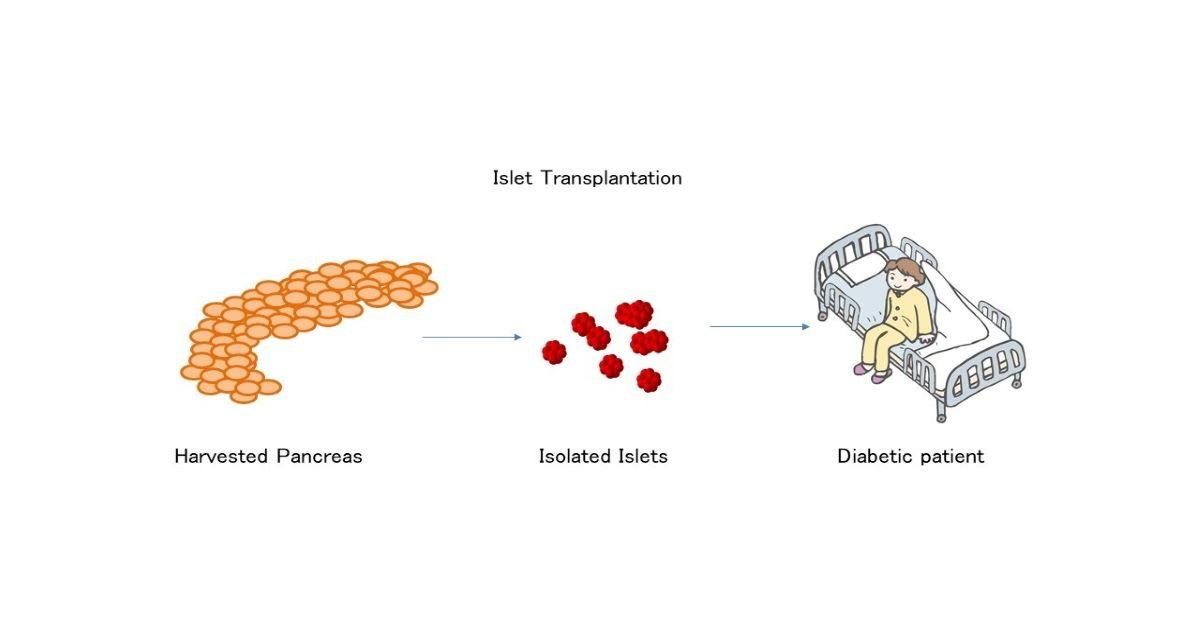
Islet Transplantation
A special issue of Cells (ISSN 2073-4409).
Deadline for manuscript submissions: closed (26 April 2024) | Viewed by 7497
Special Issue Editor
Special Issue Information
Dear Colleagues,
To date, diabetes is an incurable disease; however, beta cell replacement therapy can be a curative treatment for the diabetes.
Among the beta cell replacement therapies, islet transplantation has been evolutionally developed.
Allogenic islet transplantation has become the standard therapy for the treatment of type 1 diabetes, and, in some countries, autologous islet transplantation with total pancreatectomy has also become the standard therapy for the treatment of painful chronic pancreatitis.
Xenogeneic islet transplantation and regenerative medicine using stem cells for the treatment of diabetes is now entering the clinical trial phase.
Islet transplantation has been leading in the field of cell therapy and the progress being currently obtained is considerably exciting.
This Special Issue aims to explore the current state of the art of islet transplantation and future research focuses within this area.
Dr. Shinichi Matsumoto
Guest Editor
Manuscript Submission Information
Manuscripts should be submitted online at www.mdpi.com by registering and logging in to this website. Once you are registered, click here to go to the submission form. Manuscripts can be submitted until the deadline. All submissions that pass pre-check are peer-reviewed. Accepted papers will be published continuously in the journal (as soon as accepted) and will be listed together on the special issue website. Research articles, review articles as well as short communications are invited. For planned papers, a title and short abstract (about 100 words) can be sent to the Editorial Office for announcement on this website.
Submitted manuscripts should not have been published previously, nor be under consideration for publication elsewhere (except conference proceedings papers). All manuscripts are thoroughly refereed through a single-blind peer-review process. A guide for authors and other relevant information for submission of manuscripts is available on the Instructions for Authors page. Cells is an international peer-reviewed open access semimonthly journal published by MDPI.
Please visit the Instructions for Authors page before submitting a manuscript. The Article Processing Charge (APC) for publication in this open access journal is 2700 CHF (Swiss Francs). Submitted papers should be well formatted and use good English. Authors may use MDPI's English editing service prior to publication or during author revisions.
Keywords
- allogeneic islet transplantation
- islet isolation
- immunosuppression for islet transplantation
- autologous islet transplantation
- xenogeneic islet transplantation
- transplantation site for islet transplantation
- regenerative medicine for the treatment of diabetes






