Advancements in Drug Delivery Systems for the Treatment of Sarcopenia: An Updated Overview
Abstract
1. Introduction
2. Drug Delivery Systems and Formulations
2.1. Overview of Drug Delivery Approaches
2.2. Importance for Sarcopenia Treatment
3. Oral Delivery Systems
3.1. Advantages and Challenges
3.2. Oral Drug Delivery System
3.3. Recent Advantages in Oral Formulations
4. Injectable Delivery Systems
4.1. Intramuscular and Subcutaneous Injections
4.2. Innovations in Injectable Formulations
5. Transdermal Delivery Systems
State-of-the-Art Technologies
6. Nanotechnology-Based Drug Delivery Systems
6.1. Nanoparticles and Liposomes
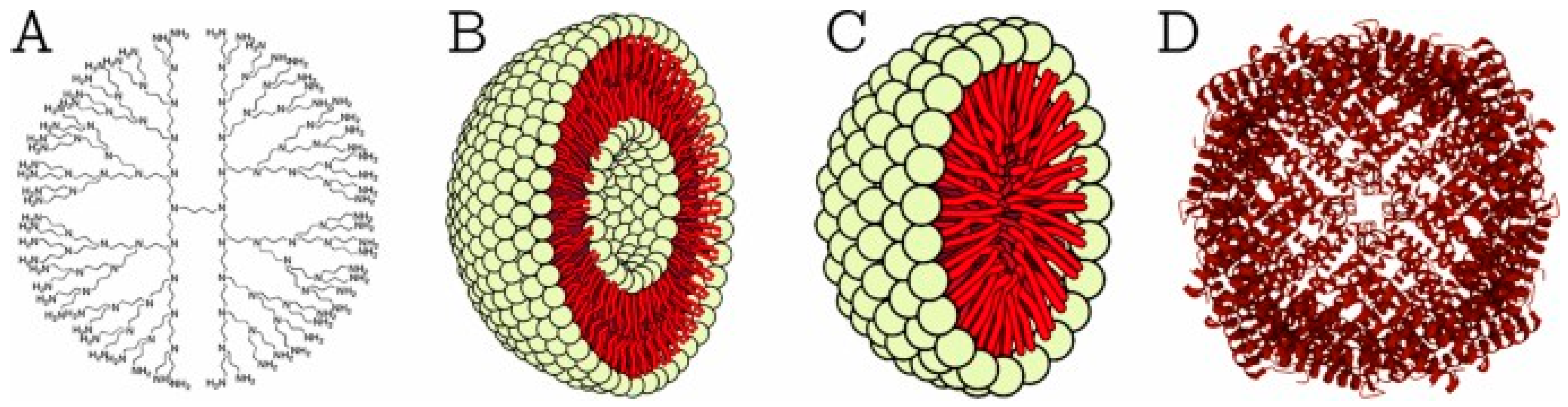
6.2. Micelles and Dendrimers
6.3. Targeted Delivery and Controlled Release
7. Polymer-Based Drug Delivery Systems
7.1. Biodegradable Polymers
7.2. Hydrogels and Smart Polymers
8. Peptide- and Protein-Based Delivery Systems
9. Emerging Delivery Technologies
9.1. Gene Therapy and Nucleic Acid Delivery
9.2. Cell-Based Delivery Systems
9.3. 3D Printing and Customized Drug Delivery
10. Preclinical and Clinical Studies
10.1. Key Findings from Animal Studies
10.2. Clinical Trials and Human Studies
10.2.1. Myostatin-Targeted Delivery Systems
10.2.2. Activin Receptor Antagonists
10.2.3. Follistatin Fusion Proteins and Gene Therapy
10.2.4. ACE Inhibitors
11. Regulatory and Ethical Considerations
12. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Evans, W.J.; Guralnik, J.; Cawthon, P.; Appleby, J.; Landi, F.; Clarke, L.; Vellas, B.; Ferrucci, L.; Roubenoff, R. Sarcopenia: No consensus, no diagnostic criteria, and no approved indication—How did we get here? GeroScience 2024, 46, 183–190. [Google Scholar] [CrossRef] [PubMed]
- Cho, M.-R.; Lee, S.; Song, S.-K. A Review of Sarcopenia Pathophysiology, Diagnosis, Treatment and Future Direction. J. Korean Med. Sci. 2022, 37, e146. [Google Scholar] [CrossRef] [PubMed]
- Lo, J.H.T.; Yiu, T.; Ong, M.T.Y.; Lee, W.Y.W. Sarcopenia: Current treatments and new regenerative therapeutic approaches. J. Orthop. Transl. 2020, 23, 38–52. [Google Scholar] [CrossRef] [PubMed]
- Sayer, A.A.; Cruz-Jentoft, A. Sarcopenia definition, diagnosis and treatment: Consensus is growing. Age Ageing 2022, 51, afac220. [Google Scholar] [CrossRef]
- Coletta, G.; Phillips, S.M. An elusive consensus definition of sarcopenia impedes research and clinical treatment: A narrative review. Ageing Res. Rev. 2023, 86, 101883. [Google Scholar] [CrossRef] [PubMed]
- Priego, T.; Martín, A.I.; González-Hedström, D.; Granado, M.; López-Calderón, A. Chapter Twenty—Role of hormones in sarcopenia. In Vitamins and Hormones; Litwack, G., Ed.; Academic Press: Cambridge, MA, USA, 2021; Volume 115, pp. 535–570. [Google Scholar]
- Shu, H.; Huang, Y.; Zhang, W.; Ling, L.; Hua, Y.; Xiong, Z. An integrated study of hormone-related sarcopenia for modeling and comparative transcriptome in rats. Front. Endocrinol. 2023, 14, 1073587. [Google Scholar] [CrossRef]
- Bian, A.; Ma, Y.; Zhou, X.; Guo, Y.; Wang, W.; Zhang, Y.; Wang, X. Association between sarcopenia and levels of growth hormone and insulin-like growth factor-1 in the elderly. BMC Musculoskelet. Disord. 2020, 21, 214. [Google Scholar] [CrossRef]
- Bellanti, F.; Lo Buglio, A.; Vendemiale, G. Mitochondrial Impairment in Sarcopenia. Biology 2021, 10, 31. [Google Scholar] [CrossRef]
- Wiedmer, P.; Jung, T.; Castro, J.P.; Pomatto, L.C.D.; Sun, P.Y.; Davies, K.J.A.; Grune, T. Sarcopenia—Molecular mechanisms and open questions. Ageing Res. Rev. 2021, 65, 101200. [Google Scholar] [CrossRef]
- Keller, K. Sarcopenia. Wien. Med. Wochenschr. 2019, 169, 157–172. [Google Scholar] [CrossRef]
- Hunter, G.R.; Singh, H.; Carter, S.J.; Bryan, D.R.; Fisher, G. Sarcopenia and Its Implications for Metabolic Health. J. Obes. 2019, 2019, 8031705. [Google Scholar] [CrossRef] [PubMed]
- Dunne, R.F.; Loh, K.P.; Williams, G.R.; Jatoi, A.; Mustian, K.M.; Mohile, S.G. Cachexia and Sarcopenia in Older Adults with Cancer: A Comprehensive Review. Cancers 2019, 11, 1861. [Google Scholar] [CrossRef] [PubMed]
- Dhillon, R.J.S.; Hasni, S. Pathogenesis and Management of Sarcopenia. Clin. Geriatr. Med. 2017, 33, 17–26. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Y.; Feng, J.; Yu, Y.; Ling, M.; Wang, X. Advances in sarcopenia: Mechanisms, therapeutic targets, and intervention strategies. Arch. Pharmacal Res. 2024, 47, 301–324. [Google Scholar] [CrossRef]
- Xie, W.-Q.; Xiao, G.-L.; Hu, P.-W.; He, Y.-Q.; Lv, S.; Xiao, W.-F. Possible sarcopenia: Early screening and intervention-narrative review. Ann. Palliat. Med. 2020, 9, 4283–4293. [Google Scholar] [CrossRef]
- Ackermans, L.L.G.C.; Rabou, J.; Basrai, M.; Schweinlin, A.; Bischoff, S.C.; Cussenot, O.; Cancel-Tassin, G.; Renken, R.J.; Gómez, E.; Sánchez-González, P.; et al. Screening, diagnosis and monitoring of sarcopenia: When to use which tool? Clin. Nutr. ESPEN 2022, 48, 36–44. [Google Scholar] [CrossRef]
- Li, Y.; Chen, M.; Zhao, Y.; Li, M.; Qin, Y.; Cheng, S.; Yang, Y.; Yin, P.; Zhang, L.; Tang, P. Advance in Drug Delivery for Ageing Skeletal Muscle. Front. Pharmacol. 2020, 11, 1016. [Google Scholar] [CrossRef]
- Naranjo, J.D.; Dziki, J.L.; Badylak, S.F. Regenerative Medicine Approaches for Age-Related Muscle Loss and Sarcopenia: A Mini-Review. Gerontology 2017, 63, 580–589. [Google Scholar] [CrossRef]
- Trucillo, P. Drug Carriers: Classification, Administration, Release Profiles, and Industrial Approach. Processes 2021, 9, 470. [Google Scholar] [CrossRef]
- Adepu, S.; Ramakrishna, S. Controlled Drug Delivery Systems: Current Status and Future Directions. Molecules 2021, 26, 5905. [Google Scholar] [CrossRef]
- Laffleur, F.; Keckeis, V. Advances in drug delivery systems: Work in progress still needed? Int. J. Pharm. 2020, 590, 119912. [Google Scholar] [CrossRef] [PubMed]
- Pandey, S.; Rajput, H. A Review Article on Novel Drug Delivery System. J. Res. Pharm. Sci. 2024, 10, 21–31. [Google Scholar]
- Vargason, A.M.; Anselmo, A.C.; Mitragotri, S. The evolution of commercial drug delivery technologies. Nat. Biomed. Eng. 2021, 5, 951–967. [Google Scholar] [CrossRef] [PubMed]
- Reza Rezaie, H.; Esnaashary, M.; Aref arjmand, A.; Öchsner, A. (Eds.) Classification of Drug Delivery Systems. In A Review of Biomaterials and Their Applications in Drug Delivery; Springer: Singapore, 2018; pp. 9–25. [Google Scholar]
- Khan, M.; Dangi, Y.S. Comprehensive review on controlled drug delivery systems: Future directions. World J. Pharm. Med. Res. 2023, 9, 158–166. [Google Scholar]
- Wang, S.; Liu, R.; Fu, Y.; Kao, W.J. Release mechanisms and applications of drug delivery systems for extended-release. Expert Opin. Drug Deliv. 2020, 17, 1289–1304. [Google Scholar] [CrossRef]
- Bellanti, F.; Lo Buglio, A.; Vendemiale, G. Muscle Delivery of Mitochondria-Targeted Drugs for the Treatment of Sarcopenia: Rationale and Perspectives. Pharmaceutics 2022, 14, 2588. [Google Scholar] [CrossRef]
- Vorrius, B.; Qiao, Z.; Ge, J.; Chen, Q. Smart Strategies to Overcome Drug Delivery Challenges in the Musculoskeletal System. Pharmaceuticals 2023, 16, 967. [Google Scholar] [CrossRef] [PubMed]
- Lou, J.; Duan, H.; Qin, Q.; Teng, Z.; Gan, F.; Zhou, X.; Zhou, X. Advances in Oral Drug Delivery Systems: Challenges and Opportunities. Pharmaceutics 2023, 15, 484. [Google Scholar] [CrossRef]
- Ahadian, S.; Finbloom, J.A.; Mofidfar, M.; Diltemiz, S.E.; Nasrollahi, F.; Davoodi, E.; Hosseini, V.; Mylonaki, I.; Sangabathuni, S.; Montazerian, H.; et al. Micro and nanoscale technologies in oral drug delivery. Adv. Drug Deliv. Rev. 2020, 157, 37–62. [Google Scholar] [CrossRef]
- Zhang, S.; Xing, M.; Li, B. Recent advances in musculoskeletal local drug delivery. Acta Biomater. 2019, 93, 135–151. [Google Scholar] [CrossRef]
- Mellen, R.H.; Girotto, O.S.; Marques, E.B.; Laurindo, L.F.; Grippa, P.C.; Mendes, C.G.; Garcia, L.N.H.; Bechara, M.D.; Barbalho, S.M.; Sinatora, R.V.; et al. Insights into Pathogenesis, Nutritional and Drug Approach in Sarcopenia: A Systematic Review. Biomedicines 2023, 11, 136. [Google Scholar] [CrossRef] [PubMed]
- Cao, W.; Zhu, A.; Chu, S.; Zhou, Q.; Zhou, Y.; Qu, X.; Tang, Q.; Zhang, Y. Correlation between nutrition, oral health, and different sarcopenia groups among elderly outpatients of community hospitals: A cross-sectional study of 1505 participants in China. BMC Geriatr. 2022, 22, 332. [Google Scholar] [CrossRef] [PubMed]
- Benet, L.Z.; Hosey, C.M.; Ursu, O.; Oprea, T.I. BDDCS, the Rule of 5 and drugability. Adv. Drug Deliv. Rev. 2016, 101, 89–98. [Google Scholar] [CrossRef] [PubMed]
- Homayun, B.; Lin, X.; Choi, H.-J. Challenges and Recent Progress in Oral Drug Delivery Systems for Biopharmaceuticals. Pharmaceutics 2019, 11, 129. [Google Scholar] [CrossRef] [PubMed]
- Dinh, L.; Yan, B. Oral Drug Delivery via Intestinal Lymphatic Transport Utilizing Lipid-Based Lyotropic Liquid Crystals. Liquids 2023, 3, 456–468. [Google Scholar] [CrossRef]
- Azman, M.; Sabri, A.H.; Anjani, Q.K.; Mustaffa, M.F.; Hamid, K.A. Intestinal Absorption Study: Challenges and Absorption Enhancement Strategies in Improving Oral Drug Delivery. Pharmaceuticals 2022, 15, 975. [Google Scholar] [CrossRef]
- Dan, N.; Samanta, K.; Almoazen, H. An Update on Pharmaceutical Strategies for Oral Delivery of Therapeutic Peptides and Proteins in Adults and Pediatrics. Children 2020, 7, 307. [Google Scholar] [CrossRef]
- Shreya, A.B.; Raut, S.Y.; Managuli, R.S.; Udupa, N.; Mutalik, S. Active Targeting of Drugs and Bioactive Molecules via Oral Administration by Ligand-Conjugated Lipidic Nanocarriers: Recent Advances. AAPS PharmSciTech 2018, 20, 15. [Google Scholar] [CrossRef]
- Campins, L.; Camps, M.; Riera, A.; Pleguezuelos, E.; Yebenes, J.C.; Serra-Prat, M. Oral Drugs Related with Muscle Wasting and Sarcopenia. A Review. Pharmacology 2016, 99, 1–8. [Google Scholar] [CrossRef]
- Alqahtani, M.S.; Kazi, M.; Alsenaidy, M.A.; Ahmad, M.Z. Advances in Oral Drug Delivery. Front. Pharmacol. 2021, 12, 618411. [Google Scholar] [CrossRef]
- Fasinu, P.; Pillay, V.; Ndesendo, V.M.; du Toit, L.C.; Choonara, Y.E. Diverse approaches for the enhancement of oral drug bioavailability. Biopharm. Drug Dispos. 2011, 32, 185–209. [Google Scholar] [CrossRef] [PubMed]
- Sohail Arshad, M.; Zafar, S.; Yousef, B.; Alyassin, Y.; Ali, R.; AlAsiri, A.; Chang, M.-W.; Ahmad, Z.; Ali Elkordy, A.; Faheem, A.; et al. A review of emerging technologies enabling improved solid oral dosage form manufacturing and processing. Adv. Drug Deliv. Rev. 2021, 178, 113840. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.-J.; Lee, J.-H.; Kim, S.-W.; Lee, S.-H.; Jung, D.-W.; Williams, D.R. Investigation of niclosamide as a repurposing agent for skeletal muscle atrophy. PLoS ONE 2021, 16, e0252135. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.; Zhang, H.; Chi, M.; Yang, Q.; Guo, C. Drugs for the Treatment of Muscle Atrophy. In Background and Management of Muscular Atrophy; Julianna, C., Ed.; IntechOpen: Rijeka, Croatia, 2021; Chapter 5. [Google Scholar]
- McCartan, A.J.S.; Curran, D.W.; Mrsny, R.J. Evaluating parameters affecting drug fate at the intramuscular injection site. J. Control. Release 2021, 336, 322–335. [Google Scholar] [CrossRef] [PubMed]
- Jin, J.-F.; Zhu, L.-L.; Chen, M.; Xu, H.-M.; Wang, H.-F.; Feng, X.-Q.; Zhu, X.-P.; Zhou, Q. The optimal choice of medication administration route regarding intravenous, intramuscular, and subcutaneous injection. Patient Prefer. Adherence 2015, 9, 923–942. [Google Scholar] [CrossRef]
- Tezze, C.; Sandri, M.; Tessari, P. Anabolic Resistance in the Pathogenesis of Sarcopenia in the Elderly: Role of Nutrition and Exercise in Young and Old People. Nutrients 2023, 15, 4073. [Google Scholar] [CrossRef]
- Jativa, S.D.; Thapar, N.; Broyles, D.; Dikici, E.; Daftarian, P.; Jiménez, J.J.; Daunert, S.; Deo, S.K. Enhanced Delivery of Plasmid DNA to Skeletal Muscle Cells using a DLC8-Binding Peptide and ASSLNIA-Modified PAMAM Dendrimer. Mol. Pharm. 2019, 16, 2376–2384. [Google Scholar] [CrossRef]
- Michiue, K.; Takayama, K.; Taniguchi, A.; Hayashi, Y.; Kogure, K. Increasing Skeletal Muscle Mass in Mice by Non-Invasive Intramuscular Delivery of Myostatin Inhibitory Peptide by Iontophoresis. Pharmaceuticals 2023, 16, 397. [Google Scholar] [CrossRef]
- Qazi, T.H.; Duda, G.N.; Ort, M.J.; Perka, C.; Geissler, S.; Winkler, T. Cell therapy to improve regeneration of skeletal muscle injuries. J. Cachexia Sarcopenia Muscle 2019, 10, 501–516. [Google Scholar] [CrossRef]
- Shushanov, S.S.; Kalinina, A.A.; Kravtsova, T.A.; Sherbakov, A.M.; Chernykh, Y.B.; Akentieva, N.P. Dual effect exhibited by insulin in myeloma and lymphoblastoid cells. Biointerface Res. Appl. Chem. 2022, 12, 2715–2728. [Google Scholar] [CrossRef]
- Zein, N.; Shehata, M.; Amer, A.M. Carvone’s Hypoglycemic and Hypolipidemic Potent Activity Via Regulation Insulin-Induced Genes in Diabetic Hyperlipidemic Rats. Biointerface Res. Appl. Chem. 2023, 13, 206. [Google Scholar] [CrossRef]
- Schou, J. Subcutaneous and Intramuscular Injection of Drugs. In Concepts in Biochemical Pharmacology: Part 1; Brodie, B.B., Gillette, J.R., Ackerman, H.S., Eds.; Springer: Berlin/Heidelberg, Germany, 1971; pp. 47–66. [Google Scholar]
- Afzal, M.; Kazmi, I.; Kaur, R.; Hosawi, S.B.I.; Kaleem, M.; Alzarea, S.I.; Ahmad, M.M. Chapter 1—Introduction to molecular pharmacology: Basic concepts. In How Synthetic Drugs Work; Kazmi, I., Karmakar, S., Shaharyar, M.A., Afzal, M., Al-Abbasi, F.A., Eds.; Academic Press: Cambridge, MA, USA, 2023; pp. 1–25. [Google Scholar]
- Bolger, G.T. Routes of Drug Administration. In Reference Module in Biomedical Sciences; Elsevier: Amsterdam, The Netherlands, 2018. [Google Scholar]
- Usach, I.; Martinez, R.; Festini, T.; Peris, J.-E. Subcutaneous Injection of Drugs: Literature Review of Factors Influencing Pain Sensation at the Injection Site. Adv. Ther. 2019, 36, 2986–2996. [Google Scholar] [CrossRef] [PubMed]
- Bittner, B.; Richter, W.; Schmidt, J. Subcutaneous Administration of Biotherapeutics: An Overview of Current Challenges and Opportunities. BioDrugs 2018, 32, 425–440. [Google Scholar] [CrossRef] [PubMed]
- Rigo, D.; da Silva, L.M.; Fischer, B.; Colet, R.; Dallago, R.M.; Zeni, J. Hyaluronic Acid—From Production to Application: A Review. Biointerface Res. Appl. Chem. 2023, 13, 211. [Google Scholar] [CrossRef]
- Fauzian, F.; Garmana, A.N.; Mauludin, R. Applications of Nanotechnology-Based Drug Delivery System for Delivering Natural Products into Acute and Chronic Wounds: A Review. Biointerface Res. Appl. Chem. 2023, 13, 426. [Google Scholar] [CrossRef]
- Obe Destiny, B.; Oluwatoyin, A.-F.; Oluwatosin, O.; Chinedu Paschal, M.; Chiamaka Chinaemelum, O.; Abdulraheem Olaide, B.; Olamide Tolulope, S. Innovations in drug delivery systems: A review of the pharmacist’s role in enhancing efficacy and patient compliance. World J. Adv. Res. Rev. 2023, 20, 1268–1282. [Google Scholar] [CrossRef]
- Peña-Juárez, M.C.; Guadarrama-Escobar, O.R.; Escobar-Chávez, J.J. Transdermal Delivery Systems for Biomolecules. J. Pharm. Innov. 2022, 17, 319–332. [Google Scholar] [CrossRef]
- Prasad, D.N.; Dua, J.S.; Soni, A. Article Reviewing Transdermal Drug Delivery System. J. Drug Deliv. Ther. 2022, 12, 176–180. [Google Scholar] [CrossRef]
- Alkilani, A.Z.; Nasereddin, J.; Hamed, R.; Nimrawi, S.; Hussein, G.; Abo-Zour, H.; Donnelly, R.F. Beneath the Skin: A Review of Current Trends and Future Prospects of Transdermal Drug Delivery Systems. Pharmaceutics 2022, 14, 1152. [Google Scholar] [CrossRef]
- Bird, D.; Ravindra, N.M. Transdermal drug delivery and patches—An overview. Med. Devices Sens. 2020, 3, e10069. [Google Scholar] [CrossRef]
- Jeong, W.Y.; Kwon, M.; Choi, H.E.; Kim, K.S. Recent advances in transdermal drug delivery systems: A review. Biomater. Res. 2021, 25, 24. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Zeng, L.; Song, W.; Liu, J. Influencing factors and drug application of iontophoresis in transdermal drug delivery: An overview of recent progress. Drug Deliv. Transl. Res. 2022, 12, 15–26. [Google Scholar] [CrossRef] [PubMed]
- Helmy, A.M. Overview of recent advancements in the iontophoretic drug delivery to various tissues and organs. J. Drug Deliv. Sci. Technol. 2021, 61, 102332. [Google Scholar] [CrossRef]
- Stephan, A.; Graca, F.A.; Hunt, L.C.; Demontis, F. Electroporation of Small Interfering RNAs into Tibialis Anterior Muscles of Mice. Bio Protoc. 2022, 12, e4428. [Google Scholar] [CrossRef] [PubMed]
- Marathe, D.; Bhuvanashree, V.S.; Mehta, C.H.; T., A.; Nayak, U.Y. Low-Frequency Sonophoresis: A Promising Strategy for Enhanced Transdermal Delivery. Adv. Pharmacol. Pharm. Sci. 2024, 2024, 1247450. [Google Scholar] [CrossRef]
- Teles, R.H.G.; Dutra, Y.M.; do Vale, D.B.N.; dos Santos, T.P.; Neto, J.C.R.M.; de Brito, T.V.; de Souza Costa, M.; de Oliveira, S.B.; de Souza Brauna, I.; da Silva, F.R.P. Photobiomodulation in the treatment of muscle injury: A systematic review. Crit. Rev.™ Phys. Rehabil. Med. 2018, 30, 1–14. [Google Scholar] [CrossRef]
- Zhang, Y.; Xu, Y.; Kong, H.; Zhang, J.; Chan, H.F.; Wang, J.; Shao, D.; Tao, Y.; Li, M. Microneedle system for tissue engineering and regenerative medicine. Exploration 2023, 3, 20210170. [Google Scholar] [CrossRef]
- Huang, D.; Yue, F.; Qiu, J.; Deng, M.; Kuang, S. Polymeric nanoparticles functionalized with muscle-homing peptides for targeted delivery of phosphatase and tensin homolog inhibitor to skeletal muscle. Acta Biomater. 2020, 118, 196–206. [Google Scholar] [CrossRef]
- Grech, A.; Breck, J.; Heidelbaugh, J. Adverse effects of testosterone replacement therapy: An update on the evidence and controversy. Ther. Adv. Drug Saf. 2014, 5, 190–200. [Google Scholar] [CrossRef]
- Bhasin, S.; Ellenberg, S.S.; Storer, T.W.; Basaria, S.; Pahor, M.; Stephens-Shields, A.J.; Cauley, J.A.; Ensrud, K.E.; Farrar, J.T.; Cella, D.; et al. Effect of testosterone replacement on measures of mobility in older men with mobility limitation and low testosterone concentrations: Secondary analyses of the Testosterone Trials. Lancet Diabetes Endocrinol. 2018, 6, 879–890. [Google Scholar] [CrossRef]
- LeBrasseur, N.K.; Lajevardi, N.; Miciek, R.; Mazer, N.; Storer, T.W.; Bhasin, S. Effects of testosterone therapy on muscle performance and physical function in older men with mobility limitations (The TOM Trial): Design and methods. Contemp. Clin. Trials 2009, 30, 133–140. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Yang, F.; Liu, Z.; Chen, W. Advances in research on pharmacotherapy of sarcopenia. Aging Med. 2021, 4, 221–233. [Google Scholar] [CrossRef]
- Thuraisingam, S.; Salim, N.; Azmi, I.D.M.; Kassim, N.K.; Basri, H. Development of Nanoemulsion containing Centella Asiatica Crude Extract as a Promising Drug Delivery System for Epilepsy Treatment. Biointerface Res. Appl. Chem. 2023, 13, 10–33263. [Google Scholar] [CrossRef]
- Yusuf, A.; Almotairy, A.R.Z.; Henidi, H.; Alshehri, O.Y.; Aldughaim, M.S. Nanoparticles as Drug Delivery Systems: A Review of the Implication of Nanoparticles’ Physicochemical Properties on Responses in Biological Systems. Polymers 2023, 15, 1596. [Google Scholar] [CrossRef]
- Sahu, T.; Ratre, Y.K.; Chauhan, S.; Bhaskar, L.V.K.S.; Nair, M.P.; Verma, H.K. Nanotechnology based drug delivery system: Current strategies and emerging therapeutic potential for medical science. J. Drug Deliv. Sci. Technol. 2021, 63, 102487. [Google Scholar] [CrossRef]
- Patra, J.K.; Das, G.; Fraceto, L.F.; Campos, E.V.R.; Rodriguez-Torres, M.d.P.; Acosta-Torres, L.S.; Diaz-Torres, L.A.; Grillo, R.; Swamy, M.K.; Sharma, S.; et al. Nano based drug delivery systems: Recent developments and future prospects. J. Nanobiotechnology 2018, 16, 71. [Google Scholar] [CrossRef] [PubMed]
- Afzal, O.; Altamimi, A.S.A.; Nadeem, M.S.; Alzarea, S.I.; Almalki, W.H.; Tariq, A.; Mubeen, B.; Murtaza, B.N.; Iftikhar, S.; Riaz, N.; et al. Nanoparticles in Drug Delivery: From History to Therapeutic Applications. Nanomaterials 2022, 12, 4494. [Google Scholar] [CrossRef]
- Colapicchioni, V.; Millozzi, F.; Parolini, O.; Palacios, D. Nanomedicine, a valuable tool for skeletal muscle disorders: Challenges, promises, and limitations. Wiley Interdiscip. Rev. Nanomed. Nanobiotechnology 2022, 14, e1777. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, Z.; Qaisar, R. Nanomedicine for Treating Muscle Dystrophies: Opportunities, Challenges, and Future Perspectives. Int. J. Mol. Sci. 2022, 23, 12039. [Google Scholar] [CrossRef]
- Malik, S.; Muhammad, K.; Waheed, Y. Emerging Applications of Nanotechnology in Healthcare and Medicine. Molecules 2023, 28, 6624. [Google Scholar] [CrossRef]
- Sim, S.; Wong, N.K. Nanotechnology and its use in imaging and drug delivery (Review). Biomed. Rep. 2021, 14, 42. [Google Scholar] [CrossRef] [PubMed]
- Rizvi, S.A.A.; Saleh, A.M. Applications of nanoparticle systems in drug delivery technology. Saudi Pharm. J. 2018, 26, 64–70. [Google Scholar] [CrossRef] [PubMed]
- Joudeh, N.; Linke, D. Nanoparticle classification, physicochemical properties, characterization, and applications: A comprehensive review for biologists. J. Nanobiotechnology 2022, 20, 262. [Google Scholar] [CrossRef] [PubMed]
- Mekuye, B.; Abera, B. Nanomaterials: An overview of synthesis, classification, characterization, and applications. Nano Sel. 2023, 4, 486–501. [Google Scholar] [CrossRef]
- Radzi, M.R.M.; Lim, C.K.; Sulaiman, N.; Jemon, K. Nanoparticles-based Chemo-Phototherapy Synergistic Effects for Breast Cancer Treatment: A Systematic Review. Biointerface Res. Appl. Chem. 2023, 13, 232. [Google Scholar] [CrossRef]
- Abbasi, A.; Sabahi, S.; Shahbazi, N.; Karimi, A.; Barkhordari, H. Nano Lipid Carrier in Augmenting the Bioavailability of Functional Bio-compounds. Biointerface Res. Appl. Chem. 2023, 13, 51. [Google Scholar] [CrossRef]
- Ishida, Y.; Kiyokawa, Y.; Asai, T.; Oku, N. Ameliorating Effects of Sphingomyelin-Based Liposomes on Sarcopenia in Senescence-Accelerated Mice. Biol. Pharm. Bull. 2016, 39, 786–793. [Google Scholar] [CrossRef]
- Chandrakala, V.; Aruna, V.; Angajala, G. Review on metal nanoparticles as nanocarriers: Current challenges and perspectives in drug delivery systems. Emergent Mater. 2022, 5, 1593–1615. [Google Scholar] [CrossRef]
- Foroughi, J.; Spinks, G. Carbon nanotube and graphene fiber artificial muscles. Nanoscale Adv. 2019, 1, 4592–4614. [Google Scholar] [CrossRef]
- Millozzi, F.; Papait, A.; Bouché, M.; Parolini, O.; Palacios, D. Nano-Immunomodulation: A New Strategy for Skeletal Muscle Diseases and Aging? Int. J. Mol. Sci. 2023, 24, 1175. [Google Scholar] [CrossRef]
- Law, S.K. Mini-Review for an Electrocatalytic Application of Carbon Nanotube in Medical Fields—Tissue Engineering, Drug Delivery, Cancer and SARS-CoV-2. Biointerface Res. Appl. Chem. 2023, 13, 43. [Google Scholar] [CrossRef]
- Kotta, S.; Aldawsari, H.M.; Badr-Eldin, S.M.; Nair, A.B.; Yt, K. Progress in Polymeric Micelles for Drug Delivery Applications. Pharmaceutics 2022, 14, 1636. [Google Scholar] [CrossRef] [PubMed]
- Atanase, L.I. Micellar Drug Delivery Systems Based on Natural Biopolymers. Polymers 2021, 13, 477. [Google Scholar] [CrossRef] [PubMed]
- Yetisgin, A.A.; Cetinel, S.; Zuvin, M.; Kosar, A.; Kutlu, O. Therapeutic Nanoparticles and Their Targeted Delivery Applications. Molecules 2020, 25, 2193. [Google Scholar] [CrossRef]
- Chavda, V.P. Chapter 4—Nanobased Nano Drug Delivery: A Comprehensive Review. In Applications of Targeted Nano Drugs and Delivery Systems; Mohapatra, S.S., Ranjan, S., Dasgupta, N., Mishra, R.K., Thomas, S., Eds.; Elsevier: Amsterdam, The Netherlands, 2019; pp. 69–92. [Google Scholar]
- Lu, Y.; Zhang, E.; Yang, J.; Cao, Z. Strategies to improve micelle stability for drug delivery. Nano Res. 2018, 11, 4985–4998. [Google Scholar] [CrossRef]
- Hari, S.K.; Gauba, A.; Shrivastava, N.; Tripathi, R.M.; Jain, S.K.; Pandey, A.K. Polymeric micelles and cancer therapy: An ingenious multimodal tumor-targeted drug delivery system. Drug Deliv. Transl. Res. 2023, 13, 135–163. [Google Scholar] [CrossRef]
- Torchilin, V.P. Micellar Nanocarriers: Pharmaceutical Perspectives. Pharm. Res. 2007, 24, 1–16. [Google Scholar] [CrossRef]
- Wang, J.; Li, B.; Qiu, L.; Qiao, X.; Yang, H. Dendrimer-based drug delivery systems: History, challenges, and latest developments. J. Biol. Eng. 2022, 16, 18. [Google Scholar] [CrossRef]
- Prabahar, K.; Alanazi, Z.; Qushawy, M. Targeted Drug Delivery System: Advantages, Carriers and Strategies. Indian J. Pharm. Educ. 2021, 55, 346–353. [Google Scholar] [CrossRef]
- Jana, P.; Shyam, M.; Singh, S.; Jayaprakash, V.; Dev, A. Biodegradable polymers in drug delivery and oral vaccination. Eur. Polym. J. 2021, 142, 110155. [Google Scholar] [CrossRef]
- Jafernik, K.; Ładniak, A.; Blicharska, E.; Czarnek, K.; Ekiert, H.; Wiącek, A.E.; Szopa, A. Chitosan-Based Nanoparticles as Effective Drug Delivery Systems—A review. Molecules 2023, 28, 1963. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.-C.; Su, M.-C.; Wu, C.-S.; Chen, P.-Y.; Chen, I.-F.; Lin, F.-H.; Kuo, S.-M. Ameliorative Effects of Cumin Extract-Encapsulated Chitosan Nanoparticles on Skeletal Muscle Atrophy and Grip Strength in Streptozotocin-Induced Diabetic Rats. Antioxidants 2024, 13, 6. [Google Scholar] [CrossRef] [PubMed]
- Mahdy, M.A.A.; Akl, M.A.; Madkour, F.A. Effect of chitosan and curcumin nanoparticles against skeletal muscle fibrosis at early regenerative stage of glycerol-injured rat muscles. BMC Musculoskelet. Disord. 2022, 23, 670. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.; Liu, H.; Luo, W.; Cai, T.; Li, Z.; Liu, Y.; Gao, W.; Wan, Q.; Wang, X.; Wang, J.; et al. Regeneration of skeletal system with genipin crosslinked biomaterials. J. Tissue Eng. 2020, 11, 2041731420974861. [Google Scholar] [CrossRef]
- Hariyadi, D.M.; Islam, N. Current Status of Alginate in Drug Delivery. Adv. Pharmacol. Pharm. Sci. 2020, 2020, 8886095. [Google Scholar] [CrossRef]
- Ciolacu, D.E.; Nicu, R.; Ciolacu, F. Cellulose-Based Hydrogels as Sustained Drug-Delivery Systems. Materials 2020, 13, 5270. [Google Scholar] [CrossRef]
- Velasco-Mallorquí, F.; Fernández-Costa, J.M.; Neves, L.; Ramón-Azcón, J. New volumetric CNT-doped gelatin-cellulose scaffolds for skeletal muscle tissue engineering. Nanoscale Adv. 2020, 2, 2885–2896. [Google Scholar] [CrossRef]
- Repellin, M.; Carton, F.; Boschi, F.; Galiè, M.; Perduca, M.; Calderan, L.; Jacquier, A.; Carras, J.; Schaeffer, L.; Briançon, S.; et al. Repurposing pentamidine using hyaluronic acid-based nanocarriers for skeletal muscle treatment in myotonic dystrophy. Nanomed. Nanotechnol. Biol. Med. 2023, 47, 102623. [Google Scholar] [CrossRef] [PubMed]
- Dienes, J.; Browne, S.; Farjun, B.; Amaral Passipieri, J.; Mintz, E.L.; Killian, G.; Healy, K.E.; Christ, G.J. Semisynthetic Hyaluronic Acid-Based Hydrogel Promotes Recovery of the Injured Tibialis Anterior Skeletal Muscle Form and Function. ACS Biomater. Sci. Eng. 2021, 7, 1587–1599. [Google Scholar] [CrossRef]
- Sikhosana, S.T.; Gumede, T.; Malebo, N.J.; Ogundeji, A. Poly(lactic acid) and its composites as functional materials for 3-D scaffolds in biomedical applications: A mini-review of recent trends. Express Polym. Lett. 2021, 15, 568–580. [Google Scholar] [CrossRef]
- Santoro, M.; Shah, S.R.; Walker, J.L.; Mikos, A.G. Poly (lactic acid) nanofibrous scaffolds for tissue engineering. Adv. Drug Deliv. Rev. 2016, 107, 206–212. [Google Scholar] [CrossRef] [PubMed]
- Tsung, T.-H.; Tsai, Y.-C.; Lee, H.-P.; Chen, Y.-H.; Lu, D.-W. Biodegradable Polymer-Based Drug-Delivery Systems for Ocular Diseases. Int. J. Mol. Sci. 2023, 24, 12976. [Google Scholar] [CrossRef] [PubMed]
- Jang, H.J.; Han, C.S.; Kwon, S.; Kwon, S.H.; Ko, S.; Kim, J.H.; Yoon, M.S.; Baek, S.; Lee, K.P. Poly(D, L-lactic-co-glycolic acid)-based microspheres loaded with camphor regulate skeletal muscle atrophy. Macromol. Res. 2024. [Google Scholar] [CrossRef]
- Pawar, R.; Pathan, A.; Nagaraj, S.; Kapare, H.; Giram, P.; Wavhale, R. Polycaprolactone and its derivatives for drug delivery. Polym. Adv. Technol. 2023, 34, 3296–3316. [Google Scholar] [CrossRef]
- Jain, A.; Behera, M.; Ravi, V.; Mishra, S.; Sundaresan, N.R.; Chatterjee, K. Recapitulating pathophysiology of skeletal muscle diseases in vitro using primary mouse myoblasts on a nanofibrous platform. Nanomed. Nanotechnol. Biol. Med. 2021, 32, 102341. [Google Scholar] [CrossRef]
- Yang, G.H.; Lee, J.; Kim, G. The fabrication of uniaxially aligned micro-textured polycaprolactone struts and application for skeletal muscle tissue regeneration. Biofabrication 2019, 11, 025005. [Google Scholar] [CrossRef]
- Ni, Z.; Yu, H.; Wang, L.; Shen, D.; Elshaarani, T.; Fahad, S.; Khan, A.; Haq, F.; Teng, L. Recent research progress on polyphosphazene-based drug delivery systems. J. Mater. Chem. B 2020, 8, 1555–1575. [Google Scholar] [CrossRef]
- Li, G.; Zhao, M.; Xu, F.; Yang, B.; Li, X.; Meng, X.; Teng, L.; Sun, F.; Li, Y. Synthesis and Biological Application of Polylactic Acid. Molecules 2020, 25, 5023. [Google Scholar] [CrossRef]
- Nuge, T.; Liu, Z.; Liu, X.; Ang, B.C.; Andriyana, A.; Metselaar, H.S.C.; Hoque, M.E. Recent Advances in Scaffolding from Natural-Based Polymers for Volumetric Muscle Injury. Molecules 2021, 26, 699. [Google Scholar] [CrossRef]
- Vigata, M.; Meinert, C.; Hutmacher, D.W.; Bock, N. Hydrogels as Drug Delivery Systems: A Review of Current Characterization and Evaluation Techniques. Pharmaceutics 2020, 12, 1188. [Google Scholar] [CrossRef]
- Liu, B.; Chen, K. Advances in Hydrogel-Based Drug Delivery Systems. Gels 2024, 10, 262. [Google Scholar] [CrossRef] [PubMed]
- Thang, N.H.; Chien, T.B.; Cuong, D.X. Polymer-Based Hydrogels Applied in Drug Delivery: An Overview. Gels 2023, 9, 523. [Google Scholar] [CrossRef] [PubMed]
- Priya James, H.; John, R.; Alex, A.; Anoop, K.R. Smart polymers for the controlled delivery of drugs—A concise overview. Acta Pharm. Sin. B 2014, 4, 120–127. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Mooney, D.J. Designing hydrogels for controlled drug delivery. Nat. Rev. Mater. 2016, 1, 16071. [Google Scholar] [CrossRef] [PubMed]
- Fattah-alhosseini, A.; Chaharmahali, R.; Alizad, S.; Kaseem, M.; Dikici, B. A review of smart polymeric materials: Recent developments and prospects for medicine applications. Hybrid Adv. 2024, 5, 100178. [Google Scholar] [CrossRef]
- Wells, C.M.; Harris, M.; Choi, L.; Murali, V.P.; Guerra, F.D.; Jennings, J.A. Stimuli-Responsive Drug Release from Smart Polymers. J. Funct. Biomater. 2019, 10, 34. [Google Scholar] [CrossRef]
- Du, J.; Bu, Z.; Jing, J.; Liu, W.; Fan, Z.; Huang, J.; Zhou, Z.; Hu, J.; An, J.; Hong, J.; et al. Treatment of Denervated Muscle Atrophy by Injectable Dual-responsive Hydrogels Loaded with Extracellular Vesicles, 01 August 2024, PREPRINT (Version 1). Available online: https://www.researchsquare.com/article/rs-4715142/v1 (accessed on 12 September 2024).
- Wang, L.; Zhang, X.; He, Y.; Wang, Y.; Zhong, W.; Mequanint, K.; Qiu, X.; Xing, M. Ultralight Conductive and Elastic Aerogel for Skeletal Muscle Atrophy Regeneration. Adv. Funct. Mater. 2019, 29, 1806200. [Google Scholar] [CrossRef]
- Chang, L.; Li, Y.; Li, M.; Liu, S.; Han, J.; Zhao, G.; Ji, C.; Lyu, Y.; Genin, G.M.; Bai, B.; et al. An Injectable, biodegradable magnetic hydrogel system for exogenous promotion of muscle mass and regeneration. Chem. Eng. J. 2021, 420, 130398. [Google Scholar] [CrossRef]
- Kurrikoff, K.; Vunk, B.; Langel, Ü. Status update in the use of cell-penetrating peptides for the delivery of macromolecular therapeutics. Expert Opin. Biol. Ther. 2021, 21, 361–370. [Google Scholar] [CrossRef]
- Huang, L.; Li, M.; Deng, C.; Qiu, J.; Wang, K.; Chang, M.; Zhou, S.; Gu, Y.; Shen, Y.; Wang, W.; et al. Potential Therapeutic Strategies for Skeletal Muscle Atrophy. Antioxidants 2023, 12, 44. [Google Scholar] [CrossRef]
- Berillo, D.; Yeskendir, A.; Zharkinbekov, Z.; Raziyeva, K.; Saparov, A. Peptide-Based Drug Delivery Systems. Medicina 2021, 57, 1209. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.; An, H.-W.; Wang, H. Self-Assembled Peptide Drug Delivery Systems. ACS Appl. Bio Mater. 2021, 4, 24–46. [Google Scholar] [CrossRef] [PubMed]
- Arun, A.; Malrautu, P.; Laha, A.; Luo, H.; Ramakrishna, S. Collagen Nanoparticles in Drug Delivery Systems and Tissue Engineering. Appl. Sci. 2021, 11, 11369. [Google Scholar] [CrossRef]
- Fischer, K.M.; Scott, T.E.; Browe, D.P.; McGaughey, T.A.; Wood, C.; Wolyniak, M.J.; Freeman, J.W. Hydrogels for Skeletal Muscle Regeneration. Regen. Eng. Transl. Med. 2021, 7, 353–361. [Google Scholar] [CrossRef]
- Jao, D.; Xue, Y.; Medina, J.; Hu, X. Protein-Based Drug-Delivery Materials. Materials 2017, 10, 517. [Google Scholar] [CrossRef]
- Yazdi, M.K.; Zarrintaj, P.; Ghavami, M.; Alizadeh, R.; Saeb, M.R. 7—Protein and peptide-based delivery systems. In Nanoengineered Biomaterials for Advanced Drug Delivery; Mozafari, M., Ed.; Elsevier: Amsterdam, The Netherlands, 2020; pp. 145–161. [Google Scholar]
- Yadav, A.R.; Mohite, S.K. Recent advances in protein and peptide drug delivery. Res. J. Pharm. Dos. Technol. 2020, 12, 205–212. [Google Scholar] [CrossRef]
- Lin, M.; Qi, X. Advances and Challenges of Stimuli-Responsive Nucleic Acids Delivery System in Gene Therapy. Pharmaceutics 2023, 15, 1450. [Google Scholar] [CrossRef]
- Fu, B.; Yang, J.; Yang, Y.; Xia, J.; He, Y.; Wang, Q.; Zhao, H.; Yang, H. Enhanced Muscle Fibers of Epinephelus coioides by Myostatin Autologous Nucleic Acid Vaccine. Int. J. Mol. Sci. 2022, 23, 6997. [Google Scholar] [CrossRef] [PubMed]
- Torres-Vanegas, J.D.; Cruz, J.C.; Reyes, L.H. Delivery Systems for Nucleic Acids and Proteins: Barriers, Cell Capture Pathways and Nanocarriers. Pharmaceutics 2021, 13, 428. [Google Scholar] [CrossRef]
- Gupta, A.; Andresen, J.L.; Manan, R.S.; Langer, R. Nucleic acid delivery for therapeutic applications. Adv. Drug Deliv. Rev. 2021, 178, 113834. [Google Scholar] [CrossRef]
- Poddar, A.; Banerjee, R.; Shukla, R. Editorial: Non-viral vectors for gene therapy/nucleic acid delivery. Front. Bioeng. Biotechnol. 2023, 11, 1304769. [Google Scholar] [CrossRef] [PubMed]
- Mollé, L.M.; Smyth, C.H.; Yuen, D.; Johnston, A.P.R. Nanoparticles for vaccine and gene therapy: Overcoming the barriers to nucleic acid delivery. WIREs Nanomed. Nanobiotechnology 2022, 14, e1809. [Google Scholar] [CrossRef] [PubMed]
- Andreana, I.; Repellin, M.; Carton, F.; Kryza, D.; Briançon, S.; Chazaud, B.; Mounier, R.; Arpicco, S.; Malatesta, M.; Stella, B.; et al. Nanomedicine for Gene Delivery and Drug Repurposing in the Treatment of Muscular Dystrophies. Pharmaceutics 2021, 13, 278. [Google Scholar] [CrossRef] [PubMed]
- Philippou, S.; Mastroyiannopoulos, N.P.; Makrides, N.; Lederer, C.W.; Kleanthous, M.; Phylactou, L.A. Selection and Identification of Skeletal-Muscle-Targeted RNA Aptamers. Mol. Ther.-Nucleic Acids 2018, 10, 199–214. [Google Scholar] [CrossRef]
- Jiang, W.; Zhan, W.; Zhou, L.; Dong, M.; Liu, L.; Xu, X.; Cao, Z. Potential therapeutic targets for sarcopenia identified by Mendelian randomisation. Age Ageing 2023, 52, afad024. [Google Scholar] [CrossRef]
- Chen, B.-B.; Wang, J.-Q.; Meng, X.-H.; Luo, Z.; Liu, X.-W.; Shen, H.; Xiao, H.-M.; Deng, H.-W. Putative Candidate Drug Targets for Sarcopenia-Related Traits Identified Through Mendelian Randomization Analysis of the Blood Proteome. Front. Genet. 2022, 13, 923429. [Google Scholar] [CrossRef]
- Yu, X.; Wang, Y.; Ran, L.; Jiang, Y.; Chen, M.; Du, H.; Zhang, Y.; Wu, D.; Xiang, X.; Zhang, J.; et al. Tetrahedral Framework Nucleic Acids Inhibit Muscular Mitochondria-Mediated Apoptosis and Ameliorate Muscle Atrophy in Sarcopenia. Nano Lett. 2023, 23, 8816–8826. [Google Scholar] [CrossRef]
- Yanai, K.; Kaneko, S.; Ishii, H.; Aomatsu, A.; Ito, K.; Hirai, K.; Ookawara, S.; Ishibashi, K.; Morishita, Y. MicroRNAs in Sarcopenia: A Systematic Review. Front. Med. 2020, 7, 180. [Google Scholar] [CrossRef]
- Lee, J.; Kang, H. Role of MicroRNAs and Long Non-Coding RNAs in Sarcopenia. Cells 2022, 11, 187. [Google Scholar] [CrossRef]
- Cai, Z.; Liu, D.; Yang, Y.; Xie, W.; He, M.; Yu, D.; Wu, Y.; Wang, X.; Xiao, W.; Li, Y. The role and therapeutic potential of stem cells in skeletal muscle in sarcopenia. Stem Cell Res. Ther. 2022, 13, 28. [Google Scholar] [CrossRef]
- Turkel, I.; Ozerklig, B.; Yılmaz, M.; Ulger, O.; Kubat, G.B.; Tuncer, M. Mitochondrial transplantation as a possible therapeutic option for sarcopenia. J. Mol. Med. 2023, 101, 645–669. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Yang, Y.; Chen, Y.; Xu, Y.; Peng, J. Cell-based drug delivery systems and their in vivo fate. Adv. Drug Deliv. Rev. 2022, 187, 114394. [Google Scholar] [CrossRef] [PubMed]
- Yu, H.; Yang, Z.; Li, F.; Xu, L.; Sun, Y. Cell-mediated targeting drugs delivery systems. Drug Deliv. 2020, 27, 1425–1437. [Google Scholar] [CrossRef] [PubMed]
- Bashor, C.J.; Hilton, I.B.; Bandukwala, H.; Smith, D.M.; Veiseh, O. Engineering the next generation of cell-based therapeutics. Nat. Rev. Drug Discov. 2022, 21, 655–675. [Google Scholar] [CrossRef] [PubMed]
- Elkasabgy, N.A.; Mahmoud, A.A.; Maged, A. 3D printing: An appealing route for customized drug delivery systems. Int. J. Pharm. 2020, 588, 119732. [Google Scholar] [CrossRef]
- Pandey, M.; Choudhury, H.; Fern, J.L.C.; Kee, A.T.K.; Kou, J.; Jing, J.L.J.; Her, H.C.; Yong, H.S.; Ming, H.C.; Bhattamisra, S.K.; et al. 3D printing for oral drug delivery: A new tool to customize drug delivery. Drug Deliv. Transl. Res. 2020, 10, 986–1001. [Google Scholar] [CrossRef]
- Wang, J.; Zhang, Y.; Aghda, N.H.; Pillai, A.R.; Thakkar, R.; Nokhodchi, A.; Maniruzzaman, M. Emerging 3D printing technologies for drug delivery devices: Current status and future perspective. Adv. Drug Deliv. Rev. 2021, 174, 294–316. [Google Scholar] [CrossRef]
- Beg, S.; Almalki, W.H.; Malik, A.; Farhan, M.; Aatif, M.; Rahman, Z.; Alruwaili, N.K.; Alrobaian, M.; Tarique, M.; Rahman, M. 3D printing for drug delivery and biomedical applications. Drug Discov. Today 2020, 25, 1668–1681. [Google Scholar] [CrossRef]
- Zielińska, A.; Karczewski, J.; Eder, P.; Kolanowski, T.; Szalata, M.; Wielgus, K.; Szalata, M.; Kim, D.; Shin, S.R.; Słomski, R.; et al. Scaffolds for drug delivery and tissue engineering: The role of genetics. J. Control. Release 2023, 359, 207–223. [Google Scholar] [CrossRef]
- Singh, R.P.; Sarju, N.; Sharma, A.; Singh, S.G.; Sanket, K. Microchip for Drug Delivery System: A Review. J. Appl. Pharm. Sci. 2011, 1, 7–11. [Google Scholar]
- Najm, A.; Niculescu, A.G.; Grumezescu, A.M.; Beuran, M. Emerging Therapeutic Strategies in Sarcopenia: An Updated Review on Pathogenesis and Treatment Advances. Int. J. Mol. Sci. 2024, 25, 4300. [Google Scholar] [CrossRef] [PubMed]
- Veronese, N.; Beaudart, C.; Sabico, S. Sarcopenia Research and Clinical Implications: Research and Clinical Implications; Springer International Publishing: Cham, Switzerland, 2021. [Google Scholar]
- Bahat, G.; Ozkok, S. The Current Landscape of Pharmacotherapies for Sarcopenia. Drugs Aging 2024, 41, 83–112. [Google Scholar] [CrossRef]
- Kwak, J.Y.; Kwon, K.S. Pharmacological Interventions for Treatment of Sarcopenia: Current Status of Drug Development for Sarcopenia. Ann. Geriatr. Med. Res. 2019, 23, 98–104. [Google Scholar] [CrossRef]
- Mantuano, P.; Boccanegra, B.; Bianchini, G.; Conte, E.; De Bellis, M.; Sanarica, F.; Camerino, G.M.; Pierno, S.; Cappellari, O.; Allegretti, M.; et al. BCAAs and Di-Alanine supplementation in the prevention of skeletal muscle atrophy: Preclinical evaluation in a murine model of hind limb unloading. Pharm. Res 2021, 171, 105798. [Google Scholar] [CrossRef]
- Mantuano, P.; Boccanegra, B.; Bianchini, G.; Cappellari, O.; Tulimiero, L.; Conte, E.; Cirmi, S.; Sanarica, F.; De Bellis, M.; Mele, A.; et al. Branched-Chain Amino Acids and Di-Alanine Supplementation in Aged Mice: A Translational Study on Sarcopenia. Nutrients 2023, 15, 330. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Arnau, F.M.; Fonfría-Vivas, R.; Buigues, C.; Castillo, Y.; Molina, P.; Hoogland, A.J.; van Doesburg, F.; Pruimboom, L.; Fernández-Garrido, J.; Cauli, O. Effects of Leucine Administration in Sarcopenia: A Randomized and Placebo-controlled Clinical Trial. Nutrients 2020, 12, 932. [Google Scholar] [CrossRef]
- Ebert, S.M.; Dyle, M.C.; Bullard, S.A.; Dierdorff, J.M.; Murry, D.J.; Fox, D.K.; Bongers, K.S.; Lira, V.A.; Meyerholz, D.K.; Talley, J.J.; et al. Identification and Small Molecule Inhibition of an Activating Transcription Factor 4 (ATF4)-dependent Pathway to Age-related Skeletal Muscle Weakness and Atrophy. J. Biol. Chem. 2015, 290, 25497–25511. [Google Scholar] [CrossRef] [PubMed]
- Ryu, D.; Mouchiroud, L.; Andreux, P.A.; Katsyuba, E.; Moullan, N.; Nicolet-dit-Félix, A.A.; Williams, E.G.; Jha, P.; Lo Sasso, G.; Huzard, D.; et al. Urolithin A induces mitophagy and prolongs lifespan in C. elegans and increases muscle function in rodents. Nat. Med. 2016, 22, 879–888. [Google Scholar] [CrossRef]
- Saud Gany, S.L.; Chin, K.-Y.; Tan, J.K.; Aminuddin, A.; Makpol, S. Curcumin as a Therapeutic Agent for Sarcopenia. Nutrients 2023, 15, 2526. [Google Scholar] [CrossRef]
- Uchitomi, R.; Oyabu, M.; Kamei, Y. Vitamin D and Sarcopenia: Potential of Vitamin D Supplementation in Sarcopenia Prevention and Treatment. Nutrients 2020, 12, 3189. [Google Scholar] [CrossRef]
- Sakuma, K.; Hamada, K.; Yamaguchi, A.; Aoi, W. Current Nutritional and Pharmacological Approaches for Attenuating Sarcopenia. Cells 2023, 12, 2422. [Google Scholar] [CrossRef]
- Becker, C.; Lord, S.R.; Studenski, S.A.; Warden, S.J.; Fielding, R.A.; Recknor, C.P.; Hochberg, M.C.; Ferrari, S.L.; Blain, H.; Binder, E.F.; et al. Myostatin antibody (LY2495655) in older weak fallers: A proof-of-concept, randomised, phase 2 trial. Lancet Diabetes Endocrinol. 2015, 3, 948–957. [Google Scholar] [CrossRef] [PubMed]
- Morvan, F.; Rondeau, J.-M.; Zou, C.; Minetti, G.; Scheufler, C.; Scharenberg, M.; Jacobi, C.; Brebbia, P.; Ritter, V.; Toussaint, G.; et al. Blockade of activin type II receptors with a dual anti-ActRIIA/IIB antibody is critical to promote maximal skeletal muscle hypertrophy. Proc. Natl. Acad. Sci. USA 2017, 114, 12448–12453. [Google Scholar] [CrossRef] [PubMed]
- Lach-Trifilieff, E.; Minetti, G.C.; Sheppard, K.; Ibebunjo, C.; Feige, J.N.; Hartmann, S.; Brachat, S.; Rivet, H.; Koelbing, C.; Morvan, F.; et al. An antibody blocking activin type II receptors induces strong skeletal muscle hypertrophy and protects from atrophy. Mol. Cell. Biol. 2014, 34, 606–618. [Google Scholar] [CrossRef] [PubMed]
- Rooks, D.; Praestgaard, J.; Hariry, S.; Laurent, D.; Petricoul, O.; Perry, R.G.; Lach-Trifilieff, E.; Roubenoff, R. Treatment of Sarcopenia with Bimagrumab: Results from a Phase II, Randomized, Controlled, Proof-of-Concept Study. J. Am. Geriatr. Soc. 2017, 65, 1988–1995. [Google Scholar] [CrossRef] [PubMed]
- Hanna, M.G.; Badrising, U.A.; Benveniste, O.; Lloyd, T.E.; Needham, M.; Chinoy, H.; Aoki, M.; Machado, P.M.; Liang, C.; Reardon, K.A.; et al. Safety and efficacy of intravenous bimagrumab in inclusion body myositis (RESILIENT): A randomised, double-blind, placebo-controlled phase 2b trial. Lancet Neurol. 2019, 18, 834–844. [Google Scholar] [CrossRef]
- Polkey, M.I.; Praestgaard, J.; Berwick, A.; Franssen, F.M.E.; Singh, D.; Steiner, M.C.; Casaburi, R.; Tillmann, H.C.; Lach-Trifilieff, E.; Roubenoff, R.; et al. Activin Type II Receptor Blockade for Treatment of Muscle Depletion in Chronic Obstructive Pulmonary Disease. A Randomized Trial. Am. J. Respir. Crit. Care Med. 2019, 199, 313–320. [Google Scholar] [CrossRef]
- Pearsall, R.S.; Davies, M.V.; Cannell, M.; Li, J.; Widrick, J.; Mulivor, A.W.; Wallner, S.; Troy, M.E.; Spaits, M.; Liharska, K.; et al. Follistatin-based ligand trap ACE-083 induces localized hypertrophy of skeletal muscle with functional improvement in models of neuromuscular disease. Sci. Rep. 2019, 9, 11392. [Google Scholar] [CrossRef]
- Onder, G.; Penninx, B.W.; Balkrishnan, R.; Fried, L.P.; Chaves, P.H.; Williamson, J.; Carter, C.; Di Bari, M.; Guralnik, J.M.; Pahor, M. Relation between use of angiotensin-converting enzyme inhibitors and muscle strength and physical function in older women: An observational study. Lancet 2002, 359, 926–930. [Google Scholar] [CrossRef]
- Hutcheon, S.D.; Gillespie, N.D.; Crombie, I.K.; Struthers, A.D.; McMurdo, M.E. Perindopril improves six minute walking distance in older patients with left ventricular systolic dysfunction: A randomised double blind placebo controlled trial. Heart 2002, 88, 373–377. [Google Scholar] [CrossRef]
- Maggio, M.; Ceda, G.P.; Lauretani, F.; Pahor, M.; Bandinelli, S.; Najjar, S.S.; Ling, S.M.; Basaria, S.; Ruggiero, C.; Valenti, G.; et al. Relation of Angiotensin-Converting Enzyme Inhibitor Treatment to Insulin-Like Growth Factor-1 Serum Levels in Subjects >65 Years of Age (the InCHIANTI Study). Am. J. Cardiol. 2006, 97, 1525–1529. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Band, M.M.; Sumukadas, D.; Struthers, A.D.; Avenell, A.; Donnan, P.T.; Kemp, P.R.; Smith, K.T.; Hume, C.L.; Hapca, A.; Witham, M.D. Leucine and ACE inhibitors as therapies for sarcopenia (LACE trial): Study protocol for a randomised controlled trial. Trials 2018, 19, 6. [Google Scholar] [CrossRef] [PubMed]
- Ragelle, H.; Danhier, F.; Préat, V.; Langer, R.; Anderson, D.G. Nanoparticle-based drug delivery systems: A commercial and regulatory outlook as the field matures. Expert Opin. Drug Deliv. 2017, 14, 851–864. [Google Scholar] [CrossRef] [PubMed]
- Chen, H.-H.; Yeo, H.-T.; Huang, Y.-H.; Tsai, L.-K.; Lai, H.-J.; Tsao, Y.-P.; Chen, S.-L. AAV-NRIP gene therapy ameliorates motor neuron degeneration and muscle atrophy in ALS model mice. Skelet. Muscle 2024, 14, 17. [Google Scholar] [CrossRef]
| Principles | Factors |
|---|---|
| Patient-related principles |
|
| Medication-related principles |
|
| Pharmacoeconomic-related principles |
|
| Advantages |
|
| Disadvantages |
|
| Classification | Polymer | Characteristics | Refs. | |
|---|---|---|---|---|
| Natural | Chitosan |
| [107,108,109,110,111] | |
| Alginate |
| [107,111,112] | ||
| Cellulose |
| [107,113,114] | ||
| Hyaluronic acid |
| [107,115,116] | ||
| Synthetic | Polylactic acid |
| [66,117,118] | |
| Poly (lactic-co-glycolic acid) |
| [119,120] | ||
| Polycaprolactone |
| [107,121,122,123] | ||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Najm, A.; Moldoveanu, E.-T.; Niculescu, A.-G.; Grumezescu, A.M.; Beuran, M.; Gaspar, B.S. Advancements in Drug Delivery Systems for the Treatment of Sarcopenia: An Updated Overview. Int. J. Mol. Sci. 2024, 25, 10766. https://doi.org/10.3390/ijms251910766
Najm A, Moldoveanu E-T, Niculescu A-G, Grumezescu AM, Beuran M, Gaspar BS. Advancements in Drug Delivery Systems for the Treatment of Sarcopenia: An Updated Overview. International Journal of Molecular Sciences. 2024; 25(19):10766. https://doi.org/10.3390/ijms251910766
Chicago/Turabian StyleNajm, Alfred, Elena-Theodora Moldoveanu, Adelina-Gabriela Niculescu, Alexandru Mihai Grumezescu, Mircea Beuran, and Bogdan Severus Gaspar. 2024. "Advancements in Drug Delivery Systems for the Treatment of Sarcopenia: An Updated Overview" International Journal of Molecular Sciences 25, no. 19: 10766. https://doi.org/10.3390/ijms251910766
APA StyleNajm, A., Moldoveanu, E.-T., Niculescu, A.-G., Grumezescu, A. M., Beuran, M., & Gaspar, B. S. (2024). Advancements in Drug Delivery Systems for the Treatment of Sarcopenia: An Updated Overview. International Journal of Molecular Sciences, 25(19), 10766. https://doi.org/10.3390/ijms251910766







