Animal Models for Investigating Osseointegration: An Overview of Implant Research over the Last Three Decades
Abstract
:1. Introduction
2. Use of Animal Models in Pre-Clinical Research
3. Small Animal Models
3.1. Rat
3.2. Rabbit
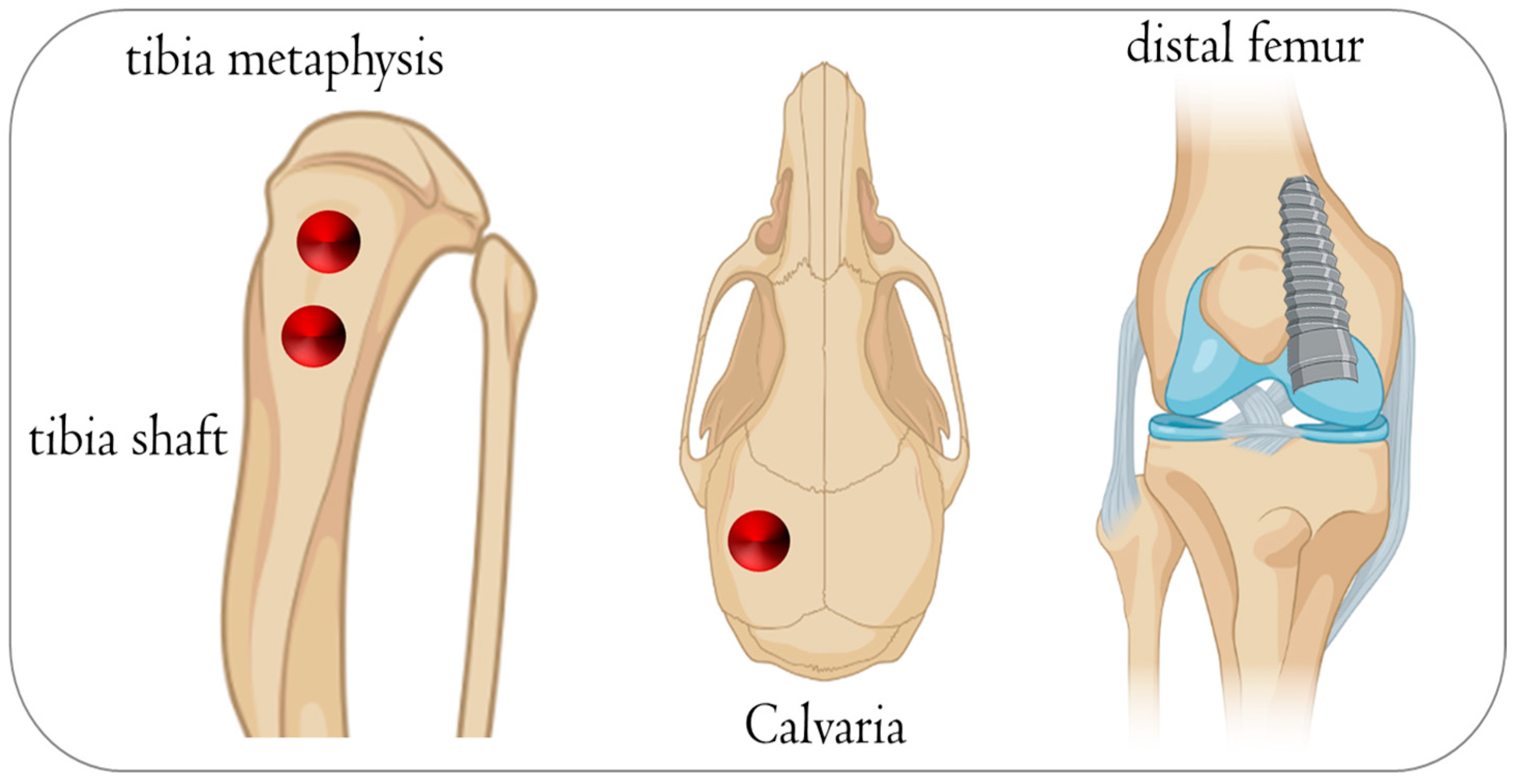
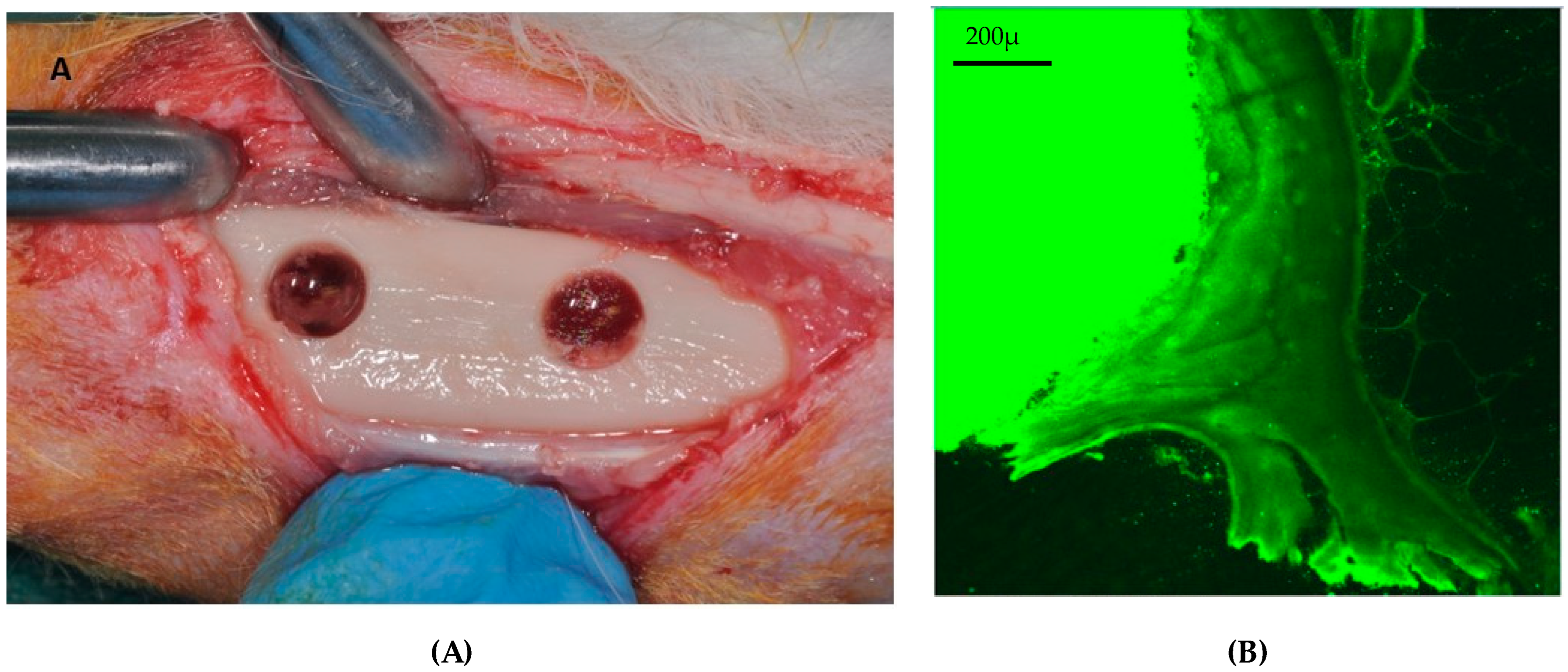
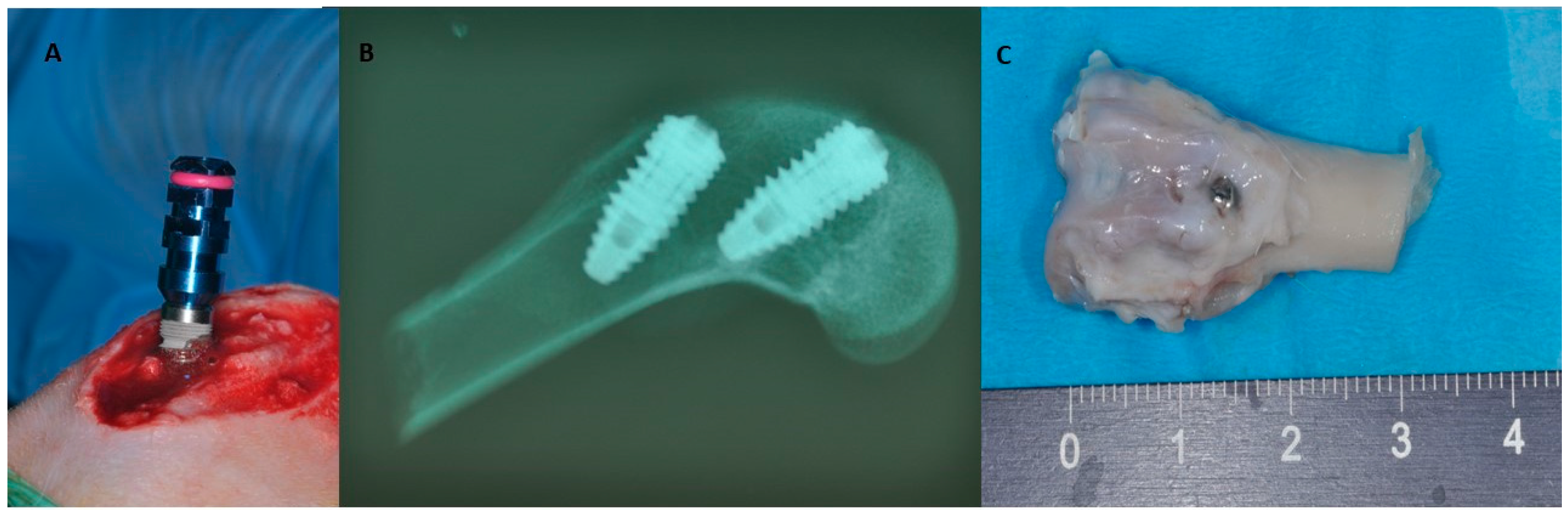
4. Large Animal Models
4.1. Sheep
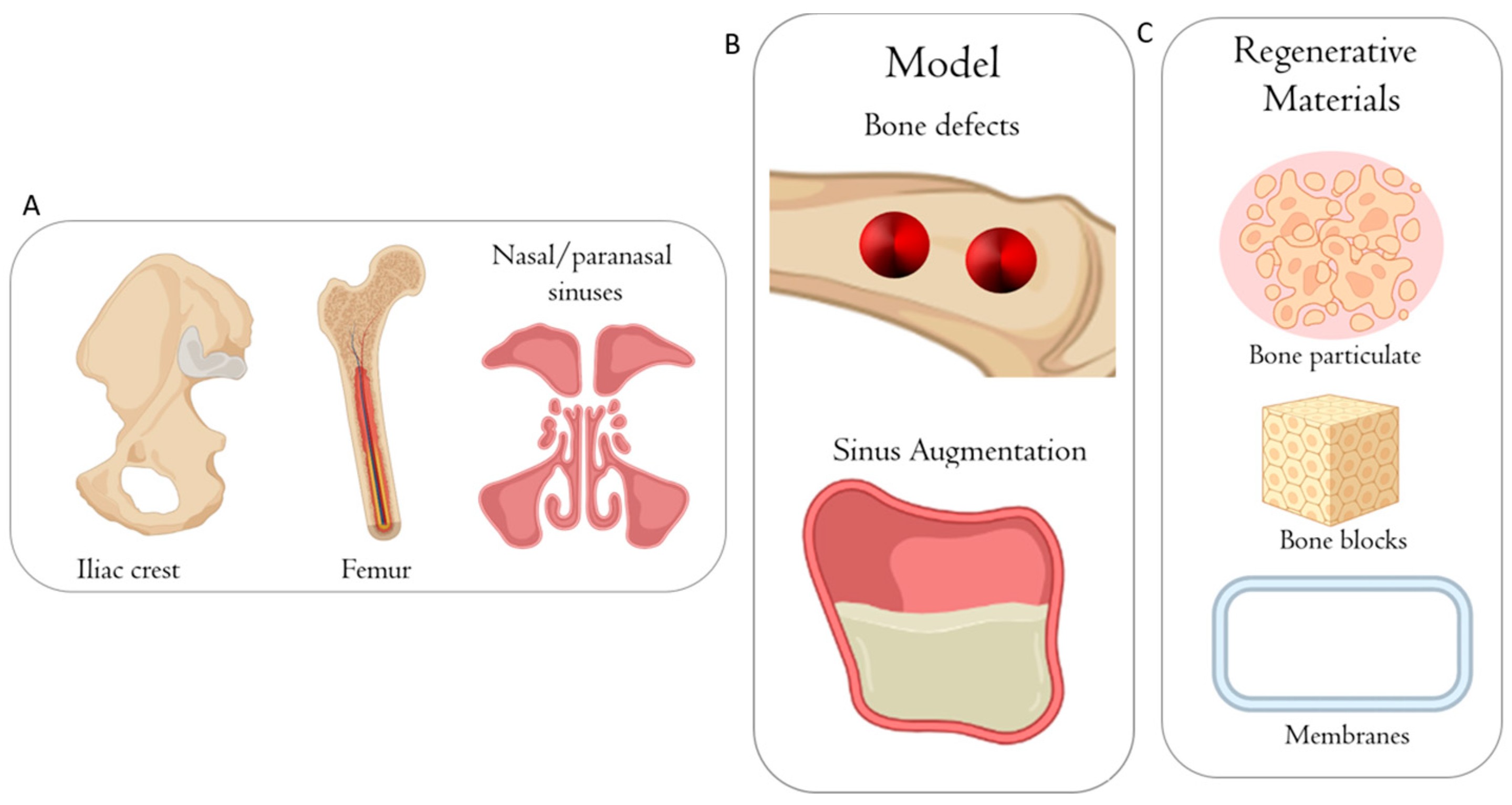
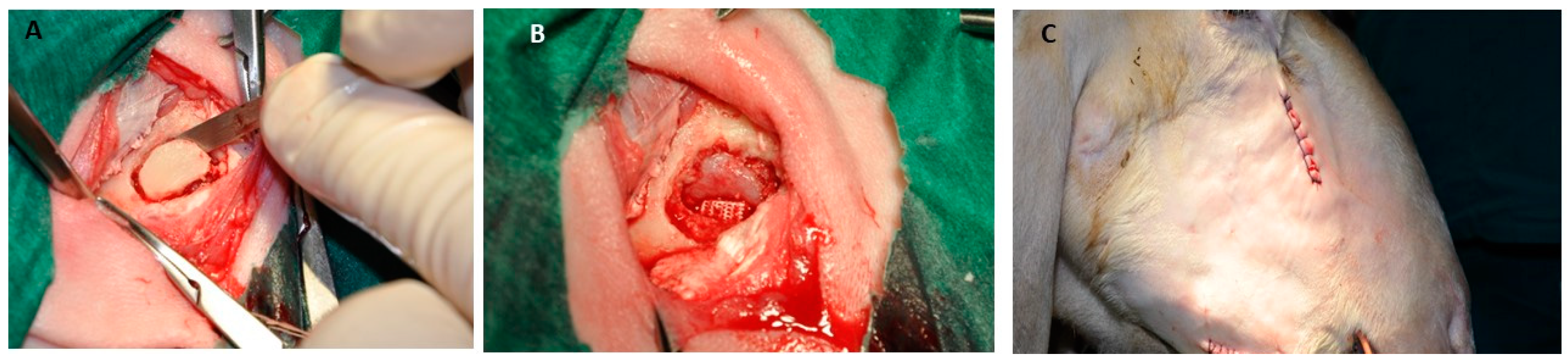
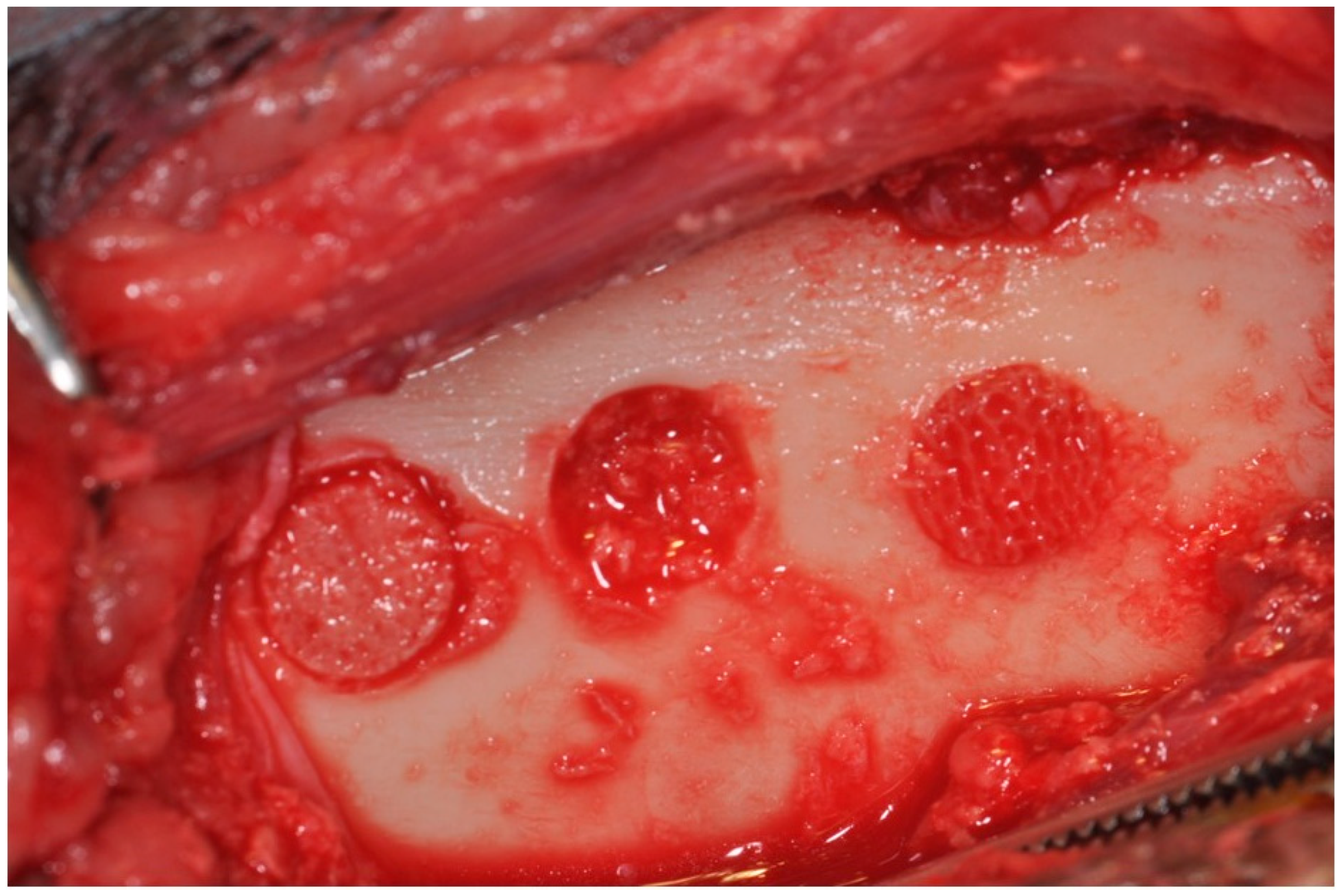
4.2. Minipig


4.3. Pig
4.4. Dogs
5. Discussion
6. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Tumedei, M.; Piattelli, A.; Degidi, M.; Mangano, C.; Iezzi, G. A Narrative Review of the Histological and Histomorphometrical Evaluation of the Peri-Implant Bone in Loaded and Unloaded Dental Implants. A 30-Year Experience (1988–2018). Int. J. Environ. Res. Public Health 2020, 17, 2088. [Google Scholar] [CrossRef] [PubMed]
- Tealdo, T.; Gelpi, F.; Grivetto, F.; Vallerga, E.; Tfaily, A.; De Santis, D.; Alberti, C.; Bevilacqua, M. A Retrospective Multicentric Study of 56 Patients Treated with 92 Pterygoid Implants for Partial/Full Arch Implant Supported Fixed Rehabilitation: Implant and Prosthesis Success Rat. Eur. J. Musculoskelet. Dis. 2023, 12, 119–126. [Google Scholar]
- Chrcanovic, B.R.; Kisch, J.; Albrektsson, T.; Wennerberg, A. Analysis of Risk Factors for Cluster Behavior of Dental Implant Failures. Clin. Implant Dent. Relat. Res. 2017, 19, 632–642. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Kang, T.; Liang, P.; Tang, Y.; Quan, C. Biological Activity of an Injectable Biphasic Calcium Phosphate/PMMA Bone Cement for Induced Osteogensis in Rabbit Model. Macromol. Biosci. 2018, 18, 1700331. [Google Scholar] [CrossRef] [PubMed]
- Yoshizawa, S.; Brown, A.; Barchowsky, A.; Sfeir, C. Magnesium Ion Stimulation of Bone Marrow Stromal Cells Enhances Osteogenic Activity, Simulating the Effect of Magnesium Alloy Degradation. Acta Biomater. 2014, 10, 2834–2842. [Google Scholar] [CrossRef] [PubMed]
- Park, C.; Park, S.; Lee, D.; Choi, K.S.; Lim, H.-P.; Kim, J. Graphene as an Enabling Strategy for Dental Implant and Tissue Regeneration. Tissue Eng. Regen. Med. 2017, 14, 481–493. [Google Scholar] [CrossRef] [PubMed]
- Del Fabbro, M.; Testori, T.; Kekovic, V.; Goker, F.; Tumedei, M.; Wang, H.-L. A Systematic Review of Survival Rates of Osseointegrated Implants in Fully and Partially Edentulous Patients Following Immediate Loading. J. Clin. Med. 2019, 8, 2142. [Google Scholar] [CrossRef]
- Piattelli, A.; Piattelli, M.; Romasco, N.; Trisi, P. Histochemical and Laser Scanning Microscopy Characterization of the Hydroxyapatite-Bone Interface: An Experimental Study in Rabbits. Int. J. Oral Maxillofac. Implants 1994, 9, 163–168. [Google Scholar]
- Greco, G.; Borgia, R.; Casto, C. Occlusal-Vertical Rebalancing for Implantprosthetic Planning: Technical Considerations. Eur. J. Musculoskelet. Dis. 2023, 12, 13–18. [Google Scholar]
- Cecchetti, F.; Di Girolamo, M.; Spuntarelli, M.; Baggi, L.; Ottria, L.; Mazza, D. Sub-Crestal Implants with Platform-Switching and One Time Abutment. Eur. J. Musculoskelet. Dis. 2023, 12, 133–137. [Google Scholar]
- Tchinda, A.; Chézeau, L.; Pierson, G.; Kouitat-Njiwa, R.; Rihn, B.H.; Bravetti, P. Biocompatibility of ZrO2 vs. Y-TZP Alloys: Influence of Their Composition and Surface Topography. Materials 2022, 15, 4655. [Google Scholar] [CrossRef]
- Syahruddin, M.H.; Anggraeni, R.; Ana, I.D. A Microfluidic Organ-on-a-Chip: Into the next Decade of Bone Tissue Engineering Applied in Dentistry. Future Sci. OA 2023, 9, FSO902. [Google Scholar] [CrossRef]
- Ribitsch, I.; Baptista, P.M.; Lange-Consiglio, A.; Melotti, L.; Patruno, M.; Jenner, F.; Schnabl-Feichter, E.; Dutton, L.C.; Connolly, D.J.; van Steenbeek, F.G.; et al. Large Animal Models in Regenerative Medicine and Tissue Engineering: To Do or Not to Do. Front. Bioeng. Biotechnol. 2020, 8, 972. [Google Scholar] [CrossRef]
- Animals in Science. Available online: https://environment.ec.europa.eu/topics/chemicals/animals-science_en (accessed on 21 October 2023).
- Prabhakar, S. Translational Research Challenges: Finding the Right Animal Models. J. Investig. Med. Off. Publ. Am. Fed. Clin. Res. 2012, 60, 1141–1146. [Google Scholar] [CrossRef]
- Wendler, A.; Wehling, M. The Translatability of Animal Models for Clinical Development: Biomarkers and Disease Models. Curr. Opin. Pharmacol. 2010, 10, 601–606. [Google Scholar] [CrossRef]
- Shanks, N.; Greek, R.; Greek, J. Are Animal Models Predictive for Humans? Philos. Ethics Humanit. Med. PEHM 2009, 4, 2. [Google Scholar] [CrossRef]
- Guidelines. Available online: https://www.isscr.org/guidelines (accessed on 21 October 2023).
- U.S. Food and Drug Administration. Animal Rule Information. 2023. Available online: https://www.fda.gov/emergency-preparedness-and-response/mcm-regulatory-science/animal-rule-information (accessed on 21 November 2023).
- du Sert, N.P.; Ahluwalia, A.; Alam, S.; Avey, M.T.; Baker, M.; Browne, W.J.; Clark, A.; Cuthill, I.C.; Dirnagl, U.; Emerson, M.; et al. Reporting Animal Research: Explanation and Elaboration for the ARRIVE Guidelines 2.0. PLoS Biol. 2020, 18, e3000411. [Google Scholar] [CrossRef]
- Home. ARRIVE Guidelines. Available online: https://arriveguidelines.org/ (accessed on 21 October 2023).
- Blanc-Sylvestre, N.; Bouchard, P.; Chaussain, C.; Bardet, C.; Preti, G.; Cavagnetto, D.; Gambarini, G. Pre-Clinical Models in Implant Dentistry: Past, Present, Future. Biomedicines 2021, 9, 1538. [Google Scholar] [CrossRef]
- Cao, X.; Gibbs, S.T.; Fang, L.; Miller, H.A.; Landowski, C.P.; Shin, H.C.; Lennernas, H.; Zhong, Y.; Amidon, G.L.; Yu, L.X.; et al. Why Is It Challenging to Predict Intestinal Drug Absorption and Oral Bioavailability in Human Using Rat Model. Pharm. Res. 2006, 23, 1675–1686. [Google Scholar] [CrossRef]
- Scarano, A.; Piattelli, M.; Vrespa, G.; Petrone, G.; Iezzi, G.; Piattelli, A. Bone Healing around Titanium and Titanium Nitride-Coated Dental Implants with Three Surfaces: An Experimental Study in Rats. Clin. Implant Dent. Relat. Res. 2003, 5, 103–111. [Google Scholar] [CrossRef]
- Jilka, R.L. The Relevance of Mouse Models for Investigating Age-Related Bone Loss in Humans. J. Gerontol. A Biol. Sci. Med. Sci. 2013, 68, 1209–1217. [Google Scholar] [CrossRef]
- Baron, R.; Tross, R.; Vignery, A. Evidence of Sequential Remodeling in Rat Trabecular Bone: Morphology, Dynamic Histomorphometry, and Changes during Skeletal Maturation. Anat. Rec. 1984, 208, 137–145. [Google Scholar] [CrossRef]
- Bagi, C.M.; Berryman, E.; Moalli, M.R. Comparative Bone Anatomy of Commonly Used Laboratory Animals: Implications for Drug Discovery. Comp. Med. 2011, 61, 76–85. [Google Scholar]
- Aerssens, J.; Boonen, S.; Lowet, G.; Dequeker, J. Interspecies Differences in Bone Composition, Density, and Quality: Potential Implications for in Vivo Bone Research. Endocrinology 1998, 139, 663–670. [Google Scholar] [CrossRef]
- Pilawski, I.; Tulu, U.S.; Ticha, P.; Schüpbach, P.; Traxler, H.; Xu, Q.; Pan, J.; Coyac, B.R.; Yuan, X.; Tian, Y.; et al. Interspecies Comparison of Alveolar Bone Biology, Part I: Morphology and Physiology of Pristine Bone. JDR Clin. Transl. Res. 2021, 6, 352–360. [Google Scholar] [CrossRef]
- Chen, C.-H.; Pei, X.; Tulu, U.S.; Aghvami, M.; Chen, C.-T.; Gaudillière, D.; Arioka, M.; Maghazeh Moghim, M.; Bahat, O.; Kolinski, M.; et al. A Comparative Assessment of Implant Site Viability in Humans and Rats. J. Dent. Res. 2018, 97, 451–459. [Google Scholar] [CrossRef]
- Vieira, A.E.; Repeke, C.E.; Ferreira Junior, S.B.; Colavite, P.M.; Biguetti, C.C.; Oliveira, R.C.; Assis, G.F.; Taga, R.; Trombone, A.P.F.; Garlet, G.P. Intramembranous Bone Healing Process Subsequent to Tooth Extraction in Mice: Micro-Computed Tomography, Histomorphometric and Molecular Characterization. PLoS ONE 2015, 10, e0128021. [Google Scholar] [CrossRef]
- Nunes, F.; Oliveira, P.; Bergamo, E.; Kjellin, P.; Novaes, A.; Ghiraldini, B.; Bezerra, F.; Scombatti de Souza, S. Effect of Smoke Exposure on Gene Expression in Bone Healing around Implants Coated with Nanohydroxyapatite. Nanomaterials 2022, 12, 3737. [Google Scholar] [CrossRef]
- He, X.; Yamada, M.; Watanabe, J.; Tiskratok, W.; Ishibashi, M.; Kitaura, H.; Mizoguchi, I.; Egusa, H. Titanium Nanotopography Induces Osteocyte Lacunar-Canalicular Networks to Strengthen Osseointegration. Acta Biomater. 2022, 151, 613–627. [Google Scholar] [CrossRef]
- Suliman, M.; Nagasawa, M.; Al-Omari, F.A.; Uoshima, K. The Effects of Collagen Cross-Link Deficiency on Osseointegration Process of Pure Titanium Implants. J. Prosthodont. Res. 2023. [Google Scholar] [CrossRef]
- Remísio, M.J.S.; Borges, T.; Castro, F.; Gehrke, S.A.; Fernandes, J.C.H.; Fernandes, G.V.d.O. Histologic Osseointegration Level Comparing Titanium and Zirconia Dental Implants: Meta-Analysis of Preclinical Studies. Int. J. Oral Maxillofac. Implants 2023, 38, 667–680. [Google Scholar] [CrossRef]
- Busuttil Naudi, K.; Ayoub, A.; McMahon, J.; Di Silvio, L.; Lappin, D.; Hunter, K.D.; Barbenel, J. Mandibular Reconstruction in the Rabbit Using Beta-Tricalcium Phosphate (β-TCP) Scaffolding and Recombinant Bone Morphogenetic Protein 7 (rhBMP-7)—Histological, Radiographic and Mechanical Evaluations. J. Cranio-Maxillo-Fac. Surg. Off. Publ. Eur. Assoc. Cranio-Maxillo-Fac. Surg. 2012, 40, e461–e469. [Google Scholar] [CrossRef]
- Mapara, M.; Thomas, B.S.; Bhat, K.M. Rabbit as an Animal Model for Experimental Research. Dent. Res. J. 2012, 9, 111. [Google Scholar] [CrossRef]
- Piattelli, A.; Scarano, A.; Piattelli, M. Detection of Alkaline and Acid Phosphatases around Titanium Implants: A Light Microscopical and Histochemical Study in Rabbits. Biomaterials 1995, 16, 1333–1338. [Google Scholar] [CrossRef]
- Brånemark, P.I.; Hansson, B.O.; Adell, R.; Breine, U.; Lindström, J.; Hallén, O.; Ohman, A. Osseointegrated Implants in the Treatment of the Edentulous Jaw. Experience from a 10-Year Period. Scand. J. Plast. Reconstr. Surg. Suppl. 1977, 16, 1–132. [Google Scholar]
- Brånemark, P.I. Intravital Microscopy. Its Present Status and Its Potentialities. Med. Biol. Illus. 1966, 16, 100–108. [Google Scholar]
- Castañeda, S.; Largo, R.; Calvo, E.; Rodríguez-Salvanés, F.; Marcos, M.E.; Díaz-Curiel, M.; Herrero-Beaumont, G. Bone Mineral Measurements of Subchondral and Trabecular Bone in Healthy and Osteoporotic Rabbits. Skelet. Radiol. 2006, 35, 34–41. [Google Scholar] [CrossRef]
- Calvo, E.; Castañeda, S.; Largo, R.; Fernández-Valle, M.E.; Rodríguez-Salvanés, F.; Herrero-Beaumont, G. Osteoporosis Increases the Severity of Cartilage Damage in an Experimental Model of Osteoarthritis in Rabbits. Osteoarthr. Cartil. 2007, 15, 69–77. [Google Scholar] [CrossRef]
- Scarano, A.; Inchingolo, F.; Rapone, B.; Lucchina, A.G.; Qorri, E.; Lorusso, F. Role of Autologous Platelet Gel (APG) in Bone Healing: A Rabbit Study. Appl. Sci. 2021, 11, 395. [Google Scholar] [CrossRef]
- Lorusso, F.; Ascani, G.; Inchingolo, F.; Tari, S.; Bugea, C.; Scarano, A. The bone-implant contact and osseointegration of different implant surface treatment: The findings from a systematic review of literature. Eur. J. Musculoskelet. Dis. 2023, 13, 95–117. [Google Scholar]
- Scarano, A.; Piattelli, A.; Quaranta, A.; Lorusso, F. Bone Response to Two Dental Implants with Different Sandblasted/Acid-Etched Implant Surfaces: A Histological and Histomorphometrical Study in Rabbits. BioMed Res. Int. 2017, 2017, 8724951. [Google Scholar] [CrossRef]
- Forni, F.; Marzagalli, M.; Tesei, P.; Grassi, A. Platelet Gel: Applications in Dental Regenerative Surgery. Blood Transfus. 2013, 11, 102. [Google Scholar] [CrossRef] [PubMed]
- Gehrke, S.A.; Pérez-Díaz, L.; Mazón, P.; De Aza, P.N. Biomechanical Effects of a New Macrogeometry Design of Dental Implants: An In Vitro Experimental Analysis. J. Funct. Biomater. 2019, 10, 47. [Google Scholar] [CrossRef] [PubMed]
- Gehrke, S.A.; Pérez-Albacete Martínez, C.; Piattelli, A.; Shibli, J.A.; Markovic, A.; Calvo Guirado, J.L. The Influence of Three Different Apical Implant Designs at Stability and Osseointegration Process: Experimental Study in Rabbits. Clin. Oral Implants Res. 2017, 28, 355–361. [Google Scholar] [CrossRef]
- Newman, E. The Potential of Sheep for the Study of Osteopenia: Current Status and Comparison with Other Animal Models. Bone 1995, 16, 277S–284S. [Google Scholar] [CrossRef] [PubMed]
- Ferguson, J.C.; Tangl, S.; Barnewitz, D.; Genzel, A.; Heimel, P.; Hruschka, V.; Redl, H.; Nau, T. A Large Animal Model for Standardized Testing of Bone Regeneration Strategies. BMC Vet. Res. 2018, 14, 330. [Google Scholar] [CrossRef] [PubMed]
- Pobloth, A.-M.; Johnson, K.A.; Schell, H.; Kolarczik, N.; Wulsten, D.; Duda, G.N.; Schmidt-Bleek, K. Establishment of a Preclinical Ovine Screening Model for the Investigation of Bone Tissue Engineering Strategies in Cancellous and Cortical Bone Defects. BMC Musculoskelet. Disord. 2016, 17, 111. [Google Scholar] [CrossRef]
- Ravaglioli, A.; Krajewski, A.; Celotti, G.C.; Piancastelli, A.; Bacchini, B.; Montanari, L.; Zama, G.; Piombi, L. Mineral Evolution of Bone. Biomaterials 1996, 17, 617–622. [Google Scholar] [CrossRef]
- Anderson, M.L.; Dhert, W.J.; de Bruijn, J.D.; Dalmeijer, R.A.; Leenders, H.; van Blitterswijk, C.A.; Verbout, A.J. Critical Size Defect in the Goat’s Os Ilium. A Model to Evaluate Bone Grafts and Substitutes. Clin. Orthop. 1999, 364, 231–239. [Google Scholar] [CrossRef]
- Eitel, F.; Klapp, F.; Jacobson, W.; Schweiberer, L. Bone Regeneration in Animals and in Man. A Contribution to Understanding the Relative Value of Animal Experiments to Human Pathophysiology. Arch. Orthop. Trauma. Surg. Arch. Orthop. Unf.-Chir. 1981, 99, 59–64. [Google Scholar] [CrossRef]
- Banstola, A.; Reynolds, J.N.J. The Sheep as a Large Animal Model for the Investigation and Treatment of Human Disorders. Biology 2022, 11, 1251. [Google Scholar] [CrossRef]
- Scarano, A.; Lorusso, F.; Ravera, L.; Mortellaro, C.; Piattelli, A. Bone Regeneration in Iliac Crestal Defects: An Experimental Study on Sheep. BioMed Res. Int. 2016, 2016, 4086870. [Google Scholar] [CrossRef]
- Parra, M.; Benalcázar Jalkh, E.B.; Tovar, N.; Torroni, A.; Badalov, R.M.; Bonfante, E.A.; Nayak, V.; Castellano, A.; Coelho, P.G.; Witek, L. The Influence of Surface Treatment on Osseointegration of Endosteal Implants Presenting Decompressing Vertical Chambers: An In Vivo Study in Sheep. Int. J. Oral Maxillofac. Implants 2022, 37, 929–936. [Google Scholar] [CrossRef]
- Sheftel, Y.; Ruddiman, F.; Schmidlin, P.; Duncan, W. Biphasic Calcium Phosphate and Polymer-Coated Bovine Bone Matrix for Sinus Grafting in an Animal Model. J. Biomed. Mater. Res. B Appl. Biomater. 2020, 108, 750–759. [Google Scholar] [CrossRef]
- Iezzi, G.; Scarano, A.; Valbonetti, L.; Mazzoni, S.; Furlani, M.; Mangano, C.; Muttini, A.; Raspanti, M.; Barboni, B.; Piattelli, A.; et al. Biphasic Calcium Phosphate Biomaterials: Stem Cell-Derived Osteoinduction or In Vivo Osteoconduction? Novel Insights in Maxillary Sinus Augmentation by Advanced Imaging. Materials 2021, 14, 2159. [Google Scholar] [CrossRef]
- Scarano, A.; Crincoli, V.; Di Benedetto, A.; Cozzolino, V.; Lorusso, F.; Podaliri Vulpiani, M.; Grano, M.; Kalemaj, Z.; Mori, G.; Grassi, F.R. Bone Regeneration Induced by Bone Porcine Block with Bone Marrow Stromal Stem Cells in a Minipig Model of Mandibular “Critical Size” Defect. Stem Cells Int. 2017, 2017, 9082869. [Google Scholar] [CrossRef]
- Nafei, A.; Kabel, J.; Odgaard, A.; Linde, F.; Hvid, I. Properties of Growing Trabecular Ovine Bone. J. Bone Jt. Surg. 2000, 82-B, 921–927. [Google Scholar] [CrossRef]
- Wang, S.; Liu, Y.; Fang, D.; Shi, S. The Miniature Pig: A Useful Large Animal Model for Dental and Orofacial Research. Oral Dis. 2007, 13, 530–537. [Google Scholar] [CrossRef]
- Yi, H.; Guo, W.; Chen, W.; Chen, L.; Ye, J.; Yang, S. Miniature Pigs: A Large Animal Model of Cochlear Implantation. Am. J. Transl. Res. 2016, 8, 5494. [Google Scholar]
- Bode, G.; Clausing, P.; Gervais, F.; Loegsted, J.; Luft, J.; Nogues, V.; Sims, J. The Utility of the Minipig as an Animal Model in Regulatory Toxicology. J. Pharmacol. Toxicol. Methods 2010, 62, 196–220. [Google Scholar] [CrossRef]
- Musskopf, M.L.; Stadler, A.F.; Wikesjö, U.M.E.; Susin, C. The Minipig Intraoral Dental Implant Model: A Systematic Review and Meta-Analysis. PLoS ONE 2022, 17, e0264475. [Google Scholar] [CrossRef] [PubMed]
- Pearce, A.I.; Richards, R.G.; Milz, S.; Schneider, E.; Pearce, S.G. Animal Models for Implant Biomaterial Research in Bone: A Review. Eur. Cells Mater. 2007, 13, 1–10. [Google Scholar] [CrossRef]
- Shahdad, S.; Bosshardt, D.; Patel, M.; Razaghi, N.; Patankar, A.; Roccuzzo, M. Benchmark Performance of Anodized vs. Sandblasted Implant Surfaces in an Acute Dehiscence Type Defect Animal Model. Clin. Oral Implants Res. 2022, 33, 1135–1146. [Google Scholar] [CrossRef] [PubMed]
- Glauser, R.; Schupbach, P. Early Bone Formation around Immediately Placed Two-Piece Tissue-Level Zirconia Implants with a Modified Surface: An Experimental Study in the Miniature Pig Mandible. Int. J. Implant Dent. 2022, 8, 37. [Google Scholar] [CrossRef] [PubMed]
- Rendenbach, C.; Fischer, H.; Kopp, A.; Schmidt-Bleek, K.; Kreiker, H.; Stumpp, S.; Thiele, M.; Duda, G.; Hanken, H.; Beck-Broichsitter, B.; et al. Improved in Vivo Osseointegration and Degradation Behavior of PEO Surface-Modified WE43 Magnesium Plates and Screws after 6 and 12 Months. Mater. Sci. Eng. C Mater. Biol. Appl. 2021, 129, 112380. [Google Scholar] [CrossRef] [PubMed]
- El Chaar, E.; Puisys, A.; Sabbag, I.; Bellón, B.; Georgantza, A.; Kye, W.; Pippenger, B.E. A Novel Fully Tapered, Self-Cutting Tissue-Level Implant: Non-Inferiority Study in Minipigs. Clin. Oral Investig. 2021, 25, 6127–6137. [Google Scholar] [CrossRef]
- Ide, Y.; Nakahara, T.; Nasu, M.; Matsunaga, S.; Iwanaga, T.; Tominaga, N.; Tamaki, Y. Postnatal Mandibular Cheek Tooth Development in the Miniature Pig Based on Two-Dimensional and Three-Dimensional X-ray Analyses. Anat. Rec. 2013, 296, 1247–1254. [Google Scholar] [CrossRef]
- Hou, N.; Du, X.; Wu, S. Advances in Pig Models of Human Diseases. Anim. Models Exp. Med. 2022, 5, 141–152. [Google Scholar] [CrossRef]
- Assenza, B.; Scarano, A.; Perrotti, V.; Vozza, I.; Quaranta, A.; Quaranta, M.; Piattelli, A.; Iezzi, G. Peri-Implant Bone Reactions around Immediately Loaded Conical Implants with Different Prosthetic Suprastructures: Histological and Histomorphometrical Study on Minipigs. Clin. Oral Investig. 2010, 14, 285–290. [Google Scholar] [CrossRef]
- Erdogan, Ö.; Üstün, Y.; Tatli, U.; Damlar, I.; Daglıoglu, K. A Pig Model for the Histomorphometric Evaluation of Hard Tissue Around Dental Implants. J. Oral Implantol. 2013, 39, 551–557. [Google Scholar] [CrossRef]
- Sova, S.S.; Tjäderhane, L.; Heikkilä, P.A.; Jernvall, J. A microCT Study of Three-Dimensional Patterns of Biomineralization in Pig Molars. Front. Physiol. 2018, 9, 71. [Google Scholar] [CrossRef] [PubMed]
- Olsen, M.L.; Aaboe, M.; Hjørting-Hansen, E.; Hansen, A.K. Problems Related to an Intraoral Approach for Experimental Surgery on Minipigs. Clin. Oral Implants Res. 2004, 15, 333–338. [Google Scholar] [CrossRef]
- Piattelli, A.; Cordioli, G.P.; Trisi, P.; Passi, P.; Favero, G.A.; Meffert, R.M. Light and Confocal Laser Scanning Microscopic Evaluation of Hydroxyapatite Resorption Patterns in Medullary and Cortical Bone. Int. J. Oral Maxillofac. Implants 1993, 8, 309–315. [Google Scholar]
- Schroeder, H.E.; Lindhe, J. Conversion of Stable Established Gingivitis in the Dog into Destructive Periodontitis. Arch. Oral Biol. 1975, 20, 775-IN2. [Google Scholar] [CrossRef] [PubMed]
- Huja, S.S.; Fernandez, S.A.; Hill, K.J.; Li, Y. Remodeling Dynamics in the Alveolar Process in Skeletally Mature Dogs. Anat. Rec. Part A Discov. Mol. Cell. Evol. Biol. 2006, 288, 1243–1249. [Google Scholar] [CrossRef] [PubMed]
- Vajda, E.G.; Kneissel, M.; Muggenburg, B.; Miller, S.C. Increased Intracortical Bone Remodeling during Lactation in Beagle Dogs. Biol. Reprod. 1999, 61, 1439–1444. [Google Scholar] [CrossRef]
- Scarano, A.; Assenza, B.; Piattelli, M.; Thams, U.; San Roman, F.; Favero, G.A.; Piattelli, A. Interimplant Distance and Crestal Bone Resorption: A Histologic Study in the Canine Mandible. Clin. Implant Dent. Relat. Res. 2004, 6, 150–156. [Google Scholar] [CrossRef]
- Tarnow, D.P.; Cho, S.C.; Wallace, S.S. The Effect of Inter-Implant Distance on the Height of Inter-Implant Bone Crest. J. Periodontol. 2000, 71, 546–549. [Google Scholar] [CrossRef]
- Berglundh, T.; Abrahamsson, I.; Lang, N.P.; Lindhe, J. De Novo Alveolar Bone Formation Adjacent to Endosseous Implants. Clin. Oral Implants Res. 2003, 14, 251–262. [Google Scholar] [CrossRef]
- Abrahamsson, I.; Berglundh, T.; Linder, E.; Lang, N.P.; Lindhe, J. Early Bone Formation Adjacent to Rough and Turned Endosseous Implant Surfaces. An Experimental Study in the Dog. Clin. Oral Implants Res. 2004, 15, 381–392. [Google Scholar] [CrossRef]
- Taguchi, T.; Lopez, M.J. An Overview of de Novo Bone Generation in Animal Models. J. Orthop. Res. Off. Publ. Orthop. Res. Soc. 2021, 39, 7–21. [Google Scholar] [CrossRef] [PubMed]
- International Organization for Standardization. Dentistry-Evaluation of Biocompatibility of Medical Devices Used in Dentistry; ISO: Geneva, Switzerland, 2018. [Google Scholar]
- Celletti, R.; Pameijer, C.H.; Bracchetti, G.; Donath, K.; Persichetti, G.; Visani, I. Histologic Evaluation of Osseointegrated Implants Restored in Nonaxial Functional Occlusion with Preangled Abutments. Int. J. Periodontics Restor. Dent. 1995, 15, 562–573. [Google Scholar]


| Animal Features | Species | |||||
|---|---|---|---|---|---|---|
| Rat | Rabbit | Dog | Minipig | Pig | Sheep | |
| Body temperature (°C) | 37.5–39.5 | 38–39.5 | 38–39 | 38.3–38.8 | 38–40 | 38.5–39.5 |
| Heart rate (bpm) | 250–450 | 150–300 | 60–160 | 68–72 | 90–100 | 60–80 |
| Respiration rate (pm) | 70–120 | 35–100 | 15–30 | 14–18 | 10–20 | 16–30 |
| Maximum weight (kg) * | 0.2–0.5 | 5–6 | 1–30 | 20–40 * | 150–400 | 40–70 |
| Mean life span (years) * | 2.5–3.5 | 5–15 | 10–15 | 15–18 | 15–20 | 10–12 |
| Species | Advantages | Disadvantages |
|---|---|---|
| Rat | Easy handling Low housing and breeding costs Widely available Short life span Short vital cycles Laboratory animal consciousness Model of diseases Easy genetic manipulation | Small size Huge differences compared to the human skeleton Limited surgery |
| Rabbit | Easy handling Low housing and breeding costs Widely available Docile Relatively short life span * Short vital cycles | Small size Macro and microstructures differ from human Limited surgery |
| Dog | Bone properties similar to human | Major ethical concerns (companion animals) Long life span Elevated costs Special facilities required |
| Minipig | Bone properties similar to human | |
| Pig | Size and weight near to human Good for surgery Bone properties similar to human Genetic tools available | Long life span Relatively elevated housing and breeding costs |
| Sheep | Size and weight near human Relatively low housing and breeding costs Widely available Hormone profile similar to women Good for surgery Bone properties similar to human | Long life span Seasonal breeders Higher trabecular bone densities in some locations |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scarano, A.; Khater, A.G.A.; Gehrke, S.A.; Inchingolo, F.; Tari, S.R. Animal Models for Investigating Osseointegration: An Overview of Implant Research over the Last Three Decades. J. Funct. Biomater. 2024, 15, 83. https://doi.org/10.3390/jfb15040083
Scarano A, Khater AGA, Gehrke SA, Inchingolo F, Tari SR. Animal Models for Investigating Osseointegration: An Overview of Implant Research over the Last Three Decades. Journal of Functional Biomaterials. 2024; 15(4):83. https://doi.org/10.3390/jfb15040083
Chicago/Turabian StyleScarano, Antonio, Ahmad G. A. Khater, Sergio Alexandre Gehrke, Francesco Inchingolo, and Sergio Rexhep Tari. 2024. "Animal Models for Investigating Osseointegration: An Overview of Implant Research over the Last Three Decades" Journal of Functional Biomaterials 15, no. 4: 83. https://doi.org/10.3390/jfb15040083






