- Article
Evaluation of the Efficacy of a Vibrotactile Device for Positional Therapy of Sleep-Disordered Breathing: A Pilot Study in Healthy Volunteers
- Andrey R. Alexandrov,
- Anton R. Kiselev and
- Ivan A. Kudashov
- + 2 authors
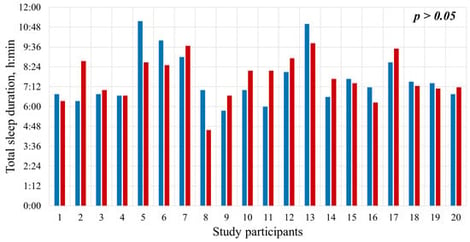
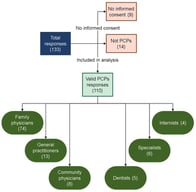
The role of body position during sleep, particularly the supine position, is now recognized as an important factor in the development of sleep-disordered breathing such as snoring, apnea, and hypopnea. This pilot study aimed to evaluate the efficacy of a new wearable vibrotactile device (SoftSleep) in reducing sleep time in the supine position without negatively affecting total sleep duration or perceived sleep quality. This pilot study included 20 healthy volunteers. Sleep was monitored over two consecutive nights: the first night without positional therapy (PT) and the second night using a PT device. The primary outcome measures were total sleep time, sleep duration in the supine position, number of position changes, and subjective sleep quality (using the modified Pittsburgh Sleep Quality Index). Use of SoftSleep showed a significant reduction in the mean proportion of sleep in the supine position from 56.01% to 7.84% (p < 0.001). Total sleep time did not change significantly (7:39 ± 1:33 vs. 7:42 ± 1:19; p > 0.05). A moderate increase in the number of position changes was not accompanied by a deterioration in subjective sleep quality: 90% of participants rated their sleep with the device as very good or fairly good. Only three participants reported brief awakenings, which did not affect their overall perception of nighttime rest. These results indicate that the SoftSleep device effectively promotes sleep in a non-supine position without altering sleep quality or subjective perception of sleep. The high tolerability of the device confirms its potential for further clinical evaluation in patients with positional sleep apnea.
16 March 2026