Journal Description
Hearts
Hearts
is an international, peer-reviewed, open access journal on cardiology and cardiac & vascular surgery, published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within FSTA, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 18.5 days after submission; acceptance to publication is undertaken in 1.9 days (median values for papers published in this journal in the first half of 2024).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Latest Articles
Strategies for the Management of Cardiorenal Syndrome in the Acute Hospital Setting
Hearts 2024, 5(3), 329-348; https://doi.org/10.3390/hearts5030024 - 1 Aug 2024
Abstract
Cardiorenal syndrome (CRS) is a life-threatening disorder that involves a complex interplay between the two organs. Managing this multifaceted syndrome is challenging in the hospital and requires a multidisciplinary approach to tackle the many manifestations and complications. There is no universally accepted algorithm
[...] Read more.
Cardiorenal syndrome (CRS) is a life-threatening disorder that involves a complex interplay between the two organs. Managing this multifaceted syndrome is challenging in the hospital and requires a multidisciplinary approach to tackle the many manifestations and complications. There is no universally accepted algorithm to treat patients, and therapeutic options vary from one patient to another. The mainstays of therapy involve the stabilization of hemodynamics, decongestion using diuretics or renal replacement therapy, improvement of cardiac output with inotropes, and goal-directed medical treatment with renin–angiotensin–aldosterone system inhibitors, beta-blockers, and other medications. Mechanical circulatory support is another viable option in the armamentarium of agents that improve symptoms in select patients.
Full article
(This article belongs to the Collection Feature Papers from Hearts Editorial Board Members)
►
Show Figures
Open AccessSystematic Review
Does Endodontic Treatment Influence Human Endocarditis? Systematic Review
by
Jennifer Santos Pereira, Anna Carolina Neves Leutz, Brenda P. F. A. Gomes, Lauter E. Pelepenko and Marina Angélica Marciano
Hearts 2024, 5(3), 308-328; https://doi.org/10.3390/hearts5030023 - 31 Jul 2024
Abstract
►▼
Show Figures
Endocarditis is a severe infection affecting the heart’s inner layer, the endocardium. Its pathophysiology may involve heart valve damage, bacteria adhesion and biofilm formation, potentially leading to fatal complications. Bacteria from various sources, including from endodontic diseases and its treatments may enter the
[...] Read more.
Endocarditis is a severe infection affecting the heart’s inner layer, the endocardium. Its pathophysiology may involve heart valve damage, bacteria adhesion and biofilm formation, potentially leading to fatal complications. Bacteria from various sources, including from endodontic diseases and its treatments may enter the bloodstream provoking this condition. This systematic review aimed to explore the influence of endodontic factors on endocarditis. Searches across PubMed, Embase, Cochrane Library and manual sources yielded 14 relevant articles from 1562 screened studies. Assessment platforms from JBI Critical Appraisal Tools evaluated studies biases. Findings mainly focused on transient bacteraemia as a key indicator of risk correlating bacterial virulence and counts with endocarditis development. Worryingly, multi-species bacteraemia post-endodontic treatment was noted including the genera Enterococcus, Parvimonas, Streptococcus and Staphylococcus. Conclusive validation of the incidence and association between endodontic patients and endocarditis was limited due to a lack of robust longitudinal investigations, such as randomized controlled trials. This emphasizes the need for further research with well-designed methodologies to provide a full understanding of the causative bacterial population and its pathological mechanisms. A current guideline (2023 European Society of Cardiology) was developed to support healthcare professionals in diagnosing and managing infective endocarditis; this 2023 version is introducing a new diagnostic algorithm to aid in patient classification aiming to improve outcomes for this challenging disease. The study was a priori registered on PROSPERO (CRD42023407736).
Full article

Figure 1
Open AccessFeature PaperReview
A Focus on Heart Failure Management through Diet and Nutrition: A Comprehensive Review
by
Lee P. Liao, Anushriya Pant, Simone Marschner, Peter Talbot and Sarah Zaman
Hearts 2024, 5(3), 293-307; https://doi.org/10.3390/hearts5030022 - 29 Jul 2024
Abstract
►▼
Show Figures
There is emerging evidence to suggest that diet and dietary interventions can have an impact on heart failure (HF) outcomes. Currently, the restriction of salt intake is the only dietary advice that is consistently guideline-recommended for the management of HF despite conflicting evidence
[...] Read more.
There is emerging evidence to suggest that diet and dietary interventions can have an impact on heart failure (HF) outcomes. Currently, the restriction of salt intake is the only dietary advice that is consistently guideline-recommended for the management of HF despite conflicting evidence for its efficacy. Dietary components that have been investigated in people with HF include middle-chain triglyceride (MCT) oil, beta-hydroxybutyrate (BHB) salts, ketone esters and coenzyme Q10 (CoQ10). Supplementation with these components is thought to be cardioprotective possibly due to an increase in myocardial energy production. There have been research studies on the effectiveness of The Dietary Approaches to Stop Hypertension (DASH) diet and the Mediterranean Diet (MedDiet) in the treatment of HF, but with conflicting results. The ketogenic diet (KD) has come to the forefront of interest due to evidence indicating its effectiveness in addressing the metabolic shift that occurs in HF. However, there is a lack of randomised controlled trials (RCT) centred around the KD. In any dietary intervention, factors such as adherence and compliance affect the validity of the results. Malnutrition, sarcopenia and/or cardiac cachexia can be present in the more advanced stages of heart failure. Nutritional screening, assessment and support/intervention are important aspects of treatment in the advanced stages of heart failure. Furthermore, HF management through dietary intervention is further complicated by the presence of comorbidities, such as diabetes mellitus (DM) and coronary artery disease (CAD). Long-term studies on the use of dietary modifications in people with HF are warranted to ascertain their efficacy, safety and side effects.
Full article

Figure 1
Open AccessCase Report
Breaking Boundaries: From Fall to Rapid Cardiac Rescue
by
Michele D’Alonzo, Mariantonietta Piscitelli and Francesco Cilia
Hearts 2024, 5(3), 288-292; https://doi.org/10.3390/hearts5030021 - 22 Jul 2024
Abstract
►▼
Show Figures
The occurrence of pericardial rupture as a complication of blunt thoracic trauma has the potential to result in cardiac dislocation unless promptly identified and subjected to suitable surgical intervention. This phenomenon is exceptionally uncommon and is associated with a significant mortality rate between
[...] Read more.
The occurrence of pericardial rupture as a complication of blunt thoracic trauma has the potential to result in cardiac dislocation unless promptly identified and subjected to suitable surgical intervention. This phenomenon is exceptionally uncommon and is associated with a significant mortality rate between 30 and 67%. The diagnosis remains complex due to the scarcity of symptoms. However, the routine application of computed tomography (CT) scans in the management of trauma patients could facilitate the early identification of cardiac dislocation. In this case report, we described the diagnostic–therapeutic pathway of a pericardial rupture due to high-intensity trauma.
Full article

Figure 1
Open AccessArticle
Supervised Machine Learning to Examine Factors Associated with Respiratory Sinus Arrhythmias and Ectopic Heart Beats in Adults: A Pilot Study
by
Peyton Lahr, Chloe Carling, Joseph Nauer, Ryan McGrath and James W. Grier
Hearts 2024, 5(3), 275-287; https://doi.org/10.3390/hearts5030020 - 5 Jul 2024
Abstract
►▼
Show Figures
Background: There are many types of arrhythmias which may threaten health that are well-known or opaque. The purpose of this pilot study was to examine how different cardiac health risk factors rank together in association with arrhythmias in young, middle-aged, and older adults.
[...] Read more.
Background: There are many types of arrhythmias which may threaten health that are well-known or opaque. The purpose of this pilot study was to examine how different cardiac health risk factors rank together in association with arrhythmias in young, middle-aged, and older adults. Methods: The analytic sample included 101 adults aged 50.6 ± 22.6 years. Several prominent heart-health-related risk factors were self-reported. Mean arterial pressure and body mass index were collected using standard procedures. Hydraulic handgrip dynamometry measured strength capacity. A 6 min single-lead electrocardiogram evaluated arrhythmias. Respiratory sinus arrhythmias (RSAs) and ectopic heart beats were observed and specified for analyses. Classification and Regression Tree analyses were employed. Results: A mean arterial pressure ≥ 104 mmHg was the first level predictor for ectopic beats, while age ≥ 41 years was the first level predictor for RSAs. Age, heart rate, stress and anxiety, and physical activity emerged as important variables for ectopic beats (p < 0.05), whereas age, sodium, heart rate, and gender were important for RSAs (p < 0.05). Conclusions: RSAs and ectopic arrhythmias may have unique modifiable and non-modifiable factors that may help in understanding their etiology for prevention and treatment as appropriate across the lifespan.
Full article

Figure 1
Open AccessArticle
Occupational Physical Activity and Fitness in Predicting Cardiovascular Mortality among European Cohorts of Middle-Aged Men: A 60-Year Follow-Up in the Seven Countries Study
by
Paolo Emilio Puddu, Anthony Kafatos, Hanna Tolonen, Johanna M. Geleijnse and Alessandro Menotti
Hearts 2024, 5(3), 259-274; https://doi.org/10.3390/hearts5030019 - 30 Jun 2024
Abstract
►▼
Show Figures
Aim and Background: To determine whether occupational physical activity (OPA) and physical fitness (Fitscore) predict cardiovascular disease (CVD) mortality and its components. Methods: Among middle-aged men (N = 5482) of seven cohorts of the Seven Countries Study (SCS), several baseline risk factors were
[...] Read more.
Aim and Background: To determine whether occupational physical activity (OPA) and physical fitness (Fitscore) predict cardiovascular disease (CVD) mortality and its components. Methods: Among middle-aged men (N = 5482) of seven cohorts of the Seven Countries Study (SCS), several baseline risk factors were measured, and there was a follow-up for 60 years until virtual extinction. OPA was estimated from the type of work while Fitscore was derived from linear combinations of levels of arm circumference, heart rate and vital capacity computed as a factor score by principal component analysis. The predictive adjusted power of these characteristics was obtained by Cox models for coronary heart disease (CHD), heart diseases of uncertain etiology (HDUE), stroke and CVD outcomes. Results: Single levels of the three indicators of fitness were highly related to the three levels of OPA and Fitscore. High levels of both OPA and Fitscore forced into the same models were associated with lower CVD, CHD, HDUE and stroke mortality. When assessed concomitantly in the same models, hazard ratios (high versus low) for 60-year CVD mortality were 0.88 (OPA: 95% CI: 0.78–0.99) and 0.68 (Fitscore 95% CI: 0.61–0.75), and the predictive power of Fitscore outperformed that of OPA for CHD, HDUE and stroke outcomes. Similar results were obtained in individual outcome models in the presence of risk factors. Segregating the first 30 from the second 30 years of follow-up indicated that people dying earlier had lower arm circumference and vital capacity, whereas heart rate was higher for CVD and most of its major components (all p < 0.0001). Conclusions: OPA was well related to the indicators of fitness involving muscular mass, cardio-circulatory and respiratory functions, thus adding predictive power for CVD events. The Fitscore derived from the above indicators represents another powerful long-term predictor of CHD, HDUE and stroke mortality.
Full article

Figure 1
Open AccessArticle
Bicuspid Aortic Valve Disease with Early-Onset Complications: Characteristics and Aortic Outcomes
by
Maximilian A. Selbst, Colin R. Ward, Megan L. Svetgoff, Hector I. Michelena, Anna Sabate-Rotes, Julie De Backer, Laura Muiño Mosquera, Anji T. Yetman, Malenka M. Bissell, Maria Grazia Andreassi, Ilenia Foffa, Dawn S. Hui, Anthony Caffarelli, Yuli Y. Kim, Dongchuan Guo, Rodolfo Citro, Margot De Marco, Justin T. Tretter, Shaine A. Morris, Kim L. McBride, Simon C. Body and Siddharth K. Prakashadd
Show full author list
remove
Hide full author list
Hearts 2024, 5(3), 253-258; https://doi.org/10.3390/hearts5030018 - 21 Jun 2024
Abstract
Bicuspid aortic valve (BAV) is the most common congenital heart malformation in adults, but it can also cause childhood-onset complications. The presentation and clinical course of young adults who present due to BAV complications are relatively uncharacterized. In a multicenter study, we found
[...] Read more.
Bicuspid aortic valve (BAV) is the most common congenital heart malformation in adults, but it can also cause childhood-onset complications. The presentation and clinical course of young adults who present due to BAV complications are relatively uncharacterized. In a multicenter study, we found that young people who experience significant complications related to BAV disease before age 30 are distinguished from the majority of BAV cases that manifest after age 50 by a relatively severe clinical course, with higher rates of surgical interventions, more frequent second interventions, and a greater burden of congenital heart malformations. These observations highlight the need for prompt recognition, regular lifelong surveillance, and targeted interventions to address the significant health burdens of patients with early-onset BAV complications.
Full article
Open AccessReview
Unpacking Trastuzumab-Induced Cardiomyopathy: A Cardiac Conundrum
by
Supriya Peshin, Shivani Modi, Lalith Namburu and Malay Rathod
Hearts 2024, 5(2), 246-252; https://doi.org/10.3390/hearts5020017 - 20 Jun 2024
Abstract
►▼
Show Figures
Cardiovascular diseases are a leading cause of mortality in the United States. The increasing number of cancer patients experiencing cardiovascular side effects from chemotherapeutic drugs is a cause for concern. Trastuzumab is a highly effective targeted therapy for HER2-positive cancers but its use
[...] Read more.
Cardiovascular diseases are a leading cause of mortality in the United States. The increasing number of cancer patients experiencing cardiovascular side effects from chemotherapeutic drugs is a cause for concern. Trastuzumab is a highly effective targeted therapy for HER2-positive cancers but its use is limited globally due to its cardiotoxic effects. The most severe adverse effect is cardiomyopathy, which is characterized by contractile dysfunction and reduced left ventricular systolic function. The electrophysiological side effects of trastuzumab are still not fully understood. Due to these life-threatening side effects, trastuzumab is routinely discontinued. This review aims to provide a comprehensive overview of trastuzumab-induced cardiomyopathy, including the mechanisms by which trastuzumab exerts its cardiotoxic effects, the clinical manifestations, diagnostic strategies, and potential interventions to protect the heart. By shedding light on the various aspects of this condition, we hope to emphasize the importance of early detection and effective management, as well as the urgent need for further research to optimize the balance between successful cancer treatment and cardiovascular well-being. Cardiologists, oncologists, and researchers are at the forefront of this critical intersection between oncology and cardiology, working collaboratively to enhance patient outcomes in the era of trastuzumab therapy.
Full article

Figure 1
Open AccessArticle
The Impact of Sickle Cell Disease on Acute Coronary Syndrome and PCI Outcomes: A Retrospective Observational Study
by
Abdulmajeed Alharbi, Clarissa Pena, Mohammed Mhanna, Caleb Spencer, Masharib Bashar, Michelle Cherian, Ahmad Abdulrahman, Halah Alfatlawi, Eun Seo Kwak, Mohammad Siddique and Ragheb Assaly
Hearts 2024, 5(2), 236-245; https://doi.org/10.3390/hearts5020016 - 27 May 2024
Abstract
►▼
Show Figures
Introduction: Sickle cell disease (SCD) is a genetic disorder that is widely observed on a global scale and known for its substantial negative impact on health and mortality. The purpose of this research was to explore how SCD influences the outcomes of acute
[...] Read more.
Introduction: Sickle cell disease (SCD) is a genetic disorder that is widely observed on a global scale and known for its substantial negative impact on health and mortality. The purpose of this research was to explore how SCD influences the outcomes of acute coronary syndrome (ACS) and Percutaneous Coronary Intervention (PCI). Methods: A retrospective observational analysis was conducted using the National Inpatient Sample (NIS) data for the year 2020. Adult patients with concurrent ACS and SCD diagnoses were included in the study. Demographic information, clinical characteristics, in-hospital outcomes, and PCI complications were examined and compared between ACS patients with and without SCD. Results: Among a total of 779,895 ACS patients, 1495 had coexisting SCD. SCD patiets exhibited distinct demographic features, such as younger age (mean age: 59 vs. 66 years), predominantly female (53% vs. 35%), and primarily African American (91% vs. 11%). Comorbid conditions such as hypertension and chronic lung disease were more prevalent in SCD patients. While inpatient mortality odds did not significantly differ, SCD patients demonstrated slightly shorter lengths of stay in cases of STEMI and NSTEMI/UA. Notably, SCD patients faced a statistically significant increased risk of coronary dissection, highlighting a unique complication in this population. Although an increased incidence of atrial fibrillation and acute heart failure was observed in SCD patients, statistical significance was not achieved. Conclusions: This study provides valuable insight into the intricate interplay between SCD and ACS outcomes. SCD patients presented with distinctive demographic and clinical profiles that influenced their experience with ACS. The elevated risk of coronary dissection emphasizes the necessity for tailored interventions and careful management in SCD patients. These findings underscore the need for further research to elucidate underlying mechanisms and optimize treatment strategies for individuals with both SCD and ACS.
Full article

Figure 1
Open AccessArticle
Prognostic Value and Limits of Heart Rate and QT—Corrected in A Large Population
by
Paolo Giovanardi, Cecilia Vernia, Sara Roversi, Enrico Tincani, Giuseppe Spadafora, Federico Silipo and Claudio Giberti
Hearts 2024, 5(2), 225-235; https://doi.org/10.3390/hearts5020015 - 27 May 2024
Abstract
►▼
Show Figures
Background: The study aimed to compare the prognostic importance of the heart rate (HR) and QT—corrected (QTc) according to Fridericia, Framingham, and Bazett with respect to all-cause mortality in a large non-selected population. Methods: The analysis of digital electrocardiograms archived from 2008 to
[...] Read more.
Background: The study aimed to compare the prognostic importance of the heart rate (HR) and QT—corrected (QTc) according to Fridericia, Framingham, and Bazett with respect to all-cause mortality in a large non-selected population. Methods: The analysis of digital electrocardiograms archived from 2008 to 2022 in the metropolitan area of Modena, Italy, was carried out. The population under study was divided into three groups based on age, and survival analysis was performed. Results: 131,627 patients were enrolled and, during the follow-up (mean 1641.4 days), all-cause mortality was 8.9%. Both HR and QTc were associated with mortality. All-cause mortality significantly increased with HR values greater than 81 BPM and QTc values greater than 440 msec in young subjects and 455 msec in old subjects (values of the 75th percentiles/optimal operating point). A Cox analysis confirmed the better prognostic value of Bazett’s QTc and HR in the whole population and in the three age-groups. Conclusion: Bazett’s method performed better than the others, but, unexpectedly, the HR had the same or an even better correlation with all-cause mortality. Since the HR is simple and readily available, its evaluation should be improved. However, QTC and HR values are difficult to define, causing many confounding factors, and further population studies are required.
Full article

Graphical abstract
Open AccessArticle
Arterial Stiffness Is an Important Predictor of Heart Failure with Preserved Ejection Fraction (HFpEF)—The Effects of Phosphate Retention
by
Yuji Mizuno, Toshifumi Ishida, Kenichi Tsujita and Michihiro Yoshimura
Hearts 2024, 5(2), 211-224; https://doi.org/10.3390/hearts5020014 - 17 May 2024
Abstract
►▼
Show Figures
Heart failure with preserved ejection fraction (HFpEF) is a major health concern. There is a growing recognition of the causal interplay between arterial stiffness and HFpEF. We recently reported that phosphate retention is a trigger for arterial stiffness. This study focuses on whether
[...] Read more.
Heart failure with preserved ejection fraction (HFpEF) is a major health concern. There is a growing recognition of the causal interplay between arterial stiffness and HFpEF. We recently reported that phosphate retention is a trigger for arterial stiffness. This study focuses on whether arterial stiffness due to phosphate retention could be a predictor for HFpEF. Methods: The subjects of this study were 158 patients (68 males and 90 females, mean age 74.8 ± 11.2). HFpEF was defined according to the guidelines of the ESC 2019. Pulse wave velocity (PWV) and central systolic blood pressure (CSBP) were used as markers for arterial stiffness and afterload, respectively. We measured serum levels of fibroblast growth factor 23 (FGF23) as a marker of phosphate retention. Results: The serum levels of FGF23 had a significant relationship with PWV. PWV had significant relationships with LV mass index, plasma BNP levels, and relative wall thickness, e′, and E/e′ (p < 0.001, respectively). Multivariate logistic regression analysis revealed that higher PWV values and hypertension were significant predictors for the dependent factor (HFpEF). Arterial stiffness amplified afterload, leading to LV concentric hypertrophy and diastolic dysfunction. This study presents that arterial stiffness is a key predictor of HFpEF, and that phosphate retention is involved in the pathology of HFpEF.
Full article

Graphical abstract
Open AccessArticle
Dietary Fatty Acids Predicting Long Term Cardiovascular Mortality in a Cohort of Middle-Aged Men Followed-Up until Extinction
by
Alessandro Menotti and Paolo Emilio Puddu
Hearts 2024, 5(2), 196-210; https://doi.org/10.3390/hearts5020013 - 23 Mar 2024
Cited by 2
Abstract
Objectives: To report the relationships of major dietary fatty acids with major cardiovascular disease mortality groups in a cohort of middle-aged men followed up with until extinction. Material and Methods: In the early 1960s, a cohort of men aged 40 to 59 years
[...] Read more.
Objectives: To report the relationships of major dietary fatty acids with major cardiovascular disease mortality groups in a cohort of middle-aged men followed up with until extinction. Material and Methods: In the early 1960s, a cohort of men aged 40 to 59 years was enrolled and examined within the Italian Rural Areas section of the Seven Countries Study including dietary history that allowed for the estimation of major fatty acid (FA) intake (saturated FAs: SAFAs; mono-unsaturated FAs: MUFAs; and poly-unsaturated FAs: PUFAs), their ratios, and the production of a dietary score derived from 18 food groups, the high levels of which corresponded to a Mediterranean diet profile. Results: During a follow-up of 61 years, the intake of SAFAs was directly while that of MUFAs was inversely and significantly associated with coronary heart disease (CHD) mortality (the hazard ratio for one standard deviation was 1.28 and 0.84, respectively) but not with other cases of Heart Disease of Uncertain Etiology (HDUE) and stroke mortality. The hazard ratio for SAFAs remained significant after factoring into the multivariate models the dietary score and other classical cardiovascular risk factors (age, smoking habits, cholesterol levels, and systolic blood pressure). The role of the dietary score was inverse and significant (hazard ratio of 0.73). Again, this was true for CHD but not for HDUE and stroke mortality. Conclusions: Both SAFAs and MUFAs predict long-term CHD mortality, together with a dietary score, but not HDUE and stroke, which represent different diseases also in relation to dietary habits.
Full article
Open AccessArticle
Significance of Smoking in Patients with Acute ST Elevation Myocardial Infarction (STEMI) Undergoing Primary Percutaneous Coronary Intervention: Evaluation of Coronary Flow, Microcirculation and Left Ventricular Systolic Function
by
Mariana Boulos, Yasmine Sharif, Nimer Assy and Dawod Sharif
Hearts 2024, 5(1), 182-195; https://doi.org/10.3390/hearts5010012 - 21 Mar 2024
Abstract
►▼
Show Figures
In the thrombolytic care era, myocardial infarction in cigarette smokers was associated with better six-month outcomes compared to non-smokers. Aims: We tested the hypothesis that in patients with anterior myocardial infarction with ST-segment elevation (STEMI) treated with primary percutaneous coronary intervention (PPCI), cigarette
[...] Read more.
In the thrombolytic care era, myocardial infarction in cigarette smokers was associated with better six-month outcomes compared to non-smokers. Aims: We tested the hypothesis that in patients with anterior myocardial infarction with ST-segment elevation (STEMI) treated with primary percutaneous coronary intervention (PPCI), cigarette smoking is associated with better coronary artery flow, myocardial perfusion, and left ventricular systolic function. Methods: Ninety-nine patients (sixty-six smokers) with anterior STEMI treated with PPCI were studied. Angiographic coronary artery flow TIMI grades, myocardial blush grades (MBGs) before and after PPCI, ST-segment elevation resolution, maximal troponin I and creatine phosphokinase blood levels, left ventricular echocardiographic systolic function as well as left anterior descending coronary artery (LAD) velocity parameters at admission and at discharge were evaluated. Results: Smokers and non-smokers were treated similarly. In smokers, the age was significantly younger, 54 ± 10, compared to non-smokers, 71.8 ± 10 years, p < 0.05, and had a lower prevalence of women, 13.6% compared to 36.6%. TIMI and MBG before and after PPCI were similar between smokers and non-smokers. Smokers had a lower prevalence of complete ST elevation resolution, 33% compared to 50% in non-smokers. Diastolic LAD velocity and integral were lower in smokers, p < 0.05. Maximal biomarker blood levels as well as LV systolic function at admission and on discharge were similar. Conclusions: Cigarette smokers with anterior STEMI treated with PPCI were younger with a lower prevalence of women and of complete ST elevation resolution and had lower LAD diastolic velocity and integral late after PPCI. However, angiographic parameters and LV systolic function parameters were similar.
Full article
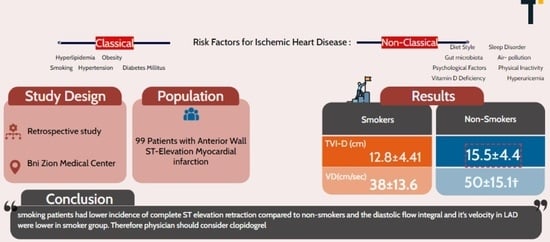
Graphical abstract
Open AccessArticle
Temporal Responses of a Low-Energy Meal Replacement Plan or Exercise Training on Cardiovascular Function and Fibro-Inflammatory Markers in People with Type 2 Diabetes—A Secondary Analysis of the “Diabetes Interventional Assessment of Slimming or Training to Lessen Inconspicuous Cardiovascular Dysfunction” Study
by
Joanna M. Bilak, Gaurav S. Gulsin, Vasiliki Bountziouka, Kelly S. Parke, Emma Redman, Joseph Henson, Lei Zhao, Phillipe Costet, Mary Ellen Cvijic, Juan Maya, Ching-Pin Chang, Melanie J. Davies, Thomas Yates, Gerry P. McCann and Emer M. Brady
Hearts 2024, 5(1), 165-181; https://doi.org/10.3390/hearts5010011 - 16 Mar 2024
Abstract
►▼
Show Figures
Background: This study assesses the temporal responses of cardiovascular function, fibro-inflammation, and glucometabolic profiles in asymptomatic adults with type 2 diabetes, following a low-energy meal replacement plan (MRP) or exercise training. Methods: Secondary analysis of DIASTOLIC: a randomised, open-label, blinded-endpoint trial of 12
[...] Read more.
Background: This study assesses the temporal responses of cardiovascular function, fibro-inflammation, and glucometabolic profiles in asymptomatic adults with type 2 diabetes, following a low-energy meal replacement plan (MRP) or exercise training. Methods: Secondary analysis of DIASTOLIC: a randomised, open-label, blinded-endpoint trial of 12 weeks MRP (~810 kcal/day) or exercise training. Cardiac magnetic resonance, plasma fibroinflammatory, and metabolic markers were undertaken at baseline, 4, and 12 weeks. Results: Out of 24 participants in the MRP group and 22 in exercise training, 18 and 11 completed all three visits. MRP resulted in early (0–4 weeks) improvement in insulin resistance (HOMA-IR: 10.82 to 4.32), decrease in FABP-4 (4.87 ± 0.19 to 5.15 ± 0.32 mg/L), and improvement in left ventricular remodelling LV mass: volume (0.86 ± 0.14 to 0.78 ± 0.11), all with large effect sizes. MMP8 levels increased moderately at 4–12 weeks. Peak early diastolic strain rate (cPEDSR) initially decreased, then improved. Exercise training led to minor improvements in insulin resistance and MMP-8 levels, with no significant changes in cPEDSR or LV remodelling. Conclusions: MRP resulted in early improvements in insulin resistance, cardiac remodelling, and inflammation, but with an initial decrease in diastolic function, improving by 12 weeks. Exercise training showed minor early benefits in insulin resistance and inflammation, but no significant cardiac changes.
Full article

Figure 1
Open AccessEditorial
Second Edition of the German–Austrian S3 Guideline “Infarction-Related Cardiogenic Shock: Diagnosis, Monitoring and Treatment”
by
Kevin Pilarczyk, Udo Boeken, Martin Russ, Josef Briegel, Michael Buerke, Alexander Geppert, Uwe Janssens, Malte Kelm, Guido Michels, Axel Schlitt, Holger Thiele, Stephan Willems, Uwe Zeymer, Bernhard Zwissler, Georg Delle-Karth, Markus Wolfgang Ferrari, Hans Reiner Figulla, Axel Heller, Gerhard Hindricks, Emel Pichler-Cetin, Burkert Pieske, Roland Prondzinsky, Johann Bauersachs, Ina Kopp, Karl Werdan and Matthias Thielmannadd
Show full author list
remove
Hide full author list
Hearts 2024, 5(1), 142-164; https://doi.org/10.3390/hearts5010010 - 14 Mar 2024
Abstract
►▼
Show Figures
The mortality of patients with MI has significantly decreased in recent decades, mainly due to early reperfusion therapy with a probability of surviving of more than 90% if the patient reaches the hospital [...]
Full article

Figure 1
Open AccessReview
Complications in Acute Myocardial Infarction: Navigating Challenges in Diagnosis and Management
by
Errol Moras, Shreyas Yakkali, Kruti D. Gandhi, Hafeez Ul Hassan Virk, Mahboob Alam, Syed Zaid, Nitin Barman, Hani Jneid, Saraschandra Vallabhajosyula, Samin K. Sharma and Chayakrit Krittanawong
Hearts 2024, 5(1), 122-141; https://doi.org/10.3390/hearts5010009 - 13 Mar 2024
Abstract
►▼
Show Figures
In recent decades, significant advancements in pharmacological, catheter-based, and surgical reperfusion technologies have markedly improved outcomes for individuals undergoing acute myocardial infarction. Despite these remarkable progressions, a segment of patients, particularly those with extensive infarctions or delays in revascularization, remains vulnerable to the
[...] Read more.
In recent decades, significant advancements in pharmacological, catheter-based, and surgical reperfusion technologies have markedly improved outcomes for individuals undergoing acute myocardial infarction. Despite these remarkable progressions, a segment of patients, particularly those with extensive infarctions or delays in revascularization, remains vulnerable to the onset of mechanical complications associated with myocardial infarction. These complications, spanning mechanical, electrical, ischemic, inflammatory, and thromboembolic events, pose substantial risks of morbidity, mortality, and increased utilization of hospital resources. The management of patients experiencing these complications is intricate, necessitating collaborative efforts among various specialties. Timely identification, accurate diagnosis, hemodynamic stabilization, and decision-making support are crucial for guiding patients and their families in choosing between definitive treatments or palliative care. This review underscores the critical importance of promptly identifying and initiating therapy to reduce prolonged periods of cardiogenic shock and the potential for fatality. By presenting key clinical and diagnostic insights, this review aims to further improve early diagnosis and offer an updated perspective on current management strategies for the diverse range of complications associated with acute myocardial infarction.
Full article

Figure 1
Open AccessReview
The Evolution and Complications of Long-Term Mechanical Circulatory Support Devices
by
Christian R. Sargent, Sabrina Ali and Venkateswarlu Kanamarlapudi
Hearts 2024, 5(1), 105-121; https://doi.org/10.3390/hearts5010008 - 28 Feb 2024
Abstract
Heart failure, a common clinical syndrome caused by functional and structural abnormalities of the heart, affects 64 million people worldwide. Long-term mechanical circulatory support can offer lifesaving treatment for end-stage systolic heart failure patients. However, this treatment is not without complications. This review
[...] Read more.
Heart failure, a common clinical syndrome caused by functional and structural abnormalities of the heart, affects 64 million people worldwide. Long-term mechanical circulatory support can offer lifesaving treatment for end-stage systolic heart failure patients. However, this treatment is not without complications. This review covers the major complications associated with implantable mechanical circulatory support devices, including strokes, pump thrombosis and gastrointestinal bleeding. These complications were assessed in patients implanted with the following devices: Novacor, HeartMate XVE, CardioWest, Jarvik 2000, HeartMate II, EVAHEART, Incor, VentrAssist, HVAD and HeartMate 3. Complication rates vary among devices and remain despite the introduction of more advanced technology, highlighting the importance of device design and flow patterns. Beyond clinical implications, the cost of complications was explored, highlighting the difference in costs and the need for equitable healthcare, especially with the expected rise in the use of mechanical circulatory support. Future directions include continued improvement through advancements in design and technology to reduce blood stagnation and mitigate high levels of shear stress. Ultimately, these alterations can reduce complications and enhance cost-effectiveness, enhancing both the survival and quality of life for patients receiving mechanical circulatory support.
Full article
(This article belongs to the Topic Mechanical Circulatory Support in Heart Failure)
►▼
Show Figures

Figure 1
Open AccessReview
An Update on the Use of Artificial Intelligence in Cardiovascular Medicine
by
Shiavax J. Rao, Shaikh B. Iqbal, Ameesh Isath, Hafeez Ul Hassan Virk, Zhen Wang, Benjamin S. Glicksberg and Chayakrit Krittanawong
Hearts 2024, 5(1), 91-104; https://doi.org/10.3390/hearts5010007 - 9 Feb 2024
Abstract
►▼
Show Figures
Artificial intelligence, specifically advanced language models such as ChatGPT, have the potential to revolutionize various aspects of healthcare, medical education, and research. In this review, we evaluate the myriad applications of artificial intelligence in diverse healthcare domains. We discuss its potential role in
[...] Read more.
Artificial intelligence, specifically advanced language models such as ChatGPT, have the potential to revolutionize various aspects of healthcare, medical education, and research. In this review, we evaluate the myriad applications of artificial intelligence in diverse healthcare domains. We discuss its potential role in clinical decision-making, exploring how it can assist physicians by providing rapid, data-driven insights for diagnosis and treatment. We review the benefits of artificial intelligence such as ChatGPT in personalized patient care, particularly in geriatric care, medication management, weight loss and nutrition, and physical activity guidance. We further delve into its potential to enhance medical research, through the analysis of large datasets, and the development of novel methodologies. In the realm of medical education, we investigate the utility of artificial intelligence as an information retrieval tool and personalized learning resource for medical students and professionals.
Full article

Figure 1
Open AccessSystematic Review
Inspiratory Muscle Training Intensity in Patients Living with Cardiovascular Diseases: A Systematic Review
by
Anaïs Beaujolin, Jessica Mané, Céline Presse, Jordana Barbosa-Silva, Michela Bernini, Camilo Corbellini and Raphael Martins de Abreu
Hearts 2024, 5(1), 75-90; https://doi.org/10.3390/hearts5010006 - 7 Feb 2024
Abstract
►▼
Show Figures
The benefits of inspiratory muscle training (IMT) have been demonstrated in patients with cardiovascular diseases (CVD); however, the optimal training intensity is not yet fully clarified. The purpose of this study was to review the impact of IMT intensity on respiratory muscle strength,
[...] Read more.
The benefits of inspiratory muscle training (IMT) have been demonstrated in patients with cardiovascular diseases (CVD); however, the optimal training intensity is not yet fully clarified. The purpose of this study was to review the impact of IMT intensity on respiratory muscle strength, functional and exercise capacity, pulmonary function, and quality of life in patients with CVD. This systematic review was carried out according to PRISMA statement and registered in the PROSPERO database (review protocol: CRD42023442378). Randomized controlled trials were retrieved on 3 July 2023 in the following electronic databases: Web of Science, PubMed, EMBASE, and SCOPUS. Studies were included if they assessed the impact of isolated IMT on CVD patients in comparison with sham, different intensities and/or intervention groups. Eight studies were included for final analysis; IMT consistently led to significantly greater improvements in inspiratory muscle strength compared to control (CON) groups. The intensity of IMT varied in the studies based on different percentages of maximal inspiratory pressure (MIP), ranging from 25% to 60% of MIP. The time of intervention ranged from 4 to 12 weeks. Despite this variability, the studies collectively suggested that IMT is beneficial for enhancing CVD patients’ conditions. However, the optimal intensity range for benefits appeared to vary, and no single intensity emerged as universally superior across all studies.
Full article

Graphical abstract
Open AccessReview
Different Mechanisms in Doxorubicin-Induced Cardiomyopathy: Impact of BRCA1 and BRCA2 Mutations
by
Hien C. Nguyen, Jefferson C. Frisbee and Krishna K. Singh
Hearts 2024, 5(1), 54-74; https://doi.org/10.3390/hearts5010005 - 23 Jan 2024
Cited by 3
Abstract
Germline mutations in Breast cancer susceptibility genes 1 and 2 (BRCA1 and BRCA2) cause breast, ovarian, and other cancers, and the chemotherapeutic drug doxorubicin (Dox) is widely used to treat these cancers. However, Dox use is limited by the latent induction of severe
[...] Read more.
Germline mutations in Breast cancer susceptibility genes 1 and 2 (BRCA1 and BRCA2) cause breast, ovarian, and other cancers, and the chemotherapeutic drug doxorubicin (Dox) is widely used to treat these cancers. However, Dox use is limited by the latent induction of severe cardiotoxicity known as Dox-induced cardiomyopathy, for which there are no specific treatments currently available. Dox is administered into the systemic circulation, where it readily translocates into sub-cellular compartments and disrupts the integrity of DNA. Accumulating evidence indicates that oxidative stress, DNA damage, inflammation, and apoptosis all play a central role in Dox-induced cardiomyopathy. The BRCA1 and BRCA2 proteins are distinct as they perform crucial yet separate roles in the homologous recombination repair of DNA double-strand breaks, thereby maintaining genomic integrity. Additionally, both BRCA1 and BRCA2 mitigate oxidative stress and apoptosis in both cardiomyocytes and endothelial cells. Accordingly, BRCA1 and BRCA2 are essential regulators of pathways that are central to the development of cardiomyopathy induced by Doxorubicin. Despite extensive investigations, there exists a gap in knowledge about the role of BRCA1 and BRCA2 in Doxorubicin-induced cardiomyopathy. Here, we review the previous findings and associations about the expected role and associated mechanisms of BRCA1 and 2 in Dox-induced cardiomyopathy and future perspectives.
Full article
(This article belongs to the Collection Feature Papers from Hearts Editorial Board Members)
►▼
Show Figures
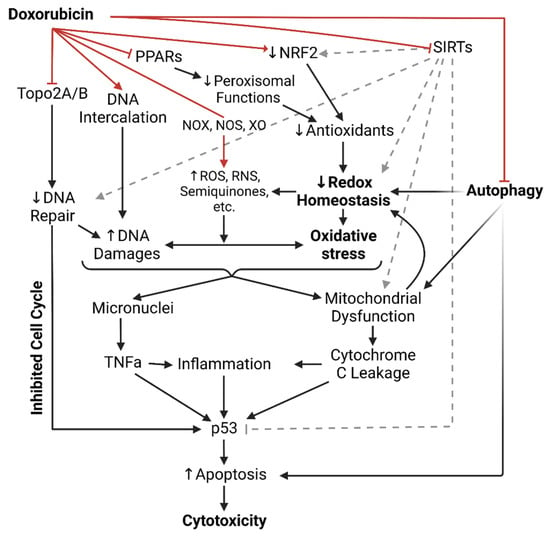
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Cardiogenetics, Hearts, JCDD, JCM, Medicina
Biomarkers in Cardiovascular Disease—Chances and Risks, 2nd Volume
Topic Editors: Alexander E. Berezin, Michael LichtenauerDeadline: 31 December 2025

Conferences
Special Issues
Special Issue in
Hearts
Current Developments in Coronary Artery Bypass Grafting
Guest Editor: Matthias ThielmannDeadline: 15 September 2024
Special Issue in
Hearts
Selected Papers from 72nd International Congress European Society of Cardiovascular Surgery
Guest Editors: Matthias Thielmann, Ergun Demirsoy, Igor B. KončarDeadline: 30 November 2024
Topical Collections
Topical Collection in
Hearts
Feature Papers from Hearts Editorial Board Members
Collection Editor: Matthias Thielmann





