Highlights
What are the main findings?
- Colloidal form of silver is biologically more reactive than the ionic form.
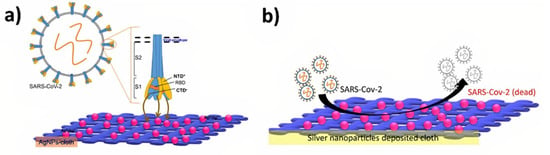
- Silver nanoparticles (AgNPs) can strongly bind to the spikes of the SARS-CoV-2 virus and prevent host cell attachment.
- Anti-viral activity of the AgNPs mainly depends on their size and structural features.
What is the implication of the main finding?
- AgNPs could be used to tackle the variants of SARS-CoV-2 virus effectively.
- Increased toxicity of AgNPs at the higher concentrations is a point of concern to be addressed.
Abstract
COVID-19 is an epizootic and life-threatening outbreak affecting millions of people globally. Coronavirus variants have emerged in different locations since their origin. Silver and its compounds, including silver nanoparticles (AgNPs), have been used in the medical field for a long period, especially in surgical treatments. The anti-microbial and anti-viral properties of silver are well documented. These properties depend on the size of the particles, concentration, precursor, method of preparation, and the presence of other benefiting compounds. Several experiments were conducted by researchers worldwide to prove the anti-bacterial and anti-viral properties of silver (Ag) and AgNPs, emphasizing that silver can be introduced to multiple organs in the human body and exhibit the expected antiviral characteristics. In this review article, use of silver nanoparticles to fight the COVID-19 pandemic according with the current information is discussed. The mechanisms involving antiviral activity and toxicity are discussed in detail. This article concludes that strong binding of AgNPs with SARS-CoV-2 virus prevents binding with the host cell, leading to the death of the virus. However, increased cytotoxic effect of the silver compounds at higher concentrations is a matter of concern.
1. Introduction
Public concerns regarding the emergence of infectious diseases are on the rise. Chronic respiratory diseases such as asthma and acute respiratory distress syndrome are long-term diseases characterized by the destruction of neutrophils or cycles of infection. The reports from 2010 show that, in India, acute respiratory diseases account for 15.9% of the total death rate in children under the age of 5 [1]. In a global scenario, 1.4 million infants (20% of mortality rate) were found to be the victims of acute lower respiratory infection (ALRI) [1,2]. In recent years, several variants of coronavirus have been imputed for the rapidly increasing severe respiratory diseases, with Severe Acute Respiratory Syndrome coronavirus (SARS-CoV) observed in 2002 and Middle East Respiratory Syndrome coronavirus (MERS CoV) observed in 2012 leading the table. The new version of SARS coronavirus, i.e., SARS-CoV-2, turned out to be more contagious and engendered a severe respiratory disease. The coronavirus disease (COVID-19) has deeply affected the world with high mortality rates [3]. As per the reports of the World Health Organization (WHO), this COVID-19 pandemic has caused more than 6.3 million deaths in the world (as of September 2022) [4] and has emerged as the most significant global health crisis after the Spanish flu pandemic of 1918 [5]. As stated by the World Health Organization (WHO), the outbreak of SARS-CoV-2 might have been initiated between mid-November and early December 2019. SARS-CoV-2 is the ninth documented coronavirus to torment human beings. Although bats, pangolins, and civets function as hosts for other coronaviruses, epidemiological and epizootic studies have revealed that there is no clear evidence of transmission of SARS-CoV-2 by the human–animal interface. SARS-CoV-2 is found in frozen food, packaging, and cold storage, indicating that the viruses’ transmission could occur between various surfaces [6].
The main reason for the transmission of coronaviruses is respiratory droplets [6,7,8]. Excrements from the infected animals and untreated wastewater are also proven to spread the infection [9]. Some studies [10,11] have demonstrated that blood plasma of SARS-CoV-2 infected people could also transmit the disease. However, these findings are not substantial [12]. Studies have also shown that the indiscretion of touching contaminated surfaces before contacting the mouth and other associated organs is the main cause of the mass transmission of viruses in a confined region [13]. Surface contamination raises concerns regarding transmission through food contamination, bioaccumulation of viruses in shellfish, and consumption of gobbets without proper cooking, even though transmission via food and water are not yet proven [14]. In an experiment conducted on a group of students, unintended touching of the nose and other facial organs was found to be an average of 23 times in an hour, which signifies the compulsory use of masks and standard clothing as a preventative measure to stop the spread of the coronavirus [15]. The lifetime of coronavirus was found to be unalike on different surfaces and under different conditions. Coronavirus was found to survive with an average of 672 h (28 days) at a temperature around 4 °C, while at higher temperatures (viz., 30 to 40 °C), the lifetime decreases to 2–9 h [16]. It was seen that, on steel surfaces, the coronavirus can survive for a period of about 120 h (5 days), whereas on aluminum surfaces, it can last for only about 2–8 h [17,18,19]. On the other materials, such as wood, paper, and glass, the coronavirus was found to survive for an average of 96 h [16]. Surfaces/materials made of metals, alloys, and metal oxides are highly effective in deactivating the coronavirus [20,21,22]. Especially, pure nanoparticles of copper [23,24,25,26], zinc [27,28,29], magnesium [30,31], and silver [32,33,34] and the corresponding oxides have proven to be highly effective against coronavirus. This article focuses on the antiviral and antimicrobial applications of silver ions and silver nanoparticles and their potential utility in tackling the life-threatening SARS-CoV-2 virus and its variants. Analysis of the impact of silver-based materials in the various facets of COVID-19 treatment is described. The different synthetic methods of AgNPs and their advantages and disadvantages are also discussed. Furthermore, toxicity profile of the AgNPs is assessed.
2. Role of Silver (Ag) in Medicine
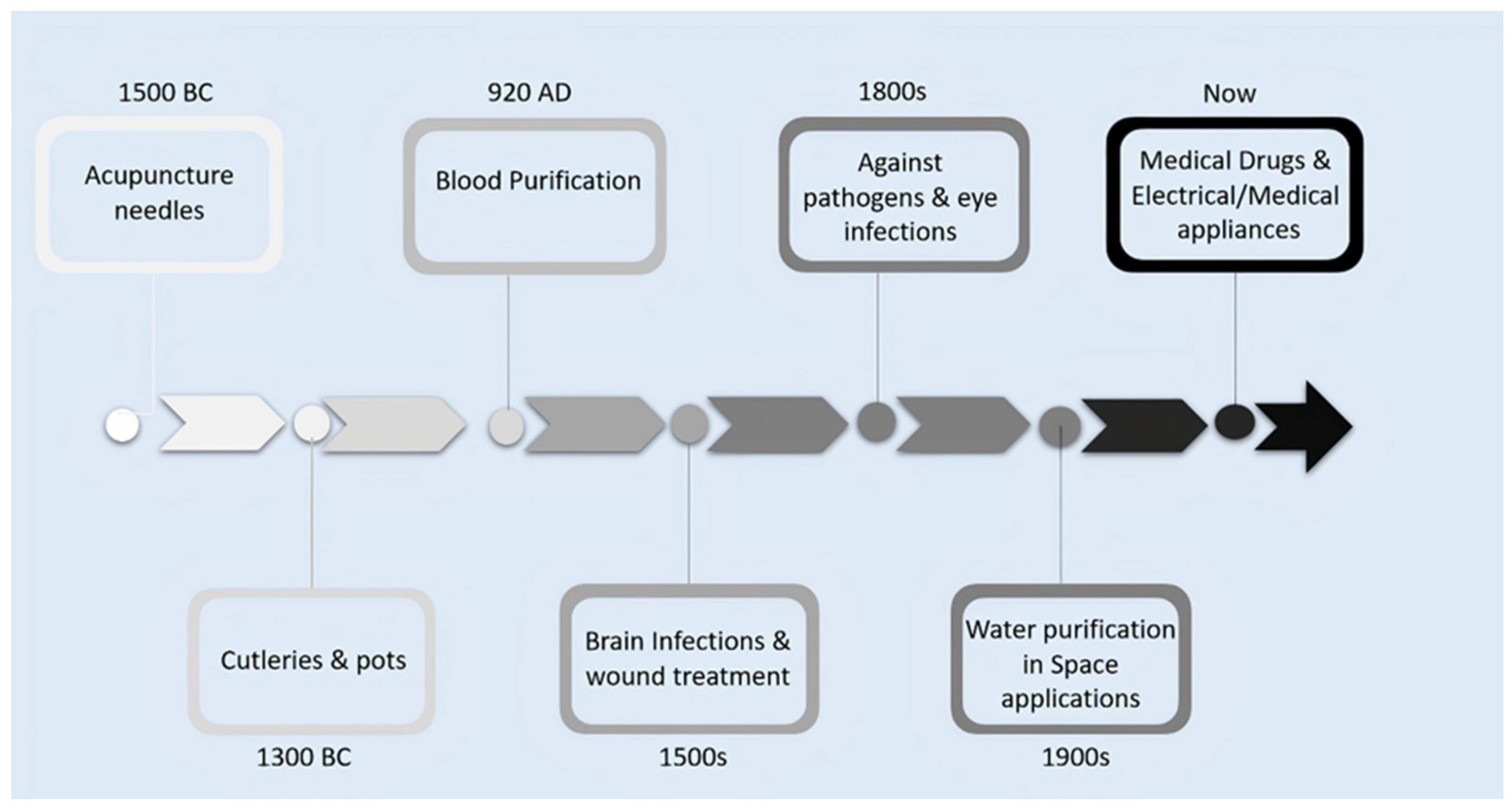
Metallic nanoparticles/compounds/oxides are widely recommended materials for the medical field (silver, titanium, copper, zinc oxide, and iron oxide) for disinfectants, cosmetics, and personal protective equipment [35]. Silver nanoparticles (AgNPs) possesses special characteristics of targeting viruses and can easily attach to viral surface glycoproteins. Then, AgNPs can enter into virus cells to exhibit virucidal activity by attacking the viral genome [36]. Silver (Ag) is one of the seven metals of antiquity known to ancient humans. Although it was established as a precious metal, its use in human healthcare and medicine can be found in prehistoric data. The term silver has been derived from an Anglo-Saxon word siolfur, which means shiny substance, and its symbol ‘Ag’ was acquired from the Latin word argentum and Sanskrit term argunas [37]. Early applications of silver were in disinfection and storage of water. Figure 1 portrays various applications of silver from prehistoric to the present period.
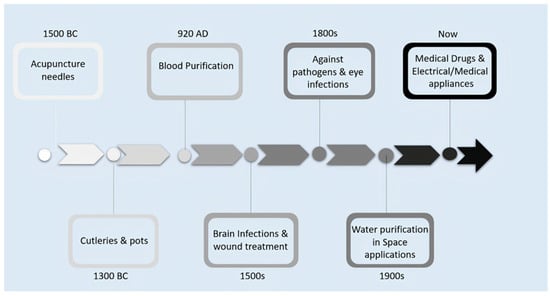
Figure 1.
Timeline of various applications of silver (Ag).
Silver has been extensively used in the medical field even before the advancements in medicine. Use of silver plates for cranioplasty [38,39], catheters [40], sutures [32,38], and silver wire for replacing fractured bones [41], and silver-coated endotracheal tubes [42] is well known. The anti-microbial property of silver is indirectly exploited in household applications and home appliances. Refrigerators and washing machines made by Samsung electronics use AgNPs, as they possess the features of fumigating and sterilizing apparel and help in the safekeeping of the machines from foreign microbes. The refrigerators manufactured by LG Electronics and Hitachi dishwashers also follow the same principles [32,38].
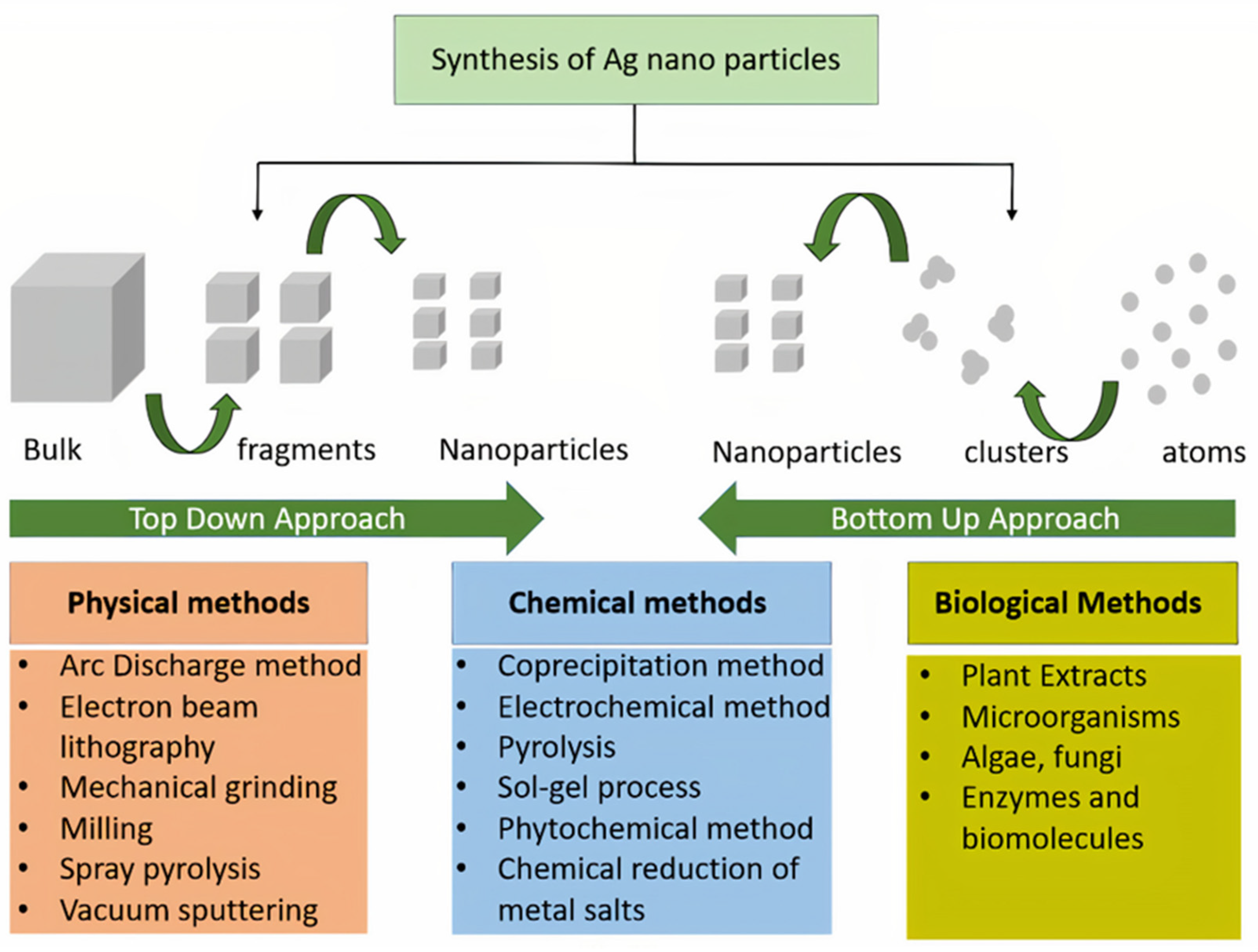
Various methods, including chemical, physical–biological, and hybrid techniques, can be adopted to manufacture nano- and micro-silver particles, as shown in Figure 2 by either a top-to-bottom or bottom-to-top approach. Physical methods of synthesis include plasma arcing [43], ball milling [44], pulsed laser deposition [45], spray pyrolysis [46], and lithographic techniques [47]. The chemical methods used to produce AgNPs are electro-deposition method, sol–gel process [48], chemical solution, chemical vapor deposition methods [49], hydrolysis co-precipitation, and wet chemical method [50]. Microwaves-assisted (frequency range 300 MHz to 300 GHz) nanoparticle synthesis from a blend of silver nitrate and carboxymethyl chitosan was also proven to be a good method for the efficient synthesis of silver nanoparticles [51]. Both physical and chemical methods produce high radiation and utilize stabilizing chemical agents that are harmful to human beings and the environment. Therefore, the biosynthetic route has gained much attention. AgNPs are manufactured with greater stability and precise dimension by biosynthetic routes, as they are made in a single step. In addition, this method provides an eco-friendly, non-toxic and safe route. Biosynthesis of AgNPs is normally achieved by treating the silver salts with plant extracts or microorganisms such as bacteria or fungi. The bio-reducing components of the plant extract polyphenols or proteins and enzymes of the microorganisms are found to play a key role in this bottom-to-top synthetic approach and serve as stabilizing agents.
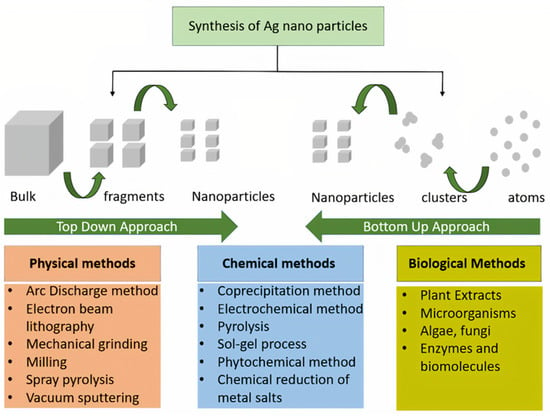
Figure 2.
Different methods of synthesizing silver nanoparticles (AgNPs).
Although silver possesses many advantages, its toxic effects cannot be neglected. A high concentration of silver in water bodies can affect the aquatic species and cause ecological imbalance [52,53]. Silver components enter the body through absorption, inhalation, and excretion. Ingestion causes the deposition of silver in the stomach and other intestinal regions, whereas inhalation deposits silver in the respiratory tract, such as the larynx trachea, and lungs [52,53,54,55]. Silver particles can induce alveolar inflammation and disrupt the heart and vascular function. Continuous inhalation of silver particles for more than 60 s can damage the lungs and cause many diseases [56]. Excessive consumption of the silver solution leads to a bluish-gray color on the skin known as Argyria [57]. The same effect that occurs in the eye is called Argyrosis. The use of silver-based creams for the treatment of wounds and burns is found to have severe side effects, such as methemoglobinemia, hypochloremia, hyponatremia, and eschars [58]. Aqueous solutions of silver compounds are known to damage various organs, including the liver and kidney, cause infections in the respiratory tract and colons, and affect platelet, white blood cells (WBCs), and red blood cells (RBCs) concentrations. Although the high antimicrobial efficacy of silver is beneficial, the lack of selectivity toward the particular strains of microbes also makes it dangerous for essential ecological bacteria [59]. Several experimental studies have validated the toxicity profile of the AgNPs. Experiments on the shrimp Penaeus monodon showed that AgNPs exhibit high anti-bacterial properties at lower concentrations along with a high survival rate. However, at higher concentrations, the toxic effect of the AgNPs becomes predominant, leading to the death of the specimen. Similar observations are made in the case of other aquatic animals and plants [60].
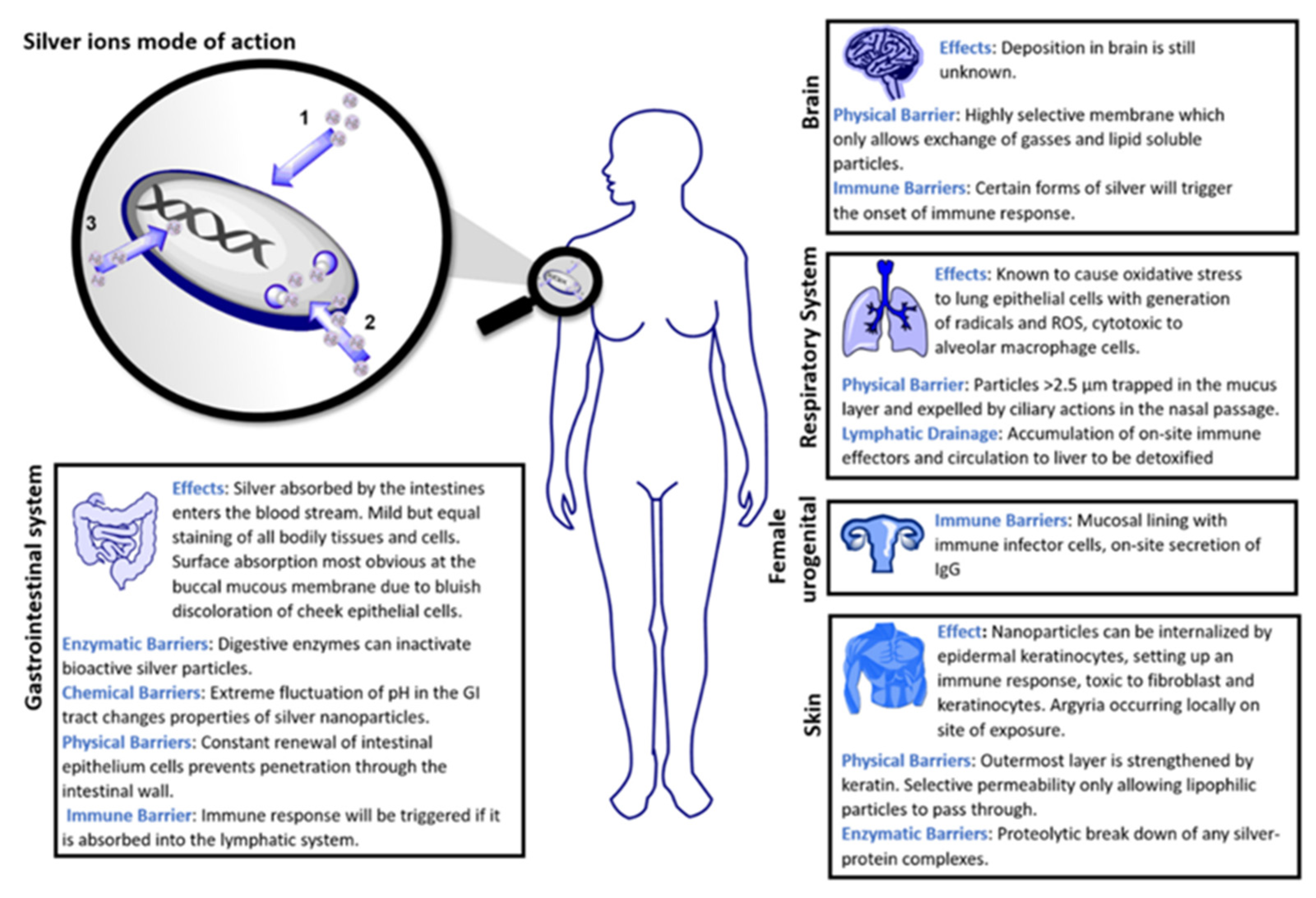
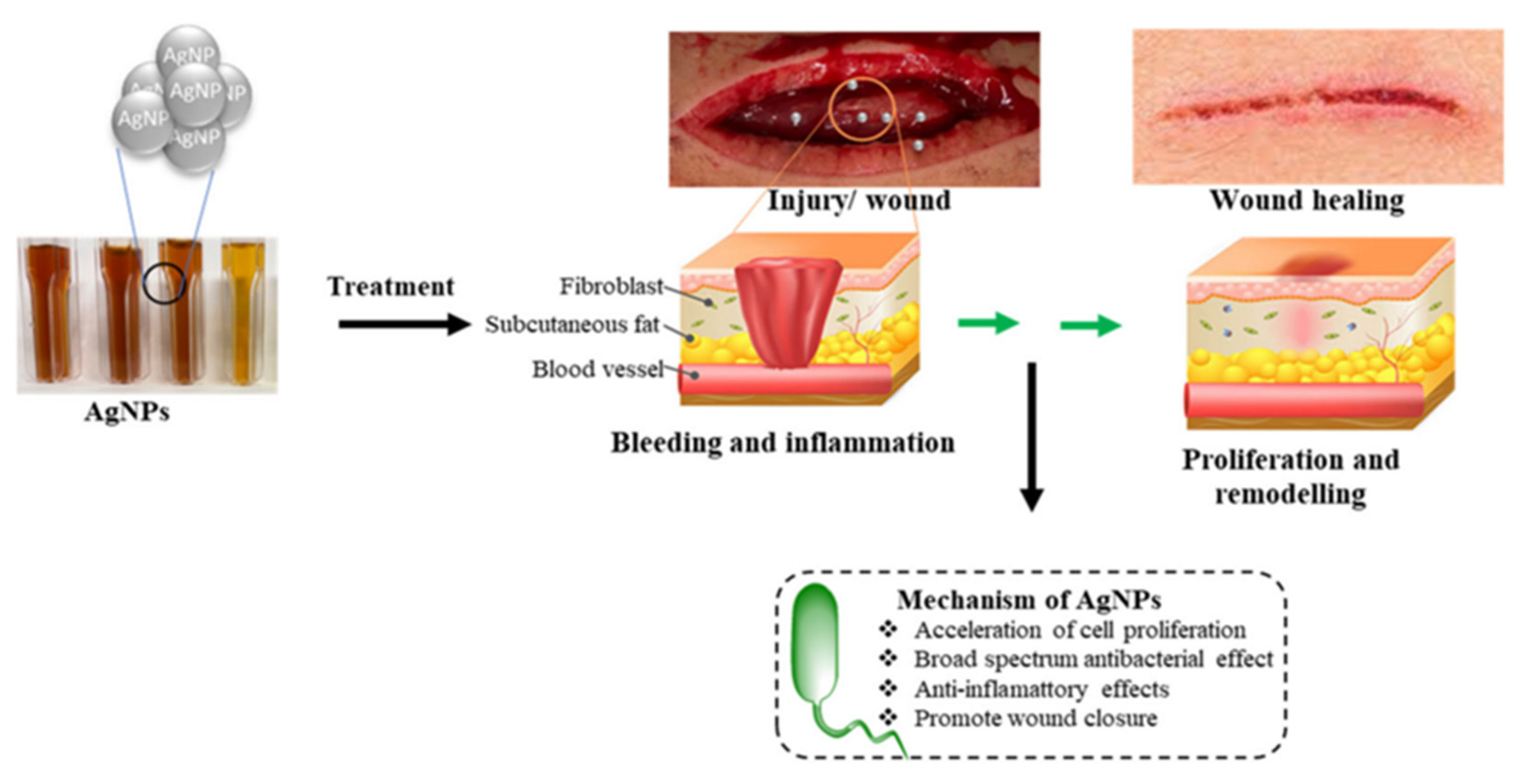
Silver (Ag) is a metal with high electrical and thermal conductivity and has been exploited to manufacture various utensils, jewelry, dental alloys, and explosives for a long time [61]. However, it also has good antimicrobial properties resulting in its ability to fight various infections [62,63,64,65,66]. Pure metallic silver is inert and usually does not interact with human tissues or microorganisms. However, in the presence of aqueous media such as wound fluid moisture, silver can readily form silver ions (i.e., Ag+) and exhibit various bio-activities [33]. The Ag+ form is found to be the active ionic form of silver, while the other possible oxidation states of silver, i.e., Ag2+, Ag3+, are unstable under regular conditions and hence, Ag2+, Ag3+ are generally not considered relevant in biological applications. Silver, being a heavy metal, exhibits oligodynamic effect and is therefore used in minimal quantities in said biological applications [67]. Studies have revealed that Ag+ ions form anionic complexes with the halide ions of the form [AgX2]−, where X could be Cl, Br, etc., and can combine with species containing nitrogen or oxygen donor groups to form stable compounds with improved bioactivity [67]. Silver nanoparticles are also known to form a colloidal solution or composite materials with the suitable polymeric matrix [68,69]. Impregnation, complexation, or blending of silver with suitable materials such as activated charcoal, phosphorous, zirconium lactate, allantoin, etc., are also found to be efficient ways of administration of silver in biological systems [70,71,72]. A trace amount of silver is found in all humans, with about 0.1 µg of silver in the blood itself. A general diet supplies about 40 µg of silver per day; however, about 99 percent of it would be readily excreted from the body. Silver in the blood level can increase to 23 μg/L when exposed to silver either as a medicine or in other forms. This absorption rate can be further increased during inflammation and cell growth [32]. Figure 3 shows the different parts of the human body where deposition of silver can occur. Although the effect of deposition of silver in the human brain is not investigated in detail, its effect on other organs such as the gastrointestinal tract, respiratory tract, skin, and genitals has been well documented [73]. Due to the divergent physical, chemical, and enzymatic barriers they encounter in the different organs and tissues of the body, silver particles can undergo drastic alterations in the structural properties and hence can exhibit unique and specific functional properties. The earlier use of silver particles for medicine has been associated with its significant burn and wound healing applications. Figure 4 shows the action of silver on the wound regions. The wound healing process of bandages containing silver particles is well understood. Diffusion of fluids from the wound triggers the release of silver ions (concentration of around 10–40 ppm) from the dressing material, and the free silver ions are found to be responsible for the observed anti-microbial action [74,75].
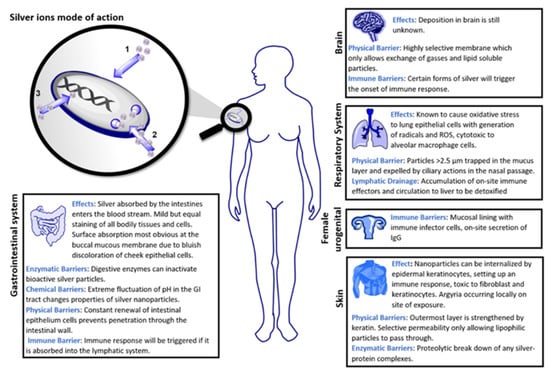
Figure 3.
Mode of action of silver ions in the human body. Reprinted from Elsevier [73]. 2022, Karthik V Shankar.
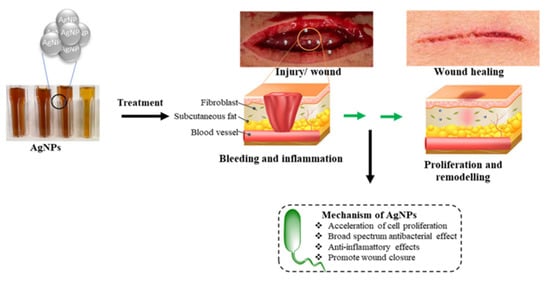
Figure 4.
Images showing the action of silver ions in wound dressing. Reprinted with permission from MDPI [76]. 2022, Karthik V Shankar.
Some studies show that silver and mercury ions hold the prime positions of all metal ions in antimicrobial action when used at concentrations less than 1 ppm in vitro [76]. These ions are absorbed into the bacterial membranes when compounded as silver sulfhydryl, which acts as a cytoplasmic poison. It was found that restrained strains of bacteria show a five-fold lower accumulation of silver as compared to the sensitive stains and produce a lower amount of hydrogen sulfide (about 33% only) [77,78]. The resistance observed in the restrained bacteria can be ascribed to the formation of intracellular protective systems. Figure 5 depicts the microbial action of silver from various devices against bacterial cells. In the sensitive bacterial strains, the silver ions are absorbed by phosphate and other electron-donating receptors on the membrane, which will then diffuse into the cell by endocytic vacuoles and phagocytosis. These silver particles inactivate membrane-related enzymes that distort the bacterial cell envelope, disrupting their ability to absorb nutrients. This also prevents the rejection of metabolic waste from the membrane, leading to pitting, which eventually becomes dangerous to bacteria. The inactivation of enzymes also prevents the replication of RNA and DNA in the cell [78]. The silver free radicals also exhibit excellent antimicrobial activity. Due to the presence of unpaired electrons, free radicals can readily react with several amino acids of cell protein such as arginine and glutamic acid and affect their regular functioning, ultimately leading to the destruction of bacterial cells [64,79,80].
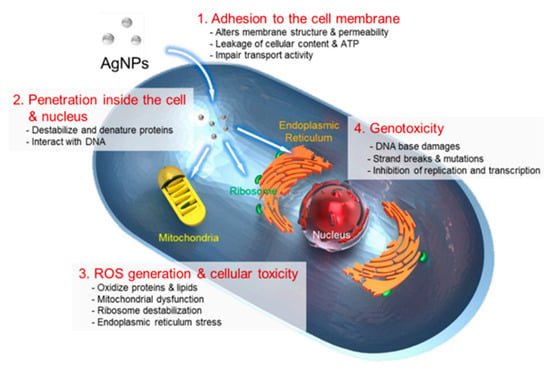
Figure 5.
Image showing the antimicrobial action of AgNPs. Reprinted with permission from MDPI [77]. 2022, Karthik V Shankar.
Nano-silver or silver nanoparticles (AgNPs) are an important form of silver with physical and chemical properties significantly different from those of normal silver particles [81]. Multiple studies have revealed that silver nanoparticles of the size range 50–100 nm exhibit a high order of anti-microbial properties [82,83]. Due to their smaller size, AgNPs can easily reach inaccessible organs and tissues and exhibit superior disinfection effects. AgNPs are found to be very effective against bacteria, fungi, leishmania, plasmodium, and neoplastic cells. AgNPs can activate the enzymes or interfere with the mitotic and meiotic stages of cell division of cancer cells and prevent their growth in various parts of the body. It is seen that in the presence of an appropriate amount of AgNPs, a vital nutrient present in acute lymphoblastic leukemia would exist in an inactive acidic form rather than in an active neutral form, which averts or slows down the growth and spreading of cancer [84]. Extensive experimental analyses conducted by Xiang et al. [85] demonstrated the potential of AgNPs against various viruses such as H1N1 Influenza A, and H3N2 Influenza. Both in vitro and in vivo results showed a significant decrease in the virus concentration and formation of lesions in the lung tissues of the test animals treated with AgNPs [86]. AgNPs were found to be useful in the treatment of genital herpes. From the detailed in vivo and in vitro studies, it was found that the AgNPs inhibit the growth and spread of the virus by boosting the virus immunological response system, which will then efficiently block the penetration of the virus into the cells and suppress inflammation [87]. Shahverdi et al. [88,89] identified that AgNPs can greatly enhance the inhibitory action of various antibiotics such as penicillin G, amoxicillin, erythromycin, clindamycin, and vancomycin against the bacteria E. coli and S. aureus. Detailed in vitro studies carried out on dengue virus (DEN-2) revealed that the mechanism of action of the prominent antiviral activity exhibited by the AgNPs originates from the effective inhibition of gene expression of the virus.
4. Conclusions
The COVID-19 outbreak that began in 2019 led to the rapid spread of the disease worldwide within a few months, resulting in an exponential death toll in most countries. Numerous variants of SARS-CoV-2 emerged during this period, including alpha, beta, gamma, and omicron, and continued with changes in the DNA sequences and mutations. The omicron variant is the current significant strain spread in various parts of the world. Several metals are identified with continuous research on metallo-medicines, and their effects on tackling diseases are established. Silver has been used in medicinal applications since ancient times. The anti-microbial properties of silver nanoparticles (AgNPs) depend on concentration, method of synthesis, size, presence of ‘helper molecules’, and various other factors. Prominent anti-viral properties of AgNPs could be utilized to tackle current variants as well as future mutants of coronavirus. Evidence collected from various experiments showed the inhibition of spikes of SARS-CoV-2 on ACE receptors when treated with AgNPs. AgNPs can also serve as a suitable drug delivery system for hydroxychloroquine and chloroquine medicines used to treat COVID-19. Administration of AgNPs via nasal or oral routes was found to help in controlling respiratory diseases. Silver-based textiles used for hospital requirements, including PPE kits and masks, are proven to limit the surface contact transmission of viruses to a great extent. Silver-based sanitizers and disinfectants have proven their high efficacy. However, high toxicity and adverse effect of AgNPs are still points of concern and should be addressed systematically. Even though extensive research and analysis are continuously being carried out with several materials for understanding their potential for tackling the pandemic, the development of superior inhibitory agents for the SARS-CoV-2 virus or its variants requires more time and effort.
Author Contributions
Conceptualization, K.V.S.; methodology, P.N.J.A. and B.S. (Bipin Sankar); software, K.V.S.; formal analysis, P.N.J.A., B.S. (Bipin Sankar) and K.V.S.; investigation, P.N.J.A., B.S. (Bipin Sankar), K.V.S. and N.V.K.; resources, P.N.J.A. and B.S. (Bipin Sankar); writing—original draft preparation, P.N.J.A., B.S. (Bipin Sankar) and K.V.S.; writing—review and editing, K.V.S., N.V.K., S.S. and B.S. (Balakrishnan Shankar); visualization, B.S. (Bipin Sankar) and P.N.J.A. supervision, N.V.K., S.S., B.S. (Balakrishnan Shankar) and K.V.S.; project administration, N.V.K., S.S., B.S. (Balakrishnan Shankar) and K.V.S.; funding acquisition, K.V.S., S.S. and N.V.K. All authors have read and agreed to the published version of the manuscript.
Funding
This research was funded by Amrita Vishwa Vidyapeetham, Amritapuri, India.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Murarkar, S.; Gothankar, J.; Doke, P.; Dhumale, G.; Pore, P.D.; Lalwani, S.; Quraishi, S.; Patil, R.S.; Waghachavare, V.; Dhobale, R. Prevalence of the acute respiratory infections and associated factors in the rural areas and urban slum areas of western Maharashtra, India: A community-based cross-sectional study. Front. Public Health 2021, 9, 723807. [Google Scholar] [CrossRef] [PubMed]
- Nair, H.; Simões, E.A.F.; Rudan, I.; Gessner, B.D.; Azziz-Baumgartner, E.; Zhang, J.S.F.; Feikin, D.R.; Mackenzie, G.A.; Moiïsi, J.C.; Roca, A. Global and regional burden of hospital admissions for severe acute lower respiratory infections in young children in 2010: A systematic analysis. Lancet 2013, 381, 1380. [Google Scholar] [CrossRef]
- Acter, T.; Uddin, N.; Das, J.; Akhter, A.; Choudhury, T.R.; Kim, S. Evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) as coronavirus disease 2019 (COVID-19) pandemic: A global health emergency. Sci. Total Environ. 2020, 730, 138996. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization Website. Available online: https://covid19.who.int/ (accessed on 25 September 2021).
- AlSamman, M.; Caggiula, A.; Ganguli, S.; Misak, M.; Pourmand, A. Non-respiratory presentations of COVID-19, a clinical review. Am. J. Emerg. Med. 2020, 38, 2444. [Google Scholar] [CrossRef] [PubMed]
- Joint WHO-China Study Team. WHO-convened global study of origins of SARS-CoV-2: China part (text extract). Infect. Dis. Immun. 2021, 1, 125. [Google Scholar]
- Jayaweera, M.; Perera, H.; Gunawardana, B.; Manatunge, J. Transmission of COVID-19 virus by droplets and aerosols: A critical review on the unresolved dichotomy. Environ. Res. 2020, 188, 109819. [Google Scholar] [CrossRef]
- Burke, R.M.; Midgley, C.M.; Dratch, A.; Fenstersheib, M.; Haupt, T.; Holshue, M.; Ghinai, I.; Jarashow, M.C.; Lo, J.; McPherson, T.D. Active monitoring of persons exposed to patients with confirmed COVID-19—United States, January–February 2020. Morb. Mortal. Wkly. Rep. 2020, 69, 245. [Google Scholar] [CrossRef]
- Guo, Y.; Korteweg, C.; McNutt, M.A.; Gu, J. Pathogenetic mechanisms of severe acute respiratory syndrome. Virus Res. 2008, 133, 4. [Google Scholar] [CrossRef]
- Wang, W.; Xu, Y.; Gao, R.; Lu, R.; Han, K.; Wu, G.; Tan, W. Detection of SARS-CoV-2 in different types of clinical specimens. JAMA 2020, 23, 1843. [Google Scholar] [CrossRef]
- Chang, L.; Zhao, L.; Gong, H.; Wang, L.; Wang, L. Severe acute respiratory syndrome coronavirus 2 RNA detected in blood donations. Emerg. Infect. Dis. 2020, 26, 1631. [Google Scholar] [CrossRef]
- Chang, L.; Yan, Y.; Wang, L. Coronavirus disease 2019: Coronaviruses and blood safety. Transfus. Med. Rev. 2020, 34, 75. [Google Scholar] [CrossRef]
- Xu, J.; Zhao, S.; Teng, T.; Abdalla, A.E.; Zhu, W.; Xie, L.; Wang, Y.; Guo, X. Systematic Comparison of Two Animal-to-Human Transmitted Human Coronaviruses: SARS-CoV-2 and SARS-CoV. Viruses 2020, 12, 244. [Google Scholar] [CrossRef]
- Thippareddi, H.; Balamurugan, S.; Patel, J.; Singh, M.; Brassard, J. Coronaviruses–Potential human threat from foodborne transmission? Lebensm Wiss Technol. 2020, 134, 110147. [Google Scholar] [CrossRef]
- Kwok, Y.L.A.; Gralton, J.; McLaws, M.L. Face touching: Un hábito frecuente que tiene implicaciones para la higiene de las manos. Am. J. Infectar. 2015, 43, 112. [Google Scholar]
- Kampf, G.; Todt, D.; Pfaender, S.; Steinmann, E. A review and analysis Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents. J. Hosp. Infect. 2020, 104, 246. [Google Scholar] [CrossRef]
- Casanova, L.M.; Jeon, S.; Rutala, W.A.; Weber, D.J.; Sobsey, M.D. Effects of air temperature and relative humidity on coronavirus survival on surfaces. Appl. Environ. Microbiol. 2010, 76, 2712. [Google Scholar] [CrossRef]
- Sizun, J.; Yu, M.W.N.; Talbot, P.J. Survival of human coronaviruses 229E and OC43 in suspension and after drying onsurfaces: A possible source ofhospital-acquired infections. J. Hosp. Infect. 2000, 46, 55. [Google Scholar] [CrossRef]
- Duan, S.-M.; Zhao, X.-S.; Wen, R.-F.; Huang, J.J.; Pi, G.-H.; Zhang, S.-X.; Sheng, J.H.; Bi, L.; Ruan, L.; Dong, X.-P.; et al. Stability of SARS coronavirus in human specimens and environment and its sensitivity to heating and UV irradiation. Biomed. Environ. Sci. 2003, 16, 246. [Google Scholar]
- Sportelli, C.N. Materials Science Help the Fight against SARS-CoV-2. Nanomaterials 2020, 10, 802. [Google Scholar] [CrossRef]
- Govind, V.; Bharadwaj, S.; Sai Ganesh, M.R.; Vishnu, J.; Shankar, K.V.; Shankar, B.; Rajesh, R. Antiviral properties of copper and its alloys to inactivate covid-19 virus: A review. Biometals 2021, 34, 1217. [Google Scholar] [CrossRef]
- Wang, L.; Hu, C.; Shao, L. The antimicrobial activity of nanoparticles: Present situation and prospects for the future. Int. J. Nanomed. 2017, 12, 1227. [Google Scholar] [CrossRef] [PubMed]
- Wijesinghe, W.; Mantilaka, M.; Ruparathna, K.A.A.; Rajapakshe, R.; Sameera, S.A.L.; Thilakarathna, M. Filler matrix interfaces of inorganic/biopolymer composites and their applications. Interfaces Part. Fibre Reinf. Compos. 2020, 1, 95–112. [Google Scholar]
- Longano, D.; Ditaranto, N.; Sabbatini, L.; Torsi, L.; Cioffi, N. Synthesis and antimicrobial activity of copper nanomaterials. In Nano-Antimicrobials; Springer: Berlin/Heidelberg, Germany, 2012; p. 85. [Google Scholar]
- Bogdanovic, U.; Vodnik, V.; Mitric, M.; Dimitrijevic, S.; Skapin, S.D.; Zunic, V.; Budimir, M.; Stoiljkovic, M. Nanomaterial with High Antimicrobial Efficacy Copper/Polyaniline Nanocomposite. ACS Appl. Mater. Interfaces 2015, 7, 1955. [Google Scholar] [CrossRef] [PubMed]
- Galúcio, J.M.P.; de Souza, S.G.B.; Vasconcelos, A.A.; Lima, A.K.O.; da Costa, K.S.; de Campos Braga, H.; Taube, P.S. Synthesis, characterization, applications, and toxicity of green synthesized nanoparticles. Curr. Pharm. Biotechnol. 2022, 23, 420. [Google Scholar] [CrossRef]
- Chiriac, V.; Stratulat, D.N.; Calin, G.; Nichitus, S.; Burlui, V.; Stadoleanu, C.; Popa, M.; Popa, I.M. Antimicrobial property of zinc based nanoparticles. In IOP Conference Series: Materials Science and Engineering; IOP Publishing: Bristol, UK, 2016; p. 12055. [Google Scholar]
- Mishra, P.K.; Mishra, H.; Ekielski, A.; Talegaonkar, S.; Vaidya, B. Zinc oxide nanoparticles: A promising nanomaterial for biomedical applications. Drug Discov. Today 2017, 22, 1825. [Google Scholar] [CrossRef] [PubMed]
- Król, A.; Pomastowski, P.; Ranska, K.; Railean-Plugaru, V.; Buszewski, B. Zinc oxide nanoparticles: Synthesis, antiseptic activity and toxicity mechanism. Adv. Colloid Interface Sci. 2017, 249, 37. [Google Scholar] [CrossRef] [PubMed]
- Vimbela, G.V.; Ngo, S.M.; Fraze, C.; Yang, L.; Stout, D.A. Antibacterial properties and toxicity from metallic nanomaterials. Int. J. Nanomed. 2017, 12, 3941. [Google Scholar] [CrossRef]
- Balraj, B.; Senthilkumar, N.; Potheher, I.V.; Arulmozhi, M. Characterization, antibacterial, anti-arthritic and in-vitro cytotoxic potentials of biosynthesized magnesium oxide nanomaterial. Mater. Sci. Eng. B 2018, 231, 121. [Google Scholar] [CrossRef]
- Lansdown, A.B.G. Silver in health care: Antimicrobial effects and safety in use. Biofunctional Text. Ski. 2006, 33, 17. [Google Scholar]
- Melayie, A.; Youngs, J.W. Silver and its application on antimicrobial agents. Expert. Opin. Ther. Pat. 2005, 15, 125. [Google Scholar] [CrossRef]
- Walker, M.; Parsons, D. The biological fate of silver ions following the use of silver-containing wound care products–a review. Int. Wound J. 2014, 11, 496. [Google Scholar] [CrossRef]
- Ratan, Z.A.; Mashrur, F.R.; Chhoan, A.P.; Shahriar, S.M.; Haidere, M.F.; Runa, N.J.; Kim, S.; Kweon, D.-H.; Hosseinzadeh, H.; Cho, J.Y. Silver nanoparticles as potential antiviral agents. Pharmaceutics 2021, 13, 2034. [Google Scholar] [CrossRef]
- Galdiero, S.; Falanga, A.; Vitiello, M.; Cantisani, M.; Marra, V.; Galdiero, M. Silver nanoparticles as potential antiviral agents. Molecules 2011, 16, 8894. [Google Scholar] [CrossRef]
- Holden, N.E. History of the Origin of the Chemical Elements and Their Discoverers; Brookhaven National Lab. (BNL): Upton, NY, USA, 2019. [Google Scholar]
- Barillo, D.J.; Marx, D.E. Silver in medicine: A brief history BC 335 to present. Burns 2014, 40, S3. [Google Scholar] [CrossRef]
- Leone, G.; Pepi, S.; Consumi, M.; Mahdizadeh, F.F.; Lamponi, S.; Magnani, A. Phosphorylated xanthan gum-Ag (I) complex as antibacterial viscosity enhancer for eye drops formulation. Carbohydr. Polym. 2021, 267, 118196. [Google Scholar] [CrossRef]
- Kremer, J.R.; Mastronarde, D.N.; McIntosh, J.R. Computer visualization of three-dimensional image data using IMOD. J. Struct. Biol. 1996, 116, 71. [Google Scholar] [CrossRef]
- Ludwigson, D.C.; Mears, D.C. Today’s prosthetic metals. J. Miner. Met. Mater. Soc. 1964, 16, 226. [Google Scholar] [CrossRef]
- Konop, M.; Damps, T.; Misicka, A.; Rudnicka, L. Certain aspects of silver and silver nanoparticles in wound care: A minireview. J. Nanomater. 2016, 2016, 7614753. [Google Scholar] [CrossRef]
- Pietro Reverberi, A.; Vocciante, M.; Salerno, M.; Ferretti, M.; Fabiano, B. Green synthesis of silver nanoparticles by low-energy wet bead milling of metal spheres. Materials 2020, 13, 63. [Google Scholar] [CrossRef]
- Zakaria, M.A.; Menazea, A.A.; Mostafa, A.M.; Al-Ashkar, E.A. Ultra-thin silver nanoparticles film prepared via pulsed laser deposition: Synthesis, characterization, and its catalytic activity on reduction of 4-nitrophenol. Surf. Interfaces 2020, 19, 100438. [Google Scholar] [CrossRef]
- Semenova, A.A.; Ivanov, V.K.; Savilov, S.V.; Goodilin, E.A. Unusual silver nanostructures prepared by aerosol spray pyrolysis. CrystEngComm 2013, 15, 7863. [Google Scholar] [CrossRef]
- Colson, P.; Henrist, C.; Cloots, R. Nanosphere lithography: A powerful method for the controlled manufacturing of nanomaterials. J. Nanomater. 2013, 2013, 948510. [Google Scholar] [CrossRef]
- Rivero, P.J.; Urrutia, A.; Goicoechea, J.; Zamarreño, C.R.; Arregui, F.J.; Matías, I.R. An antibacterial coating based on a polymer/sol-gel hybrid matrix loaded with silver nanoparticles. Nanoscale Res. Lett. 2011, 6, 1. [Google Scholar] [CrossRef] [PubMed]
- Nasretdinova, G.R.; Fazleeva, R.R.; Mukhitova, R.K.; Nizameev, I.R.; Kadirov, M.K.; Ziganshina, A.Y.; Yanilkin, V.V. Electrochemical mediated synthesis of silver nanoparticles in solution. Russ. J. Electrochem. 2015, 51, 1029. [Google Scholar] [CrossRef]
- Raza, S. Shape-Dependent Antibacterial Studies of Silver Nanoparticles Synthesized by Wet Chemical Routes. Nanomaterials 2016, 6, 74. [Google Scholar] [CrossRef]
- Borase, H.P.; Salunke, B.K.; Salunkhe, R.B.; Patil, C.D.; Hallsworth, J.E.; Kim, B.S.; Patil, S.V. Plant extract: A promising biomatrix for ecofriendly, controlled synthesis of silver nanoparticles. Appl. Biochem. Biotechnol. 2014, 173, 1. [Google Scholar] [CrossRef]
- Maya, F.; Muhl, S.; Peña, O.; Miki-Yoshida, M. Synthesis and characterization of silver–carbon nanoparticles produced by high-current pulsed arc. Thin Solid Films 2009, 518, 1484. [Google Scholar] [CrossRef]
- Ratte, H.T. Bioaccumulation and toxicity of silver compounds: A review. Environ. Toxicol. Chem. Int. J. 1999, 18, 89. [Google Scholar] [CrossRef]
- Hollinger, M.A. Toxicological aspects of topical silver pharmaceuticals. Crit. Rev. Toxicol. 1996, 26, 255.2. [Google Scholar] [CrossRef]
- Parveen, K.; Banse, V.; Ledwani, L. Green synthesis of nanoparticles: Their advantages and disadvantages. In AIP Conference Proceedings; AIP Publishing LLC: Bristol, UK, 2016; p. 20048. [Google Scholar]
- Hayat, M.; Uzair, M.; Ali Syed, R.; Arshad, M.; Bashir, S. Status of COVID-19 vaccination around South Asia. Hum. Vaccin. Immunother. 2022, 18, 2016010. [Google Scholar] [CrossRef]
- Marshall, J.P.; Schneider, R.P. Systemic argyria secondary to topical silver nitrate. Arch. Dermatol. 1977, 113, 1077. [Google Scholar] [CrossRef]
- Fung, M.C.; Bowen, D.L. Silver products for medical indications: Risk-benefit assessment. J. Toxicol. Clin. Toxicol. 1996, 34, 119. [Google Scholar] [CrossRef]
- Tashi, T.; Gupta, N.V.; Mbuya, V.B. Silver nanoparticles: Synthesis, mechanism of antimicrobial action, characterization, medical applications, and toxicity effects. J. Chem. Pharm. Res. 2016, 8, 526. [Google Scholar]
- Griffitt, R.J.; Luo, J.; Gao, J.; Bonzongo, J.; Barber, D.S. Effects of particle composition and species on toxicity of metallic nanomaterials in aquatic organisms. Environ. Toxicol. Chem. Int. J. 2008, 27, 1972. [Google Scholar] [CrossRef]
- Rezvani, E.; Rafferty, A.; McGuinness, C.; Kennedy, J. Adverse effects of nanosilver on human health and the environment. Acta Biomater. 2019, 94, 145. [Google Scholar] [CrossRef]
- Ayrault, S.; Priadi, C.R.; Evrard, O.; Lefèvre, I.; Bonté, P. Silver and thallium historical trends in the Seine River basin. J. Environ. Monit. 2010, 12, 2177. [Google Scholar] [CrossRef]
- Rai, M.; Agarkar, G. Plant–fungal interactions: What triggers the fungi to switch among lifestyles? Crit. Rev. Microbiol. 2016, 42, 428. [Google Scholar] [CrossRef]
- Furno, F.; Morley, K.S.; Wong, B.; Sharp, B.L.; Arnold, P.L.; Howdle, S.M.; Bayston, R.; Brown, P.D.; Winship, P.D.; Reid, H.J. Silver nanoparticles and polymeric medical devices: A new approach to prevention of infection? J. Antimicrob. Chemother. 2004, 54, 1019. [Google Scholar] [CrossRef]
- Maillard, J.-Y.; Hartemann, P. Silver as an antimicrobial: Facts and gaps in knowledge. Crit. Rev. Microbiol. 2013, 39, 373. [Google Scholar] [CrossRef]
- Chernousova, S.; Epple, M. Silver as antibacterial agent: Ion, nanoparticle, and metal. Angew. Chem. Int. Ed. 2013, 52, 1636–1653. [Google Scholar] [CrossRef]
- Marx, D.E.; Barillo, D.J. Silver in medicine: The basic science. Burns 2014, 40 (Suppl. S1), S9–S18. [Google Scholar] [CrossRef] [PubMed]
- Damm, C.; Münstedt, H.; Rösch, A. The antimicrobial efficacy of polyamide 6/silver-nano-and microcomposites. Mater. Chem. Phys. 2008, 108, 61. [Google Scholar] [CrossRef]
- Anastasiadis, S.H.; Chrissopoulou, K.; Frick, B. Structure and dynamics in polymer/layered silicate nanocomposites. Mater. Sci. Eng. B 2008, 152, 33. [Google Scholar] [CrossRef]
- Chen, M.; Wang, M.-Y.; Han, J.-T.; Zhang, J.-Y.; Li, Z.-Y.; Qian, D.-J. Preparation and study of polyacryamide-stabilized silver nanoparticles through a one-pot process. J. Phys. Chem. B 2006, 110, 11224. [Google Scholar] [CrossRef] [PubMed]
- Rong, C.; Chen, Y.; Chen, C.; Hu, L.; Wang, H.; Li, Y. Toward simultaneous compatibilization and nucleation of fully biodegradabe nanocomposites: Effect of nanorod-assisted interfacial stereocomplex crystals in immiscible polymer blends. Compos. Part B Eng. 2022, 234, 109708. [Google Scholar] [CrossRef]
- Bragg, P.D.; Rainnie, D.J. The effect of silver ions on the respiratory chain of Escherichia coli. Can. J. Microbiol. 1974, 20, 883. [Google Scholar] [CrossRef]
- Kędziora, A.; Speruda, M.; Krzyżewska, E.; Rybka, J.; Łukowiak, A.; Bugla-Płoskońska, G. Similarities and differences between silver ions and silver in nanoforms as antibacterial agents. Int. J. Mol. Sci. 2018, 19, 444. [Google Scholar] [CrossRef]
- Möhler, J.S.; Sim, W.; Blaskovich, M.A.T.; Cooper, M.A.; Ziora, Z.M. Silver bullets: A new lustre on an old antimicrobial agent. Biotechnol. Adv. 2018, 36, 1391. [Google Scholar] [CrossRef]
- Lansdown, A.B.G.; Williams, A. How safe is silver in wound care? J. Wound Care 2004, 13, 131. [Google Scholar] [CrossRef]
- Lansdown, A.B.G.; Williams, A.; Chandler, S.; Benfield, S. Silver absorption and antibacterial efficacy of silver dressings. J. Wound Care 2005, 14, 155–160. [Google Scholar] [CrossRef]
- Nqakala, Z.B.; Sibuyi, N.R.S.; Fadaka, A.O.; Meyer, M.; Onani, M.O.; Madiehe, A.M. Advances in nanotechnology towards development of silver nanoparticle-based wound-healing agents. Int. J. Mol. Sci. 2021, 22, 11272. [Google Scholar] [CrossRef]
- Lee, S.H.; Jun, B.-H. Silver nanoparticles: Synthesis and application for nanomedicine. Int. J. Mol. Sci. 2019, 20, 865. [Google Scholar] [CrossRef]
- Lansdown, A.B.G. A review of the use of silver in wound care: Facts and fallacies. Br. J. Nurs. 2004, 13, S6. [Google Scholar] [CrossRef]
- Zhao, G.J.; Stevens, S.E. Multiple parameters for the comprehensive evaluation of the susceptibility of Escherichia coli to the silver ion. Biometals 1998, 11, 27–32. [Google Scholar] [CrossRef]
- Spacciapoli, P.; Buxton, D.; Rothstein, D.; Friden, P. Antimicrobial activity of silver nitrate against periodontal pathogens. J. Periodontal Res. 2001, 36, 108. [Google Scholar] [CrossRef]
- Teirumnieks, E.; Balchev, I.; Ghalot, R.S.; Lazov, L. Antibacterial and anti-viral effects of silver nanoparticles in medicine against COVID-19—A review. Laser Phys. 2020, 31, 13001. [Google Scholar] [CrossRef]
- Nazeruddin, G.M.; Prasad, N.R.; Prasad, S.R.; Shaikh, Y.I.; Waghmare, S.R.; Adhyapak, P. Coriandrum sativum seed extract assisted in situ green synthesis of silver nanoparticle and its anti-microbial activity. Ind. Crops Prod. 2014, 60, 212. [Google Scholar] [CrossRef]
- Mpenyana-Monyatsi, L.; Mthombeni, N.H.; Onyango, M.S.; Momba, M.N.B. Cost-effective filter materials coated with silver nanoparticles for the removal of pathogenic bacteria in groundwater. Int. J. Environ. Res. Public Health 2012, 9, 244. [Google Scholar] [CrossRef]
- Ahmadi, S. The importance of silver nanoparticles in human life. Adv. Appl. NanoBio-Technol. 2020, 1, 5. [Google Scholar]
- Xiang, D.; Zheng, Y.; Duan, W.; Li, X.; Yin, J.; Shigdar, S.; O’Connor, M.L.; Marappan, M.; Zhao, X.; Miao, Y. Inhibition of A/Human/Hubei/3/2005 (H3N2) influenza virus infection by silver nanoparticles in vitro and in vivo. Int. J. Nanomed. 2013, 8, 4103. [Google Scholar]
- Siadati, S.A.; Afzali, M.; Sayyadi, M. Could silver nano-particles control the 2019-nCoV virus?; An urgent glance to the past. Chem. Rev. Lett. 2020, 3, 9. [Google Scholar]
- Behbudi, G. Effect of silver nanoparticles disinfectant on covid-19. Adv. Appl. NanoBio-Technol. 2021, 2, 63. [Google Scholar]
- Shahverdi, A.R.; Fakhimi, A.; Shahverdi, H.R.; Minaian, S. Synthesis and effect of silver nanoparticles on the antibacterial activity of different antibiotics against Staphylococcus aureus and Escherichia coli, Nanomedicine Nanotechnology. Biol. Med. 2007, 3, 168. [Google Scholar]
- Fisman, D.N.; Tuite, A.R. Evaluation of the relative virulence of novel SARS-CoV-2 variants: A retrospective cohort study in Ontario, Canada. Cmaj 2021, 193, E1619. [Google Scholar] [CrossRef] [PubMed]
- Sokhansanj, B.A.; Zhao, Z.; Rosen, G.L. Interpretable and predictive deep modeling of the SARS-CoV-2 spike protein sequence. medRxiv 2021. [Google Scholar] [CrossRef]
- Caputo, V.; Calvino, G.; Strafella, C.; Termine, A.; Fabrizio, C.; Trastulli, G.; Ingrascì, A.; Peconi, C.; Bardini, S.; Rossini, A. Tracking the Initial Diffusion of SARS-CoV-2 Omicron Variant in Italy by RT-PCR and Comparison with Alpha and Delta Variants Spreading. Diagnostics 2022, 12, 467. [Google Scholar] [CrossRef]
- Boshier, F.A.T.; Venturini, C.; Stirrup, O.; Guerra-Assunção, J.A.; Alcolea-Medina, A.; Becket, A.H.; Byott, M.; Charalampous, T.; da Silva Filipe, A.; Frampton, D. The Alpha variant was not associated with excess nosocomial SARS-CoV-2 infection in a multi-centre UK hospital study. J. Infect. 2021, 83, 693. [Google Scholar] [CrossRef]
- Brejová, B.; Hodorová, V.; Boršová, K.; Čabanová, V.; Szemes, T.; Mišík, M.; Klempa, B.; Nosek, J.; Vinař, T. Sequencing SARS-CoV-2 in Slovakia: An Unofficial Genomic Surveillance Report. medRxiv 2021. [Google Scholar] [CrossRef]
- Salleh, M.Z.; Derrick, J.P.; Deris, Z.Z. Structural evaluation of the spike glycoprotein variants on SARS-CoV-2 transmission and immune evasion. Int. J. Mol. Sci. 2021, 22, 7425. [Google Scholar] [CrossRef]
- Islam, S.; Islam, T.; Islam, M.R. New coronavirus variants are creating more challenges to global healthcare system: A brief report on the current knowledge. Clin. Pathol. 2022, 15, 2632010X221075584. [Google Scholar] [CrossRef]
- Nangunoori, S.; Appavu, R.; Kethar, J. The Connection between COVID-19 Variants (Gamma and Delta Variant) and Demographics Using Python. J. Stud. Res. 2021, 10, 1. [Google Scholar] [CrossRef]
- CDC COVID-19 Vaccine Breakthrough Case Investigations Team; Birhane, M.; Bressler, S.; Chang, G.; Clark, T.; Dorough, L.; Fischer, M.; Watkins, L.F.; Goldstein, J.M.; Kugeler, K.; et al. COVID-19 vaccine breakthrough infections reported to CDC—United States, January 1–April 30, 2021. Morb. Mortal. Wkly. Rep. 2021, 70, 792. [Google Scholar]
- Johnsen, U.; Sutter, J.; Schulz, A.; Tästensen, J.; Schönheit, P. XacR—A novel transcriptional regulator of D-xylose and L-arabinose catabolism in the haloarchaeon H aloferax volcanii. Environ. Microbiol. 2015, 17, 1663. [Google Scholar] [CrossRef]
- Maggi, F.; Novazzi, F.; Genoni, A.; Baj, A.; Spezia, P.G.; Focosi, D.; Zago, C.; Colombo, A.; Cassani, G.; Pasciuta, R. Imported SARS-CoV-2 variant P. 1 in traveler returning from Brazil to Italy. Emerg. Infect. Dis. 2021, 27, 1249. [Google Scholar] [CrossRef]
- Carroll, T.; Fox, D.; van Doremalen, N.; Ball, E.; Morris, M.K.; Sotomayor-Gonzalez, A.; Servellita, V.; Rustagi, A.; Yinda, C.K.; Fritts, L. The B. 1.427/1.429 (epsilon) SARS-CoV-2 variants are more virulent than ancestral B. 1 (614G) in Syrian hamsters. PLoS Pathog. 2022, 18, e1009914. [Google Scholar] [CrossRef]
- Abrignani, M.G.; Murrone, A.; De Luca, L.; Roncon, L.; Di Lenarda, A.; Valente, S.; Caldarola, P.; Riccio, C.; Oliva, F.; Gulizia, M.M. COVID-19, Vaccines, and Thrombotic Events: A Narrative Review. J. Clin. Med. 2022, 11, 948. [Google Scholar] [CrossRef]
- Vaughan, A. Omicron emerges. New Sci. 2021, 252, 7. [Google Scholar] [CrossRef]
- Thakur, S.; Sasi, S.; Pillai, S.G.; Nag, A.; Shukla, D.; Singhal, R.; Phalke, S.; Velu, G.S.K. SARS-CoV-2 Mutations and Their Impact on Diagnostics, Therapeutics and Vaccines. Front. Med. 2022, 9, 815389. [Google Scholar] [CrossRef]
- Choi, J.Y.; Smith, D.M. SARS-CoV-2 variants of concern. Yonsei Med. J. 2021, 62, 961. [Google Scholar] [CrossRef]
- Torjesen, I. Covid-19: Omicron may be more transmissible than other variants and partly resistant to existing vaccines, scientists fear. BMJ 2021, 29, n2943. [Google Scholar] [CrossRef]
- Khandia, R.; Singhal, S.; Alqahtani, T.; Kamal, M.A.; Nahed, A.; Nainu, F.; Desingu, P.A.; Dhama, K. Emergence of SARS-CoV-2 Omicron (B. 1.1. 529) variant, salient features, high global health concerns and strategies to counter it amid ongoing COVID-19 pandemic. Environ. Res. 2022, 209, 112816. [Google Scholar] [CrossRef] [PubMed]
- Kannan, S.R.; Spratt, A.N.; Sharma, K.; Chand, H.S.; Byrareddy, S.N.; Singh, K. Omicron SARS-CoV-2 variant: Unique features and their impact on pre-existing antibodies. J. Autoimmun 2022, 126, 102779. [Google Scholar] [CrossRef] [PubMed]
- Twohig, K.A.; Nyberg, T.; Zaidi, A.; Thelwall, S.; Sinnathamby, M.A.; Aliabadi, S.; Seaman, S.R.; Harris, R.J.; Hope, R.; Lopez-Bernal, J. Hospital admission and emergency care attendance risk for SARS-CoV-2 delta (B. 1.617. 2) compared with alpha (B. 1.1. 7) variants of concern: A cohort study. Lancet Infect. Dis. 2022, 22, 35. [Google Scholar] [CrossRef]
- Saxena, S.K.; Kumar, S.; Ansari, S.; Paweska, J.T.; Maurya, V.K.; Tripathi, A.K.; Abdel-Moneim, A.S. Characterization of the novel SARS-CoV-2 Omicron (B. 1.1. 529) variant of concern and its global perspective. J. Med. Virol. 2022, 94, 1738. [Google Scholar] [CrossRef] [PubMed]
- Teo, S.P. Review of COVID-19 mRNA vaccines: BNT162b2 and mRNA-1273. J. Pharm. Pract. 2021, 12, 08971900211009650. [Google Scholar] [CrossRef]
- Oliver, S.E.; Wallace, M.; See, I.; Mbaeyi, S.; Godfrey, M.; Hadler, S.C.; Jatlaoui, T.C.; Twentyman, E.; Hughes, M.M.; Rao, A.K. Use of the Janssen (Johnson & Johnson) COVID-19 Vaccine: Updated Interim Recommendations from the Advisory Committee on Immunization Practices—United States, December 2021. Morb. Mortal. Wkly. Rep. 2022, 71, 90. [Google Scholar]
- Voysey, M.; Clemens, S.A.C.; Madhi, S.A.; Weckx, L.Y.; Folegatti, P.M.; Aley, P.K.; Angus, B.; Baillie, V.L.; Barnabas, S.L.; Bhorat, Q.E. Safety and efficacy of the ChAdOx1 nCoV-19 vaccine (AZD1222) against SARS-CoV-2: An interim analysis of four randomised controlled trials in Brazil, South Africa, and the UK. Lancet 2021, 397, 99. [Google Scholar] [CrossRef]
- Baraniuk, C. What do we know about China’s covid-19 vaccines? BMJ 2021, 373, n912. [Google Scholar] [CrossRef]
- Lawton, G. Sputnik V vaccine goes global. New Sci. 2021, 250, 10. [Google Scholar] [CrossRef]
- Knoll, M.D.; Wonodi, C. Oxford–AstraZeneca COVID-19 vaccine efficacy. Lancet 2021, 397, 72. [Google Scholar] [CrossRef]
- Das, C.; Paul, S.S.; Saha, A.; Singh, T.; Saha, A.; Im, J.; Biswas, G. Silver-based nanomaterials as therapeutic agents against coronaviruses: A review. Int. J. Nanomed. 2020, 15, 9301. [Google Scholar] [CrossRef]
- Bahrami, A.; Arabestani, M.R.; Taheri, M.; Farmany, A.; Norozzadeh, F.; Hosseini, S.M.; Nozari, H.; Nouri, F. Exploring the role of heavy metals and their derivatives on the pathophysiology of COVID-19. Biol. Trace Elem. Res. 2022, 200, 2639. [Google Scholar] [CrossRef]
- Crane, M.J.; Devine, S.; Jamieson, A.M. Graphene oxide/silver nanoparticle ink formulations rapidly inhibit influenza A virus and OC43 coronavirus infection in vitro. bioRxiv 2021. [Google Scholar] [CrossRef]
- Zachar, O. Nanomedicine formulations for respiratory infections by inhalation delivery: COVID-19 and beyond. Med. Hypotheses 2022, 159, 110753. [Google Scholar] [CrossRef]
- Jeremiah, S.S.; Miyakawa, K.; Morita, T.; Yamaoka, Y.; Ryo, A. Potent antiviral effect of silver nanoparticles on SARS-CoV-2. Biochem. Biophys. Res. Commun. 2020, 533, 195. [Google Scholar] [CrossRef]
- Campos, E.V.R.; Pereira, A.E.S.; De Oliveira, J.L.; Carvalho, L.B.; Guilger-Casagrande, M.; De Lima, R.; Fraceto, L.F. How can nanotechnology help to combat COVID-19? Opportunities and urgent need. J. Nanobiotechnol. 2020, 18, 1. [Google Scholar] [CrossRef]
- Bui, T.Q.; Loan, H.T.P.; My, T.T.A.; Quang, D.T.; Thuy, B.T.P.; Nhan, V.D.; Quy, P.T.; Van Tat, P.; Dao, N.D.Q.; Trung, T. A density functional theory study on silver and bis-silver complexes with lighter tetrylene: Are silver and bis-silver carbenes candidates for SARS-CoV-2 inhibition? Insight from molecular docking simulation. RSC Adv. 2020, 10, 30961. [Google Scholar] [CrossRef]
- Rezaee, P.; Akbari, M.; Morad, R.; Koochaki, A.; Maaz, M.; Jamshidi, Z. First principle simulation of coated hydroxychloroquine on Ag, Au and Pt nanoparticle as a potential candidate for treatment of SARS-CoV-2 (COVID-19). arXiv 2020, arXiv:2006.02343. [Google Scholar]
- Ghaffari, M.; Mollazadeh-Bajestani, M.; Moztarzadeh, F.; Uludağ, H.; Hardy, J.G.; Mozafari, M. An overview of the use of biomaterials, nanotechnology, and stem cells for detection and treatment of COVID-19: Towards a framework to address future global pandemics. Emergent Mater. 2021, 4, 19. [Google Scholar] [CrossRef]
- Ibrahim Fouad, G. A proposed insight into the anti-viral potential of metallic nanoparticles against novel coronavirus disease-19 (COVID-19). Bull. Natl. Res. Cent. 2021, 45, 36. [Google Scholar] [CrossRef]
- Nakano, R.; Ishiguro, H.; Yao, Y.; Kajioka, J.; Fujishima, A.; Sunada, K.; Minoshima, M.; Hashimoto, K.; Kubota, Y. Photocatalytic inactivation of influenza virus by titanium dioxide thin film. Photochem. Photobiol. Sci. 2012, 11, 1293. [Google Scholar] [CrossRef] [PubMed]
- Al-Sanea, M.M.; Abelyan, N.; Abdelgawad, M.A.; Musa, A.; Ghoneim, M.M.; Al-Warhi, T.; Aljaeed, N.; Alotaibi, O.J.; Alnusaire, T.S.; Abdelwahab, S.F. Strawberry and ginger silver nanoparticles as potential inhibitors for SARS-CoV-2 assisted by in silico modeling and metabolic profiling. Antibioticse 2021, 10, 824. [Google Scholar] [CrossRef] [PubMed]
- Allawadhi, P.; Singh, V.; Khurana, A.; Khurana, I.; Allwadhi, S.; Kumar, P.; Banothu, A.K.; Thalugula, S.; Barani, P.J.; Naik, R.R. Silver nanoparticle based multifunctional approach for combating COVID-19. Sens. Int. 2021, 2, 100101. [Google Scholar] [CrossRef] [PubMed]
- Wijnhoven, S.W.P.; Peijnenburg, W.J.G.M.; Herberts, C.A.; Hagens, W.I.; Oomen, A.G.; Heugens, E.H.W.; Roszek, B.; Bisschops, J.; Gosens, I.; Van De Meent, D. Nano-silver–a review of available data and knowledge gaps in human and environmental risk assessment. Nanotoxicology 2009, 3, 109. [Google Scholar] [CrossRef]
- Pilaquinga, F.; Morey, J.; Torres, M.; Seqqat, R.; de las Nieves Pina, M. Silver nanoparticles as a potential treatment against SARS-CoV-2: A review. Wiley Interdiscip. Rev. Nanomed. Nanobiotechnol. 2021, 13, e1707. [Google Scholar] [CrossRef]
- Zachar, O. Formulations for COVID-19 earlystage treatment via silver nanoparticles inhalation delivery at home and hospital. Sci. Prepr. 2020. [Google Scholar] [CrossRef]
- Dong, Y.; Zhu, H.; Shen, Y.; Zhang, W.; Zhang, L. Antibacterial activity of silver nanoparticles of different particle size against Vibrio Natriegens. PLoS ONE 2019, 14, e0222322. [Google Scholar] [CrossRef]
- Campbell, S.; Rein, A. In vitro assembly properties of human immunodeficiency virus type 1 Gag protein lacking the p6 domain. J. Virol. 1999, 73, 2270. [Google Scholar] [CrossRef]
- Swann, H.; Sharma, A.; Preece, B.; Peterson, C.A.; Eldredge, A.; Belnap, D.M.; Vershinin, M.; Saffarian, S. Minimal system for assembly of SARS-CoV-2 virus like particles. Sci. Rep. 2021, 11, 21877. [Google Scholar] [CrossRef]
- Abd Ellah, N.H.; Gad, S.F.; Muhammad, K.; Batiha, G.E.; Hetta, H.F. Nanomedicine as a promising approach for diagnosis, treatment and prophylaxis against COVID-19. Nanomedicine 2020, 15, 2085. [Google Scholar] [CrossRef]
- Vishnuvarthanan, M.; Rajeswari, N. Food packaging: Pectin–laponite–Ag nanoparticle bionanocomposite coated on polypropylene shows low O2 transmission, low Ag migration and high antimicrobial activity. Environ. Chem. Lett. 2019, 17, 439–445. [Google Scholar] [CrossRef]
- Kumar, A.; Nath, K.; Parekh, Y.; Enayathullah, M.G.; Bokara, K.K.; Sinhamahapatra, A. Antimicrobial silver nanoparticle-photodeposited fabrics for SARS-CoV-2 destruction. Colloid Interface Sci. Commun. 2021, 45, 100542. [Google Scholar] [CrossRef]
- Gulati, R.; Sharma, S.; Sharma, R.K. Antimicrobial textile: Recent developments and functional perspective. Polym. Bull. 2021, 79, 5747–5771. [Google Scholar] [CrossRef]
- Hewawaduge, C.; Senevirathne, A.; Jawalagatti, V.; Kim, J.W.; Lee, J.H. Copper-impregnated three-layer mask efficiently inactivates SARS-CoV2. Environ. Res. 2021, 196, 110947. [Google Scholar] [CrossRef]
- Balagna, C.; Perero, S.; Percivalle, E.; Nepita, E.V.; Ferraris, M. Virucidal effect against coronavirus SARS-CoV-2 of a silver nanocluster/silica composite sputtered coating. Open Ceram. 2020, 1, 100006. [Google Scholar] [CrossRef]
- Almanza-Reyes, H.; Moreno, S.; Plascencia-López, I.; Alvarado-Vera, M.; Patrón-Romero, L.; Borrego, B.; Reyes-Escamilla, A.; Valencia-Manzo, D.; Brun, A.; Pestryakov, A. Evaluation of silver nanoparticles for the prevention of SARS-CoV-2 infection in health workers: In vitro and in vivo. PLoS ONE 2021, 16, 0256401. [Google Scholar] [CrossRef]
- Tabrez, S.; Jabir, N.R.; Adhami, V.M.; Khan, M.I.; Moulay, M.; Kamal, M.A.; Mukhtar, H. Nano-encapsulated dietary polyphenols for cancer prevention and treatment: Successes and challenges. Nanomedicine 2020, 15, 1147. [Google Scholar]
- Vickers, N.J. Animal communication: When i’m calling you, will you answer too? Curr. Biol. 2017, 27, R713. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).