Initial Experience of Robot-Assisted Transabdominal Preperitoneal (TAPP) Inguinal Hernia Repair by a Single Surgeon in South Korea
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Patients
2.3. Statistics and Ethical Considerations
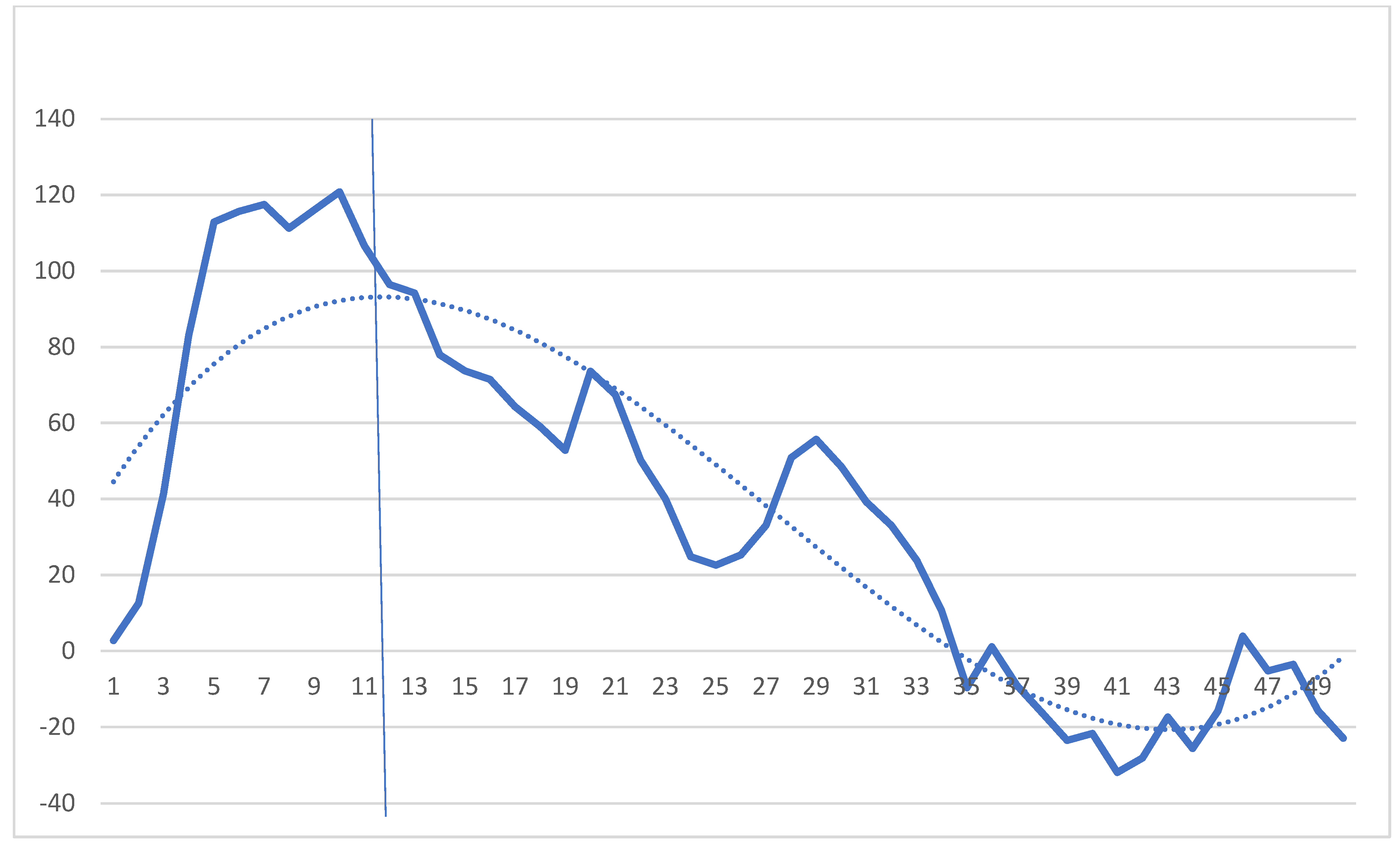
2.4. Cumulative Sum (CUSUM) Analysis
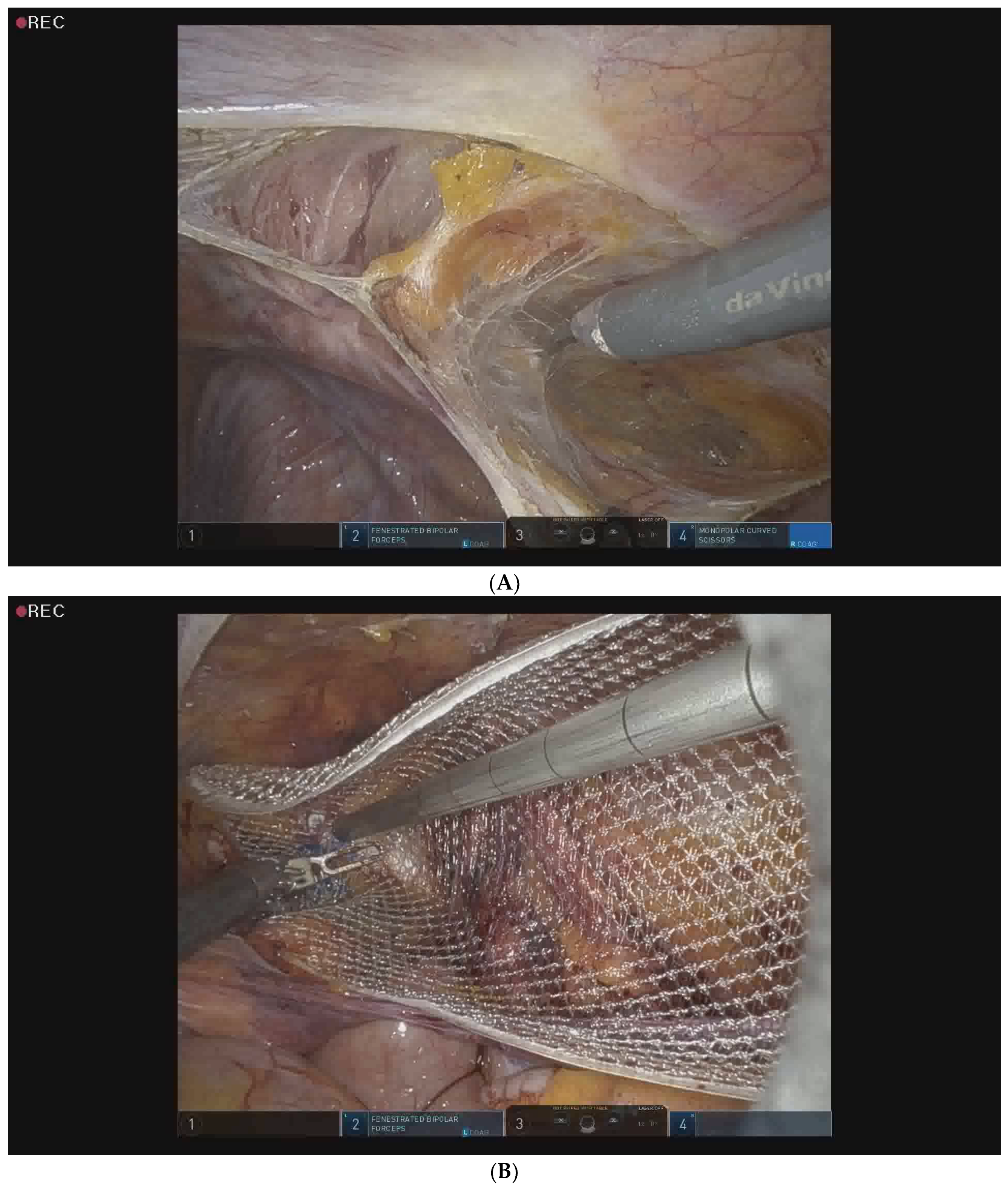
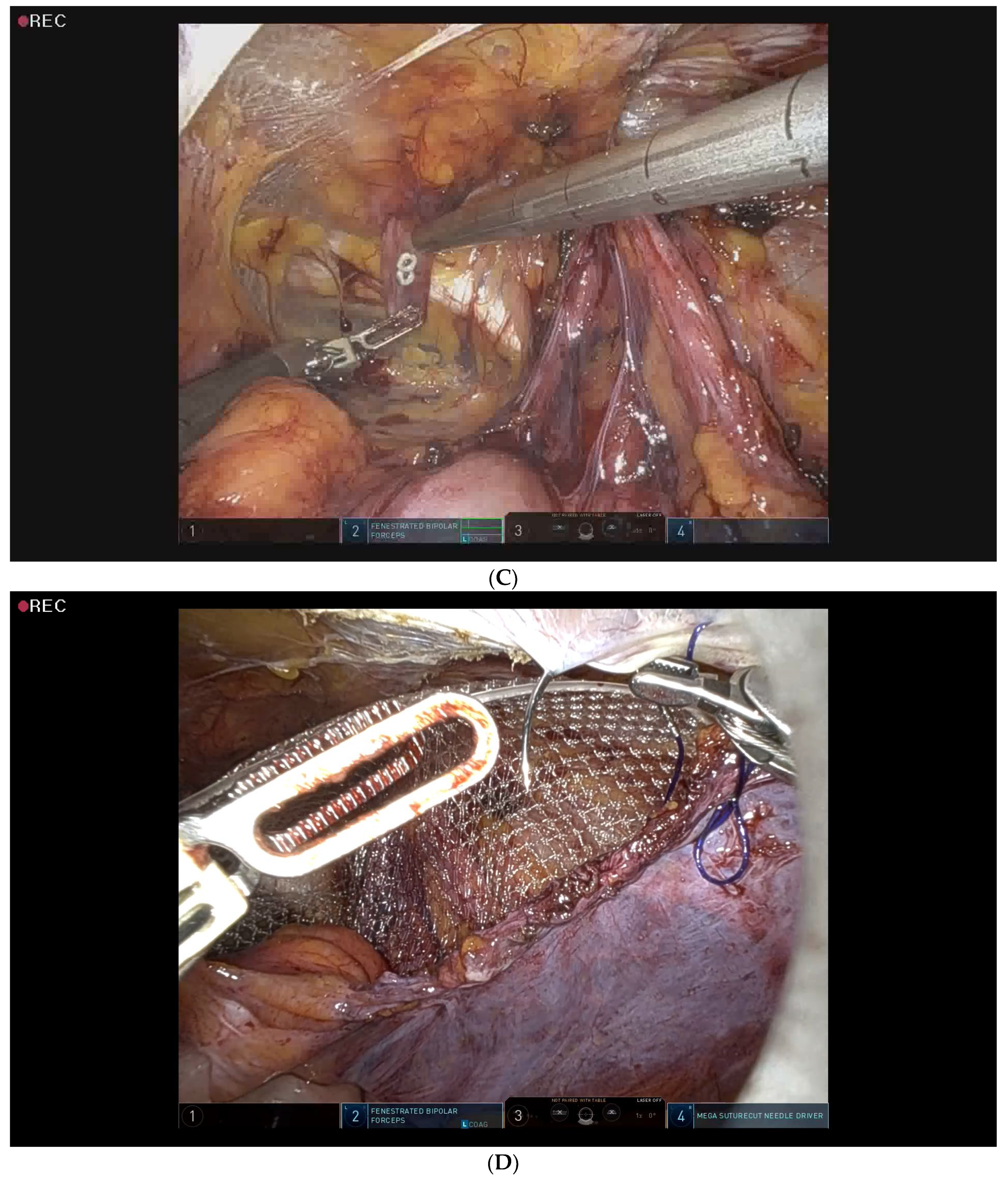
2.5. Surgical Procedure for Robotic-Assisted TAPP Inguinal Hernia Repair
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- International guidelines for groin hernia management. Hernia 2018, 22, 1–165. [CrossRef] [PubMed] [Green Version]
- Kingsnorth, A.; LeBlanc, K. Hernias: Inguinal and incisional. Lancet 2003, 362, 1561–1571. [Google Scholar] [CrossRef] [PubMed]
- Schumpelick, V.; Treutner, K.H.; Arlt, G. Inguinal hernia repair in adults. Lancet 1994, 344, 375–379. [Google Scholar] [CrossRef] [PubMed]
- Han, S.R.; Kim, H.J.; Kim, N.H.; Shin, S.; Yoo, R.N.; Kim, G.; Cho, H.M. Inguinal hernia surgery in Korea: Nationwide data from 2007–2015. Ann. Surg. Treat. Res. 2019, 97, 41–47. [Google Scholar] [CrossRef] [PubMed]
- Health Insurance Review and Assessment Service. Korea Healthcare Bigdata Hub [Internet]; Health Insurance Review and Assessment Service: Wonju, Republic of Korea, 2021. Available online: http://opendata.hira.or.kr/ (accessed on 6 January 2020).
- Ger, R. Laparoscopic hernia operation. Der Chirurg; Zeitschrift fur alle Gebiete der Operativen Medizen 1991, 62, 266–270. [Google Scholar] [PubMed]
- Aiolfi, A.; Cavalli, M.; Micheletto, G.; Lombardo, F.; Bonitta, G.; Morlacchi, A.; Bruni, P.G.; Campanelli, G.; Bona, D. Primary inguinal hernia: Systematic review and Bayesian network meta-analysis comparing open, laparoscopic transabdominal preperitoneal, totally extraperitoneal, and robotic preperitoneal repair. Hernia 2019, 23, 473–484. [Google Scholar] [CrossRef] [PubMed]
- Pirolla, E.H.; Patriota, G.P.; Pirolla, F.J.C.; Ribeiro, F.P.G.; Rodrigues, M.G.; Ismail, L.R.; Ruano, R.M. Inguinal Repair via Robotic Assisted Technique: Literature Review. Arq. Bras. Cir. Dig. ABCD Braz. Arch. Dig. Surg. 2018, 31, e1408. [Google Scholar] [CrossRef]
- Aiolfi, A.; Cavalli, M.; Micheletto, G.; Bruni, P.G.; Lombardo, F.; Perali, C.; Bonitta, G.; Bona, D. Robotic inguinal hernia repair: Is technology taking over? Systematic review and meta-analysis. Hernia 2019, 23, 509–519. [Google Scholar] [CrossRef]
- Ishii, H.; Rai, B.P.; Stolzenburg, J.U.; Bose, P.; Chlosta, P.L.; Somani, B.K.; Nabi, G.; Qazi, H.A.; Rajbabu, K.; Kynaston, H.; et al. Robotic or open radical cystectomy, which is safer? A systematic review and meta-analysis of comparative studies. J. Endourol. 2014, 28, 1215–1223. [Google Scholar] [CrossRef]
- Escobar Dominguez, J.E.; Ramos, M.G.; Seetharamaiah, R.; Donkor, C.; Rabaza, J.; Gonzalez, A. Feasibility of robotic inguinal hernia repair, a single-institution experience. Surg. Endosc. 2016, 30, 4042–4048. [Google Scholar] [CrossRef]
- Oviedo, R.J.; Robertson, J.C.; Alrajhi, S. First 101 Robotic General Surgery Cases in a Community Hospital. JSLS J. Soc. Laparoendosc. Surg. 2016, 20, e2016.00056. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Arcerito, M.; Changchien, E.; Bernal, O.; Konkoly-Thege, A.; Moon, J. Robotic Inguinal Hernia Repair: Technique and Early Experience. Am. Surg. 2016, 82, 1014–1017. [Google Scholar] [CrossRef]
- Kudsi, O.Y.; McCarty, J.C.; Paluvoi, N.; Mabardy, A.S. Transition from Laparoscopic Totally Extraperitoneal Inguinal Hernia Repair to Robotic Transabdominal Preperitoneal Inguinal Hernia Repair: A Retrospective Review of a Single Surgeon’s Experience. World J. Surg. 2017, 41, 2251–2257. [Google Scholar] [CrossRef] [PubMed]
- Escobar Dominguez, J.E.; Gonzalez, A.; Donkor, C. Robotic inguinal hernia repair. J. Surg. Oncol. 2015, 112, 310–314. [Google Scholar] [CrossRef] [PubMed]
- Qabbani, A.; Aboumarzouk, O.M.; ElBakry, T.; Al-Ansari, A.; Elakkad, M.S. Robotic inguinal hernia repair: Systematic review and meta-analysis. ANZ J. Surg. 2021, 91, 2277–2287. [Google Scholar] [CrossRef]
- Morrell, A.L.G.; Morrell Junior, A.C.; Mendes, J.M.F.; Morrell, A.G.; Morrell, A. Robotic TAPP inguinal hernia repair: Lessons learned from 97 cases. Rev. Col. Bras. Cir. 2021, 48, e20202704. [Google Scholar] [CrossRef]
- Prabhu, A.S.; Carbonell, A.; Hope, W.; Warren, J.; Higgins, R.; Jacob, B.; Blatnik, J.; Haskins, I.; Alkhatib, H.; Tastaldi, L.; et al. Robotic Inguinal vs. Transabdominal Laparoscopic Inguinal Hernia Repair: The RIVAL Randomized Clinical Trial. JAMA Surg. 2020, 155, 380–387. [Google Scholar] [CrossRef]
- Tatarian, T.; Nie, L.; McPartland, C.; Brown, A.M.; Yang, J.; Altieri, M.S.; Spaniolas, K.; Docimo, S.; Pryor, A.D. Comparative perioperative and 5-year outcomes of robotic and laparoscopic or open inguinal hernia repair: A study of 153,727 patients in the state of New York. Surg. Endosc. 2021, 35, 7209–7218. [Google Scholar] [CrossRef]
- Tam, V.; Rogers, D.E.; Al-Abbas, A.; Borrebach, J.; Dunn, S.A.; Zureikat, A.H.; Zeh, H.J., 3rd; Hogg, M.E. Robotic Inguinal Hernia Repair: A Large Health System’s Experience With the First 300 Cases and Review of the Literature. J. Surg. Res. 2019, 235, 98–104. [Google Scholar] [CrossRef]
- Kudsi, O.Y.; Bou-Ayash, N.; Gokcal, F.; Crawford, A.S.; Chung, S.K.; Chudner, A.; Litwin, D. Learning curve of robot-assisted transabdominal preperitoneal (rTAPP) inguinal hernia repair: A cumulative sum (CUSUM) analysis. Surg. Endosc. 2022, 36, 1827–1837. [Google Scholar] [CrossRef]
- González-Sánchez, M.; González-Poveda, I.; Mera-Velasco, S.; Cuesta-Vargas, A.I. Comparison of fatigue accumulated during and after prolonged robotic and laparoscopic surgical methods: A cross-sectional study. Surg. Endosc. 2017, 31, 1119–1135. [Google Scholar] [CrossRef] [PubMed]
- Armijo, P.R.; Huang, C.K.; High, R.; Leon, M.; Siu, K.C.; Oleynikov, D. Ergonomics of minimally invasive surgery: An analysis of muscle effort and fatigue in the operating room between laparoscopic and robotic surgery. Surg. Endosc. 2019, 33, 2323–2331. [Google Scholar] [CrossRef] [PubMed]
- Yoon, S.H.; Jung, M.C.; Park, S.Y. Evaluation of surgeon’s muscle fatigue during thoracoscopic pulmonary lobectomy using interoperative surface electromyography. J. Thorac. Dis. 2016, 8, 1162–1169. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Choi, Y.; Joo, H.-j.; Ahn, J.-H.; Kong, H.-J.; Yi, J. Forearm Muscle Activity Patterns during Open Thyroidectomy Using 8-Channel Surface Electromyography. J. Endocr. Surg. 2021, 21, 27–37. [Google Scholar] [CrossRef]


| Variables | All (n = 100) | Laparoscopic TAPP (n = 50) | Robotic TAPP (n = 50) | p-Value |
|---|---|---|---|---|
| Age (years, mean ± SD) | 59.4 ± 15.2 | 64.4 ± 14.8 | 54.4 ± 14.0 | 0.001 |
| BMI a | 24.3 ± 2.9 | 23.8 ± 2.9 | 24.8 ± 3.0 | 0.116 |
| Gender (%) | ||||
| Male | 99 (99%) | 49 (98%) | 50 (100%) | 0.315 |
| Female | 1 (1%) | 1 (2%) | 0 (0%) | |
| ASA b score | 2.2 ± 0.5 | 2.3 ± 0.6 | 2.0 ± 0.4 | 0.002 |
| CLASS I (%) | 5 (5%) | 2 (2%) | 3 (6%) | 0.003 |
| CLASS II (%) | 73 (60%) | 30 (60%) | 43 (86%) | |
| CLASS III (%) | 22 (100%) | 18 (36%) | 4 (8%) | |
| Comorbidities (%) | ||||
| HTN c | 44 (43%) | 30 (60%) | 14 (28%) | 0.001 |
| DM d | 14 (13%) | 9 (18%) | 5 (10%) | 0.249 |
| Cardiovascular | 15 (15%) | 10 (20%) | 5 (10%) | 0.161 |
| Pulmonary | 10 (10%) | 7 (14%) | 3 (6%) | 0.182 |
| Renal | 0 (0%) | 0 (0%) | 0 (0%) | 1 |
| Liver | 6 (6%) | 3 (6%) | 3 (6%) | 1 |
| Cerebral | 4 (4%) | 3 (6%) | 1 (2%) | 0.307 |
| Other cancer history | 10 (10%) | 6 (12%) | 4 (8%) | 0.505 |
| BPH e | 20 (20%) | 12 (24%) | 8 (16%) | 0.317 |
| Smoking | 34 (34%) | 15 (30%) | 19 (38%) | 0.398 |
| Alcohol | 42 (42%) | 20 (40%) | 22 (44%) | 0.685 |
| Steroid use | 0 (0%) | 0 (0%) | 0 (0%) | 1 |
| Variables | All (n = 100) | Laparoscopic TAPP (n = 50) | Robotic TAPP (n = 50) | p-Value |
|---|---|---|---|---|
| Operation time (minutes, mean ± SD) | 30.8 ± 11.1 | 31.5 ± 10.3 | 30.2 ± 11.9 | 0.56 |
| Conversion rate (%) (Open or Laparoscopic) | 0 (0%) | 0 (0%) | 0 (0%) | 1 |
| Cost of surgery (USD a) | 209.6 ± 27.5 | 3814.8 ± 172.9 | <0.001 | |
| Type of hernia (%) | 0.829 | |||
| Indirect only | 87 (87%) | 44 (88%) | 43 (86%) | |
| Direct only | 7 (7%) | 3 (6%) | 4 (8%) | |
| Combined direct and indirect | 3 (3%) | 1 (2%) | 2 (4%) | |
| Femoral | 1 (1%) | 0 (0%) | 1 (2%) | |
| Spigelian | 1 (1%) | 1 (2%) | 0 (0%) | |
| Hernia site (%) | 0.483 | |||
| Right | 61 (61%) | 32 (64%) | 29 (58%) | |
| Left | 31 (31%) | 13 (26%) | 18 (36%) | |
| Bilateral | 8 (8%) | 5 (10%) | 3 (6%) | |
| Previous contralateral hernia (%) | 10 (10%) | 4 (8%) | 6 (12%) | 0.505 |
| Complex hernia (%) | ||||
| Recurrent hernia | 8 (8%) | 5 (10%) | 3 (6%) | 0.461 |
| Incarceration | 9 (9%) | 4 (8%) | 5 (10%) | 0.727 |
| Prostatectomy history | 8 (8%) | 6 (12%) | 2 (4%) | 0.14 |
| Variables | All (n = 100) | Laparoscopic TAPP (n = 50) | Robotic TAPP (n = 50) | p-Value |
|---|---|---|---|---|
| Hospital stay (days, mean ± SD) | 3.4 ± 1.6 | 3.5 ± 2.2 | 3.4 ± 0.6 | 0.658 |
| VAS a score | ||||
| Operation day (0–10, mean ± SD) | 4.7 ± 1.0 | 4.6 ± 1.1 | 4.8 ± 0.9 | 0.243 |
| Postoperative 1 day (0–10, mean ± SD) | 2.7 ± 0.7 | 2.9 ± 0.5 | 2.5 ± 0.7 | 0.015 |
| Readmission within 30 days (%) | 0 (0%) | 0 (0%) | 0 (0%) | 1 |
| Hernia recurrence (%) | 1 (1%) | 1 (2%) | 0 (0%) | 0.315 |
| Postoperative outcome (%) | ||||
| Infection (Surgical site, Mesh) | 0 (0%) | 0 (0%) | 0 (0%) | 1 |
| Seroma | 2 (2%) | 2 (4%) | 0 (0%) | 0.153 |
| Hematoma | 4 (4%) | 3 (6%) | 1 (2%) | 0.307 |
| Prolonged ileus | 0 (0%) | 0 (0%) | 0 (0%) | 1 |
| Bowel obstruction | 0 (0%) | 0 (0%) | 0 (0%) | 1 |
| Bladder injury | 0 (0%) | 0 (0%) | 1 (2%) | 0.315 |
| Urinary retention | 8 (8%) | 5 (10%) | 3 (6%) | 0.461 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Choi, Y.S.; Kim, K.D.; Choi, M.S.; Heo, Y.S.; Yi, J.W.; Choe, Y.-M. Initial Experience of Robot-Assisted Transabdominal Preperitoneal (TAPP) Inguinal Hernia Repair by a Single Surgeon in South Korea. Medicina 2023, 59, 582. https://doi.org/10.3390/medicina59030582
Choi YS, Kim KD, Choi MS, Heo YS, Yi JW, Choe Y-M. Initial Experience of Robot-Assisted Transabdominal Preperitoneal (TAPP) Inguinal Hernia Repair by a Single Surgeon in South Korea. Medicina. 2023; 59(3):582. https://doi.org/10.3390/medicina59030582
Chicago/Turabian StyleChoi, Yun Suk, Kyeong Deok Kim, Moon Suk Choi, Yoon Seok Heo, Jin Wook Yi, and Yun-Mee Choe. 2023. "Initial Experience of Robot-Assisted Transabdominal Preperitoneal (TAPP) Inguinal Hernia Repair by a Single Surgeon in South Korea" Medicina 59, no. 3: 582. https://doi.org/10.3390/medicina59030582







