Abstract
Since the adhesion of resin composites to calcium silicate-based cement is considered challenging. Therefore, the best adhesion strategy should be indicated. This review aimed to assess the effect of different adhesive systems on the bond strength of resin composite to calcium silicate-based cement through a systematic review and meta-analysis. The subsequent PICOS framework used was: population, calcium silicate-based cement; intervention, use of self-etch adhesive systems; control, use of total-etch adhesive systems; outcome, bond strength; study design, in vitro studies. The literature search was conducted independently by two reviewers up to 18 February 2021. Electronic databases (PubMed, ISI Web of Science, SciELO, Scopus, and Embase) were searched for applicable articles. In vitro manuscripts studying the effect of adhesive systems on the bond strength of calcium silicate-based cement were considered. The meta-analyses were performed using Review Manager Software version 5.3.5 (The Nordic Cochrane Centre, The Cochrane Collaboration, Copenhagen, Denmark). Bond strength comparisons were made considering the type of calcium silicate-based cement (Mineral Trioxide Aggregate (MTA), Biodentine™, or TheraCal LC®). A p-value < 0.05 was considered statistically significant. A total of 7321 studies were retrieved in databases searched. After full-text evaluation, 37 eligible papers were assessed for qualitative analysis, leaving a total of 22 papers for the quantitative analysis. According to the meta-analysis, the bond strength values of resin composite materials to MTA and TheraCal LC® cement were favored when a total-etch adhesive system was used (p ≤ 0.02). On the other hand, the meta-analysis of the bond strength of resin-based materials to Biodentine™ calcium silicate-based cement was similar between both approaches (p = 0.12). The in vitro evidence suggests that the bond strength of resin-based materials to both MTA and TheraCal LC® cement was preferred by using the total-etch adhesive strategy. However, when bonding to Biodentine™, the use of self-etch or total-etch strategies displayed promising results. Given the lack of evidence related to the chemical interaction of self-etch adhesive materials with the bioceramics, if self-etch adhesives are used for bonding resin-based restorations to calcium silicate-based cement, a pretreatment with phosphoric acid could be recommended.
1. Introduction
Dental caries, restorative procedures, and tooth fractures may lead to pulp exposure and can endanger treatment prognosis [1]. When pulp exposure occurs, with the aim of maintaining pulp vitality, a biomaterial could be directly placed over the exposed pulp site (a clinical procedure called direct pulp capping) [2]. Other vital therapy procedures include indirect pulp capping (bioactive materials used as liners) and pulpotomy procedures (biomaterial applied following partial amputation of the dental pulp) [3].
A variety of pulp capping agents with specific properties, advantages, and drawbacks are available nowadays [4]. Novel biomaterials, specifically called calcium silicate-based materials, were introduced into the dental market under sealer and cement forms [5,6,7,8]. Calcium silicate-based cement (named bioceramics) is used as an alternative to the historically used calcium hydroxide. Nowadays there is a wide variety of calcium silicate-based cement in dentistry, and due to their biocompatibility, bioactivity, and biomineralization properties, they have been applied in different clinical procedures including direct and indirect pulp capping, regenerative endodontic treatments, pulpotomy and repairing of perforations [5,6].
However, after the use of a bioceramics material, it is necessary to cover it with a restoration material in order to provide an adequate seal to prevent bacterial penetration and to help it remain in place under dislodging forces [9]. Resin composites are often used as restorative materials, and the quality of the bioceramic–composite bond has a significant impact on the success of the resin composite restoration, and in this sense, the bond strength between the resin composite and calcium silicate-based cement materials is an essential clinical factor for the success of these types of treatments [10,11].
Nowadays, two different adhesion strategies can be used within a clinical scenario [10]. In the total-etch strategy, adhesives are applied after phosphoric acid etching of both enamel and dentin [11]. On the other hand, the self-etch strategy implies the use of self-etch adhesives containing acidic monomers that both etch and prime the dental substrate, and therefore, the application of the phosphoric acid is eliminated in the self-etching technique [12]. Some adhesives can be used in both total-etch or self-etch strategies, constituting what is known as universal adhesives [13].
To date, different studies have been achieved to evaluate the bond strength of resin composites to calcium silicate-based cement using different adhesive systems and strategies [14,15,16]. Considering that the quality of the bond between the calcium silicate-based cement and the composite restoration has been proved to play an important role in the success of the restoration, it is mandatory to establish which adhesive strategy provides the best bond between these materials. Therefore, this systematic review and meta-analysis aimed to assess the effect of different adhesive systems on the bond strength of resin composites to calcium silicate-based cement. The null hypothesis to be tested was that there would be no differences in bond strength to calcium silicate-based cement when using total-etch or self-etch adhesive systems.
2. Results and Discussion
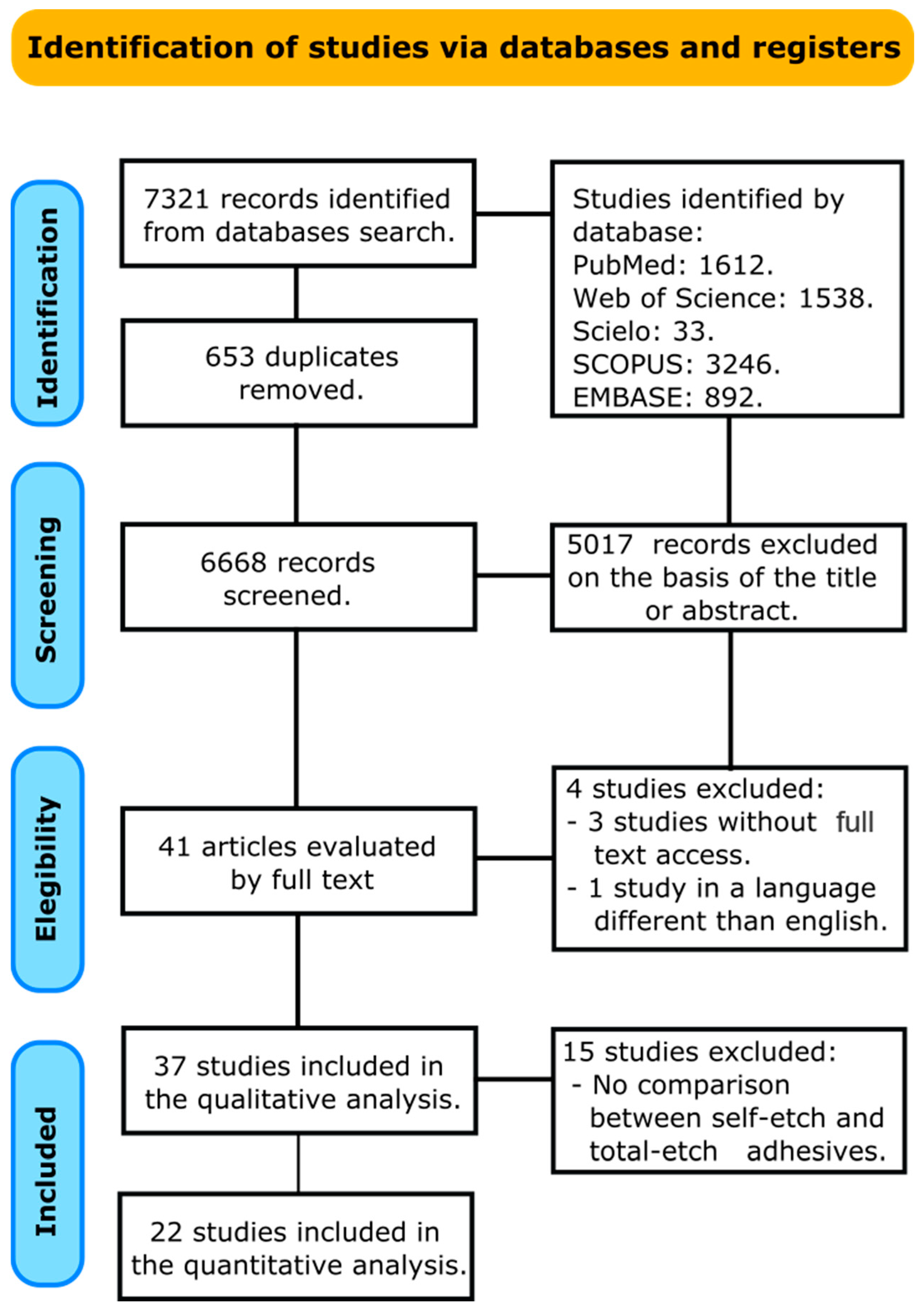
A total of 7321 papers were recognized in all databases searched. A flowchart that forms the report selection procedure agreeing to the PRISMA Statement is displayed in Figure 1. The literature review rescued 6668 articles for the initial inspection after removing the duplicates. Afterward, 5017 studies were excluded after reviewing the titles and abstracts, leaving 41 articles to be assessed by full-text interpretation. After the full-text assessment, four studies were excluded, three because the access to the full document was not achieved [17,18,19], and one because the manuscript was in a language different than English [20]. A total of thirty-seven manuscripts were included in the qualitative analysis, and from these, fifteen were excluded from the meta-analysis because they did not compare a self-etch adhesive against a total-etch adhesive [10,21,22,23,24,25,26,27,28,29,30,31,32,33,34]. Finally, twenty-two manuscripts were included in the meta-analysis [11,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55].
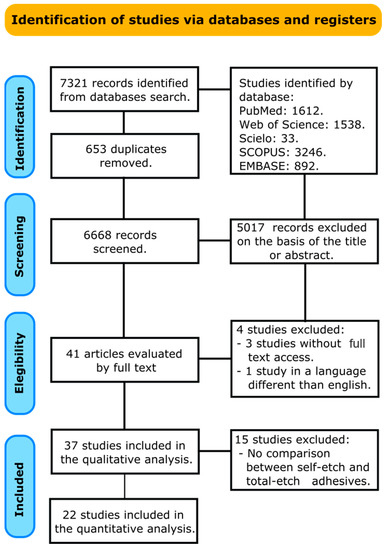
Figure 1.
Search flowchart according to the PRISMA Statement.
This review identified three main calcium silicate-based types of cement, including MTA, Biodentine™, and TheraCal LC®. The conditions for the setting of the material varied among the studies including using 37 °C with 100% of relative humidity for different periods of time. Restorative materials included composite resins placed using the total-etch or self-etch adhesive technique. Other articles evaluated self-adhesive resin composites and glass ionomer cement. The bond strength test used in the totality of the articles included was the shear bond strength (SBS) test and storing conditions of the samples were in distilled water or saliva for a period of time who ranged from 24 h until 28 days. None of the articles included in this review compared the immediate versus the long-term bond strength (Table 1).

Table 1.
Demographic data.
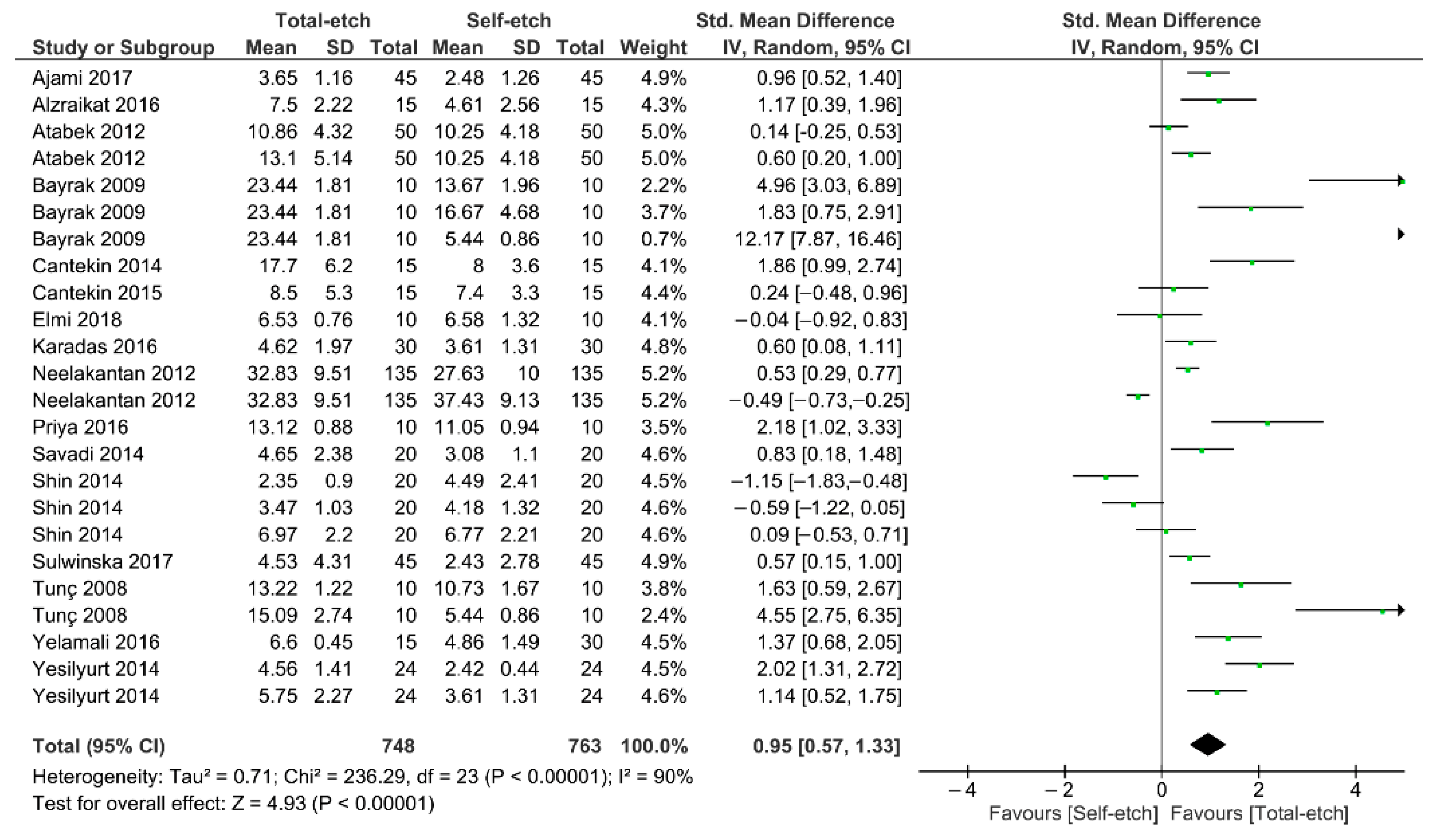
Figure 2 shows the meta-analysis of the bond strength values of resin composite materials to MTA cement. According to the analysis, the bond strength was enhanced when a total-etch adhesive system was used (p < 0.01). A high heterogenicity (90%) was observed.
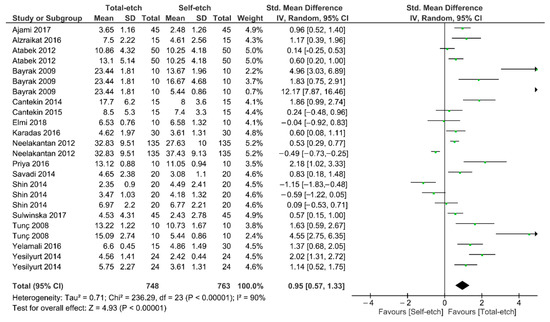
Figure 2.
Findings of the meta-analysis of the bond strength of resin-based materials to MTA calcium silicate-based cement. Bond strength was higher when a total-etch adhesive was used (p < 0.01).
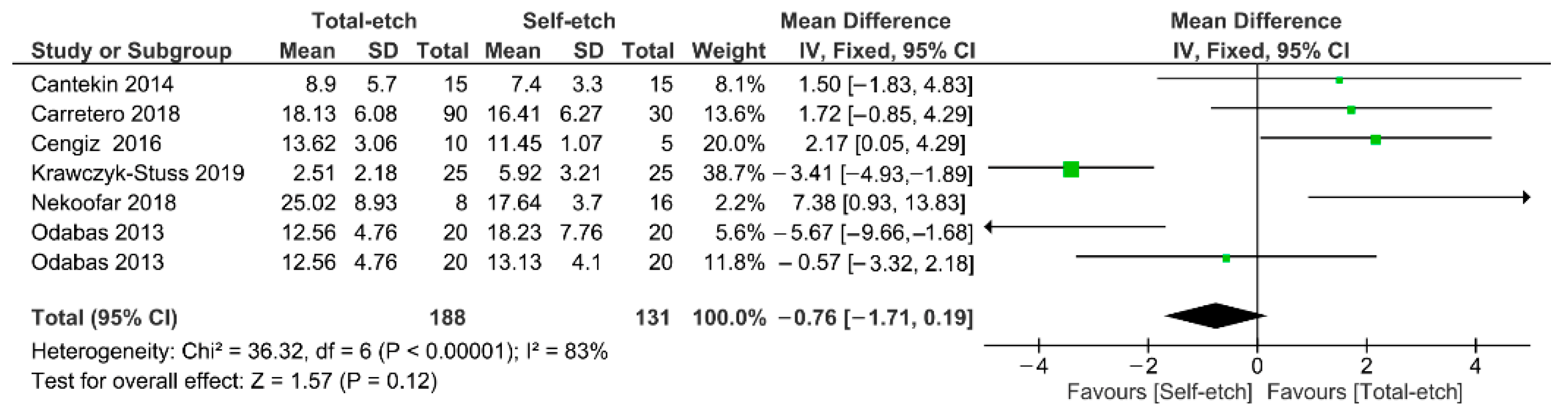
Figure 3 shows the meta-analysis of the bond strength values of resin composite materials to Biodentine™ cement. According to the analysis, the bond strength was similar between the total-etch and self-etch adhesives (p = 0.12). A high heterogenicity (83%) among the studies was observed.
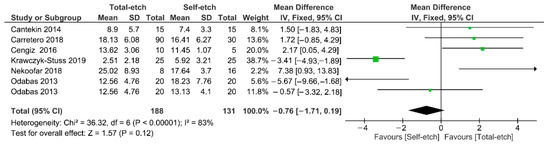
Figure 3.
Findings of the meta-analysis of the bond strength of resin-based materials to Biodentine™ calcium silicate-based cement. Bond strength was similar between both strategies (p = 0.12).
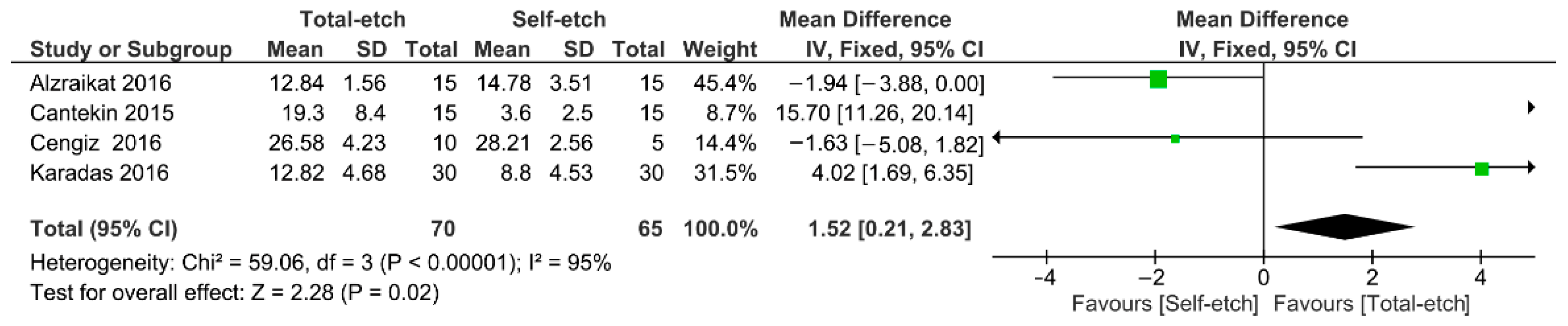
Figure 4 shows the meta-analysis of the bond strength values of resin composite materials to TheraCal LC® cement. According to the analysis, the bond strength was higher for the total-etch technique (p = 0.02). A high heterogenicity (95%) among the studies was observed.
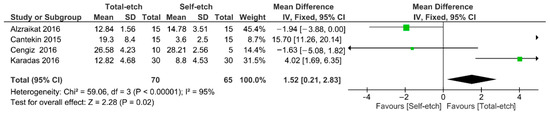
Figure 4.
Findings of the meta-analysis of the bond strength of resin-based materials to TheraCal LC® calcium silicate-based cement. Bond strength was higher for the total-etch technique (p = 0.02).
The risk of bias in the articles studied in this review is recapped in Table 2. Most of the articles included failed to meet the parameters of Single Operator, Blinded Operator, Sample Size Calculation, and Control group. The global analysis showed that the utmost of the articles included were cataloged as high and medium risk of bias.

Table 2.
Risk of bias assessment. (Red Code = High risk; Black code = Medium risk).
This systematic review and meta-analysis were directed to assess the effect of different adhesive strategies on the bond strength of resin composites to calcium silicate-based cement. The overall findings revealed that the bond strength of resin composites to MTA and TheraCal LC® cement was favored when a total-etch adhesive was used. However, for Biodentine™ cement the bond strength was similar between both total-etch and self-etch adhesives. Considering this, the null hypothesis tested in this study was partially accepted.
One should bear in mind that MTA are root canal sealers or cement that have been composed of silicate and calcium. Due to favorable outcomes obtained by MTA in addition to its excellent sealing ability, clinical applications, and biocompatibility in endodontic treatment such as root-end filling, pulp capping, apical plug for teeth with open apices, and perforation repair, investigators have been fortified to test materials with comparable promising assets though being less pricey as well as less of the present shortcomings of the unique MTA [56,57]. Higher radiopacity, handling characteristics, prevention of tooth discoloration, and lower setting time of MTA can be modified by new materials with the same composition [58,59,60]. Consequently, calcium silicate-based cement was presented. One calcium silicate-based cement, Biodentine™ (Septodont, Saint-Maur-des-Fossés, France), necessitated quicker setting times, exhibited less discoloration, and presented more satisfactory clinical outcomes than MTA [61,62]. Lately, TheraCal LC®, a novel light-cured MTA-filled was introduced in an attempt to enhance mechanical strength, handling properties, and application to tooth substrate. Furthermore, it can be cured immediately using a light curing unit and flow over a surface before it is cured [63]. Nevertheless, in human dental pulp stem cells, TheraCal LC® was stated to be more cytotoxic than Biodentine™ and MTA [64].
In restorative dentistry, resinous materials have increased popularity due to their promising esthetic outcome [55]. Proper bonding between calcium silicate-based cement and resinous materials was considered essential for the ultimate success of dental restorations and the quality of fillings [11]. It should be noted that for evaluating the adhesive properties of restorative materials, the most commonly used test is the bond strength [11]. However, choosing between total-etch or self-etch adhesive systems was considered challenging in such a situation [65].
Agreeing to the meta-analysis, the bond strength values of resin composite materials to MTA and TheraCal LC® cement were favored when a total-etch adhesive system was used (p < 0.05). It should be emphasized that a bond strength ranging between 17 to 20 MPa might be needed to challenge contraction forces adequately to generate restoration margins without gap [66]. In this review, SBS was lower using self-etch adhesives and this could be attributed to several factors. Knowing that a chief solvent/oxygen inhibition results through light activation of these materials, a lower degree of conversion of the resin monomer could be observed. In addition, combining hydrophilic and hydrophobic acidic monomers into one bottle might jeopardize the polymerization of the adhesive [67]. Further, the integrally low strength of the adhesive polymer could be responsible for the suboptimal performance of self-etch adhesives [39]. The pH of the self-etch adhesive systems could also play a role, and one of the explanations for the lower bond strength for self-etch adhesives might be the incompatibility between the adhesive and the restorative material [68]. In addition, it should be highlighted that different solvents lead to differences in the bond strength values; however, this variable was not studied in this review. This deduction appears to support the results in this analysis.
The finding showed that the acid-etch technique was deemed crucial for the enhanced bond between MTA and TheraCal LC® cement with resin composites. Acid-etch enhances the wettability of MTA and thus the bond strength with composite resin. Additionally, as a result of an acidic environment, the surface’s porosity increases, causing micro-retention zones during adhesion. It has been demonstrated that after the application of phosphoric acid, the MTA surface is altered, creating gel-like irregular structures and a spindle-shaped surface, which provides a desirable surface for resin materials to bond [46]. Actually, previous research confirmed that the structural and chemical changes within the surface of calcium-based silicate cement occur after 20 s of etching with 37% orthophosphoric acid [68]. Additionally, the high bond strength for TheraCal LC® when using acid-etch could be credited to the presence of dimethacrylate monomer that indorses chemical adhesion between the TheraCal LC® and total-etch adhesive [45]. It can be concluded that a total-etch adhesive would be the substance of choice to reach improved bond strength values when bonding composite resin to MTA and TheraCal LC® cements.
The present analysis revealed that the bond strength values of resin composite materials to Biodentine™ cement were similar between both total-etch and self-etch adhesives (p = 0.12). This could be in agreement with a previous study evaluating three adhesive systems and highlighting the variation in the composition of both adhesive systems and resin composites on the outcome of the bond strength to Biodentine™ [49]. One should state that the bond strength between restorative materials and Biodentine™ at several application periods is significant for the longevity of the restorations and their quality [9,41]. Numerous factors could affect this statement such as the low viscosity of adhesive systems which may increase the penetration of adhesive systems into the Biodentine™ cement [69]. Further, the addition of 10-methacryloyloxydecyl dihydrogen phosphate (MDP) into the composition of the adhesive system may facilitate the chemical interaction with the calcium-rich Biodentine™ surface [70,71]. Suitable resin–dentin bonding is usually instantaneously reached, and lessened bonding efficiency arises over time [65]. Low bond strength of aged Biodentine™ could be observed and might be elucidated by the fact that the surface hardness of Biodentine™ increases with time, thus resulting in reduced micro-mechanical retention and shallower etching pattern [48,72]. In summary, the use of both adhesion strategies seem to considerably increase the SBS of resin composites to Biodentine™.
From this review, the effect of different adhesive systems was analyzed to evaluate their bond strength to calcium silicate-based cement, including MTA, Biodentine™, and TheraCal LC®. Considering the results, it seems that the interaction between calcium silicate-based cement and resin-based materials, (i.e., adhesive systems) is more physical, given by the porosities that phosphoric acid creates within the surface of the material [36]. The outcomes of this study should be considered with caution since other calcium silicate-based cement were available in the dental market and not included. Further, the principal restraint of the present review was a lack of assessment of the features and surface morphology of these cement at distinctive setting times and moisture [73], which might have facilitated these findings. In addition, it is recommended that in future reports scanning electron microscopy (SEM) and atomic force microscopy (AFM) evaluation must be carried out in an attempt to supplementary elucidate the explanations for increases and/or decreases in SBS of these cements using different strategies. Further, most of the articles included were categorized as having high or medium risk of bias, and, consequently, superior investigational designs must be directed in order to obtain a higher degree of evidence. Moreover, clinical studies were needed since providing the best bond between calcium silicate materials and resin composites was scarce.
3. Conclusions
The findings of the review suggest that the bond strength of resin-based materials to both MTA and TheraCal LC® cement could be enhanced by the use of the total-etch technique. On the other hand, when bonding to Biodentine™ the use of self-etch or total-etch strategies displayed promising results. Given the lack of evidence related to the chemical interaction of self-etch adhesive materials with the bioceramics, if self-etch adhesives are used for bonding resin-based restorations to calcium silicate-based cement, a pretreatment with phosphoric acid could be recommended.
4. Materials and Methods
The present study was conducted adhering to the guidance of PRISMA [73]. The following PICOS framework was used: population, calcium silicate-based cement; intervention, use of self-etch adhesive systems; control, use of total-etch adhesive systems; outcome, bond strength; study design, in vitro studies. The research interrogation was: what is the adhesive strategy that provides the highest bond strength between calcium silicate-based cement and resin-based materials?
4.1. Literature Search
The systematic search was conducted independently by two authors (AAO and CECS) up to 18 February 2021, without date restriction, among five electronic databases (PubMed, ISI Web of Science, SciELO, Scopus, and Embase). The keywords and search strategy used in PubMed and adapted to the other data search engines are listed in Table 3. The reviewers also performed a manual search of reference lists of the included articles for supplementary literature. All articles located in the databases were imported into the Mendeley Desktop 1.17.11 software to remove duplicates.

Table 3.
Keywords used in search strategy.
4.2. Study Selection
Titles and abstracts were initially screened by two reviewers (LH and RB) in order to identify studies that potentially met the following eligibility criteria: (1) in vitro studies reporting the bond strength of total-etch and self-etch adhesive systems to calcium silicate-based cement; (2) studies including mean and standard deviation (SD) data in MPa on shear, microshear, tensile, and micro-tensile bond tests; (4) studies published in English. Case reports, case series, pilot studies, and reviews were excluded from the initial review. Full copies of all of the possibly applicable articles were inspected. If after reading the title and abstract, it was not possible to make a clear judgment, the article was designated for full analysis. The full-text manuscripts were evaluated individually in duplicate by two investigators. Any inconsistency or variation concerning the suitability of the comprised manuscripts was determined through consultation with a third reviewer, a senior experienced researcher (CECS). Only manuscripts that encountered the appropriateness criteria were integrated for review.
4.3. Data Extraction
Data of interest from the comprised articles were inserted into standardized worksheets using Microsoft Office Excel 2021 software (Microsoft Corporation, Redmond, WA, USA). These data included the year of publication, author, bioceramic used as substrate, setting conditions (time and temperature), adhesive system used, outcomes evaluated (mean, SD, n), and storing conditions. If any information was missing the corresponding author of the article was contacted to supply the exact data. If a response was not obtained within 2 weeks of the first contact, the missing information was not comprised.
4.4. Quality Assessment
The methodological quality of the included studies was evaluated by two reviewers (AAO and LH) considering the parameters of previous systematic reviews [74,75]. The risk of bias in each article was assessed according to the description of the following parameters: sample randomization; single-operator protocol implementation; blinding of the operator; the presence of a control group; standardization of the sample preparation; use of all materials according to the manufacturer’s instructions; and description of the sample size calculation. If the parameter was described within the study, the study received a “YES”. In the case of omitted data, the factor received a “NO”. The risk of bias was classified according to the sum of “YES” answers received: 1 or 2 indicated a high bias, 3 to 5 medium, and 6 or 7 indicated a low risk of bias.
4.5. Statistical Analysis
The meta-analyses were accomplished using a software program (Review Manager version 5.3.5; The Cochrane Collaboration, Copenhagen, Denmark). A random-effect model was used to carry out the different analyses by comparing the standardized mean difference of the bond strength values using the total-etch or self-etch adhesive systems. Bond strength comparisons were completed bearing in mind the calcium silicate-based cement (Mineral Trioxide Aggregate, Biodentine™, or TheraCal LC®). A p-value < 0.05 was contemplated statistically significant. The heterogeneity was calculated using the Cochran Q test and the inconsistency I2 test.
Author Contributions
Conceptualization, L.H., R.B. and C.E.C.-S.; methodology, L.H., R.B. and C.E.C.-S.; software, N.K., L.H., R.B., D.M. and M.L.-S.; validation, L.H., R.B., N.K., C.E.C.-S., M.L.-S.; A.E. and Y.H.; formal analysis, L.H., R.B., N.K. and C.E.C.-S.; investigation, A.A.-O., Y.H., N.K., L.H., R.B. and C.E.C.-S.; resources, L.E.R.-V., A.F.-L., D.M., N.K., R.B., L.H., Y.H. and M.L.-S.; data curation, L.H., R.B. and C.E.C.-S.; writing—original draft preparation, L.H., R.B., C.E.C.-S., N.K., A.A.-O. and L.E.R.-V.; writing—review and editing, M.-L.D., M.M., D.M., L.H., A.A.-O., C.E.C.-S., R.B., Y.H. and M.L.-S.; visualization, Y.H., N.K. and R.B.; supervision, L.H.; project administration, L.H. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Acknowledgments
Authors Louis Hardan and Rim Bourgi would like to recognize the Saint-Joseph University of Beirut, Lebanon. Moreover, the referees would also recognize the Medical University of Lodz, the University of Hidalgo State, Mexico, and the University of Strasbourg for accompanying this research.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Bjørndal, L.; Simon, S.; Tomson, P.; Duncan, H. Management of Deep Caries and the Exposed Pulp. Int. Endod. J. 2019, 52, 949–973. [Google Scholar] [CrossRef] [PubMed]
- Emara, R.; Krois, J.; Schwendicke, F. Maintaining Pulpal Vitality: Cost-Effectiveness Analysis on Carious Tissue Removal and Direct Pulp Capping. J. Dent. 2020, 96, 103330. [Google Scholar] [CrossRef] [PubMed]
- Kunert, M.; Lukomska-Szymanska, M. Bio-Inductive Materials in Direct and Indirect Pulp Capping—A Review Article. Materials 2020, 13, 1204. [Google Scholar] [CrossRef]
- Davaie, S.; Hooshmand, T.; Ansarifard, S. Different Types of Bioceramics as Dental Pulp Capping Materials: A Systematic Review. Ceram. Int. 2021, 47, 20781–20792. [Google Scholar] [CrossRef]
- Dawood, A.E.; Parashos, P.; Wong, R.H.; Reynolds, E.C.; Manton, D.J. Calcium Silicate-Based Cements: Composition, Properties, and Clinical Applications. J. Investig. Clin. Dent. 2017, 8, e12195. [Google Scholar] [CrossRef]
- Eid, A.; Mancino, D.; Rekab, M.S.; Haikel, Y.; Kharouf, N. Effectiveness of Three Agents in Pulpotomy Treatment of Permanent Molars with Incomplete Root Development: A Randomized Controlled Trial. Healthcare 2022, 10, 431. [Google Scholar] [CrossRef]
- Hashem, D.F.; Foxton, R.; Manoharan, A.; Watson, T.F.; Banerjee, A. The Physical Characteristics of Resin Composite–Calcium Silicate Interface as Part of a Layered/Laminate Adhesive Restoration. Dent. Mater. 2014, 30, 343–349. [Google Scholar] [CrossRef]
- Altunsoy, M.; Tanrıver, M.; Ok, E.; Kucukyilmaz, E. Shear Bond Strength of a Self-Adhering Flowable Composite and a Flowable Base Composite to Mineral Trioxide Aggregate, Calcium-Enriched Mixture Cement, and Biodentine. J. Endod. 2015, 41, 1691–1695. [Google Scholar] [CrossRef]
- Tunç, E.Ş.; Sönmez, I.; Bayrak, Ş.; Eğilmez, T. The Evaluation of Bond Strength of a Composite and a Compomer to White Mineral Trioxide Aggregate with Two Different Bonding Systems. J. Endod. 2008, 34, 603–605. [Google Scholar] [CrossRef]
- Van Meerbeek, B.; Yoshihara, K.; Yoshida, Y.; Mine, A.; De Munck, J.; Van Landuyt, K. State of the Art of Self-Etch Adhesives. Dent. Mater. 2011, 27, 17–28. [Google Scholar] [CrossRef]
- Pashley, D.H.; Tay, F.R.; Breschi, L.; Tjäderhane, L.; Carvalho, R.M.; Carrilho, M.; Tezvergil-Mutluay, A. State of the Art Etch-and-Rinse Adhesives. Dent. Mater. 2011, 27, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Moszner, N.; Hirt, T. New Polymer-chemical Developments in Clinical Dental Polymer Materials: Enamel–Dentin Adhesives and Restorative Composites. J. Polym. Sci. Part A Polym. Chem. 2012, 50, 4369–4402. [Google Scholar] [CrossRef]
- Cuevas-Suarez, C.E.; de Oliveira da Rosa, W.L.; Lund, R.G.; da Silva, A.F.; Piva, E. Bonding Performance of Universal Adhesives: An Updated Systematic Review and Meta-Analysis. J. Adhes. Dent. 2019, 21. [Google Scholar]
- Shin, H.; Kim, M.; Nam, O.; Lee, H.; Choi, S.; Kim, K. Shear Bond Strength Comparison of Different Adhesive Systems to Calcium Silicate-Based Materials. J. Korean Acad. Pediatr. Dent. 2018, 45, 445–454. [Google Scholar] [CrossRef]
- Pradelle-Plasse, N.; Mocquot, C.; Semennikova, K.; Colon, P.; Grosgogeat, B. Interface between Calcium Silicate Cement and Adhesive Systems According to Adhesive Families and Cement Maturation. Restor. Dent. Endod. 2021, 46. [Google Scholar] [CrossRef]
- Nagas, E.; Cehreli, Z.; Uyanik, M.O.; Durmaz, V. Bond Strength of a Calcium Silicate-Based Sealer Tested in Bulk or with Different Main Core Materials. Braz. Oral Res. 2014, 28, 1–7. [Google Scholar] [CrossRef]
- Alhowaish, L.; Salama, F.; Al-Harbi, M.; Abumoatti, M. Shear Bond Strength of a Resin Composite to Six Pulp Capping Materials Used in Primary Teeth. J. Clin. Pediatr. Dent. 2020, 44, 234–239. [Google Scholar] [CrossRef]
- Ali, A.; Banerjee, A.; Mannocci, F. Effect of Adhesive Materials on Shear Bond Strength of a Mineral Trioxide Aggregate. Am. J. Dent. 2016, 29, 46–50. [Google Scholar]
- Rao, A.; Shenoy, R.; BS, S. Comparative Evaluation of Tensile Bond Strength and Shear Bond Strength of Mineral Trioxide Aggregate with Composite Resin and Resin Modified Glass Ionomer. Indian J. Public Health Res. Dev. 2019, 10, 156. [Google Scholar]
- Krawczyk-Stuss, M.; Ostrowska, A.; Łapińska, B.; Nowak, J.; Bołtacz-Rzepkowska, E. Evaluation of Shear Bond Strength of the Composite to Biodentine with Different Adhesive Systems. Dent. Med. Probl. 2015, 52, 434–439. [Google Scholar] [CrossRef]
- Çolak, H.; Tokay, U.; Uzgur, R.; Uzgur, Z.; Ercan, E.; Hamidi, M.M. The Effect of Different Adhesives and Setting Times on Bond Strength between Biodentine and Composite. J. Appl. Biomater. Funct. Mater. 2016, 14, 217–222. [Google Scholar] [CrossRef] [PubMed]
- Doozaneh, M.; Koohpeima, F.; Firouzmandi, M.; Abbassiyan, F. Shear Bond Strength of Self-Adhering Flowable Composite and Resin-Modified Glass Ionomer to Two Pulp Capping Materials. Iran. Endod. J. 2017, 12, 103. [Google Scholar] [PubMed]
- Ha, H.-T. The Effect of the Maturation Time of Calcium Silicate-Based Cement (BiodentineTM) on Resin Bonding: An In Vitro Study. Appl. Adhes. Sci. 2019, 7, 1–13. [Google Scholar] [CrossRef]
- Hursh, K.A.; Kirkpatrick, T.C.; Cardon, J.W.; Brewster, J.A.; Black, S.W.; Himel, V.T.; Sabey, K.A. Shear Bond Comparison between 4 Bioceramic Materials and Dual-Cure Composite Resin. J. Endod. 2019, 45, 1378–1383. [Google Scholar] [CrossRef] [PubMed]
- Mustafa, R.M.; Al-Nasrawi, S.J.; Aljdaimi, A.I. The Effect of Biodentine Maturation Time on Resin Bond Strength When Aged in Artificial Saliva. Int. J. Dent. 2020, 2020, 8831813. [Google Scholar] [CrossRef]
- Nagi, S.M.; Omar, N.; Salem, H.N.; Aly, Y. Effect of Different Surface Treatment Protocols on the Shear Bond Strength of Perforation Repair Materials to Resin Composite. J. Adhes. Sci. Technol. 2020, 34, 417–426. [Google Scholar] [CrossRef]
- Palma, P.J.; Marques, J.A.; Falacho, R.I.; Vinagre, A.; Santos, J.M.; Ramos, J.C. Does Delayed Restoration Improve Shear Bond Strength of Different Restorative Protocols to Calcium Silicate-Based Cements? Materials 2018, 11, 2216. [Google Scholar] [CrossRef]
- Palma, P.J.; Marques, J.A.; Antunes, M.; Falacho, R.I.; Sequeira, D.; Roseiro, L.; Santos, J.M.; Ramos, J.C. Effect of Restorative Timing on Shear Bond Strength of Composite Resin/Calcium Silicate–Based Cements Adhesive Interfaces. Clin. Oral Investig. 2021, 25, 3131–3139. [Google Scholar] [CrossRef]
- Raina, A.; Sawhny, A.; Paul, S.; Nandamuri, S. Comparative Evaluation of the Bond Strength of Self-Adhering and Bulk-Fill Flowable Composites to MTA Plus, Dycal, Biodentine, and TheraCal: An In Vitro Study. Restor. Dent. Endod. 2020, 45, e10. [Google Scholar] [CrossRef]
- Samimi, P.; Kazemian, M.; Shirban, F.; Alaei, S.; Khoroushi, M. Bond Strength of Composite Resin to White Mineral Trioxide Aggregate: Effect of Different Surface Treatments. J. Conserv. Dent. JCD 2018, 21, 350–353. [Google Scholar]
- Schmidt, A.; Schäfer, E.; Dammaschke, T. Shear Bond Strength of Lining Materials to Calcium-Silicate Cements at Different Time Intervals. J Adhes. Dent. 2017, 19, 129–135. [Google Scholar] [PubMed]
- Tulumbaci, F.; Almaz, M.E.; Arikan, V.; Mutluay, M.S. Shear Bond Strength of Different Restorative Materials to Mineral Trioxide Aggregate and Biodentine. J. Conserv. Dent. JCD 2017, 20, 292–296. [Google Scholar] [CrossRef] [PubMed]
- Murat, Ü. The Comparison of Shear Bond Strenght of Different Bulk-Fill Composites to a Bioactive Dentine Substitute. Cumhur. Dent. J. 2018, 21, 274–283. [Google Scholar]
- Zarean, P.; Roozbeh, R.; Zarean, P.; Jahromi, M.Z.; Broujeni, P.M. In Vitro Comparison of Shear Bond Strength of a Flowable Composite Resin and a Single-Component Glass-Ionomer to Three Different Pulp-Capping Agents. Dent. Med. Probl. 2019, 56, 239–244. [Google Scholar]
- Ajami, A.-A.; Bahari, M.; Hassanpour-Kashani, A.; Abed-Kahnamoui, M.; Savadi-Oskoee, A.; Azadi-Oskoee, F. Shear Bond Strengths of Composite Resin and Giomer to Mineral Trioxide Aggregate at Different Time Intervals. J. Clin. Exp. Dent. 2017, 9, e906–e911. [Google Scholar] [CrossRef][Green Version]
- Ajami, A.A.; Navimipour, E.J.; Oskoee, S.S.; Kahnamoui, M.A.; Lotfi, M.; Daneshpooy, M. Comparison of Shear Bond Strength of Resin-Modified Glass Ionomer and Composite Resin to Three Pulp Capping Agents. J. Dent. Res. Dent. Clin. Dent. Prospect. 2013, 7, 164. [Google Scholar]
- Alzraikat, H.; Taha, N.A.; Qasrawi, D.; Burrow, M.F. Shear Bond Strength of a Novel Light Cured Calcium Silicate Based-Cement to Resin Composite Using Different Adhesive Systems. Dent. Mater. J. 2016, 35, 881–887. [Google Scholar] [CrossRef]
- Atabek, D.; Sillelioğlu, H.; Ölmez, A. Bond Strength of Adhesive Systems to Mineral Trioxide Aggregate with Different Time Intervals. J. Endod. 2012, 38, 1288–1292. [Google Scholar] [CrossRef]
- Bayrak, S.; Tunç, E.S.; Saroglu, I.; Egilmez, T. Shear Bond Strengths of Different Adhesive Systems to White Mineral Trioxide Aggregate. Dent. Mater. J. 2009, 28, 62–67. [Google Scholar] [CrossRef]
- Cantekin, K. Bond Strength of Different Restorative Materials to Light-Curable Mineral Trioxide Aggregate. J. Clin. Pediatr. Dent. 2015, 39, 143–148. [Google Scholar] [CrossRef]
- Cantekin, K.; Avci, S. Evaluation of Shear Bond Strength of Two Resin-Based Composites and Glass Ionomer Cement to Pure Tricalcium Silicate-Based Cement (Biodentine®). J. Appl. Oral Sci. 2014, 22, 302–306. [Google Scholar] [CrossRef] [PubMed]
- Carretero, V.; Giner-Tarrida, L.; Peñate, L.; Arregui, M. Shear Bond Strength of Nanohybrid Composite to Biodentine with Three Different Adhesives. Coatings 2019, 9, 783. [Google Scholar] [CrossRef]
- Cengiz, E.; Ulusoy, N. Microshear Bond Strength of Tri-Calcium Silicate-Based Cements to Different Restorative Materials. J Adhes Dent 2016, 18, 231–237. [Google Scholar] [PubMed]
- Elmi, M.; Ehsani, M.; Esmaeili, B.; Khafri, S. Comparison of Bond Strength of a Composite Resin with Two Different Adhesive Systems and a Resin Modified Glass Ionomer to Calcium Enriched Mixture. J. Conserv. Dent. JCD 2018, 21, 369. [Google Scholar]
- Karadas, M.; Cantekin, K.; Gumus, H.; Ateş, S.M.; Duymuş, Z.Y. Evaluation of the Bond Strength of Different Adhesive Agents to a Resin-modified Calcium Silicate Material (TheraCal LC). Scanning 2016, 38, 403–411. [Google Scholar] [CrossRef]
- Krawczyk-Stuss, M.; Nowak, J.; Bołtacz-Rzepkowska, E. Bond Strength of Biodentine to a Resin-Based Composite at Various Acid Etching Times and with Different Adhesive Strategies. Dent. Med. Probl. 2019, 56, 39–44. [Google Scholar] [CrossRef]
- Neelakantan, P.; Grotra, D.; Subbarao, C.V.; Garcia-Godoy, F. The Shear Bond Strength of Resin-Based Composite to White Mineral Trioxide Aggregate. J. Am. Dent. Assoc. 2012, 143, e40–e45. [Google Scholar] [CrossRef]
- Nekoofar, M.H.; Motevasselian, F.; Mirzaei, M.; Yassini, E.; Pouyanfar, H.; Dummer, P.M. The Micro-Shear Bond Strength of Various Resinous Restorative Materials to Aged Biodentine. Iran. Endod. J. 2018, 13, 356. [Google Scholar]
- Odabaş, M.E.; Bani, M.; Tirali, R.E. Shear Bond Strengths of Different Adhesive Systems to Biodentine. Sci. World J. 2013, 2013, 626103. [Google Scholar] [CrossRef]
- Priya, B.D.; Ganapathi, A.K.; Maroli, S.; Ramesh, K.; Vaaka, P.H. The Evaluation of Shear Bond Strength of Different Restorative Composite Resins and Glass Ionomer Cement to White Mineral Trioxide Aggregate: An in Vitro Study. Adv. Hum. Biol. 2016, 6, 16. [Google Scholar]
- Oskoee, S.S.; Bahari, M.; Kimyai, S.; Motahhari, P.; Eghbal, M.J.; Asgary, S. Shear Bond Strength of Calcium Enriched Mixture Cement and Mineral Trioxide Aggregate to Composite Resin with Two Different Adhesive Systems. J. Dent. Tehran Iran 2014, 11, 665–671. [Google Scholar]
- Shin, J.-H.; Jang, J.-H.; Park, S.H.; Kim, E. Effect of Mineral Trioxide Aggregate Surface Treatments on Morphology and Bond Strength to Composite Resin. J. Endod. 2014, 40, 1210–1216. [Google Scholar] [CrossRef] [PubMed]
- Sulwińska, M.; Szczesio, A.; Bołtacz-Rzepkowska, E. Bond Strength of a Resin Composite to MTA at Various Time Intervals and with Different Adhesive Strategies. Dent. Med. Probl. 2017, 54, 155–160. [Google Scholar] [CrossRef]
- Yelamali, S.; Patil, A.C. “Evaluation of Shear Bond Strength of a Composite Resin to White Mineral Trioxide Aggregate with Three Different Bonding Systems”-An in Vitro Analysis. J. Clin. Exp. Dent. 2016, 8, e273. [Google Scholar]
- Yesilyurt, C.; Yildirim, T.; Taşdemir, T.; Kusgoz, A. Shear Bond Strength of Conventional Glass Ionomer Cements Bound to Mineral Trioxide Aggregate. J. Endod. 2009, 35, 1381–1383. [Google Scholar] [CrossRef]
- Parirokh, M.; Torabinejad, M. Mineral Trioxide Aggregate: A Comprehensive Literature Review—Part I: Chemical, Physical, and Antibacterial Properties. J. Endod. 2010, 36, 16–27. [Google Scholar] [CrossRef]
- Torabinejad, M.; Parirokh, M. Mineral Trioxide Aggregate: A Comprehensive Literature Review—Part II: Leakage and Biocompatibility Investigations. J. Endod. 2010, 36, 190–202. [Google Scholar] [CrossRef]
- Parirokh, M.; Torabinejad, M. 10 Calcium Silicate–Based Cements. In Mineral Trioxide Aggregate: Properties and Clinical Applications; John Wiley & Sons: Hoboken, NJ, USA, 2014; p. 281. [Google Scholar]
- Kharouf, N.; Zghal, J.; Addiego, F.; Gabelout, M.; Jmal, H.; Haïkel, Y.; Bahlouli, N.; Ball, V. Tannic Acid Speeds up the Setting of Mineral Trioxide Aggregate Cements and Improves Its Surface and Bulk Properties. J. Colloid Interface Sci. 2021, 589, 318–326. [Google Scholar] [CrossRef]
- Kharouf, N.; Arntz, Y.; Eid, A.; Zghal, J.; Sauro, S.; Haikel, Y.; Mancino, D. Physicochemical and Antibacterial Properties of Novel, Premixed Calcium Silicate-Based Sealer Compared to Powder–Liquid Bioceramic Sealer. J. Clin. Med. 2020, 9, 3096. [Google Scholar] [CrossRef]
- Parinyaprom, N.; Nirunsittirat, A.; Chuveera, P.; Lampang, S.N.; Srisuwan, T.; Sastraruji, T.; Bua-On, P.; Simprasert, S.; Khoipanich, I.; Sutharaphan, T. Outcomes of Direct Pulp Capping by Using Either ProRoot Mineral Trioxide Aggregate or Biodentine in Permanent Teeth with Carious Pulp Exposure in 6-to 18-Year-Old Patients: A Randomized Controlled Trial. J. Endod. 2018, 44, 341–348. [Google Scholar] [CrossRef]
- Paula, A.; Carrilho, E.; Laranjo, M.; Abrantes, A.M.; Casalta-Lopes, J.; Botelho, M.F.; Marto, C.M.; Ferreira, M.M. Direct Pulp Capping: Which Is the Most Effective Biomaterial? A Retrospective Clinical Study. Materials 2019, 12, 3382. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, M.J.; Casey, J.A.; VanderWeele, R.A.; Vandewalle, K.S. Mechanical Properties of New Dental Pulp-Capping Materials. Gen. Dent. 2016, 64, 44–48. [Google Scholar] [PubMed]
- Bortoluzzi, E.A.; Niu, L.; Palani, C.D.; El-Awady, A.R.; Hammond, B.D.; Pei, D.; Tian, F.; Cutler, C.W.; Pashley, D.H.; Tay, F.R. Cytotoxicity and Osteogenic Potential of Silicate Calcium Cements as Potential Protective Materials for Pulpal Revascularization. Dent. Mater. 2015, 31, 1510–1522. [Google Scholar] [CrossRef]
- Al-Sarheed, M.A. Evaluation of Shear Bond Strength and SEM Observation of All-in-One Self-Etching Primer Used for Bonding of Fissure Sealants. J. Contemp Dent. Pract. 2006, 7, 9–16. [Google Scholar] [CrossRef] [PubMed]
- Davidson, C.; De Gee, A.; Feilzer, A. The Competition between the Composite-Dentin Bond Strength and the Polymerization Contraction Stress. J. Dent. Res. 1984, 63, 1396–1399. [Google Scholar] [CrossRef] [PubMed]
- Borges, M.A.P.; Matos, I.C.; Dias, K.R.H.C. Influence of Two Self-Etching Primer Systems on Enamel Adhesion. Braz. Dent. J. 2007, 18, 113–118. [Google Scholar] [CrossRef]
- Camilleri, J. Investigation of Biodentine as Dentine Replacement Material. J. Dent. 2013, 41, 600–610. [Google Scholar] [CrossRef]
- Gandolfi, M.G.; Siboni, F.; Polimeni, A.; Bossù, M.; Riccitiello, F.; Rengo, S.; Prati, C. In Vitro Screening of the Apatite-Forming Ability, Biointeractivity and Physical Properties of a Tricalcium Silicate Material for Endodontics and Restorative Dentistry. Dent. J. 2013, 1, 41–60. [Google Scholar] [CrossRef]
- Camilleri, J. Hydration Mechanisms of Mineral Trioxide Aggregate. Int. Endod. J. 2007, 40, 462–470. [Google Scholar] [CrossRef]
- Prati, C.; Gandolfi, M.G. Calcium Silicate Bioactive Cements: Biological Perspectives and Clinical Applications. Dent. Mater. 2015, 31, 351–370. [Google Scholar] [CrossRef]
- Muñoz, M.A.; Luque, I.; Hass, V.; Reis, A.; Loguercio, A.D.; Bombarda, N.H.C. Immediate Bonding Properties of Universal Adhesives to Dentine. J. Dent. 2013, 41, 404–411. [Google Scholar] [CrossRef] [PubMed]
- Luo, Q.; Li, Y.; Zhang, Z.; Peng, X.; Geng, G. Influence of Substrate Moisture on the Interfacial Bonding between Calcium Silicate Hydrate and Epoxy. Constr. Build. Mater. 2022, 320, 126252. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 Statement: An Updated Guideline for Reporting Systematic Reviews. Int. J. Surg. 2021, 88, 105906. [Google Scholar] [CrossRef] [PubMed]
- Hardan, L.; Bourgi, R.; Kharouf, N.; Mancino, D.; Zarow, M.; Jakubowicz, N.; Haikel, Y.; Cuevas-Suárez, C.E. Bond Strength of Universal Adhesives to Dentin: A Systematic Review and Meta-Analysis. Polymers 2021, 13, 814. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).