Plant-Derived Alkaloids as a Potential Source of Treatment for Colorectal Cancer over the Past Five Years: A Comprehensive Review
Abstract
1. Introduction
2. Results and Discussion
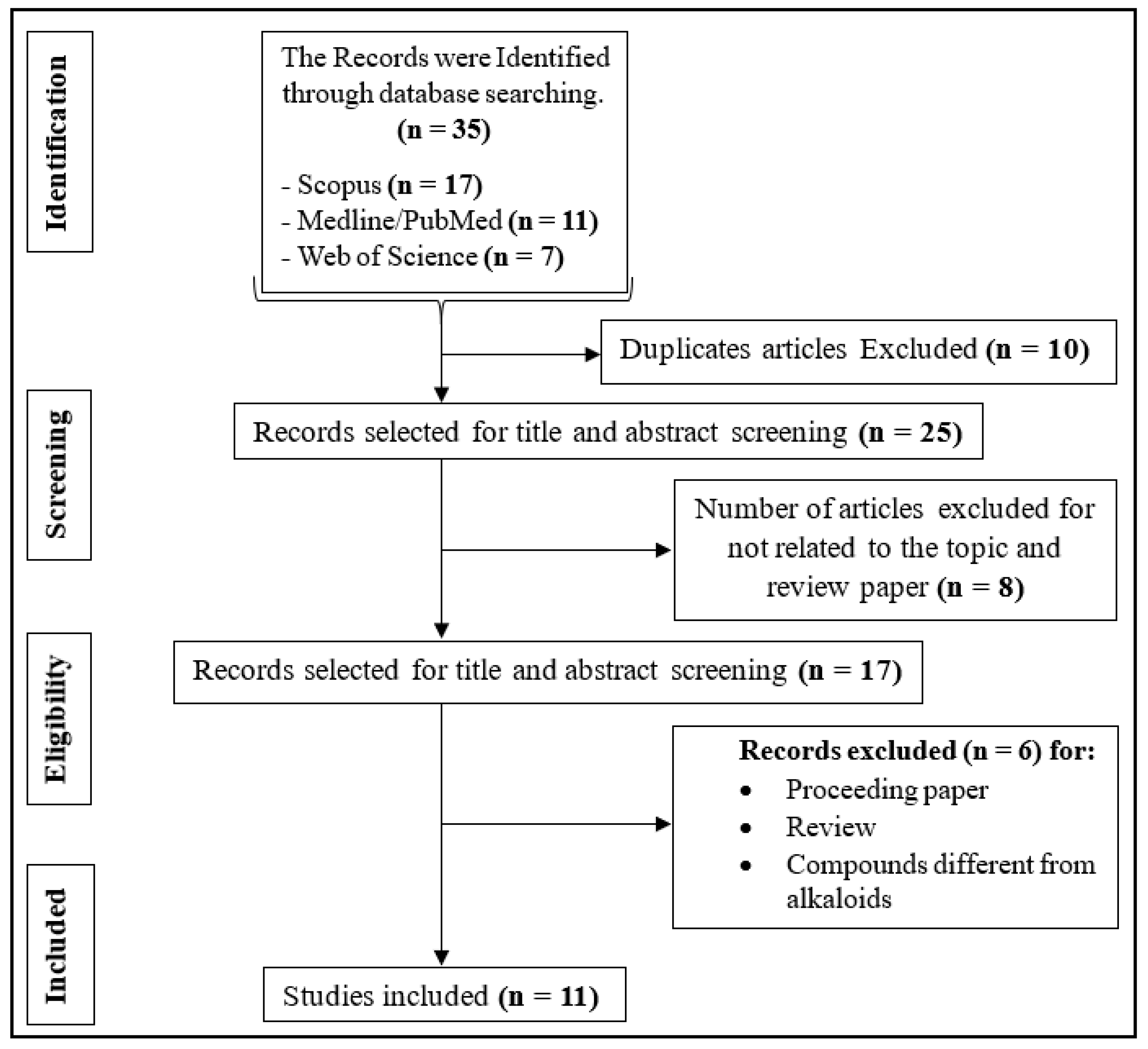
2.1. Characteristics of Results from Literature Search
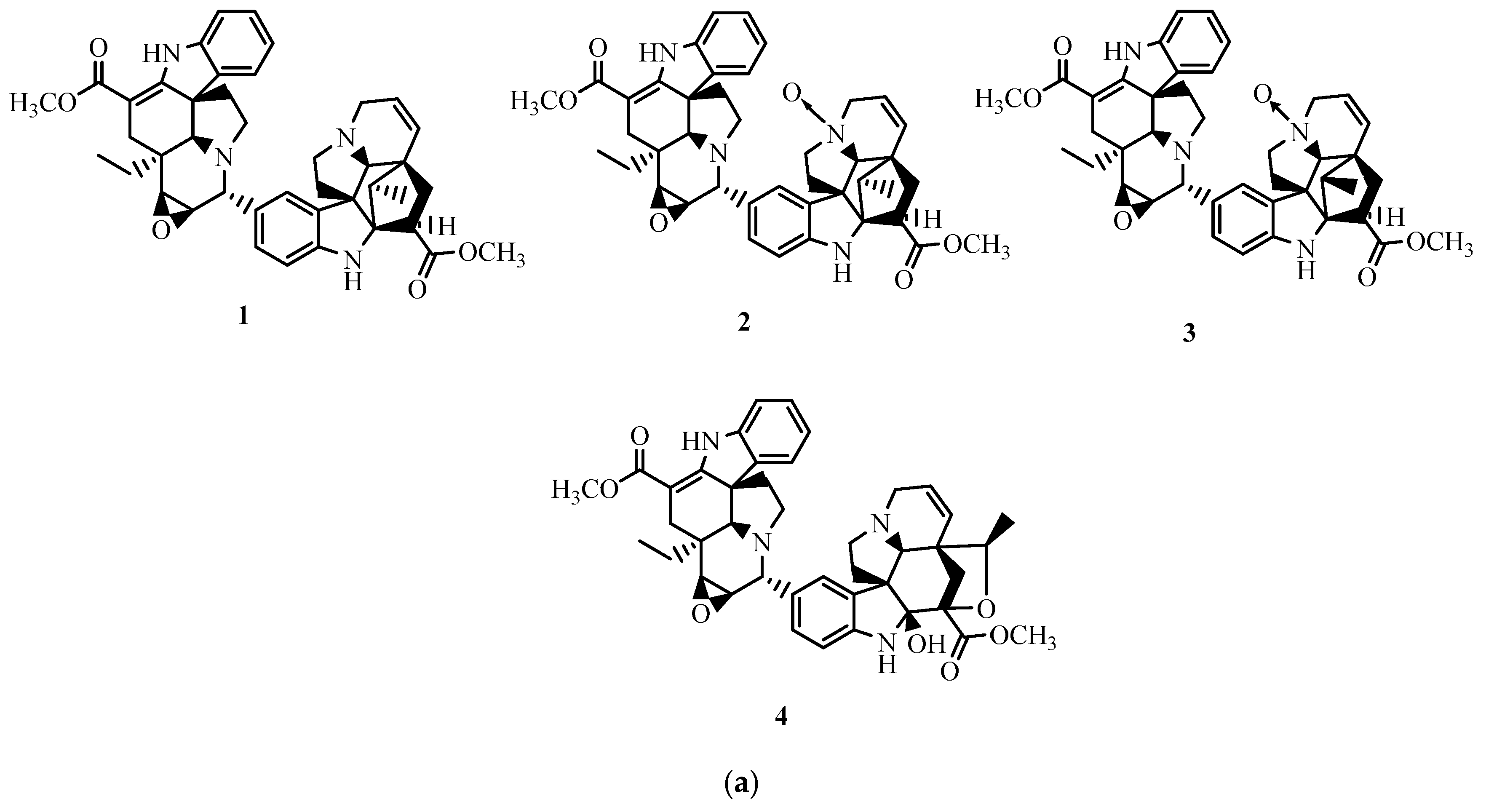
2.2. Axidimins C and D
2.3. Axidimins A and B
2.4. Tabersonine
2.5. 19R-Hydroxytabersonine and 11-Hydroxytabersonine
| Compounds | Targets | Cell Lines | Mode of Action | References |
|---|---|---|---|---|
| Acidimins C (3) and D (4) | Cyclin B1 and cdc2 | HCT116 | Downregulation inducing G2/M phase arrest. | [15] |
| Acidimins C (3) and D (4) | Bax and Bcl-2 | HCT116 | Alteration promoting apoptosis. | [15] |
| Acidimins C (3) and D (4) | P38 MAPK | HCT116 | Increase that caused G2/M cell cycle arrest and death. | [15] |
| 11-methoxytabersonine (12) | AMPK/mTOR and JNK | H157 | Activation caused autophagy. | [28] |
| Solasonin (17) | HDAC/P53/P21 | SW620 | Downregulation of HDAC. Increase P53 acetylation, increase P51 suppressing the growth of colorectal cancer. | [16] |
| Berbamine (21) | P21/Cyclin E1/Cyclin E2/CDK6/Cyclin D1/ | HT-29, HCT-116, RKO, SW480 | Increase P21 levels causing G1–S phase arrest; decreased cyclin E1, E2, D1 and CDK6. | [17] |
| Berbamine (21) | RT-qPCR | Downregulation on AKT1, EGFR, PDG-FRα and FGFR4. | [17] | |
| Nitidine chloride (19) | RKO | HCT116 | Suppress the cell proliferation. | [18] |
| Nitidine chloride (19) | HT29 | Colony inhibition. | [19] | |
| GB7 Acetate (20) | AMPK signaling pathway | HCT116 | Suppression of cell proliferation. | [19] |
| GB7 Acetate (20) | AMPK signaling pathway | HCT116 | Anti-metastatic, anti-metabolite capabilities. | [19] |
2.6. 11-Methoxytabersonine
2.7. Vandrikidine
2.8. Fusiformine A
2.9. 3-Oxotabersonine
2.10. Venalstonidine
2.11. (–)-Larutienine
2.12. Solasonin
2.13. Berbamine
2.14. Nitidine Chloride
2.15. GB7 Acetate
2.16. Berberine
2.17. Boldine
2.18. Worenine
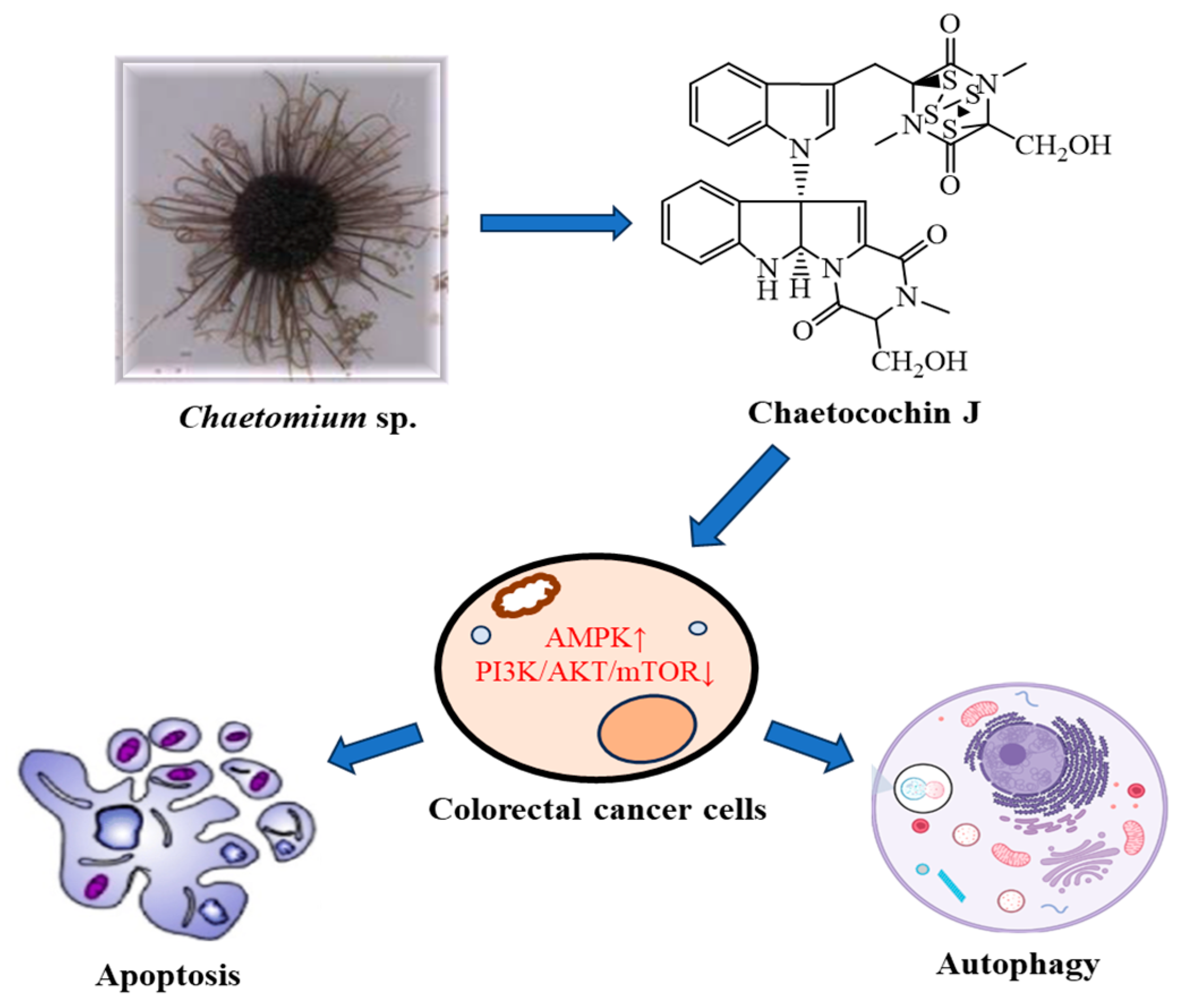
2.19. Chaetocochin J
2.20. Scandine, Melodinine W2 and 3-oxo-11-Methoxytabersonine
3. Methods
3.1. Eligibility Criteria
3.2. Data Sources with Search Tip
3.3. Study Choice
3.4. Data Gathering and Evaluation of Methodological Quality
4. General Discussion
5. Limitation
6. Critical Synthesis and Perspectives
7. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. International Agency for Research on Cancer; World Health Organization: Geneva, Switzerland, 2023. [Google Scholar]
- Ervik, M.; Lam, F.; Laversanne, M.; Ferlay, J.; Bray, F. Global Cancer Observatory: Cancer Over Time. Available online: https://gco.iarc.fr/overtime (accessed on 23 March 2023).
- Ferlay, J.; Ervik, M.; Lam, F.; Colombet, M.; Mery, L.; Piñeros, M.; Znaor, A.; Soerjomataram, I.; Bray, F. Global Cancer Observatory: Cancer Today. Available online: https://gco.iarc.fr/today (accessed on 10 October 2023).
- Ferlay, J.; Laversanne, M.; Ervik, M.; Lam, F.; Colombet, M.; Mery, L.; Piñeros, M.; Znaor, A.; Soerjomataram, I.; Bray, F. Global Cancer Observatory: Cancer Tomorrow. Available online: https://gco.iarc.fr/tomorrow (accessed on 10 October 2023).
- Roshandel, G.; Fatemeh, G.-K.; Malekzadeh, R. Colorectal Cancer: Epidemiology, Risk Factors, and Prevention. Cancers 2024, 16, 1530. [Google Scholar] [CrossRef] [PubMed]
- Sung, H.; Ferlay, J.M.E.; Rebecca, L.; Siegel, M.P.H.; Laversanne, M.; Soerjomataram, M.D.I.; Ahmedin Jemal, D.M.V.A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA A Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef] [PubMed]
- Arnold, M.; Sierra, M.S.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global patterns and trends in colorectal cancer incidence and mortality. Gut 2017, 66, 683–691. [Google Scholar] [CrossRef] [PubMed]
- Barbirou, M.; Woldu, H.G.; Sghaier, I.; Bedoui, S.A.; Mokrani, A.; Aami, R.; Mezlini, A.; Yacoubi-Loueslati, B.; Tonellato, P.J.; Bouhaouala-Zahar, B. Western influenced lifestyle and Kv2.1 association as predicted biomarkers for Tunisian colorectal cancer. BMC Cancer 2020, 20, 1086. [Google Scholar] [CrossRef]
- Safiri, S.; Sepanlou, S.G.; Ikuta, K.S.; Bisignano, C.; Salimzadeh, H.; Delavari, A.; Ansari, R.; Roshandel, G.; Merat, S.; Fitzmaurice, C.; et al. The global, regional, and national burden of colorectal cancer and its attributable risk factors in 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet Gastroenterol. Hepatol. 2019, 4, 913–933. [Google Scholar] [CrossRef] [PubMed]
- Adebayo, A.S.; Agbaje, K.; Adesina, S.K.; Olajubutu, O. Colorectal Cancer: Disease Process, Current Treatment Options, and Future Perspectives. Pharmaceutics 2023, 15, 2620. [Google Scholar] [CrossRef]
- Majolo, F.; de Oliveira Becker Delwing, L.K.; Marmitt, D.J.; Bustamante-Filho, I.C.; Goettert, M.I. Medicinal plants and bioactive natural compounds for cancer treatment: Important advances for drug discovery. Phytochem. Lett. 2019, 31, 196–207. [Google Scholar] [CrossRef]
- O’connor, S.E. Alkaloids. Compr. Nat. Prod. II Chem. Biol. 2010, 22, 728. [Google Scholar] [CrossRef]
- Aniszewski, T. Alkaloids: Chemistry, Biology, Ecology, and Applications, 2nd ed.; Elsevier: Amsterdam, The Netherlands, 2015. [Google Scholar]
- Hallajzadeh, J.; Maleki, D.P.; Mobini, M.; Asemi, Z.; Mansournia, M.A.; Sharifi, M.; Yousefi, B. Targeting of oncogenic signaling pathways by berberine for treatment of colorectal cancer. Med. Oncol. 2020, 37, 49. [Google Scholar] [CrossRef]
- Du, K.; Li, X.; Zheng, C.; Lai, L.; Shen, M.; Wang, Y.; Meng, D. Monoterpenoid indole alkaloid dimers from the Melodinus axillaris induce G2/M phase arrest and apoptosis via p38 MAPK activation in HCT116 cells. Bioorganic Chem. 2023, 140, 106841. [Google Scholar] [CrossRef]
- Lan, X.; Lu, M.; Fang, X.; Cao, Y.; Sun, M.; Shan, M.; Gao, W.; Wang, Y.; Yu, W.; Luo, H. Anti-Colorectal Cancer Activity of Solasonin from Solanum nigrum L. via Histone Deacetylases-Mediated p53 Acetylation Pathway. Molecules 2023, 28, 6649. [Google Scholar] [CrossRef] [PubMed]
- Liu, L.; Liang, D.; Zheng, Q.; Zhao, M.; Lv, R.T.; Tang, J.; Chen, N. Berbamine dihydrochloride suppresses the progression of colorectal cancer via RTKs/Akt axis. J. Ethnopharmacol. 2023, 303, 116025. [Google Scholar] [CrossRef] [PubMed]
- Zheng, Q.; Zhang, Y.; Zhang, L.; Chen, N.; Zhang, G.; Zhao, M.; Liao, W.; Zeng, Z.; Wei, Y.; Zhou, G.; et al. Nitidine chloride inhibits proliferation and induces apoptosis in colorectal cancer cells by activating the p53 signaling pathway. 2022, 1–20. [Google Scholar] [CrossRef]
- Li, Z.; Mao, L.; Yu, B.; Liu, H.; Zhang, Q.; Bian, Z.; Zhang, X.; Liao, W.; Sun, S. GB7 acetate, a galbulimima alkaloid from Galbulimima belgraveana, possesses anticancer effects in colorectal cancer cells. J. Pharm. Anal. 2022, 12, 339–349. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.; Liu, X.; Yu, M.; Xu, M.; Xiao, Y.; Ma, W.; Huang, L.; Li, X.; Ye, X. Berberine inhibits proliferation and induces G0/G1 phase arrest in colorectal cancer cells by downregulating IGF2BP3. Life Sci. 2020, 260, 118–413. [Google Scholar] [CrossRef] [PubMed]
- Samad, M.A.; Saiman, M.Z.; Abdul Majid, N.; Yaacob, J.S.; Karsani, S.A. Berberine inhibits telomerase activity and induces cell cycle arrest and telomere erosion in colorectal cancer cell line, hct 116. Molecules 2021, 26, 376. [Google Scholar] [CrossRef]
- Ji, L.; Shen, W.; Zhang, F.; Qian, J.; Jiang, J.; Weng, L.; Tan, J.; Li, L.; Chen, Y.; Cheng, H.; et al. Worenine reverses the Warburg effect and inhibits colon cancer cell growth by negatively regulating HIF-1α. Cell. Mol. Biol. Lett. 2021, 26, 19. [Google Scholar] [CrossRef]
- Hu, S.; Yin, J.; Yan, S.; Hu, P.; Huang, J.; Zhang, G.; Wang, F.; Tong, Q.; Zhang, Y. Chaetocochin J, an epipolythiodioxopiperazine alkaloid, induces apoptosis and autophagy in colorectal cancer via AMPK and PI3K/AKT/mTOR pathways. Bioorganic Chem. 2021, 109, 104–693. [Google Scholar] [CrossRef]
- Kuete, V.; Efferth, T. African Flora Has the Potential to Fight Multidrug Resistance of Cancer. BioMed Res. Int. 2015, 10, 914813. [Google Scholar] [CrossRef]
- Zhang, D.; Li, X.; Hu, Y.; Jiang, H.; Wu, Y.; Ding, Y.; Yu, K.; He, H.; Xu, J.; Sun, L.; et al. Tabersonine attenuates lipopolysaccharide-induced acute lung injury via suppressing TRAF6 ubiquitination. Biochem. Pharmacol. 2018, 154, 183–192. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Deng, Y.; Kang, L.; Chen, L.; Zheng, Z.; Huang, W.; Xu, C.; Kai, G.; Lin, D.; Tong, Q.; et al. Cytotoxic active ingredients from the seeds of Voacanga africana. S. Afr. J. Bot. 2021, 137, 311–319. [Google Scholar] [CrossRef]
- Jian, H.; Ye, Y.-L.; Zhou, Z.; Heng, H.; Francoise, P. Alkaloids from melodinus suaveolens. Phyrochemistry 1991, 30, 3168–3170. [Google Scholar] [CrossRef]
- Ge, D.; Tao, H.R.; Fang, L.; Kong, X.Q.; Han, L.N.; Li, N.; Xu, Y.X.; Li, L.Y.; Yu, M.; Zhang, H. 11-Methoxytabersonine induces necroptosis with autophagy through AMPK/mTOR and JNK Pathways in human lung cancer cells. Chem. Pharm. Bull. 2020, 68, 244–250. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.C.; Yang, J.; Zhou, X.R.; Liang, X.H.; Fu, Q.Y. Fusiformines A and B: New indole alkaloids from Melodinus fusiformis. Z. Fur Naturforschung—Sect. B J. Chem. Sci. 2016, 71, 193–195. [Google Scholar] [CrossRef]
- Mehri, H.; Rochat, C.; Baassou, S. Plante de Nouvelle-Calédonie* Alcaloïdes De Melodinus Reticulatus. Planta Medica 1983, 48, 72–76. [Google Scholar] [CrossRef] [PubMed]
- Xu, R.; Dong, Q.; Yu, Y.; Zhao, X.; Gan, X.; Wu, D.; Lu, Q.; Xu, X.; Yu, X.F. Berbamine: A novel inhibitor of bcr/abl fusion gene with potent anti-leukemia activity. Leuk. Res. 2006, 30, 17–23. [Google Scholar] [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. BMJ 2021, 372, 5. [Google Scholar] [CrossRef]
- Ndebia, E.J.; Kamsu, G.T. Natural Alkaloids as Potential Treatments for Esophageal Squamous-Cell Cancer: A Comprehensive Review. Gastroenterol. Endosc. 2024, 2, 131–136. [Google Scholar] [CrossRef]
- Xu, D.; Xu, Z. Indole Alkaloids with Potential Anticancer Activity. Curr. Top. Med. Chem. 2020, 20, 1938–1949. [Google Scholar] [CrossRef]
- Luo, M.-L.; Huang, W.; Zhu, H.-P.; Peng, C.; Zhao, Q.; Han, B. Advances in indole-containing alkaloids as potential anticancer agents by regulating autophagy. Biomed. Pharmacother. 2022, 149, 112–827. [Google Scholar] [CrossRef] [PubMed]
- Gonçalves, B.M.F.; Duarte, N.; Ramalhete, C.; Barbosa, F.; Madureira, A.M.; Ferreira, M.-J.U. Monoterpene indole alkaloids with anticancer activity from Tabernaemontana species. Phytochem. Rev. 2024, 14. [Google Scholar] [CrossRef]
- Chan, E.W.C.; Wong, S.K.; Chan, H.T. Apocynaceae species with antiproliferative and/or antiplasmodial properties: A review of ten genera. J. Integr. Med. 2016, 4, 269–284. [Google Scholar] [CrossRef] [PubMed]
- Mallikarjuna, K.; Bathula, C.; Reddy, G.D.; Shrestha, N.K.; Kim, H.; Noh, Y.-Y. Au-pd bimetallic nanoparticles embedded highly porous fenugreek polysaccharide based micro networks for catalytic applications. Int. J. Biol. Macromol. 2019, 126, 352–358. [Google Scholar] [CrossRef] [PubMed]
- Rehman, K.U.; Gouda, M.; Zaman, U.; Tahir, K.; Khan, S.U.; Saeed, S.; Khojah, E.; El-Beltagy, A.; Zaky, A.A.; Naeem, M.; et al. Optimization of Platinum Nanoparticles (PtNPs) Synthesis by Acid Phosphatase Mediated Eco-Benign Combined with Photocatalytic and Bioactivity Assessments. Nanomaterials 2022, 12, 1079. [Google Scholar] [CrossRef]
- Zong, W.; Gouda, M.; Cai, E.; Wang, R.; Xu, W.; Wu, Y.; Munekata, P.E.S.; Lorenzo, J.M. The Antioxidant Phytochemical Schisandrin A Promotes Neural Cell Proliferation and Differentiation after Ischemic Brain Injury. Molecules 2021, 26, 7466. [Google Scholar] [CrossRef]
| Names of Compounds | Molecular Formula | Molecular Mass (Cal.) |
|---|---|---|
| Monoterpenoid indole alkaloid dimers | ||
| Axidimin A (1) | C42H46N4O5 | 686.3468 |
| Axidimin B (2) | C42H46N4O6 | 702.3417 |
| Axidimin C (3) | C42H46N4O6 | 702.3417 |
| Axidimin D (4) | C42H46N4O7 | 718.3366 |
| Monoterpenoid indole alkaloid | ||
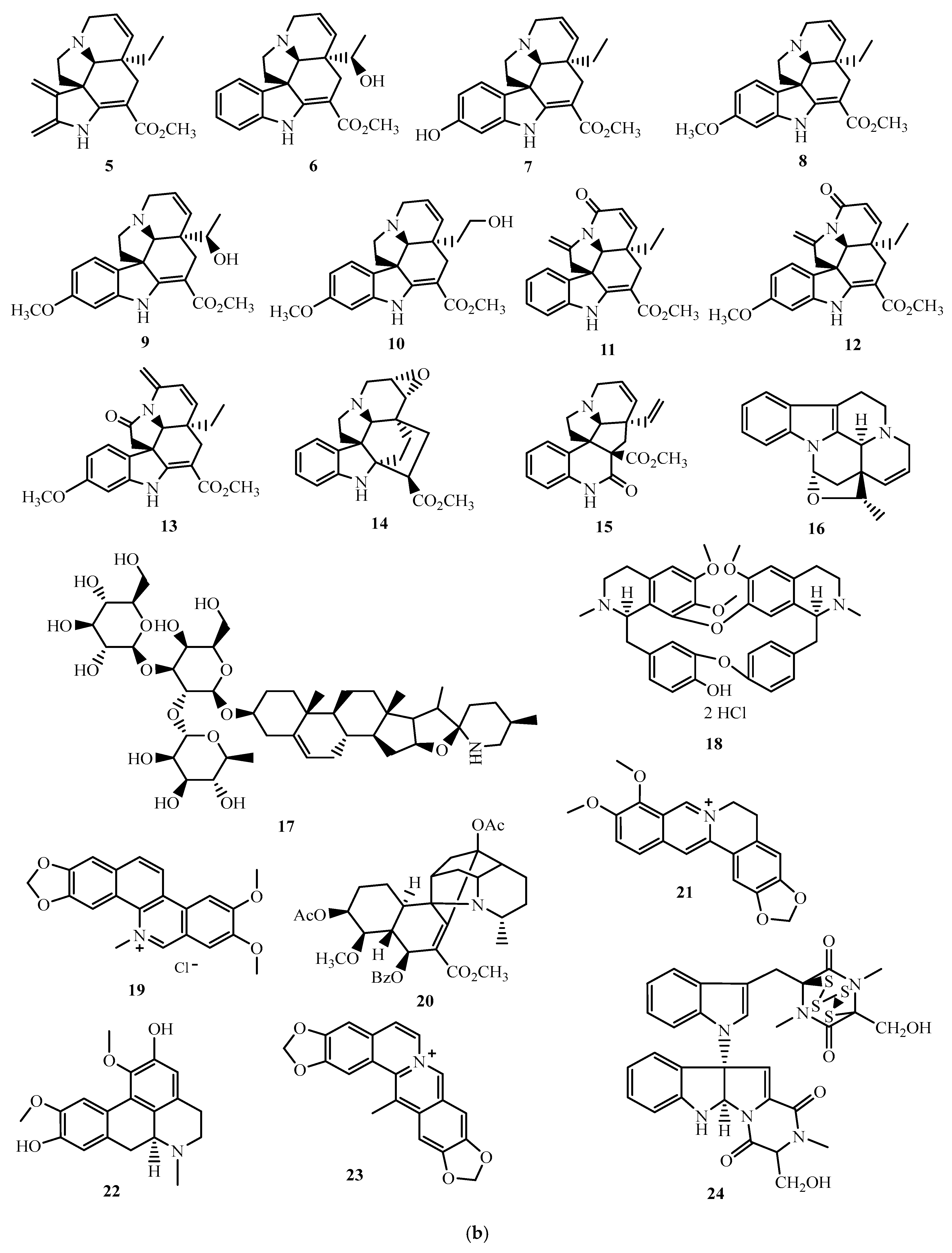
| Tabersonine (5) | C19H24N2O2 | 312.1838 |
| 19R-Hydroxytabersonine (6) | C21H24N2O3 | 352.1787 |
| 11-Hydroxytabersonine (7) | C21H24N2O3 | 352.1787 |
| 11-Methoxytabersonine (8) | C22H26N2O3 | 366.1943 |
| Vandrikidine (9) | C22H26N2O4 | 382.1893 |
| Fusiformine A (10) | C22H26N2O4 | 382.1893 |
| 3-oxotabersonine (11) | C22H22N2O3 | 362.1630 |
| 3-oxo-11-methoxytabersonine (12) | C23H24N2O4 | 392.1736 |
| Melodinine W2 (13) | C23H24N2O4 | 392.1736 |
| Venalstonidine (14) | C21H24N2O3 | 352.1787 |
| Scandine (15) | C21H22N2O3 | 350.1630 |
| (–)-larutienine A (16) | C19H20N2O | 292.1576 |
| Steroidal alkaloid | ||
| Solasonin (17) | C45H73N2O3 | 883.4929 |
| Bisbenzylisoquinoline alkaloid | ||
| Berbamine dihydrochloride (18) | C37H40N2O6 | 608.2886 |
| Nitidine chloride (19) | C21H18ClNO4 | 383.0924 |
| Galbulimima alkaloid | ||
| GB7 acetate (20) | C34H41NO9 | 607.2781 |
| Protoberberine alkaloid | ||
| Berberine (21) | C20H18NO4+ | 336.1230 |
| Aporphine alkaloid | ||
| Boldine (22) | C19H21NO4 | 327.1471 |
| Isoquinoline alkaloid | ||
| Worenine (23) | C20H14NO4+ | 332.0917 |
| Epipolythiodioxopiperazine alkaloid | ||
| Chaetocochin J (24) | C31H30N6O6S4 | 710.1110 |
| (a) | ||||||
| Alkaloids (Number) | Classes | Plant Source (Family) | Year | Country | Type of Cancer Cells Lines | References (Name of First Author) |
| Axidimin A (1) | Monoterpenoid indole alkaloid dimers | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Axidimin B (2) | Monoterpenoid indole alkaloid dimers | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Axidimin C (3) | Monoterpenoid indole alkaloid dimers | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Axidimin D (4) | Monoterpenoid indole alkaloid dimers | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| (b) | ||||||
| Alkaloids (Number) | Class | Plant Source (Family) | Year | Country | Type of Cancer Cell Line (IC50 Values) | Reference (Name of First Author) |
| Tabersonine (5) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| 19R-Hydroxytabersonine (6) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| 11-Hydroxytabersonine (7) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| 11-Methoxytabersonine (8) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Vandrikidine (9) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Fusiformine A (10) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| 3-oxotabersonine (11) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| 3-oxo-11-methoxytabersonine (12) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Melodinine W2 (13) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Venalstonidine (14) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Scandine (15) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| (–)-larutienine A (16) | Monoterpenoid indole alkaloid | Melodinus axillaris (Apocynaceae) | 2023 | China | CRC (HCT116) | [15] |
| Solasonin (17) | Steroidal alkaloid | Solanum nigrum L. (Solanaceae) | 2023 | China | CRC (SW620, SW480 and MGC803) | [16] |
| Berbamine dihydrochloride (18) | Bisbenzylisoquinoline alkaloid | Berberis amurensis (Berberidaceae) | 2023 | China | CRC (HT-29, HCT116, RKO and SW480) | [17] |
| Nitidine chloride (19) | Benzophenanthridine alkaloid | Zanthoxylum nitidum (Roxb.) DC (Rutaceae) | 2022 | China | CRC (RKO, HCT116 and HT29) | [18] |
| GB7 acetate (20) | Galbulimima alkaloid | Galbulimima belgraveana (Himantandraceae) | 2022 | China | CRC (HCT116) | [19] |
| Berberine (21) | Protoberberine alkaloid | Berberis spp. (Berberidaceae) Tinospora spp. (Menispermaceae) | 2021 | Malaysia | CRC (HCT116) | [21] |
| Coptidis rhizoma (Ranunculaceae) | 2020 | China | CRC (HCT116 and SW480, in vitro) | [20] | ||
| Boldine (22) | Aporphine alkaloid | Peumus boldus (Monimiaceae) | 2021 | Malaysia | CRC (HCT116) | [21] |
| Worenine (23) | Isoquinoline alkaloid | Coptis chinensis (Renonculacées) | 2021 | China | CRC (HCT116 and SW620) | [22] |
| Chaetocochin J (24) | Epipolythiodioxopiperazine alkaloid | Chaetomium sp. (Chaetomiaceae) | 2021 | China | CRC (RKO, HCT116 and SW480) | [23] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tabakam, T.G.; Makhafola, T.J. Plant-Derived Alkaloids as a Potential Source of Treatment for Colorectal Cancer over the Past Five Years: A Comprehensive Review. Plants 2024, 13, 2723. https://doi.org/10.3390/plants13192723
Tabakam TG, Makhafola TJ. Plant-Derived Alkaloids as a Potential Source of Treatment for Colorectal Cancer over the Past Five Years: A Comprehensive Review. Plants. 2024; 13(19):2723. https://doi.org/10.3390/plants13192723
Chicago/Turabian StyleTabakam, Tchangou Gaetan, and Tshepiso Jan Makhafola. 2024. "Plant-Derived Alkaloids as a Potential Source of Treatment for Colorectal Cancer over the Past Five Years: A Comprehensive Review" Plants 13, no. 19: 2723. https://doi.org/10.3390/plants13192723
APA StyleTabakam, T. G., & Makhafola, T. J. (2024). Plant-Derived Alkaloids as a Potential Source of Treatment for Colorectal Cancer over the Past Five Years: A Comprehensive Review. Plants, 13(19), 2723. https://doi.org/10.3390/plants13192723







