Cutter, D.J.; Darby, S.C.; Jagsi, R.; Lorenzen, E.L.; McArdle, O.; McGale, P.; Myerson, S.; et al. A cardiac contouring atlas for radiotherapy. Radiother. Oncol. 2017, 122, 416–422. [Google Scholar] [CrossRef]
- Veinot, J.P.; Edwards, W.D. Pathology of radiation-induced heart disease: A surgical and autopsy study of 27 cases. Hum. Pathol. 1996, 27, 766–773. [Google Scholar] [CrossRef]
- Yan, R.; Song, J.; Wu, Z.; Guo, M.; Liu, J.; Li, J.; Hao, X.; Li, S. Detection of myocardial metabolic abnormalities by 18F-FDG PET/CT and corresponding pathological changes in beagles with local heart irradiation. Korean J. Radiol. 2015, 16, 919–928. [Google Scholar] [CrossRef]
- Lauk, S.; Kiszel, Z.; Buschmann, J.; Trott, K.R. Radiation-induced heart disease in rats. Int. J. Radiat. Oncol. Biol. Phys. 1985, 11, 801–808. [Google Scholar] [CrossRef]
- Barjaktarovic, Z.; Schmaltz, D.; Shyla, A.; Azimzadeh, O.; Schulz, S.; Haagen, J.; Dorr, W.; Sarioglu, H.; Schafer, A.; Atkinson, M.J.; et al. Radiation-induced signaling results in mitochondrial impairment in mouse heart at 4 weeks after exposure to X-rays. PLoS ONE 2011, 6, e27811. [Google Scholar] [CrossRef]
- Azimzadeh, O.; Scherthan, H.; Sarioglu, H.; Barjaktarovic, Z.; Conrad, M.; Vogt, A.; Calzada-Wack, J.; Neff, F.; Aubele, M.; Buske, C.; et al. Rapid proteomic remodeling of cardiac tissue caused by total body ionizing radiation. Proteomics 2011, 11, 3299–3311. [Google Scholar] [CrossRef]
- Kim, J.; Cho, S.G.; Kang, S.R.; Yoo, S.W.; Kwon, S.Y.; Min, J.J.; Bom, H.S.; Song, H.C. Association between FDG uptake in the right ventricular myocardium and cancer therapy-induced cardiotoxicity. J. Nucl. Cardiol. 2019, 1–10. [Google Scholar] [CrossRef]
- Correa, C.R.; Litt, H.I.; Hwang, W.T.; Ferrari, V.A.; Solin, L.J.; Harris, E.E. Coronary artery findings after left-sided compared with right-sided radiation treatment for early-stage breast cancer. J. Clin. Oncol. 2007, 25, 3031–3037. [Google Scholar] [CrossRef]
- Boellaard, R.; Krak, N.C.; Hoekstra, O.S.; Lammertsma, A.A. Effects of noise, image resolution, and ROI definition on the accuracy of standard uptake values: A simulation study. J. Nucl. Med. 2004, 45, 1519–1527. [Google Scholar]
- Ziai, P.; Hayeri, M.R.; Salei, A.; Salavati, A.; Houshmand, S.; Alavi, A.; Teytelboym, O.M. Role of optimal quantification of FDG PET imaging in the clinical practice of radiology. Radiographics 2016, 36, 481–496. [Google Scholar] [CrossRef]
- Bauckneht, M.; Ferrarazzo, G.; Fiz, F.; Morbelli, S.; Sarocchi, M.; Pastorino, F.; Ghidella, A.; Pomposelli, E.; Miglino, M.; Ameri, P.; et al. Doxorubicin effect on myocardial metabolism as a prerequisite for subsequent development of cardiac toxicity: A translational (18)F-FDG PET/CT observation. J. Nucl. Med. 2017, 58, 1638–1645. [Google Scholar] [CrossRef]
- Frille, A.; Steinhoff, K.G.; Hesse, S.; Grachtrup, S.; Wald, A.; Wirtz, H.; Sabri, O.; Seyfarth, H.J. Thoracic [18F]fluorodeoxyglucose uptake measured by positron emission tomography/computed tomography in pulmonary hypertension. Medicine (Baltimore) 2016, 95, e3976. [Google Scholar] [CrossRef]
- Hu, L.; Qiu, C.; Wang, X.; Xu, M.; Shao, X.; Wang, Y. The association between diabetes mellitus and reduction in myocardial glucose uptake: A population-based (18)F-FDG PET/CT study. BMC Cardiovasc. Disord. 2018, 18, 203. [Google Scholar] [CrossRef]
- Ko, K.Y.; Wang, S.Y.; Yen, R.F.; Shiau, Y.C.; Hsu, J.C.; Tsai, H.Y.; Lee, C.L.; Chiu, K.M.; Wu, Y.W. Clinical significance of quantitative assessment of glucose utilization in patients with ischemic cardiomyopathy. J. Nucl. Cardiol. 2018, 1–11. [Google Scholar] [CrossRef]
- Lu, Y.; Grant, C.; Xie, K.; Sweiss, N.J. Suppression of myocardial 18F-FDG uptake through prolonged high-fat, high-protein, and very-low-carbohydrate diet before FDG-PET/CT for evaluation of patients with suspected cardiac sarcoidosis. Clin. Nucl. Med. 2017, 42, 88–94. [Google Scholar] [CrossRef]
- Manabe, O.; Yoshinaga, K.; Ohira, H.; Masuda, A.; Sato, T.; Tsujino, I.; Yamada, A.; Oyama-Manabe, N.; Hirata, K.; Nishimura, M.; et al. The effects of 18-h fasting with low-carbohydrate diet preparation on suppressed physiological myocardial (18)F-fluorodeoxyglucose (FDG) uptake and possible minimal effects of unfractionated heparin use in patients with suspected cardiac involvement sarcoidosis. J. Nucl. Cardiol. 2016, 23, 244–252. [Google Scholar] [CrossRef] [PubMed]

| Characteristics | Patients with Left Breast Cancer (n = 55) | Patients with Right Breast Cancer (n = 48) | p-Value | |
|---|---|---|---|---|
| Age (years) | 51.2 ± 9.9 * | 51.4 ± 9.7 * | 0.928 | |
| Menopausal status | Premenopausal | 22 (40.0%) | 17 (35.4%) | 0.634 |
| Postmenopausal | 33 (60.0%) | 31 (64.6%) | ||
| Histopathology | Intraductal carcinoma | 48 (87.3%) | 41 (85.4%) | 0.785 |
| Intralobular carcinoma | 7 (12.7%) | 7 (14.6%) | ||
| T stage | T1 | 33 (60.0%) | 35 (72.9%) | 0.191 |
| T2 | 19 (34.5%) | 9 (18.8%) | ||
| T3 | 3 (5.5%) | 4 (8.3%) | ||
| Lymph node metastasis | Absence | 41 (74.5%) | 34 (70.8%) | 0.674 |
| Presence | 14 (25.5%) | 14 (29.2%) | ||
| Tumor size (cm) | 1.82 ± 1.20 * | 2.09 ± 1.13 * | 0.252 | |
| Histologic grade | Grade 1 | 17 (30.9%) | 15 (31.2%) | 0.980 |
| Grade 2 | 28 (50.9%) | 25 (52.1%) | ||
| Grade 3 | 10 (18.2%) | 8 (16.7%) | ||
| Estrogen receptor status | Positive | 49 (89.1%) | 39 (81.2%) | 0.263 |
| Negative | 6 (10.9%) | 9 (18.8%) | ||
| Progesterone receptor status | Positive | 42 (76.4%) | 30 (62.5%) | 0.128 |
| Negative | 13 (23.6%) | 18 (37.5%) | ||
| HER2 status | Positive | 27 (49.1%) | 23 (47.9%) | 0.906 |
| Negative | 28 (50.9%) | 25 (52.1%) | ||
| Triple negative tumor | 2 (3.6%) | 3 (6.2%) | 0.662 | |
| Ki67 expression status | Positive (≥14%) | 29 (52.7%) | 27 (56.2%) | 0.722 |
| Negative (<14%) | 26 (47.3%) | 21 (43.7%) | ||
| Hypertension | Yes | 8 (14.5%) | 11 (22.9%) | 0.277 |
| No | 47 (85.5%) | 37 (77.1%) | ||
| Diabetes mellitus | Yes | 8 (14.5%) | 9 (18.8%) | 0.568 |
| No | 47 (85.5%) | 39 (81.2%) | ||
| Dyslipidemia medication | Yes | 2 (3.6%) | 3 (6.3%) | 0.540 |
| No | 53 (96.4%) | 45 (93.7%) | ||
| Serum total cholesterol level on staging blood tests | 187 ± 29 * | 194 ± 35 * | 0.340 | |
| Serum triglyceride level on staging blood tests | 143 ± 95 * | 134 ± 103 * | 0.662 | |
| Adjuvant treatment | CTx+RT+Hx | 37 (67.3%) | 26 (54.2%) | 0.322 |
| RT+Hx | 17 (30.9%) | 18 (37.5%) | ||
| CTx+RT | 1 (1.8%) | 3 (6.2%) | ||
| RT alone | 0 (0.0%) | 1 (2.1%) | ||
| Chemotherapy regimen | AC | 14 (25.5%) | 9 (18.8%) | 0.551 |
| TAC | 11 (20.0%) | 12 (25.0%) | ||
| CMF | 8 (14.5%) | 7 (14.6%) | ||
| FAC | 3 (5.5%) | 1 (2.1%) | ||
| FEC | 2 (3.6%) | 0 (0.0%) | ||
| Prescribed total radiation dose (Gy) | Whole breast RT dose | Median, 50.4 (range, 50–50.4) | Median, 50.4 (range, 45–50.4) | 0.440 |
| Boost RT dose | Median, 16 (range, 8–16) | Median, 16 (range, 10–16) | 0.225 | |
| Boost RT location | UOQ | 24 (49%) | 24 (57.1%) | 0.077 |
| UIQ | 11 (22.4%) | 10 (23.8%) | ||
| LOQ | 4 (8.2%) | 6 (14.3%) | ||
| LIQ | 4 (8.2%) | 2 (4.8%) | ||
| Central | 6 (12.2%) | 0 (0%) | ||
| Interval between CTx and PET2 (days) | 11.9 ± 4.6 * | 13.5 ± 6.3 * | 0.322 | |
| Interval between RT and PET3 (days) | 139.7 ± 28.1 * | 132.0 ± 28.2 * | 0.170 | |
| Interval between RT and PET4 (days) | 357.4 ± 50.2 * | 363.6 ± 49.3 * | 0.605 | |
| Patients | Myocardium-to-Blood Pool Uptake Ratio | |||
|---|---|---|---|---|
| PET1 | PET2 | PET3 | PET4 | |
| Patients with left breast cancer | 1.33 ± 1.10 | 1.54 ± 1.07 | 1.41 ± 0.92 | 1.47 ± 1.00 |
| Patients with right breast cancer | 1.26 ± 0.59 | 1.61 ± 1.16 | 1.47 ± 1.16 | 1.43 ± 0.89 |
| p-values | 0.318 | 0.357 | 0.695 | 0.869 |
| Variables | PET1 (n = 55) | PET2 (n = 29) | PET3 (n = 55) | PET4 (n = 37) |
|---|---|---|---|---|
| 30 Gy uptake ratio | 0.85 ± 0.12 | 0.84 ± 0.10 | 1.09 ± 0.22 | 1.01 ± 0.18 |
| Percent change in the 30 Gy uptake ratio (%) | - | 1.7 ± 11.5 | 28.7 ± 22.3 | 18.2 ± 23.3 |
| 47.5 Gy uptake ratio | 0.81 ± 0.20 * | 0.83 ± 0.17 † | 1.19 ± 0.28 * | 1.10 ± 0.28 ‡ |
| Percent change in the 47.5 Gy uptake ratio (%) | - | 7.0 ± 28.7 † | 50.2 ± 36.9 * | 40.6 ± 51.8 ‡ |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jo, I.Y.; Lee, J.W.; Kim, W.C.; Min, C.K.; Kim, E.S.; Yeo, S.-G.; Lee, S.M. Relationship between Changes in Myocardial F-18 Fluorodeoxyglucose Uptake and Radiation Dose after Adjuvant Three-Dimensional Conformal Radiotherapy in Patients with Breast Cancer. J. Clin. Med. 2020, 9, 666. https://doi.org/10.3390/jcm9030666
Jo IY, Lee JW, Kim WC, Min CK, Kim ES, Yeo S-G, Lee SM. Relationship between Changes in Myocardial F-18 Fluorodeoxyglucose Uptake and Radiation Dose after Adjuvant Three-Dimensional Conformal Radiotherapy in Patients with Breast Cancer. Journal of Clinical Medicine. 2020; 9(3):666. https://doi.org/10.3390/jcm9030666
Chicago/Turabian StyleJo, In Young, Jeong Won Lee, Woo Chul Kim, Chul Kee Min, Eun Seog Kim, Seung-Gu Yeo, and Sang Mi Lee. 2020. "Relationship between Changes in Myocardial F-18 Fluorodeoxyglucose Uptake and Radiation Dose after Adjuvant Three-Dimensional Conformal Radiotherapy in Patients with Breast Cancer" Journal of Clinical Medicine 9, no. 3: 666. https://doi.org/10.3390/jcm9030666
APA StyleJo, I. Y., Lee, J. W., Kim, W. C., Min, C. K., Kim, E. S., Yeo, S.-G., & Lee, S. M. (2020). Relationship between Changes in Myocardial F-18 Fluorodeoxyglucose Uptake and Radiation Dose after Adjuvant Three-Dimensional Conformal Radiotherapy in Patients with Breast Cancer. Journal of Clinical Medicine, 9(3), 666. https://doi.org/10.3390/jcm9030666






