1. Introduction
Fungal infections are an important chapter in infectious diseases and their incidence has increased considerably since the 1980′s, due to the widespread use of antibiotics, corticosteroids, cytotoxic, and immunosuppressive drugs. These infections are now an increasingly common problem and more difficult to manage, especially in intensive care units, with a number of difficulties in diagnosis, treatment and a very high mortality rate [
1].
Candida albicans is responsible for causing two major types of infections: local (oral or vaginal) and systemic infections. Local infections can affect both the oropharynx and the esophagus, leading to dysfunctions of the adaptive immune system [
2].
The study on antifungal antibiotics is a growing field due to the need to fight fungal infections; in recent years, new chemical compounds with lower toxicity and with significant antifungal action have been introduced into therapy. Among them:
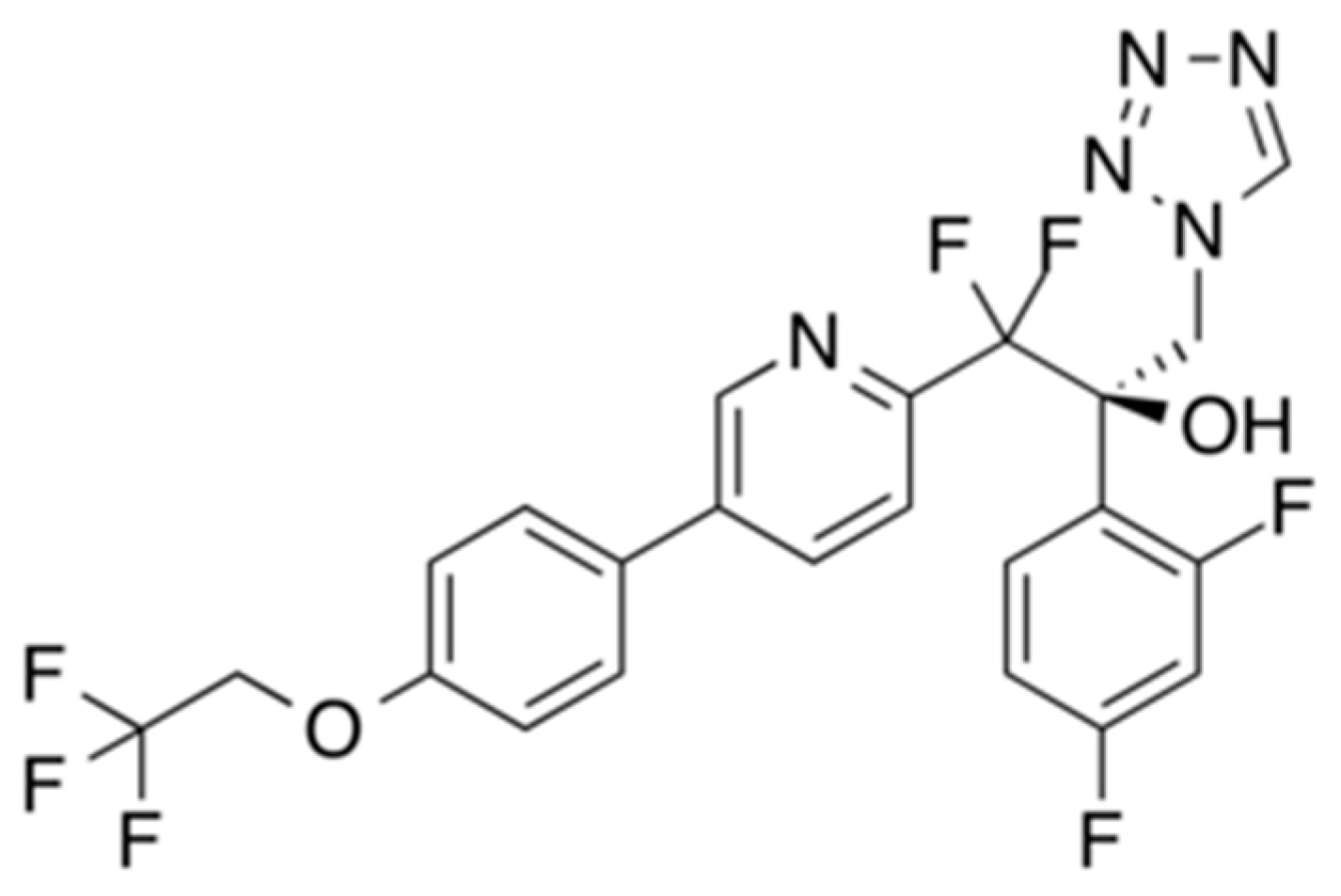
VT-1161, a tetrazole developed by Viamet Pharmaceuticals (
Figure 1), is a novel ergosterol synthesis inhibitor targeting fungal CYP51 (lanosterol 14 α-demethylase), that has been in phase 2 clinical trials for the treatment of vaginal candidiasis since 2013 [
3,
4]. Warrilow et al. have demonstrated that VT-1161 binds tightly to
C. albicans CYP51 and thus inhibits cellular function and that it also weakly inhibits human enzymes, such as CYP2C9, CYP2C19, and CYP3A4. The lack of interference with human enzymes suggests that VT-1161 may potentially have fewer negative drug interactions, thereby overcoming a major problem with triazoles. In addition, VT-1161 retains high in vitro potency against several
C. albicans isolates that are clinically resistant to fluconazole.
SCY-078 (formerly MK-3118,
Figure 2) is a potential oral glucan synthase inhibitor candidate currently used in clinical trials. SCY-078 exhibits broad-spectrum antifungal activity against several
Candida species and is also effective against filamentous fungi, including
Aspergillus fumigatus,
Paecilomyces variotii, and
Scedosporium prolificans, indicating that it is a promising antifungal agent [
5,
6].
Although there are a number of drugs used to treat these fungal infections, the need for new agents, such as new imidazole derivatives, has expanded due to increased resistance to drugs developed to date. Ketoconazole (
cis-1-acetyl-4-[4-[2-(2,4-dichlorophenyl)-2-(1H-imidazole-1-ylmethyl)-1,3-dioxolon-4-yl] methoxy] piperazin, was the first broad-spectrum antifungal drug administered orally and it is a highly effective broad spectrum antifungal agent, used in the treatment of a wide variety of superficial and systemic mycoses [
7]. It prevents the synthesis of ergosterol and the fungal equivalent of cholesterol and finally increases the membrane fluidity and prevents the growth of the fungus [
8]. According to the biopharmaceutics classification system, ketoconazole is classified as a class II drug, meaning that it has low solubility and high permeability. By using inclusion in cyclodextrins, this limitation can be reduced [
9,
10].
In 1891, Villers first described cyclodextrins, following Schardinger’s discovery of the three natural cyclodextrins, alpha, beta, and gamma types. Cyclodextrins, also called cycloamyloses, are cyclic macromolecules, belonging to the group of naturally occurring oligosaccharides, which are produced by enzymatic conversion of starch using amylase and glycosyltransferase. From a structural point of view, the cyclodxtrin molecule is rigid, arranged with a truncated architecture, which contains a hydrophilic part on the outside and a hydrophobic one inside the molecule, which makes them widely available in various fields. By encapsulation in the hydrophobic side, cyclodextrins (CD) form, hydrogen bonds with the hydroxide groups within the host molecules via Van der Waals interactions. Thus, through the encapsulation process, the compounds are protected by the action of external factors and can be released gradually in an aqueous environment, due to the stability between association-dissociation formed through the inclusion process [
9,
10,
11].
Due to their ability to incorporate various organic, inorganic, or biological molecules into the hydrophobic cavity, beta, and gamma cyclodextrins are widely used in the pharmaceutical industry. Studies have shown beneficial effects of the two “host” substances on the different drug substances. Thus, by encapsulation, the physical, chemical, and biological properties of medicinal substances can be strongly modified in order to optimize bioavailability and physico-chemical stability [
9,
10,
11,
12].
In this context, for the present study, we proposed going through the following stages in order to improve ketoconazole bioavailability: Laboratory synthesis of new derivatives based on imidazole nucleus, physico-chemical characterization, and spectral confirmation of intermediate and final compounds, obtaining new derivatives inclusion complexes with betacyclodextrin and evaluation of their antifungal action in both complexed and uncomplexed forms.
2. Materials and Methods
Starting from the idea of using aromatic aldehydes, in various reactions, to obtain compounds with reduced toxicity (which we used previously—[
9]), this time we proposed to modify the structure of ketoconazole, in order to reduce its tissue toxicity and increase its therapeutic effectiveness. Thus, to improve the antifungal potential and minimize chronic tissue toxicity of ketoconazole, we have obtained new condensation products, with a hydrazonic structure, by using two types of aromatic aldehydes: benzaldehyde and 2-hydroxy-benzaldehyde and further, betacyclodextrin (β-CD) was used to obtain the final inclusion complexes. All the reagents were purchased from Sigma–Aldrich (Romania), while β-CD was purchased from Acros Organics. All of the other materials were of analytical reagent grade and were used as received.
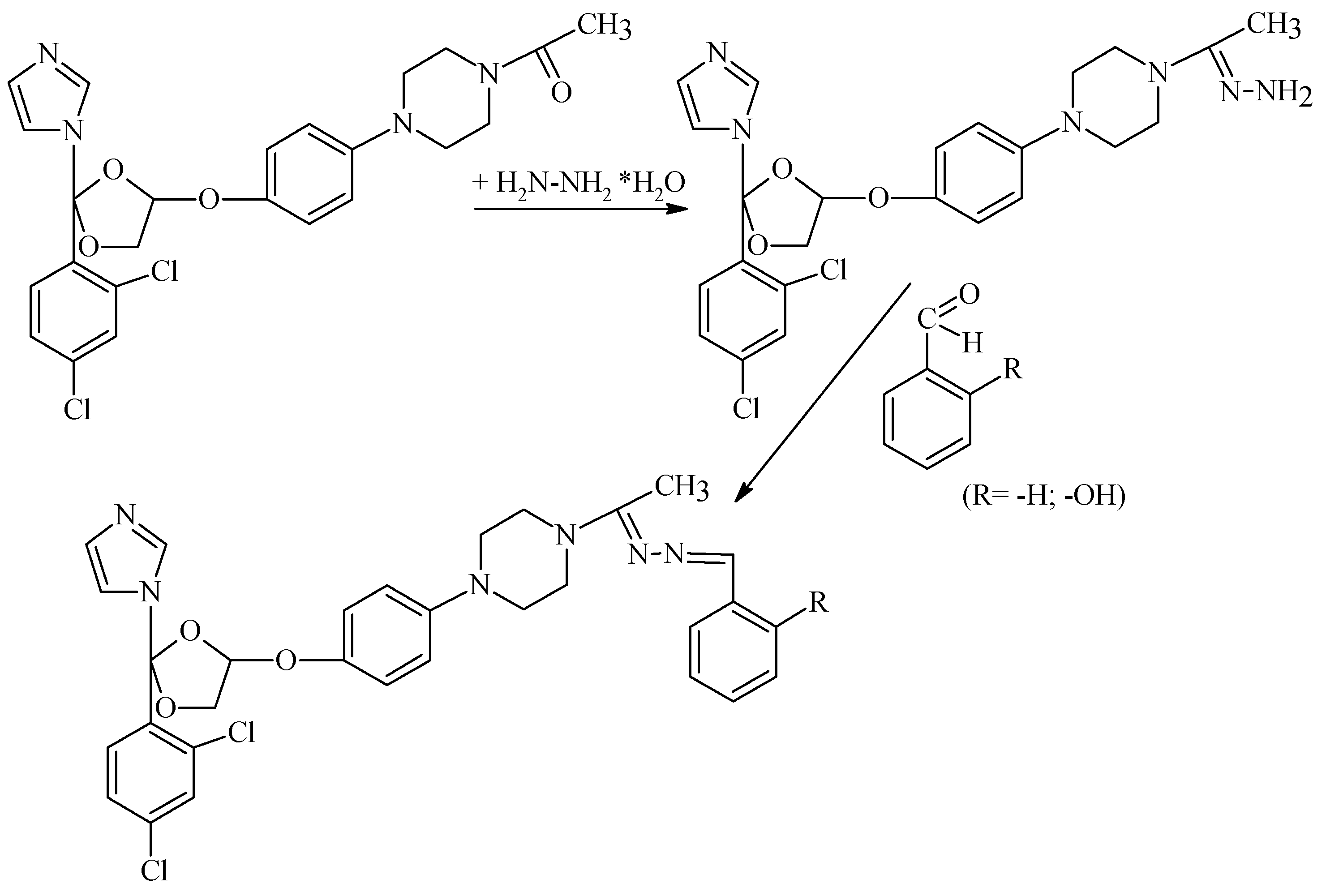
2.1. General Process for Obtaining Ketoconazole Condensation Hydrazones
The general synthesis scheme has been developed by adapting condensation methods to compounds of similar structure by using a 1:1 molar ratio [
13]. Thus, the synthesis of ketoconazole derivatives was initially based on the transformation of the parent compound into the corresponding hydrazine (here called Ketoc 1), followed by condensation with benzaldehyde and hydoxy-benzaldehyde, to obtain new hydrazones with imidazole nucleus (here called Ketoc 2 and Ketoc 3).
Thus, to obtain Ketoc 1, 5 g of Ketoconazole is treated with 1.35 mL of hydrazine hydrate (according to the molar ratio of 1:1 mentioned above), at boiling temperature, for 8 h. Further, Ketoc 2 and Ketoc 3 were obtained, in the same 1:1 molar ration, by condensing 1 g of ketoc 1 with 0.2 mL benzaldehyde (for ketoc 2) and hydroxy-benzaldehyde (for ketoc 3), in an absolute ethyl alcohol medium (50 mL) and glacial acetic acid (2–3 drops), the reaction mixture is maintained in a water bath under reflux, for another 8 h. The resulting precipitates are filtered off, washed with distilled water, dried at room temperature, and purified by recrystallization.
2.2. Physico-Chemical Characterization and Spectral Confirmation of Intermediate and Final Compounds
The new ketoconazole derivatives were characterized from a physico-chemical point of view (melting temperature, the reaction yield, the molecular formula, and the relative mass). In our case, the melting points were determined using a STUART melting point apparatus, SMP10, UK.
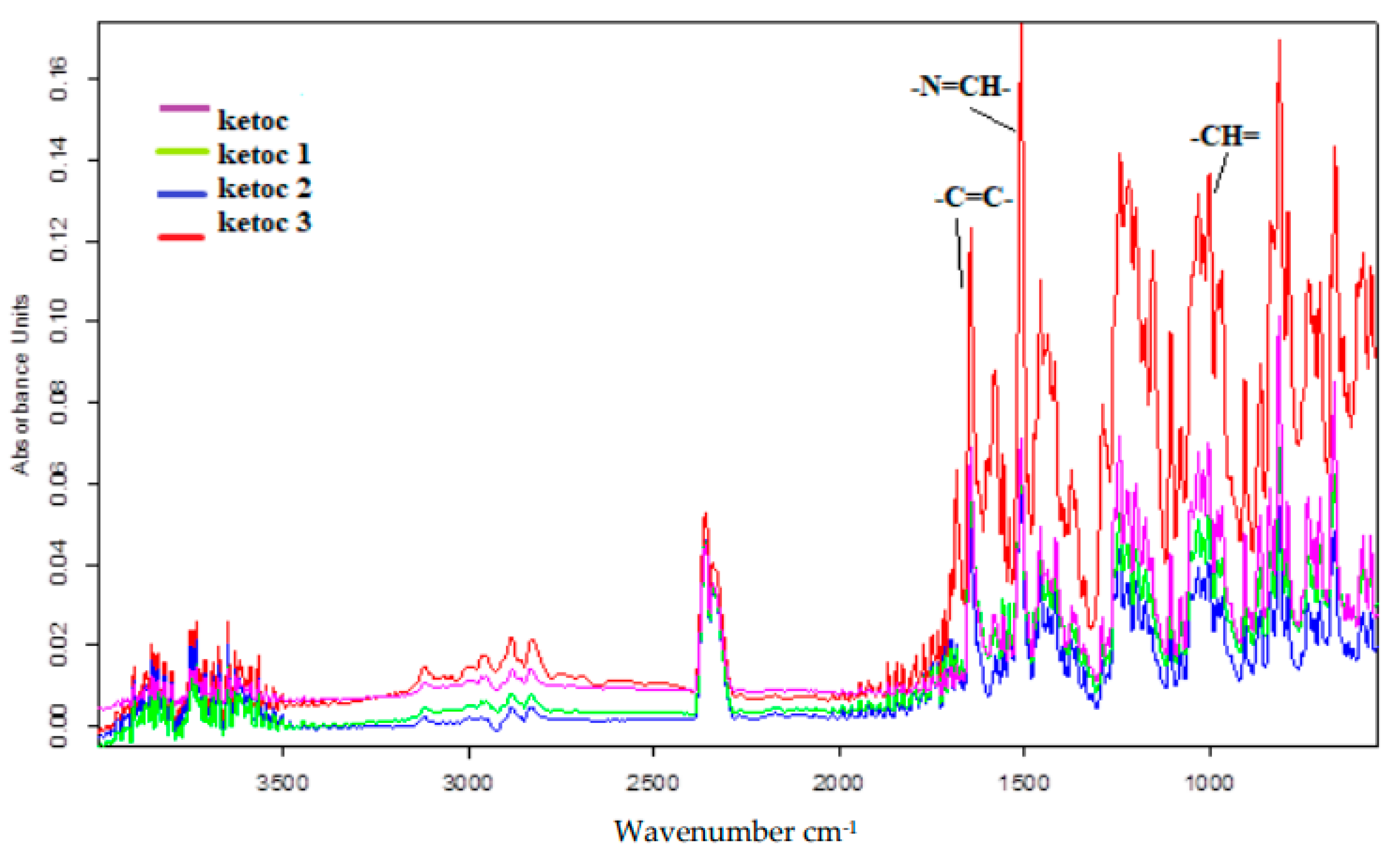
Confirmation of the chemical structure of the synthesized compounds was performed using as a spectral method, infrared spectroscopy (FT-IR). Infrared absorption spectroscopy is one of the most important techniques used in the investigation of matter being used to identify organic compounds by determining functional groups [
14].
The IR spectrum is a specific property of a pure compound, which is why it can provide information about its structure as well as its purity and concentration in a mixture. Infrared spectra of ketoconazole condensation products were recorded using an Agilent Cary 630 FTIR Spectrometer (USA), after 32 scans on a scale of 4000–500 cm−1, with a spectral resolution of 4 cm−1. Interpretation of the results was performed using Agilent MicoLab PC software, Automated IQ/OQ, 21 CFR Part 11compliant, Resolutions Pro for advanced data analysis.
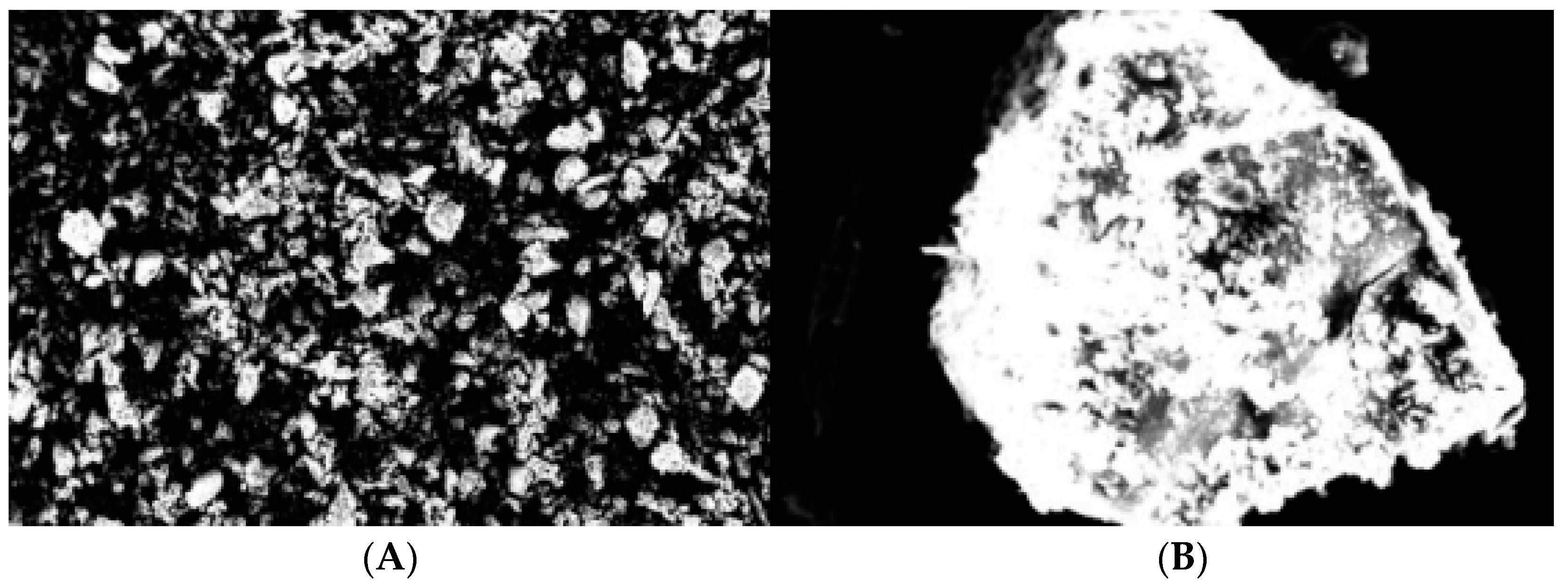
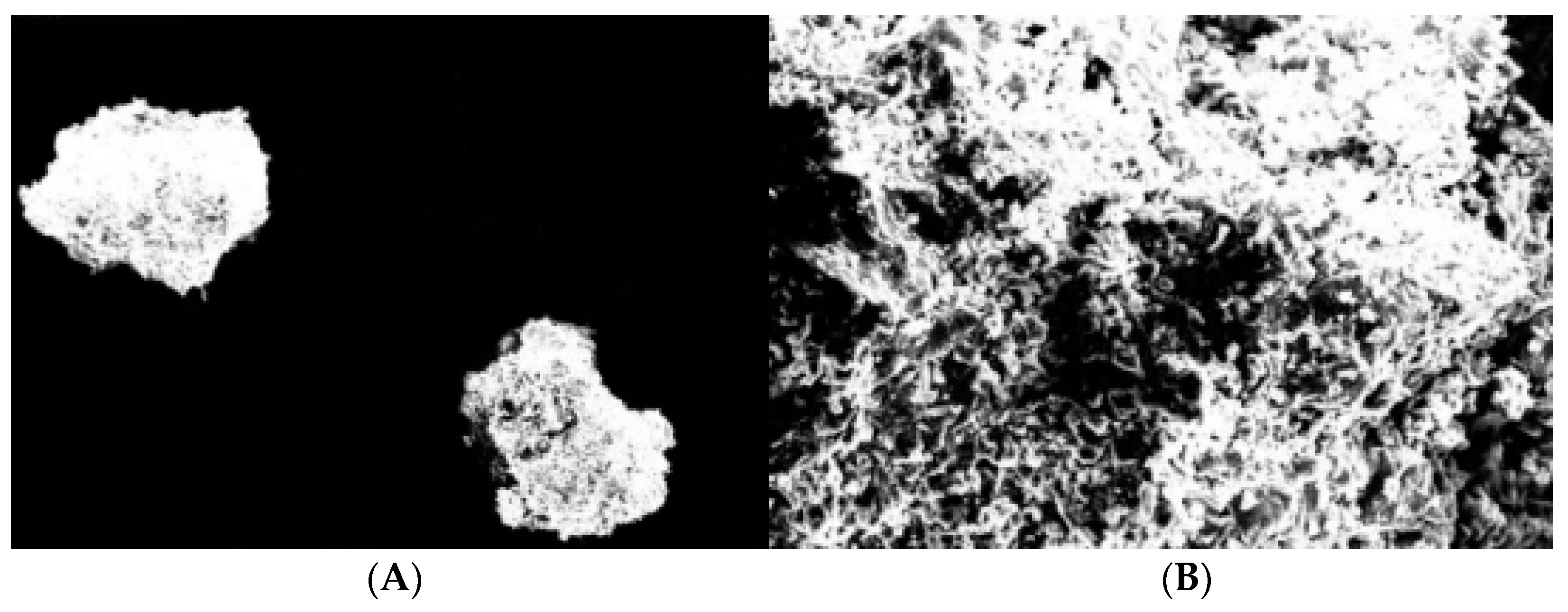
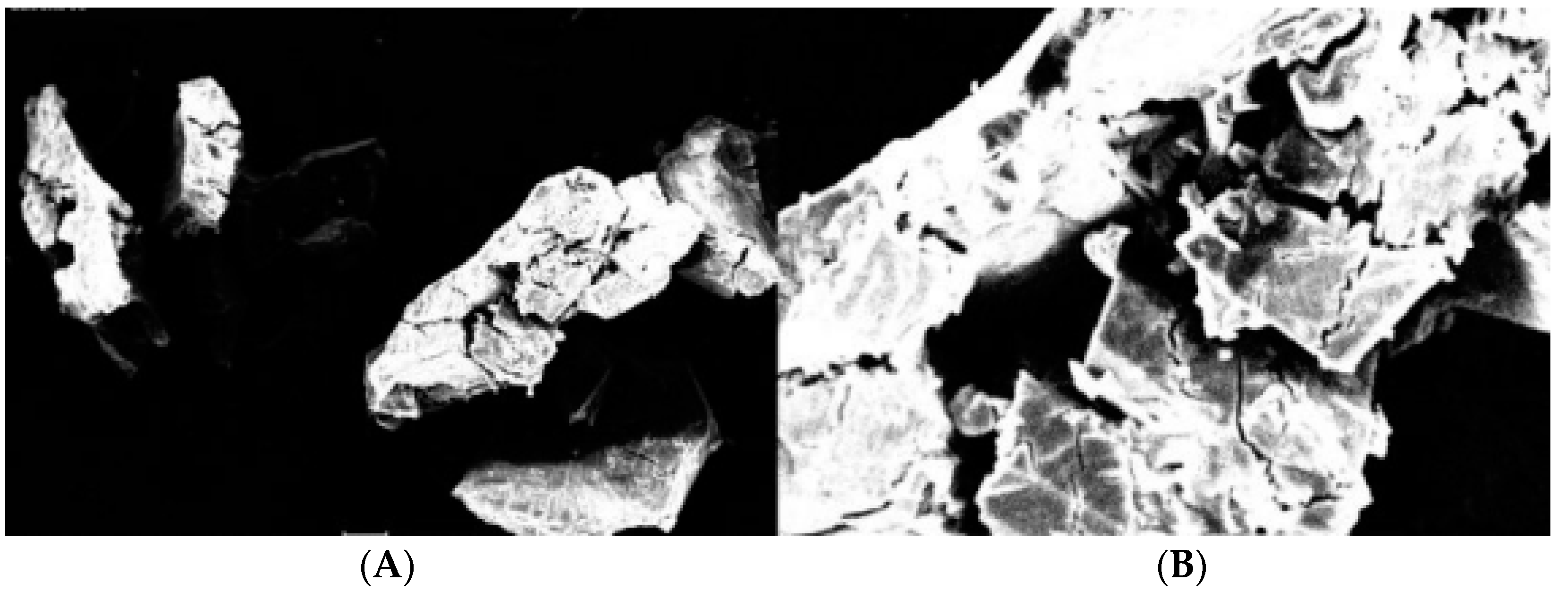
2.3. Obtaining and SEM Morphology of Inclusion Complexes with Betacyclodextrin
2.3.1. Physical Mixture Method
This method was carried out using a molar ratio of 1:1 between the ketoconazole derivative and betacyclodextrin. Both substances were brought into a mortar to obtain the desired physical mixture, through strong trituration, for a period of approximately three hours [
10].
2.3.2. Kneading Method
The method consists, initially, in the preparation of a homogeneous paste of beta-cyclodextrin, by forming a 1:1 molar mixture of water and methanol, this solvent was added in small quantities over the cyclodextrin. The ketoconazole derivative was added in small quantities to the paste thus obtained, kneading for 3 h. The obtained paste was subjected to drying, for 24 h, at 40–50 °C. The resulting complex was subsequently pulverized and stored in tightly closed boxes [
10].
2.3.3. Co-Precipitation Method
For this method, the active substance was added quantitatively in methanol, stirring continuously until dissolution. The cyclodextrin needed for the method (for the same 1:1 molar ratio) was weighed and dissolved in 10 mL of water at a temperature of 40–50 °C. After obtaining the cyclodextrin solution, the ketoconazole solution was added in drops under continuous stirring for six hours. The obtained solution was dried at 40–50 °C for 48 h, and the obtained complex was stored in tightly closed boxes [
10].
2.3.4. Solvent Evaporation Method
The last method was based on the dissolution of the ketoconazole derivative in acetone at a temperature of 25 °C, while the cyclodextrin was dissolved at a temperature of 40–50 °C, in water. The obtained cyclodextrin solution was added drop by drop over the solution of active substance, stirring continuously for four hours. The formed complex was filtered, and at the end, it underwent the drying process. The obtained product was pulverized in a mortar and finally stored in well-closed boxes [
10].
All the obtained complexes were characterized with the help of scanning electron microscopy. Thus, their morphology was studied by using a Desktop SEM (Phenom, The Nederlands).
2.4. Evaluation of the Antifungal Activity of Ketoconazole Derivatives and their BCD Inclusion Complexes
The antifungal activity of the compounds was studied using Candida albicans ATCC 90028 reference strain and also using 4 strains from patients with oral candidiasis admitted to the Emergency Clinical Hospital for Children, “St. Ioan” Galati. Ketoconazole was used as the reference agent for inhibitory activity against the tested fungi. 1% concentration was used for all complexed and non-complexed derivatives.
Disc-diffusion method: Antimicrobial tests were performed according to CLSI specifications [
15]. The fungal suspensions were inoculated on the surface of the Mueller Hinton medium with 2% glucose and methylene blue, spread in Petri plates. Sterile stainless-steel cylinders (8 mm internal diameter and 6 mm height) were applied on the agar surface in Petri plates, and 50 µL of each tested compound was added into cylinders. 1% of parent ketoconazole solution was used as positive control. For testing the antifungal activity, the plates were incubated at 35 °C/±2 °C for 24 h (or 48 h, if after 24 h there was no growth). After the incubation, the diameters of the inhibition area (mm) were measured.
4. Discussion
Fungal infections have emerged in recent decades as a growing global threat to human health. Mushrooms are generally opportunistic in nature, preying on hosts with compromised immune systems due to HIV infection or as a result of modern medical treatments, such as chemotherapy and organ transplantation [
16]. Moreover, these are more common in children and the elderly due to a weak immune system, while fungal infections between the fingers and in the groin are more common in men due to increased sweating [
17].
In contrast to the situation with antimicrobial agents, antifungal susceptibility testing has not been used in the past to guide antifungal therapy due to a lack of standardization of testing methodology. One of the methods for determining the sensitivity of fungi is currently the antifungigram, which shows us the stronger or weaker action of the therapeutic agents on different fungi [
18].
On the other hand, mechanisms of acquired resistance have arisen following the frequent and prophylactic use of antifungal agents, which has led to the development of significant resistance. Numerous mechanisms of fungal adaptation have been identified, including drug target modification, mutations, and genomic alterations [
19].
In this context, the choice of the right treatment and the observance of appropriate measures are the key points in the treatment of opportunistic infections. These measures include the prudent use of antifungals, appropriate dosage, with special emphasis on avoiding low-dose antifungal treatment, therapy with combinations of existing agents, appropriate antifungal treatment (in cases where the etiological agent is known), and the use of surveillance studies to determine the true reaction to antifungal drugs. In addition, advances in the rapid diagnosis of fungi may be helpful in reducing the use of antifungals that are unsuitable for treating resistant organisms to a particular agent.
The first reported azole compound with antifungal activity was achievedby Woolley in 1944, who declared for the first time the antifungal effect of the benzimidazole fragment. Later, other researchers indicated different azole antifungal structures, such as phenethylimidazole and substituted benzimidazoles, but the results obtained did not lead to the development of a drug until 1958, when chlorimidazole was introduced [
20,
21,
22].
Since the resistance of fungi to antifungals has increased in recent years, the synthesis of new compounds with antifungal action and lower toxicity was considered by many authors. Thus, in a recent study [
23], the antifungal activity of coumarin-piperazine hybrids has been demonstrated on different fungal strains (including
Candida albicans), for some of them, the antifungal effect is comparable to that of the fluconazole standard. In this case, both the piperazine and the coumarin components determined the achievement of a significant biological effect.
In the case of antifungal azoles, there are various changes made in the structure of these compounds, which have led to improvements in the safety, spectrum of action, and pharmacokinetics of the drugs. According to specialized literature, the disubstituted piperazine nucleus gives the compounds interesting biological properties, as it is the case of antifungal activity [
24].
For ketoconazole, an antifungal drug containing a heterocyclic dioxolane functional group corresponding to the previous azoles, the first structural changes were made, keeping the imidazolic residue [
25]. One of the main mechanisms to combat fungal infection, valid also in the case of ketoconazole, is damage to the cell membrane and the biosynthesis of ergosterol, which has an important role in cell proliferation [
26]. We can consider this mechanism of action also valid for the derivatives obtained in our study, as long as the basic imidazolic nucleus was kept in these cases, as well. However, in our case, the existence of certain obvious differences, regarding the antifungal activity of the uncomplexed compounds, compared to that of the complexed compounds with cyclodextrin, suggests that there may be additional modes of action or differential interactions with cellular components, such as drug efflux pumps [
27].
Another group of authors published in their work [
27] four new diphenyl-phosphane derivatives of ketoconazole. In this case, obtaining the derivatives was achieved by replacing the acetyl group from the ketoconazole molecule with –CH2PPh2 moiety and the phosphane chalcogenides: sulfide and selenide. In this case, the derivatization of ketoconazole, offered the possibility to develop a set of similar molecules, which are promising antifungal agents. Similar to our case, these authors also proposed the same mechanisms of action for ketoconazole derivatives.
Starting from ketoconazole, we obtained active compounds by condensation with benzaldehyde and hydoxy-benzaldehyde, which we later incorporated into betacyclodextrin. This inclusion step was used to increase the solubility of the reaction products, knowing that the synthesis of new ketoconazole derivatives can affect the solubility of the parent compound. In this context, two hydrazones of ketoconazole, were obtained and characterized from a physico-chemical and spectral point of view, determining: the melting temperature, reaction yield, molecular formula, and relative mass. The structures of the synthesized compounds were confirmed by IR spectral analysis. The IR spectra, recorded in the range 500–4000 cm−1, highlighted the group vibrations characteristic of all structural elements specific to each obtained compound: pyridine nucleus, aromatic nucleus, and the bond that marks the condensation of the two components (the azomethine group, respectively). Further, the complexation of less soluble derivatives considerably improves their solubility in water, which can increase the available concentration for the therapeutic effect.
In our case, the antifungal effect was highlighted (for all tested strains), on the one hand, due to the two active components: Piperazine and aromatic, substituted by active groups such as phenolic hydroxyl group and on the other hand, betacyclodextrin had an extremely important contribution to the antifungal effect, by increasing the solubility of the final compounds, and therefore by ensuring a higher concentration at the site of action. Thus, the activity of the ketoc 1 derivative complex, respectively, the hydrazine of ketoconazole, was best highlighted, the subsequent modifications made by coupling with benzaldehyde, causing a slight reduction of the antifungal activity.
5. Conclusions
Choosing the right treatment and following appropriate measures are the key points in treating opportunistic infections. These measures include prudent use of antifungals, appropriate dosing, with particular emphasis on avoiding low-dose antifungal therapy, combination therapy with existing agents, treatment with appropriate antifungals, and use of surveillance studies to determine the true response to antifungal drugs.
Modulation of ketoconazole structure offers the possibility of obtaining new compounds with potential use in antifungal therapy. Anticipating the mechanisms of resistance to antifungal therapy is the starting point for the development of new drugs, the ultimate goal being to increase the likelihood of a positive result with minimal toxic effects.
Since the antifungal potential and usefulness in the treatment of oropharyngeal candidiasis, in the case of derivatives with an imidazole nucleus, was demonstrated in this study, in the future we propose demonstrating their innocuousness through biocompatibility tests on cell cultures and also performing different in vivo studies.