Sporothrix brasiliensis: Epidemiology, Therapy, and Recent Developments
Abstract
:1. Introduction
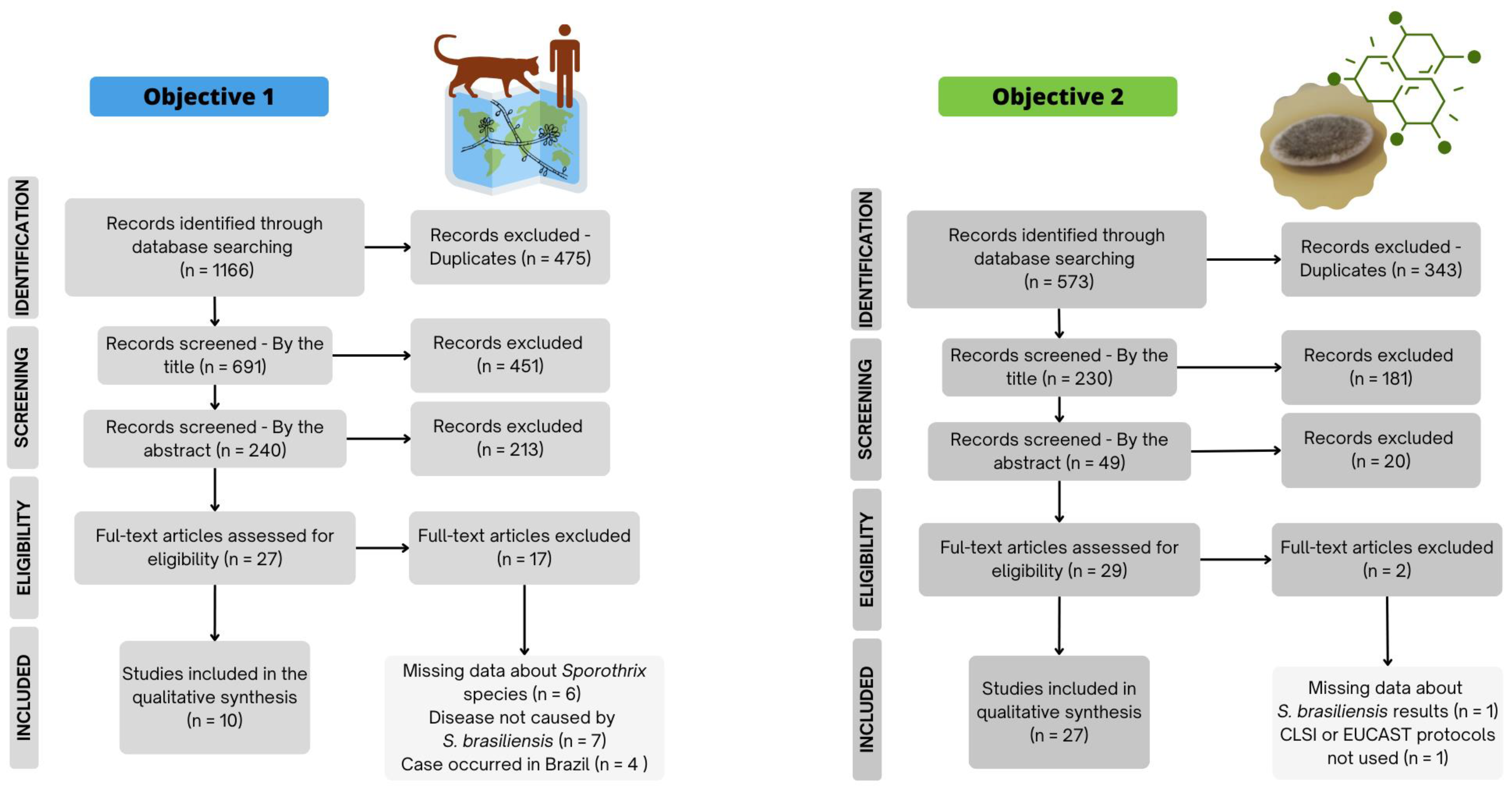
2. Materials and Methods
3. Results
3.1. Sporotrichosis Caused by S. brasiliensis Outside of Brazil
3.2. Drugs Tested (In Vitro and In Vivo) against This Pathogen
3.2.1. In Vitro Studies
3.2.2. Combination Therapy
3.2.3. In Vivo Studies
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Marimon, R.; Cano, J.; Gené, J.; Sutton, D.A.; Kawasaki, M.; Guarro, J. Sporothrix brasiliensis, S. globosa, and S. mexicana, Three New Sporothrix Species of Clinical Interest. J. Clin. Microbiol. 2007, 45, 3198–3206. [Google Scholar] [CrossRef]
- Sanchotene, K.O.; Madrid, I.M.; Klafke, G.B.; Bergamashi, M.; Terra, P.P.D.; Rodrigues, A.M.; de Camargo, Z.P.; Xavier, M.O. Sporothrix brasiliensis outbreaks and the rapid emergence of feline sporotrichosis. Mycoses 2015, 58, 652–658. [Google Scholar] [CrossRef] [PubMed]
- Rabello, V.B.S.; Almeida, M.A.; Bernardes-Engemann, A.R.; Almeida-Paes, R.; de Macedo, P.M.; Zancopé-Oliveira, R.M. The Historical Burden of Sporotrichosis in Brazil: A Systematic Review of Cases Reported from 1907 to 2020. Braz. J. Microbiol. 2022, 53, 231–244. [Google Scholar] [CrossRef] [PubMed]
- Nobre, M.O.; Potter-de-Castro, A.; Caetano, D.; Leonardo-de-Souza, L.A.-M.; Ferreiro, L.M.C. Recurrence of Sporotrichosis in Cats with Zoonotic Involvement. Rev. Iberoam. De Micol. 2001, 18, 137–140. [Google Scholar]
- Barros, M.B.; de Schubach, A.O.; do Valle, A.C.; Gutierrez Galhardo, M.C.; Conceição-Silva, F.; Schubach, T.M.; Reis, R.S.; Wanke, B.; Marzochi, K.B.; Conceição, M.J. Cat-Transmitted Sporotrichosis Epidemic in Rio de Janeiro, Brazil: Description of a Series of Cases. Clin. Infect. Dis. 2004, 38, 529–535. [Google Scholar] [CrossRef]
- Schubach, T.M.; Schubach, A.; Okamoto, T.; Barros, M.B.; Figueiredo, F.B.; Cuzzi, T.; Fialho-Monteiro, P.C.; Reis, R.S.; Perez, M.A.; Wanke, B. Evaluation of an Epidemic of Sporothricosis in Cats: 347 Cases (1998–2001). J. Am. Vet. Med. Assoc. 2004, 224, 1623–1629. [Google Scholar] [CrossRef]
- Madrid, I.M.; Mattei, A.S.; Fernandes, C.G.; Oliveira Nobre, M.; Meireles, M.C.A. Epidemiological Findings and Laboratory Evaluation of Sporotrichosis: A Description of 103 Cases in Cats and Dogs in Southern Brazil. Mycopathologia 2012, 173, 265–273. [Google Scholar] [CrossRef]
- Poester, V.R.; Mattei, A.S.; Madrid, I.M.; Pereira, J.T.B.; Klafke, G.B.; Sanchotene, K.O.; Brandolt, T.M.; Xavier, M.O. Sporotrichosis in Southern Brazil, towards an Epidemic? Zoonoses Public Health 2018, 65, 815–821. [Google Scholar] [CrossRef]
- Falcão, E.M.M.; Romão, A.R.; de Magalhães, M.A.F.M.; de Lima Filho, J.B.; do Valle, A.C.F.; Bastos, F.I.; Gutierrez-Galhardo, M.C.; Freitas, D.F.S. A Spatial Analysis of the Spread of Hyperendemic Sporotrichosis in the State of Rio de Janeiro, Brazil. J. Fungi 2022, 8, 434. [Google Scholar] [CrossRef]
- Gremião, I.D.F.; Oliveira, M.M.E.; Monteiro de Miranda, L.H.; Saraiva Freitas, D.F.; Pereira, S.A. Geographic Expansion of Sporotrichosis, Brazil. Emerg. Infect. Dis. 2020, 26, 621–624. [Google Scholar] [CrossRef]
- Munhoz, L.S.; Poester, V.R.; Severo, C.B.; Trápaga, M.R.; Madrid, I.M.; Benelli, J.L.; Stevens, D.A.; Xavier, M.O. Update of the Epidemiology of the Sporotrichosis Epidemic in the State of Rio Grande Do Sul, Brazil. Mycoses 2022, 65, 1112–1118. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention, CDC. Sporothrix brasiliensis. 2022. Available online: https://www.cdc.gov/fungal/port/sporotrichosis/brasiliensis.html (accessed on 17 July 2023).
- Gremião, I.D.F.; Martins da Silva da Rocha, E.; Montenegro, H.; Carneiro, A.J.B.; Xavier, M.O.; de Farias, M.R.; Monti, F.; Mansho, W.; de Macedo Assunção Pereira, R.H.; Pereira, S.A.; et al. Guideline for the Management of Feline Sporotrichosis Caused by Sporothrix brasiliensis and Literature Revision. Braz. J. Microbiol. 2020, 52, 107–124. [Google Scholar] [CrossRef] [PubMed]
- Marimon, R.; Gene, J.; Cano, J.; Guarro, J. Sporothrix luriei: A Rare Fungus from Clinical Origin. Med. Mycol. 2008, 46, 621–625. [Google Scholar] [CrossRef]
- Rodrigues, A.M.; Cruz Choappa, R.; Fernandes, G.F.; de Hoog, G.S.; de Camargo, Z.P. Sporothrix chilensis Sp. Nov. (Ascomycota: Ophiostomatales), a Soil-Borne Agent of Human Sporotrichosis with Mild-Pathogenic Potential to Mammals. Fungal Biol. 2016, 120, 246–264. [Google Scholar] [CrossRef] [PubMed]
- Moussa, T.A.A.; Kadasa, N.M.S.; Al Zahrani, H.S.; Ahmed, S.A.; Feng, P.; van den Ende, A.H.G.; Zhang, Y.; Kano, R.; Li, F.; Li, S.; et al. Origin and Distribution of Sporothrix globosa Causing Sapronoses in Asia. J. Med. Microbiol. 2017, 66, 560–569. [Google Scholar] [CrossRef]
- Zhang, Y.; Hagen, F.; Stielow, B.; Rodrigues, A.M.; Samerpitak, K.; Zhou, X.; Feng, P.; Yang, L.; Chen, M.; Deng, S.; et al. Phylogeography and Evolutionary Patterns in Sporothrix Spanning More than 14 000 Human and Animal Case Reports. Persoonia 2015, 35, 1–20. [Google Scholar] [CrossRef]
- Rojas, C.O.; Bonifaz, A.; Campos, C.; Treviño-Rangel, D.J.R.; González-Álvarez, R.; González, M.G. Molecular Identification, Antifungal Susceptibility, and Geographic Origin of Clinical Strains of Sporothrix schenckii Complex in Mexico. J. Fungi 2018, 4, 86. [Google Scholar] [CrossRef]
- García Duarte, J.M.; Wattiez Acosta, V.R.; Fornerón Viera, P.M.L.; Aldama Caballero, A.; Gorostiaga Matiauda, G.A.; Rivelli de Oddone, V.B.; Pereira Brunelli, J.G. Esporotricosis Trasmitida Por Gato Doméstico. Reporte de Un Caso Familiar. Rev. Del Nac. 2017, 9, 67–76. [Google Scholar]
- Córdoba, S.; Isla, G.; Szusz, W.; Vivot, W.; Hevia, A.; Davel, G.; Canteros, C.E. Molecular Identification and Susceptibility Profile of Sporothrix schenckii Sensu Lato Isolated in Argentina. Mycoses 2018, 61, 441–448. [Google Scholar] [CrossRef]
- Etchecopaz, A.N.; Lanza, N.; Toscanini, M.A.; Devoto, T.B.; Pola, S.J.; Daneri, G.L.; Iovannitti, C.A.; Cuestas, M.L. Refractory Sporotrichosis Due to Sporothrix brasiliensis in Argentina: Case Report, Molecular Identification and in Vitro Susceptibility Pattern to Antifungal Drugs. J. De Mycol. Méd. 2019, 30, 100908. [Google Scholar] [CrossRef]
- Kaadan, M.I.; Dennis, M.; Desai, N.; Yadavalli, G.; Lederer, P. One Health Education for Future Physicians: A Case Report of Cat-Transmitted Sporotrichosis. Open Forum Infect. Dis. 2020, 7, ofaa049. [Google Scholar] [CrossRef] [PubMed]
- Etchecopaz, A.; Toscanini, M.A.; Gisbert, A.; Mas, J.; Scarpa, M.; Iovannitti, C.A.; Bendezú, K.; Nusblat, A.D.; Iachini, R.; Cuestas, M.L. Sporothrix brasiliensis: A Review of an Emerging South American Fungal Pathogen, Its Related Disease, Presentation and Spread in Argentina. J. Fungi 2021, 7, 170. [Google Scholar] [CrossRef] [PubMed]
- Barnacle, J.R.; Chow, Y.J.; Borman, A.M.; Wyllie, S.; Dominguez, V.; Russell, K.; Roberts, H.; Armstrong-James, D.; Whittington, A.M. The First Three Reported Cases of Sporothrix brasiliensis Cat-Transmitted Sporotrichosis Outside South America. Med. Mycol. Case Rep. 2023, 39, 14–17. [Google Scholar] [CrossRef] [PubMed]
- Thomson, P.; González, C.; Blank, O.; Ramírez, V.; del Río, C.; Santibáñez, S.; Pena, P. Sporotrichosis Outbreak Due to Sporothrix brasiliensis in Domestic Cats in Magallanes, Chile: A One-Health-Approach Study. J. Fungi 2023, 9, 226. [Google Scholar] [CrossRef]
- Brandolt, T.M.; Madrid, I.M.; Poester, V.R.; Sanchotene, K.O.; Basso, R.P.; Klafke, G.B.; de Lima Rodrigues, M.; Xavier, M.O. Human Sporotrichosis: A Zoonotic Outbreak in Southern Brazil, 2012–2017. Med. Mycol. 2018, 57, 527–533. [Google Scholar] [CrossRef] [PubMed]
- Xavier, M.O.; Bittencourt, L.R.; Silva, C.M.; Vieira, R.S.; Pereira, H.C. Atypical Presentation of Sporotrichosis: Report of Three Cases. Rev. Da Soc. Bras. De Med. Trop. 2013, 46, 116–118. [Google Scholar] [CrossRef]
- Almeida-Paes, R.; de Oliveira, M.M.E.; Freitas, D.F.S.; do Valle, A.C.F.; Zancopé-Oliveira, R.M.; Gutierrez-Galhardo, M.C. Sporotrichosis in Rio de Janeiro, Brazil: Sporothrix brasiliensis Is Associated with Atypical Clinical Presentations. PLoS Negl. Trop. Dis. 2014, 8, e3094. [Google Scholar] [CrossRef]
- Poester, V.R.; Munhoz, L.S.; Basso, R.P.; Roca, B.M.; Vieira, M.U.; Melo, A.M.; Klafke, G.B.; Sanchotene, K.O.; Silveira, J.M.; Stevens, D.; et al. Disseminated Sporotrichosis with Immune Reconstitution Inflammatory Syndrome in an HIV Patient: Case Report and Review of the Literature. Rev. Iberoam. De Micol. 2020, 37, 97–99. [Google Scholar] [CrossRef]
- Procópio-Azevedo, A.C.; Rabello, V.B.S.; Muniz, M.M.; Figueiredo-Carvalho, M.H.G.; Almeida-Paes, R.; Zancopé-Oliveira, R.M.; Silva, J.C.A.L.; Macedo, P.M.; Valle, A.C.F.; Gutierrez-Galhardo, M.C.; et al. Hypersensitivity Reactions in Sporotrichosis: A Retrospective Cohort of 325 Patients from a Reference Hospital in Rio de Janeiro, Brazil (2005–2018). Br. J. Dermatol. 2021, 185, 1272–1274. [Google Scholar] [CrossRef]
- Fichman, V.; Mota-Damasceno, C.G.; Procópio-Azevedo, A.C.; Almeida-Silva, F.; de Macedo, P.M.; Medeiros, D.M.; Astacio, G.S.-M.; Zancopé-Oliveira, R.M.; Almeida-Paes, R.; Freitas, D.F.S.; et al. Pulmonary Sporotrichosis Caused by Sporothrix brasiliensis: A 22-Year, Single-Center, Retrospective Cohort Study. J. Fungi 2022, 8, 536. [Google Scholar] [CrossRef]
- Lima, M.A.; Freitas, D.F.S.; Oliveira, R.V.C.; Fichman, V.; Varon, A.G.; Freitas, A.D.; Lamas, C.C.; Andrade, H.B.; Veloso, V.G.; Almeida-Paes, R.; et al. Meningeal Sporotrichosis Due to Sporothrix brasiliensis: A 21-Year Cohort Study from a Brazilian Reference Center. J. Fungi 2022, 9, 17. [Google Scholar] [CrossRef] [PubMed]
- Arinelli, A.; Aleixo, A.L.Q.C.; Freitas, D.F.S.; do Valle, A.C.F.; Almeida-Paes, R.; Nobre Guimarães, A.L.; Oliveira, R.V.C.; Gutierrez-Galhardo, M.C.; Curi, A.L.L. Ocular Manifestations of Sporotrichosis in a Hyperendemic Region in Brazil: Description of a Series of 120 Cases. Ocul. Immunol. Inflamm. 2023, 31, 329–337. [Google Scholar] [CrossRef] [PubMed]
- Izoton, C.F.G.; de Brito Sousa, A.X.; Valete, C.M.; de Schubach, A.O.; Procópio-Azevedo, A.C.; Zancopé-Oliveira, R.M.; de Macedo, P.M.; Gutierrez-Galhardo, M.C.; Castro-Alves, J.; Almeida-Paes, R.; et al. Sporotrichosis in the Nasal Mucosa: A Single-Center Retrospective Study of 37 Cases from 1998 to 2020. PLoS Negl. Trop. Dis. 2023, 17, e0011212. [Google Scholar] [CrossRef] [PubMed]
- Falcão, E.M.M.; de Pires, M.C.S.; Andrade, H.B.; Gonçalves, M.L.C.; Almeida-Paes, R.; do Valle, A.C.F.; Bastos, F.I.; Gutierrez-Galhardo, M.C.; Freitas, D.F.S. Zoonotic Sporotrichosis with Greater Severity in Rio de Janeiro, Brazil: 118 Hospitalizations and 11 Deaths in the Last 2 Decades in a Reference Institution. Med. Mycol. 2020, 58, 141–143. [Google Scholar] [CrossRef] [PubMed]
- de Souza, E.W.; de Borba, C.M.; Pereira, S.A.; Gremião, I.D.F.; Langohr, I.M.; Oliveira, M.M.E.; de Oliveira, R.D.V.C.; da Cunha, C.R.; Zancopé-Oliveira, R.M.; de Miranda, L.H.M.; et al. Clinical Features, Fungal Load, Coinfections, Histological Skin Changes, and Itraconazole Treatment Response of Cats with Sporotrichosis Caused by Sporothrix brasiliensis. Sci. Rep. 2018, 8, 9074. [Google Scholar] [CrossRef]
- De Miranda, L.H.M.; Meli, M.; Conceição-Silva, F.; Novacco, M.; Menezes, R.C.; Pereira, S.A.; Sugiarto, S.; dos Reis, É.G.; Gremião, I.D.F.; Hofmann-Lehmann, R. Co-Infection with Feline Retrovirus Is Related to Changes in Immunological Parameters of Cats with Sporotrichosis. PLoS ONE 2018, 13, e0207644. [Google Scholar] [CrossRef]
- Hofmann-Lehmann, R.; Hartmann, K. Feline Leukaemia Virus Infection: A Practical Approach to Diagnosis. J. Feline Med. Surg. 2020, 22, 831–846. [Google Scholar] [CrossRef]
- Pereira, S.A.; Gremião, I.D.F.; Kitada, A.A.B.; Boechat, J.S.; Viana, P.G.; Schubach, T.M.P. The epidemiological scenario of feline sporotrichosis in Rio de Janeiro, State of Rio de Janeiro, Brazil. Rev. Da Soc. Bras. De Med. Trop. 2014, 47, 392–393. [Google Scholar] [CrossRef]
- Gremião, I.D.F.; Schubach, T.M.P.; Pereira, S.A.; Rodrigues, A.M.; Honse, C.O.; Barros, M.B.L. Treatment of Refractory Feline Sporotrichosis with a Combination of Intralesional Amphotericin B and Oral Itraconazole. Aust. Vet. J. 2011, 89, 346–351. [Google Scholar] [CrossRef]
- Reis, E.G.; Gremião, I.D.F.; Kitada, A.A.B.; Rocha, R.F.D.B.; Castro, V.S.P.; Barros, M.B.L.; Menezes, R.C.; Pereira, S.A.; Schubach, T.M.P. Potassium Iodide Capsule Treatment of Feline Sporotrichosis. J. Feline Med. Surg. 2012, 14, 399–404. [Google Scholar] [CrossRef]
- de Miranda, L.H.; Silva, J.N.; Gremião, I.D.; Menezes, R.C.; Almeida-Paes, R.; Dos Reis, É.G.; De Oliveira, R.D.; De Araujo, D.S.; Ferreiro, L.; Pereira, S.A. Monitoring Fungal Burden and Viability of Sporothrix spp. in Skin Lesions of Cats for Predicting Antifungal Treatment Response. J. Fungi 2018, 4, 92. [Google Scholar] [CrossRef]
- de Barros, M.B.L.; Schubach, A.O.; de Oliveira, R.D.V.C.; Martins, E.B.; Teixeira, J.L.; Wanke, B. Treatment of cutaneous sporotrichosis with itraconazole—Study of 645 patients. Clin. Infect. Dis. 2011, 52, e200–e206. [Google Scholar] [CrossRef] [PubMed]
- Poester, V.R.; Basso, R.P.; Stevens, D.A.; Munhoz, L.S.; de Souza Rabello, V.B.; Almeida-Paes, R.; Zancopé-Oliveira, R.M.; Zanchi, M.; Benelli, J.L.; Xavier, M.O. Treatment of Human Sporotrichosis Caused by Sporothrix brasiliensis. J. Fungi 2022, 8, 70. [Google Scholar] [CrossRef] [PubMed]
- Kauffman, C.A.; Bustamante, B.; Chapman, S.W.; Pappas, P.G. Clinical Practice Guidelines for the Management of Sporotrichosis: 2007 Update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2007, 45, 1255–1265. [Google Scholar] [CrossRef] [PubMed]
- Vilela, R.; Souza, G.F.; Cota, G.F.; Mendoza, L. Cutaneous and Meningeal Sporotrichosis in a HIV Patient. Rev. Iberoam. De Micol. 2007, 24, 161–163. [Google Scholar] [CrossRef] [PubMed]
- Xue, S.; Gu, R.; Wu, T.; Zhang, M.; Wang, X. Oral Potassium Iodide for the Treatment of Sporotrichosis. Cochrane Libr. 2009, 4, CD006136. [Google Scholar] [CrossRef]
- Poester, V.R.; Mattei, A.S.; Mendes, J.F.; Klafke, G.B.; Ramis, I.B.; Sanchotene, K.O.; Xavier, M.O. Antifungal Activity of Diphenyl Diselenide Alone and in Combination with Itraconazole against Sporothrix brasiliensis. Med. Mycol. 2018, 57, 328–331. [Google Scholar] [CrossRef]
- Borba-Santos, L.P.; Nucci, M.; Ferreira-Pereira, A.; Rozental, S. Anti-Sporothrix Activity of Ibuprofen Combined with Antifungal. Braz. J. Microbiol. 2020, 52, 101–106. [Google Scholar] [CrossRef]
- Munhoz, L.S.; Poester, V.R.; Benelli, J.L.; Melo, A.M.; Trápaga, M.R.; Nogueira, C.W.; Zeni, G.; Flores, M.M.; Stevens, D.A.; Xavier, M.O. Effectiveness of Diphenyl Diselenide against Experimental Sporotrichosis Caused by Sporothrix brasiliensis. Med. Mycol. 2023, 61, myad035. [Google Scholar] [CrossRef]
- Borba-Santos, L.P.; Reis de Sá, L.F.; Ramos, J.A.; Rodrigues, A.M.; de Camargo, Z.P.; Rozental, S.; Ferreira-Pereira, A. Tacrolimus Increases the Effectiveness of Itraconazole and Fluconazole against Sporothrix spp. Front. Microbiol. 2017, 8, 1759. [Google Scholar] [CrossRef]
- Almeida-Paes, R.; de Andrade, I.B.; Ramos, M.L.M.; de Rodrigues, M.V.A.; do Nascimento, V.A.; Bernardes-Engemann, A.R.; Frases, S. Medicines for Malaria Venture COVID Box: A Source for Repurposing Drugs with Antifungal Activity against Human Pathogenic Fungi. Memórias Do Inst. Oswaldo Cruz 2021, 116, e210207. [Google Scholar] [CrossRef] [PubMed]
- Poester, V.R.; Munhoz, L.S.; Larwood, D.; Martinez, M.; Stevens, D.A.; Xavier, M.O. Potential Use of Nikkomycin Z as an Anti-Sporothrix spp. Drug. Med. Mycol. 2020, 59, 345–349. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. BMJ 2009, 339, b2535. [Google Scholar] [CrossRef]
- Etchecopaz, A.; Scarpa, M.; Mas, J.; Cuestas, M.L. Sporothrix brasiliensis: A Growing Hazard in the Northern Area of Buenos Aires Province? Rev. Argent. De Microbiol. 2020, 52, 350–351. [Google Scholar] [CrossRef] [PubMed]
- Rachman, R.; Ligaj, M.; Chinthapalli, S.; Serafino Wani, R. Zoonotic Acquisition of Cutaneous Sporothrix braziliensis Infection in the UK. BMJ Case Rep. 2022, 15, e248418. [Google Scholar] [CrossRef]
- Rodriguez, C.H.V.; Cañataro, P.A.; Abusamra, L.; Farbman, M.A.; Daneri, A.G.L.; Mujica, M.T. Oral Terbinafine and Itraconazole Therapy Against Sporothrix brasiliensis an Emerging Species in Argentina. Mycopathologia 2023, 188, 287–289. [Google Scholar] [CrossRef]
- Brilhante, R.S.; Pereira, V.S.; Oliveira, J.S.; Lopes, R.G.; Rodrigues, A.M.; Camargo, Z.P.; Pereira-Neto, W.A.; Castelo-Branco, D.S.; Cordeiro, R.A.; Sidrim, J.J.; et al. Pentamidine Inhibits the Growth of Sporothrix schenckii Complex and Exhibits Synergism with Antifungal Agents. Future Microbiol. 2018, 13, 1129–1140. [Google Scholar] [CrossRef]
- Brilhante, R.S.N.; Malaquias, Â.D.M.; Caetano, É.P.; de Castelo-Branco, D.S.C.M.; de Lima, R.A.C.; de Farias Marques, F.J.; Silva, N.F.; de Alencar, L.P.; Monteiro, A.J.; de Camargo, Z.P.; et al. In Vitro Inhibitory Effect of Miltefosine against Strains of Histoplasma Capsulatum var. Capsulatum and Sporothrix spp. Med. Mycol. 2014, 52, 320–325. [Google Scholar] [CrossRef]
- Brilhante, R.S.N.; da Silva, M.L.Q.; Pereira, V.S.; de Oliveira, J.S.; Maciel, J.M.; da Silva, I.N.G.; Garcia, L.G.S.; de Melo Guedes, G.M.; de Aguiar Cordeiro, R.; de Aquino Pereira-Neto, W.; et al. Potassium Iodide and Miltefosine Inhibit Biofilms of Sporothrix schenckii Species Complex in Yeast and Filamentous Forms. Med. Mycol. 2019, 57, 764–772. [Google Scholar] [CrossRef]
- Borba-Santos, L.P.; Barreto, T.L.; Vila, T.; Chi, K.D.; dos Santos Monti, F.; de Farias, M.R.; Alviano, D.S.; Alviano, C.S.; Futuro, D.O.; Ferreira, V.; et al. In Vitro and In Vivo Antifungal Activity of Buparvaquone against Sporothrix brasiliensis. Antimicrob. Agents Chemother. 2021, 65, AAC0069921. [Google Scholar] [CrossRef]
- Borba-Santos, L.P.; Gagini, T.; Ishida, K.; de Souza, W.; Rozental, S. Miltefosine Is Active against Sporothrix brasiliensis Isolates with in Vitro Low Susceptibility to Amphotericin B or Itraconazole. J. Med. Microbiol. 2015, 64, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Borba-Santos, L.P.; Nicoletti, C.D.; Vila, T.; Ferreira, P.G.; Araújo-Lima, C.F.; Galvão, B.V.D.; Felzenszwalb, I.; de Souza, W.; de Carvalho da Silva, F.; Ferreira, V.F.; et al. A Novel Naphthoquinone Derivative Shows Selective Antifungal Activity against Sporothrix Yeasts and Biofilms. Braz. J. Microbiol. 2022, 53, 749–758. [Google Scholar] [CrossRef] [PubMed]
- Borba-Santos, L.P.; Rollin-Pinheiro, R.; da Silva Fontes, Y.; dos Santos, G.M.P.; de Sousa Araújo, G.R.; Rodrigues, A.M.; Guimarães, A.J.; de Souza, W.; Frases, S.; Ferreira-Pereira, A.; et al. Screening of Pandemic Response Box Library Reveals the High Activity of Olorofim against Pathogenic Sporothrix Species. J. Fungi 2022, 8, 1004. [Google Scholar] [CrossRef]
- Borba-Santos, L.P.; Vila, T.; Rozental, S. Identification of Two Potential Inhibitors of Sporothrix brasiliensis and Sporothrix schenckii in the Pathogen Box Collection. PLoS ONE 2020, 15, e0240658. [Google Scholar] [CrossRef] [PubMed]
- Borba-Santos, L.P.; Visbal, G.; Gagini, T.; Rodrigues, A.M.; de Camargo, Z.P.; Lopes-Bezerra, L.M.; Ishida, K.; de Souza, W.; Rozental, S. Δ24-Sterol Methyltransferase Plays an Important Role in the Growth and Development of Sporothrix schenckii and Sporothrix brasiliensis. Front. Microbiol. 2016, 7, 311. [Google Scholar] [CrossRef]
- Waller, S.B.; Nakasu, C.; Silva, A.L.; de Faria, R.O.; dos Santos Fernandes, J.P.; Cleff, M.B. Anti-Sporothrix brasiliensis Activity of Different Pyrazinoic Acid Prodrugs: A Repurposing Evaluation. Braz. J. Pharm. Sci. 2018, 54, e17858. [Google Scholar] [CrossRef]
- Asquith, C.R.M.; Machado, A.C.S.; de Miranda, L.H.M.; Konstantinova, L.S.; Almeida-Paes, R.; Rakitin, O.A.; Pereira, S.A. Synthesis and Identification of Pentathiepin-Based Inhibitors of Sporothrix brasiliensis. Antibiotics 2019, 8, 249. [Google Scholar] [CrossRef]
- Garcia Ferreira, P.; Pereira Borba-Santos, L.; Noronha, L.; Deckman Nicoletti, C.; de Sá Haddad Queiroz, M.; de Carvalho da Silva, F.; Rozental, S.; Omena Futuro, D.; Francisco Ferreira, V. Synthesis, Stability Studies, and Antifungal Evaluation of Substituted α- and β-2,3-Dihydrofuranaphthoquinones against Sporothrix brasiliensis and Sporothrix schenckii. Molecules 2019, 24, 930. [Google Scholar] [CrossRef]
- Artunduaga Bonilla, J.J.; Honorato, L.; Guimarães, A.J.; Miranda, K.; Nimrichter, L. Silver Chitosan Nanocomposites Are Effective to Combat Sporotrichosis. Front. Nanotechnol. 2022, 4, 857681. [Google Scholar] [CrossRef]
- Artunduaga Bonilla, J.J.; Honorato, L.; Haranahalli, K.; Dib Ferreira Gremião, I.; Pereira, S.A.; Guimarães, A.; de Souza Baptista, A.R.; de Melo Tavares, P.; Rodrigues, M.L.; Miranda, K.; et al. Antifungal Activity of Acylhydrazone Derivatives against Sporothrix spp. Antimicrob. Agents Chemother. 2021, 65, e02593-20. [Google Scholar] [CrossRef]
- De Azevedo-França, J.A.; Granado, R.; de Macedo Silva, S.T.; dos Santos-Silva, G.; Scapin, S.; Borba-Santos, L.P.; Rozental, S.; de Souza, W.; Martins-Duarte, É.S.; Barrias, E.; et al. Synthesis and Biological Activity of Novel Zinc-Itraconazole Complexes in Protozoan Parasites and Sporothrix spp. Antimicrob. Agents Chemother. 2020, 64, 111401. [Google Scholar] [CrossRef] [PubMed]
- Azevedo-França, J.A.; Borba-Santos, L.P.; de Almeida Pimentel, G.; Franco, C.H.J.; Souza, C.; de Almeida Celestino, J.; de Menezes, E.F.; dos Santos, N.P.; Vieira, E.G.; Ferreira, A.M.D.C.; et al. Antifungal Promising Agents of Zinc(II) and Copper(II) Derivatives Based on Azole Drug. J. Inorg. Biochem. 2021, 219, 111401. [Google Scholar] [CrossRef] [PubMed]
- Garcia, L.G.S.; de Melo Guedes, G.M.; Fonseca, X.M.Q.C.; Pereira-Neto, W.A.; Castelo-Branco, D.S.C.M.; Sidrim, J.J.C.; de Aguiar Cordeiro, R.; Rocha, M.F.G.; Vieira, R.S.; Brilhante, R.S.N. Antifungal activity of different molecular weight chitosans against planktonic cells and biofilm of Sporothrix brasiliensis. Int. J. Biol. Macromol. 2020, 143, 341–348. [Google Scholar] [CrossRef]
- Seibert, G.; Poletto, A.L.R.; Prade, J.V.; Mario, D.N.; Stopiglia, C.D.O. Reversal of Itraconazole Resistance in Sporothrix brasiliensis and Sporothrix schenckii by Nonsteroidal Anti-Inflammatory Drugs. Rev. Iberoam. De Micol. 2022, 39, 68–71. [Google Scholar] [CrossRef] [PubMed]
- Brandolt, T.M.; Klafke, G.B.; Ramos, D.F.; Halicki, P.C.B.; de Vicenti, J.R.M.; Pereira, W.A.; Poester, V.R.; Sanchotene, K.O.; Xavier, M.O. In Vitro Susceptibility of Sporothrix spp. to Complexes Coordinated with Co(II) and Cobalt Chloride Hexahydrate. Braz. J. Pharm. Sci. 2022, 58, e20152. [Google Scholar] [CrossRef]
- de Souza, L.C.D.S.V.; Alcântara, L.M.; de Macêdo-Sales, P.A.; Reis, N.F.; de Oliveira, D.S.; Machado, R.L.D.; Geraldo, R.B.; dos Santos, A.L.S.; Ferreira, V.F.; Gonzaga, D.T.G.; et al. Synthetic Derivatives against Wild-Type and Non-Wild-Type Sporothrix brasiliensis: In Vitro and In Silico Analyses. Pharmaceuticals 2022, 15, 55. [Google Scholar] [CrossRef]
- dos Santos, G.M.P.; Borba-Santos, L.P.; Vila, T.; Ferreira Gremião, I.D.; Pereira, S.A.; de Souza, W.; Rozental, S. Sporothrix spp. Biofilms Impact in the Zoonotic Transmission Route: Feline Claws Associated Biofilms, Itraconazole Tolerance, and Potential Repurposing for Miltefosine. Pathogens 2022, 11, 206. [Google Scholar] [CrossRef]
- Poester, V.R.; Munhoz, L.S.; Stevens, D.A.; Melo, A.M.; Trápaga, M.R.; Flores, M.M.; Larwood, D.J.; Xavier, M.O. Nikkomycin Z for the Treatment of Experimental Sporotrichosis Caused by Sporothrix brasiliensis. Mycoses 2023, 66, 898–905. [Google Scholar] [CrossRef]
- Brazil, M.D.S. Nota Técnica Acerca de Recomendações Sobre a Vigilância da Esporotricose Animal No Brasil. 2023. Available online: https://www.gov.br/saude/pt-br/centrais-de-conteudo/publicacoes/notas-tecnicas/2023/nota-tecnica-no-60-2023-cgzv-dedt-svsa-ms/view (accessed on 17 July 2023).
- Eudes Filho, J.; dos Santos, I.B.; Reis, C.M.S.; Patané, J.S.L.; Paredes, V.; Bernardes, J.P.R.A.; dos Poggiani, S.S.C.; de Castro, T.C.B.; Gomez, O.M.; Pereira, S.A.; et al. A Novel Sporothrix brasiliensis Genomic Variant in Midwestern Brazil: Evidence for an Older and Wider Sporotrichosis Epidemic. Emerg. Microbes Infect. 2020, 9, 2515–2525. [Google Scholar] [CrossRef]
- de Losada, L.C.M.L.; Monteiro, R.C.; de Carvalho, J.A.; Hagen, F.; Fisher, M.C.; Spruijtenburg, B.; Meis, J.F.; de Groot, T.; Gonçalves, S.S.; Negroni, R.; et al. High-Throughput Microsatellite Markers Development for Genetic Characterization of Emerging Sporothrix species. J. Fungi 2023, 9, 354. [Google Scholar] [CrossRef]
- Spruijtenburg, B.; Bombassaro, A.; Meijer, E.F.J.; Rodrigues, A.M.; Grisolia, M.E.; Vicente, V.A.; de Queiroz-Telles, F.; Meis, J.F.; de Groot, T. Sporothrix brasiliensis Genotyping Reveals Numerous Independent Zoonotic Introductions in Brazil. J. Infect. 2023, 86, 610–613. [Google Scholar] [CrossRef] [PubMed]
- Müller, J.; Aguado-Martínez, A.; Manser, V.; Wong, H.N.; Haynes, R.K.; Hemphill, A. Repurposing of Antiparasitic Drugs: The Hydroxy-Naphthoquinone Buparvaquone Inhibits Vertical Transmission in the Pregnant Neosporosis Mouse Model. Vet. Res. 2016, 47, 32. [Google Scholar] [CrossRef] [PubMed]
- Lazzarini, C.; Haranahalli, K.; Rieger, R.; Ananthula, H.K.; Desai, P.B.; Ashbaugh, A.; Linke, M.J.; Cushion, M.T.; Ruzsicska, B.; Haley, J.; et al. Acylhydrazones as Antifungal Agents Targeting the Synthesis of Fungal Sphingolipids. Antimicrob. Agents Chemother. 2018, 62, e00156-18. [Google Scholar] [CrossRef]
- Lazzarini, C.; Haranahalli, K.; McCarthy, J.B.; Mallamo, J.; Ojima, I.; Del Poeta, M. Preclinical Evaluation of Acylhydrazone SB-AF-1002 as a Novel Broad-Spectrum Antifungal Agent. Antimicrob. Agents Chemother. 2020, 64, e00946-20. [Google Scholar] [CrossRef]
- You, C.; Li, Q.; Wang, X.; Wu, P.; Ho, J.K.; Jin, R.; Zhang, L.; Shao, H.; Han, C. Silver Nanoparticle Loaded Collagen/Chitosan Scaffolds Promote Wound Healing via Regulating Fibroblast Migration and Macrophage Activation. Sci. Rep. 2017, 7, 10489. [Google Scholar] [CrossRef]
- Sandri, G.; Miele, D.; Faccendini, A.; Bonferoni, M.C.; Rossi, S.; Grisoli, P.; Taglietti, A.; Ruggeri, M.; Bruni, G.; Vigani, B.; et al. Chitosan/Glycosaminoglycan Scaffolds: The Role of Silver Nanoparticles to Control Microbial Infections in Wound Healing. Polymers 2019, 11, 1207. [Google Scholar] [CrossRef] [PubMed]
- Cinteza, L.; Scomoroscenco, C.; Voicu, S.; Nistor, C.; Nitu, S.; Trica, B.; Jecu, M.-L.; Petcu, C. Chitosan-Stabilized Ag Nanoparticles with Superior Biocompatibility and Their Synergistic Antibacterial Effect in Mixtures with Essential Oils. Nanomaterials 2018, 8, 826. [Google Scholar] [CrossRef]
- Dakal, T.C.; Kumar, A.; Majumdar, R.S.; Yadav, V. Mechanistic Basis of Antimicrobial Actions of Silver Nanoparticles. Front. Microbiol. 2016, 7, 1831. [Google Scholar] [CrossRef]
- Durán, N.; Durán, M.; de Jesus, M.B.; Seabra, A.B.; Fávaro, W.J.; Nakazato, G. Silver Nanoparticles: A New View on Mechanistic Aspects on Antimicrobial Activity. Nanomed. Nanotechnol. Biol. Med. 2016, 12, 789–799. [Google Scholar] [CrossRef]
- Bem, A.F.D.; Portella, R.D.L.; Farina, M.; Perottoni, J.; Paixão, M.W.; Nogueira, C.W.; Rocha, T. Low Toxicity of Diphenyl Diselenide in Rabbits: A Long-Term Study. Basic Clin. Pharmacol. Toxicol. 2007, 101, 47–55. [Google Scholar] [CrossRef]
- Benelli, J.L.; Poester, V.R.; Munhoz, L.S.; Melo, A.M.; Trápaga, M.R.; Stevens, D.A.; Xavier, M.O. Ebselen and Diphenyl Diselenide against Fungal Pathogens: A Systematic Review. Med. Mycol. 2021, 59, 409–421. [Google Scholar] [CrossRef]
- Larwood, D.J. Nikkomycin Z—Ready to Meet the Promise? J. Fungi 2020, 6, 261. [Google Scholar] [CrossRef]
- Clemons, K.V.; Stevens, D.A. Efficacy of Nikkomycin Z against Experimental Pulmonary Blastomycosis. Antimicrob. Agents Chemother. 1997, 41, 2026–2028. [Google Scholar] [CrossRef]
- Nix, D.E.; Swezey, R.R.; Hector, R.; Galgiani, J.N. Pharmacokinetics of Nikkomycin Z after Single Rising Oral Doses. Antimicrob. Agents Chemother. 2009, 53, 2517–2521. [Google Scholar] [CrossRef] [PubMed]
- Barros, M.B.L.; Schubach, T.M.P.; Coll, J.O.; Gremião, I.D.; Wanke, B.; Schubach, A.O. Esporotricose: A Evolução e Os Desafios de Uma Epidemia. Rev. Panam. De Salud Pública 2010, 27, 455–460. [Google Scholar] [CrossRef]
- Minas Gerais, M.G. Resolução SES/MG No 6.532 de 05 de Dezembro de 2018; Governo do Estado de Minas Gerais: Minas Gerais, Brazil, 2018.
- Salvador, B. Portaria No 191/2018; Secretaria Municipal da Saúde: Salvador, Brazil, 2018.
- São Paulo, S. Portaria Secretária Municipal de Saúde—SMS No 470; Prefeitura Municipal De São Paulo: São Paulo, Brazil, 2020.
- Distrito Federal, D.F. Portaria No 664, de 08 de Julho de 2021; Governo do Distrito Federal: Distrito Federal, Brazil, 2021.
- Governo do Estado do Paraná. Resolução SESA No 093/2022; Governo do Estado do Paraná: Paraná, Brazil, 2022.
- Almeida, P.; Giordano, C. Vigilância e Cenário Epidemiológico: Esporotricose No Estado Do RJ. Boletim Epidemiológico Esporotricose 2018, 001/2018, 1–6. [Google Scholar]
- Poester, V.R.; Stevens, D.A.; Basso, R.P.; Munhoz, L.S.; Zanchi, M.; Benelli, J.L.; Klafke, G.B.; Cardone, S.; Xavier, M.O. CATastrophe: Response to the Challenges of Zoonotic Sporotrichosis in Southern Brazil. Mycoses 2022, 65, 30–34. [Google Scholar] [CrossRef]
- Moreira, S.M.; Andrade, E.H.P.; Paiva, M.T.; Zibaoui, H.M.; Salvato, L.A.; Azevedo, M.I.; Oliveira, C.S.F.; Soares, D.F.M.; Keller, K.M.; Magalhães, S.L.; et al. Implementation of an Animal Sporotrichosis Surveillance and Control Program, Southeastern Brazil. Emerg. Infect. Dis. 2021, 27, 949–952. [Google Scholar] [CrossRef]
- Poester, V.R.; Brandolt, T.M.; Klafke, G.B.; Xavier, M.O. Population Knowledge on Sporotrichosis in an Endemic Area in Southern Brazil. Rev. Bras. De Pesqui. Em Saúde 2018, 20, 25–30. [Google Scholar] [CrossRef]
- Poester, V.R.; Saraiva, L.A.; Pretto, A.C.; Klafke, G.B.; Sanchotene, K.O.; Melo, A.M.; Cardone, S.; Xavier, M.O. Desconhecimento de Profissionais e Ações de Extensão Quanto à Esporotricose No Extremo Sul Do Brasil. VITTALLE—Rev. De Ciências Da Saúde 2019, 31, 8–14. [Google Scholar] [CrossRef]
- Brizeno, M.C.; da Silva, E.C.; Bassoli, A.C.D.G. The Public Health Problem of Feline Sporotrichosis in the State of Pernambuco, Brazil: A Narrative Review. Braz. J. Dev. 2020, 6, 93845–93855. [Google Scholar] [CrossRef]




| Drug | Range of Concentrations | N * | Range MIC | Reference |
|---|---|---|---|---|
| 22-hydrazone-imidazolin-2-yl-chol-5-ene-3β-ol | 0.06–4 µg/mL | 16 | 0.03–0.5 µg/mL | [66] |
| Tacrolimus | 0.008–16 µg/mL | 1 | 1 µg/mL | [51] |
| Cyclosporine A | 0.125–16 µg/mL | 1 | 1 µg/mL | |
| Diphenyl Diselenide | 0.25 to 128 µg/mL | 40 | 4–32 µg/mL | [48] |
| Pentamidine | 0.03–16 µg/mL | 10 | 0.13–1 µg/mL | [58] |
| Miltefosine | 0.0312–16 µg/mL | 48 | 0.5–2 µg/mL | [59] |
| 0.25–16 µg/mL | 13 | 1–2 µg/mL | [62] | |
| 0.0313–16 µg/mL | 10 | 1–4 µg/mL | [60] | |
| 0.03−16 µg/mL | 3 | 0.5–4 µg/mL | [78] | |
| Pyrazinoic acid | 0.006–3.18 mg/mL | 1 | 1.59 mg/mL | [67] |
| Pyrazinoic acid derivatives | 0.005–5.1 mg/mL | 5 | 0.05–3.06 mg/mL | |
| Dihydrofuranaphthoquinone derivatives (n = 9) | 0.06–32 μM | 1 | 4–32 μM | [69] |
| Nikkomycin Z | 6.25–400 µg/mL | 3 | 100–400 µg/mL | [53] |
| Acylhydrazone derivatives (n = 3) | 0.06–4 µg/mL | 1 | 0.25–2 µg/mL | [71] |
| Buparvaquone | 0.005–2.61 µg/mL | 20 | 0.005–0.16 µg/mL | [61] |
| Ibuprofen | 2–1.024 µg/mL | 7 | 128–512 µg/mL | [49] |
| 0.06–8 mg/mL | 6 | 0.12–8 mg/mL | [75] | |
| Naphthoquinone derivative (n = 5) | 0.06–32 μM | 1 | 2–32 μM | [63] |
| Acetylsalicylic acid | 0.06–8 mg/mL | 6 | 0.25–8 mg/mL | [75] |
| Diclofenac sodium | 0.06–8 mg/mL | 2 | <0.06–2 mg/mL | |
| Complexes coordinated with cobalt (n = 3) | 4–256 µg/mL | 27 | 32–128 µg/mL | [76] |
| Hydrazone derivatives (n = 3) | Data not shown | 7 | 2.7–13.3 µg/mL | [77] |
| Quinone derivatives (n = 11) | 32–128 µg/mL | |||
| Olorofilm | 0.0002–1 μM | 1 | 0.06 μM | [64] |
| Chitosan | 2–512 µg/mL | 10 | 16–128 µg/mL | [74] |
| Pentathiepin derivatives (n = 3) | Data not shown | 8 | 0.5–8 µg/mL | [68] |
| Zinc ITZ complexes | 0.04–204 μM | 1 | 0.08–0.3 μM | [72] |
| Metal complexes with KTZ and CTZ | 0.008–4 μM | 1 | 0.25 μM | [73] |
| Diaminoquinazoline derivative | 0.0002–1 μM | 5 | 0.25–1 μM | [65] |
| Iodoquinol | 5 | 0.5 μM | ||
| Azole derivative | 5 | 0.25–1 μM | ||
| Silver nanoparticles Silver nanoparticles with chitosan | 0.12–16 μg/mL | 1 | 0.12 µg/mL | [70] |
| 0.5 µg/mL |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Xavier, M.O.; Poester, V.R.; Trápaga, M.R.; Stevens, D.A. Sporothrix brasiliensis: Epidemiology, Therapy, and Recent Developments. J. Fungi 2023, 9, 921. https://doi.org/10.3390/jof9090921
Xavier MO, Poester VR, Trápaga MR, Stevens DA. Sporothrix brasiliensis: Epidemiology, Therapy, and Recent Developments. Journal of Fungi. 2023; 9(9):921. https://doi.org/10.3390/jof9090921
Chicago/Turabian StyleXavier, Melissa Orzechowski, Vanice Rodrigues Poester, Mariana Rodrigues Trápaga, and David A. Stevens. 2023. "Sporothrix brasiliensis: Epidemiology, Therapy, and Recent Developments" Journal of Fungi 9, no. 9: 921. https://doi.org/10.3390/jof9090921






