Epithelioid Hemangioma of the Nose: A Challenging Diagnosis
Abstract
:1. Introduction
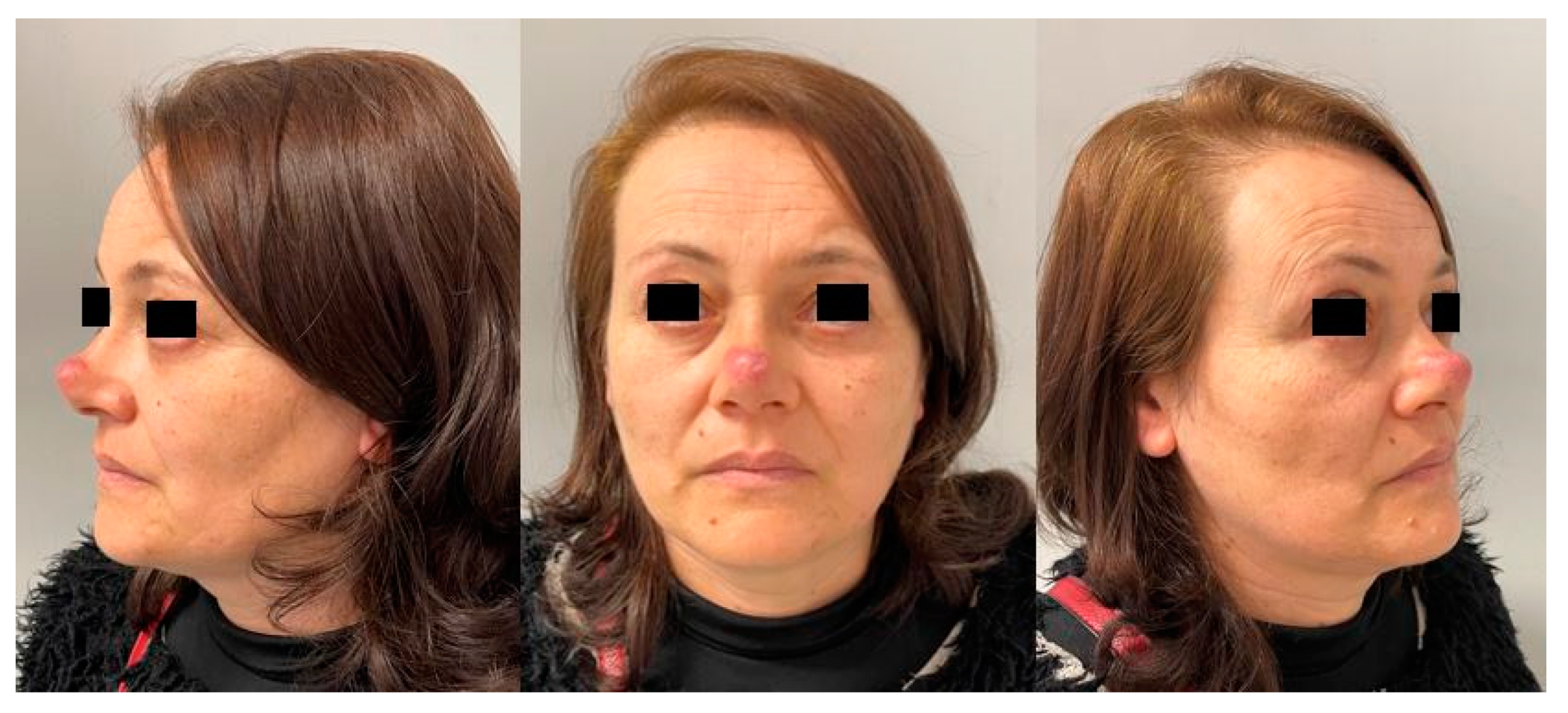
2. Case Report
3. Discussion
Author Contributions
Funding
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- ISSVA Classification of Vascular Anomalies ©2018 International Society for the Study of Vascular Anomalies. Available online: Issva.org/classification (accessed on 19 January 2022).
- Rosai, J.; Gold, J.; Landy, R. The histiocytoid hemangiomas. A unifying concept embracing several previously described entities of skin, soft tissue, large vessels, bone, and heart. Hum. Pathol. 1979, 10, 707–730. [Google Scholar] [CrossRef]
- Allen, P.W.; Ramakrishna, B.; MacCormac, L.B. The histiocytoid hemangiomas and other controversies. Pathol. Annu. 1992, 27 Pt 2, 51–87. [Google Scholar] [PubMed]
- Arnander, M.W.; Anderson, N.G.; Schönauer, F. The ultrasound halo sign in angiolymphoid hyperplasia of the temporal artery. Br. J. Radiol. 2006, 79, e184–e186. [Google Scholar] [CrossRef] [PubMed]
- Wiggins, C.J.; Dibbs, R.P.; Bartlett, E.L.; Ashton, D.J.; Maricevich, R.S. Atypical presentation and management of an epithelioid hemangioma: A case report and review of the literature. Ann. Pediatr. Surg. 2020, 16, 53. [Google Scholar] [CrossRef]
- Fetsch, J.F.; Weiss, S.W. Observations concerning the pathogenesis of epithelioid hemangioma (angiolymphoid hyperplasia). Mod. Pathol. 1991, 4, 449–455. [Google Scholar] [PubMed]
- Sharp, J.F.; Rodgers, M.J.C.; MacGregor, F.B.; Meehan, C.J.; McLaren, K. Angiolymphoid hyperplasia with eosinophilia. Laryngol. Otol. 1990, 104, 977–979. [Google Scholar] [CrossRef] [PubMed]
- Accardo, G.; Nele, G.; Turrà, F.; La Rusca, I.; Schonauer, F. A rare case of ‘histiocytoid haemangioma’ of the hand. J. Plast. Reconstr. Aesthet. Surg. 2013, 66, e318–e320. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mentzel, T.; Beham, A.; Calonje, E.; Katenkamp, D.; Fletcher, C.D. Epithelioid hemangioendothelioma of skin and soft tissues: Clinicopathologic and immunohistochemical study of 30 cases. Am. J. Surg. Pathol. 1997, 21, 363–374. [Google Scholar] [CrossRef] [PubMed]
- Kabir, S.; Teimoorian, M.; Mahdavi, M.; Meibodi, N.T.; Tajalli, M.; Goyonlo, V.M.; Sabourirad, S. A solitary erythematous papule on the nose. JAAD Case Rep. 2020, 6, 663–665. [Google Scholar] [CrossRef] [PubMed]
- Baghestani, S.; Firooz, A.; Ghazisaidi, M.R. A refractory case of angiolymphoid hyperplasia with eosinophilia successfully treated by surgery. J. Dermatol. Treat. 2011, 22, 49–51. [Google Scholar] [CrossRef] [PubMed]
- Cavaliere, A.; Maisto, B.; Zaporojan, T.; Giordano, L.; Sorbino, L.; Zaffiro, A.; Vozza, A.; La Padula, S.; D’Andrea, F.; Schonauer, F. Extended rotation flap for reconstruction of partial thickness defects of the tip and nasal ala region: In search of better aesthetic results. JPRAS Open 2021, 29, 82–88. [Google Scholar] [CrossRef] [PubMed]
- La Padula, S.; Abbate, V.; Di Monta, G.; Schonauer, F. Levator alae nasi muscle V-Y island flap for nasal tip reconstruction. J. Cranio-Maxillo-Facial Surg. 2017, 45, 432–435. [Google Scholar] [CrossRef] [PubMed]
- Schonauer, F.; Scafati, S.T.; Molea, G. Supratrochlear artery based V-Y flap for partial eyebrow reconstruction. J. Plast. Reconstr. Aesthet Surg. 2010, 63, 1391–1392. [Google Scholar] [CrossRef] [PubMed]
- Chiu, S.-C. An unusual case of angiolymphoid hyperplasia with eosinophilia of the nose. Ear Nose Throat J. 2013, 92, E10–E11. [Google Scholar] [PubMed]
- Panduranga Kamath, M.; Bhojwani, K.M.; Bhandarkar, A.M.; Pai, R.R.; Rent, N.H. Angiolymphoid hyperplasia with eosinophilia of root of nose: A rare phenomenon. J. Clin. Diagn. Res. 2014, 8, 144–145. [Google Scholar] [PubMed]
- Van Ratingen, A.R.; Linden, V.; Sillevis Smitt, J.H. Case Report: Angiolymphoid Hyperplasia with Eosinophilia of the Nose. Dermatol. Case Rep. 2016, 1, 105. [Google Scholar]
- Youssef, A.; Hasan, A.R.; Youssef, Y.; Al-Soufi, L.; Elshimali, Y.; Alshehabi, Z. Angiolymphoid hyperplasia with eosinophilia: A case report. J. Med. Case Rep. 2018, 12, 89. [Google Scholar] [CrossRef] [PubMed]
- Sedran, L.; Bonaso, M.; Mettus, A.; Roccia, F. Epithelioid Hemangioma of the Face. J. Craniofacial Surg. 2018, 29, e736–e739. [Google Scholar] [CrossRef] [PubMed]




Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Schonauer, F.; Cavaliere, A.; Pezone, G.; Calogero, A.; Sagnelli, C.; Sica, A.; D’Andrea, L.; Baldo, A. Epithelioid Hemangioma of the Nose: A Challenging Diagnosis. Healthcare 2022, 10, 633. https://doi.org/10.3390/healthcare10040633
Schonauer F, Cavaliere A, Pezone G, Calogero A, Sagnelli C, Sica A, D’Andrea L, Baldo A. Epithelioid Hemangioma of the Nose: A Challenging Diagnosis. Healthcare. 2022; 10(4):633. https://doi.org/10.3390/healthcare10040633
Chicago/Turabian StyleSchonauer, Fabrizio, Annachiara Cavaliere, Giuseppe Pezone, Armando Calogero, Caterina Sagnelli, Antonello Sica, Luca D’Andrea, and Antonello Baldo. 2022. "Epithelioid Hemangioma of the Nose: A Challenging Diagnosis" Healthcare 10, no. 4: 633. https://doi.org/10.3390/healthcare10040633
APA StyleSchonauer, F., Cavaliere, A., Pezone, G., Calogero, A., Sagnelli, C., Sica, A., D’Andrea, L., & Baldo, A. (2022). Epithelioid Hemangioma of the Nose: A Challenging Diagnosis. Healthcare, 10(4), 633. https://doi.org/10.3390/healthcare10040633






