-
 In the Mouth or in the Gut? Innovation Through Implementing Oral and Gastrointestinal Health Science in Chronic Pain Management
In the Mouth or in the Gut? Innovation Through Implementing Oral and Gastrointestinal Health Science in Chronic Pain Management -
 An Overview of Severe Myalgic Encephalomyelitis
An Overview of Severe Myalgic Encephalomyelitis -
 Effectiveness of Pharmacological Treatments for Adult ADHD on Psychiatric Comorbidity: A Systematic Review
Effectiveness of Pharmacological Treatments for Adult ADHD on Psychiatric Comorbidity: A Systematic Review -
 Non-Surgical Correction of Facial Asymmetry: A Narrative Review of Non-Surgical Modalities and Clinical Case Examples
Non-Surgical Correction of Facial Asymmetry: A Narrative Review of Non-Surgical Modalities and Clinical Case Examples -
 Breast Imaging Findings in Women with Lipedema: A Retrospective Cross-Sectional Descriptive Study
Breast Imaging Findings in Women with Lipedema: A Retrospective Cross-Sectional Descriptive Study
Journal Description
Journal of Clinical Medicine
Journal of Clinical Medicine
is an international, peer-reviewed, open access journal of clinical medicine, published semimonthly online by MDPI. The International Bone Research Association (IBRA), Spanish Society of Hematology and Hemotherapy (SEHH), Japan Association for Clinical Engineers (JACE), European Independent Foundation in Angiology/ Vascular Medicine (VAS) and others are all affiliated with JCM, and their members receive a discount on article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: JCR - Q1 (Medicine, General and Internal) / CiteScore - Q1 (General Medicine)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 18.5 days after submission; acceptance to publication is undertaken in 2.7 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
- Companion journals for JCM include: Epidemiologia, Transplantology, Uro, Sinusitis, Rheumato, Journal of Clinical & Translational Ophthalmology, Journal of Vascular Diseases, Osteology, Complications, Therapeutics, Sclerosis, Pharmacoepidemiology and Journal of CardioRenal Medicine.
- Journal Clusters of Hematology: Hemato, Hematology Reports, Thalassemia Reports and Journal of Clinical Medicine.
Impact Factor:
2.9 (2024);
5-Year Impact Factor:
3.3 (2024)
Latest Articles
Impact of In-House 3D-Printed Models on Re-Operation Rates and Volumetric Precision in Orbital Floor Reconstruction: A Comparative Study
J. Clin. Med. 2026, 15(8), 2822; https://doi.org/10.3390/jcm15082822 (registering DOI) - 8 Apr 2026
Abstract
Background/Objectives: Reconstruction of orbital floor fractures remains surgically challenging due to limited intraoperative visibility and complex anatomy. Inaccurate implant placement often leads to persistent complications and the need for a revision surgery. This study evaluated the clinical accuracy and re-operation rates of
[...] Read more.
Background/Objectives: Reconstruction of orbital floor fractures remains surgically challenging due to limited intraoperative visibility and complex anatomy. Inaccurate implant placement often leads to persistent complications and the need for a revision surgery. This study evaluated the clinical accuracy and re-operation rates of a preoperative 3D-printed model-assisted technique compared to the conventional intraoperative free-hand mesh bending method. Methods: A comparative ambispective study was conducted on 74 patients with isolated orbital floor fractures. The control group (n = 34, retrospective) underwent reconstruction using intraoperatively formed titanium meshes. In the study group (n = 40, prospective), patient-specific 3D-printed models, created by mirroring the healthy contralateral orbit, were used for preoperative mesh adaptation. Primary outcomes included the rate of revision surgery due to implant malposition, changes in orbital volume, and postoperative diplopia. Results: The 3D model group demonstrated a significantly lower rate of revision surgery compared to the control group. In the retrospective group, 5 patients (15%) required reoperation due to implant malposition, whereas no patients (0%) in the prospective 3D group required secondary intervention (p = 0.017). While both techniques effectively restored orbital volume, the 3D group showed greater volumetric precision with less variance. The mean volume difference in the affected orbit was 3078 ± 2204 mm3 in the control group, compared to 2390 ± 1893 mm3 in the study 3D group. At the 6-month follow-up, persistent diplopia was observed in 12% of the control group compared to only 3% in the study group. Conclusions: The use of in-house 3D-printed models for preoperative mesh forming significantly enhances surgical precision and eliminates the need for revision surgery due to implant malposition. This workflow offers a cost-effective, predictable, and accessible alternative to expensive patient-specific implants (PSIs) or intraoperative navigation systems, improving patient safety and long-term clinical outcomes.
Full article
(This article belongs to the Special Issue Innovations in Maxillofacial Surgery)
►
Show Figures
Open AccessSystematic Review
Contraindications to Lateral Extra-Articular Tenodesis: A Systematic Review
by
Jakub Erdmann, Jan Czerwiński, Adam Kwapisz, Maria Zabrzyńska, Gazi Huri, Piotr Walus and Jan Zabrzyński
J. Clin. Med. 2026, 15(8), 2821; https://doi.org/10.3390/jcm15082821 (registering DOI) - 8 Apr 2026
Abstract
Background: Lateral extra-articular tenodesis (LET) is a surgical procedure that is additionally implemented in concurrent anterior cruciate ligament reconstruction (ACLR). Although numerous articles have addressed the use of LET in conjunction with ACLR, few definitive contraindications were identified. Given the scarcity of
[...] Read more.
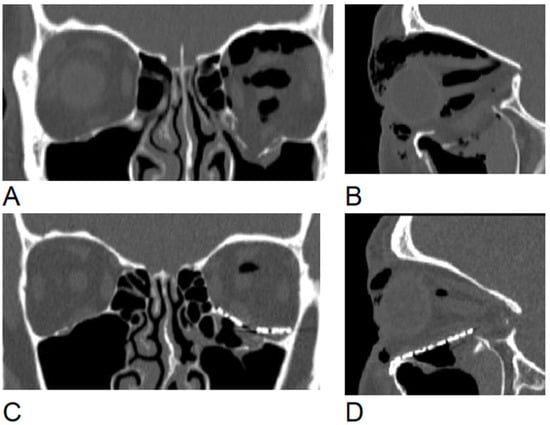
Background: Lateral extra-articular tenodesis (LET) is a surgical procedure that is additionally implemented in concurrent anterior cruciate ligament reconstruction (ACLR). Although numerous articles have addressed the use of LET in conjunction with ACLR, few definitive contraindications were identified. Given the scarcity of literature evaluating contraindications for LET modality, this study aimed to systematically review the reported contraindications of this procedure in the context of concurrent ACLR. Methods: The searched key terms: (extra-articular OR extraarticular) AND (tenodesis OR plasty OR augmentation OR procedure or reconstruction OR reconstructive OR surgical OR surgery OR technique) AND (ACL OR anterior cruciate ligament), with no publication date restrictions in PubMed, ScienceDirect, Cochrane Central, Web of Science, and Embase databases. We included clinical human studies, with levels of evidence I–III and in the English language. Results: The analysis evaluated fourteen articles published between 2012 and 2024. Level III evidence was found in the majority of studies (n = 9) and Level I evidence was found in the rest (n = 5). The majority of the included articles were retrospective (n = 8) and there were also prospective studies (n = 6). The articles reviewed showed that articular cartilage damage and concomitant injuries to other knee ligaments, alongside ACL injury, are the most frequently mentioned. Conclusions: This is the first study that systematized the contraindications for the LET procedure in ACLR. The contraindications remain unclear; however, the following may be highlighted: articular cartilage damage and injury to another ligament in the knee, in addition to ACL injury.
Full article
(This article belongs to the Special Issue Advances in Anterior Cruciate Ligament Injury Treatment)
►▼
Show Figures
Figure 1
Open AccessArticle
First Experience with Hypothermic Oxygenated Perfusion in Human Uteri: Feasibility and Metabolic Characterization
by
Keyue Sun, Nasim Eshraghi, Fernanda Walsh Fernandes, Sangeeta Satish, Chunbao Jiao, Fatma Selin Yildirim, Geofia Crasta, Omer F. Karakaya, Koki Takase, Hiroshi Horie, Karen S. Keslar, Dylan Isaacson, William Baldwin 3rd, Robert L. Fairchild, Koji Hashimoto, Alejandro Pita, Alvin Wee, Mariam AlHilli, Charles Miller, Mohamed Eltemamy, Tommaso Falcone, Andreas Tzakis, Elliot Richards and Andrea Schlegeladd
Show full author list
remove
Hide full author list
J. Clin. Med. 2026, 15(8), 2820; https://doi.org/10.3390/jcm15082820 (registering DOI) - 8 Apr 2026
Abstract
Background: Uterus transplantation (UTx) is an emerging treatment for absolute uterine factor infertility. However, the use of deceased donors is limited, and donation after circulatory death (DCD) has not yet been utilized. Ischemic injury remains a major barrier, particularly compared with living
[...] Read more.
Background: Uterus transplantation (UTx) is an emerging treatment for absolute uterine factor infertility. However, the use of deceased donors is limited, and donation after circulatory death (DCD) has not yet been utilized. Ischemic injury remains a major barrier, particularly compared with living donor procedures. Hypothermic oxygenated perfusion (HOPE), which has shown protective effects in heart, liver, and kidney transplantation, may offer similar benefits for uterine grafts. Methods: We report the first series applying HOPE to human uteri to improve preservation and enable metabolic injury assessment during perfusion. Six uteri (3 DBD, 3 DCD; median donor age 53 years) underwent 8 h of HOPE following procurement, while paired tissue controls were preserved using static cold storage (SCS). Perfusion was delivered using a pressure-controlled system (15 mmHg, 10 ± 1 °C, VitaSmart®). Perfusate and tissue samples were analyzed for mitochondrial injury, inflammation, and transcriptional responses. Results: HOPE maintained stable flows (70–150 mL/min), delivered high oxygen levels (pO2 ≈ 1000 hPa), and increased tissue ATP levels. Stratification based on perfusate flavin mononucleotide (FMN) release identified grafts with greater Complex I/II injury. HOPE was associated with lower levels of mitochondrial injury markers and inflammatory signals, preserved tissue architecture, and promoted gene expression patterns consistent with metabolic recovery compared with paired SCS tissue controls. Conclusions: These findings suggest that HOPE may serve as a preservation approach that enables metabolic and ischemic injury assessment and may facilitate broader use of deceased donor uteri for transplantation.
Full article
(This article belongs to the Special Issue New Advances in Uterus and Ovarian Transplantation: 2nd Edition)
►▼
Show Figures
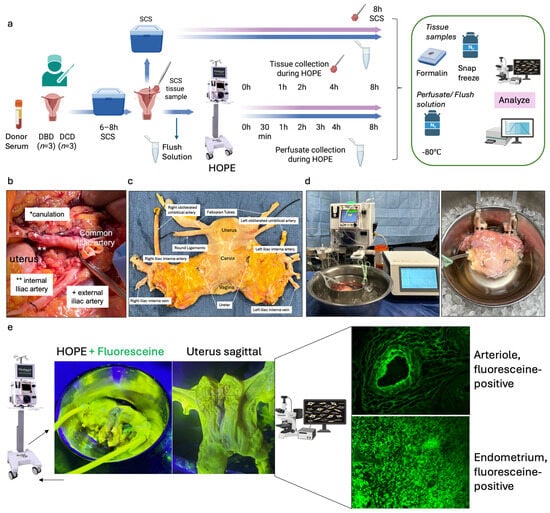
Figure 1
Open AccessReview
Insights into Acute Pancreatitis: Pathogenesis, Diagnosis, and Management
by
Silvia Carrara, Federico Cassano, Maria Terrin and Marco Spadaccini
J. Clin. Med. 2026, 15(8), 2819; https://doi.org/10.3390/jcm15082819 (registering DOI) - 8 Apr 2026
Abstract
This narrative review integrates landmark studies, recent publications, and major clinical guidelines to highlight the current state of the art concerning acute pancreatitis, a well-known yet still challenging condition. We will focus on recent practice transitions and future perspectives arising from advances in
[...] Read more.
This narrative review integrates landmark studies, recent publications, and major clinical guidelines to highlight the current state of the art concerning acute pancreatitis, a well-known yet still challenging condition. We will focus on recent practice transitions and future perspectives arising from advances in diagnostic imaging and interventional endoscopy. Pathogenesis and etiology: We carry out an overview of the fundamental mechanisms underlying acute pancreatitis, followed by an analysis of both common and uncommon causes, along with emerging evidence regarding idiopathic forms. Diagnosis and risk stratification: We pursue two objectives: on one hand, to emphasize the enduring importance of clinical assessment in the diagnosis of acute pancreatitis; on the other, to analyze the increasingly central role that imaging has acquired over recent decades. Identification of patients at higher risk for complications or an unfavorable prognosis is crucial. Several scoring systems have been proposed over the past decades, but with limited impact on daily clinical practice. Treatment: Therapeutic approaches have undergone significant revisions over time. Our objective is to provide an overview of the current standards together with best evidence-based medical approaches, targeted and interventional therapies, with focus on the endoscopic ones. Furthermore, we want to clarify the importance of nutrition and its proper management. Conclusions: Acute pancreatitis continues to stimulate discoveries and improvements in clinical management. We will place emphasis on unmet needs and emerging innovations that may importantly influence future practice also promoting evidenced-based standards of care.
Full article
(This article belongs to the Special Issue Insights into Acute Pancreatitis: Pathogenesis, Diagnosis, and Management)
►▼
Show Figures
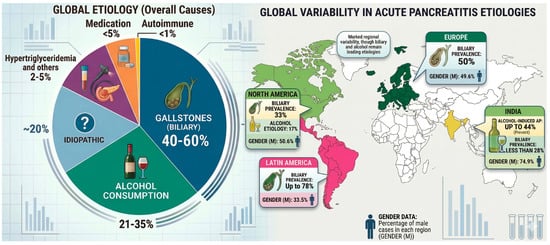
Figure 1
Open AccessArticle
Survival Outcomes After irAE-Related Nivolumab Discontinuation in mNSCLC: A Multicenter Study
by
Aysegul Merc Cetinkaya, Mehmet Haluk Yucel, Latif Karahan, Mustafa Ersoy, Ahmet Bilici, Mustafa Erman, Ali Murat Tatli and Sema Sezgin Goksu
J. Clin. Med. 2026, 15(8), 2818; https://doi.org/10.3390/jcm15082818 (registering DOI) - 8 Apr 2026
Abstract
Background: Immune checkpoint inhibitors (ICIs) such as nivolumab have transformed the treatment landscape of metastatic non-small cell lung cancer (NSCLC). We aimed to evaluate survival outcomes of patients who developed immune-related adverse events (irAEs) that required permanent treatment discontinuation. Methods: This
[...] Read more.
Background: Immune checkpoint inhibitors (ICIs) such as nivolumab have transformed the treatment landscape of metastatic non-small cell lung cancer (NSCLC). We aimed to evaluate survival outcomes of patients who developed immune-related adverse events (irAEs) that required permanent treatment discontinuation. Methods: This national, multicenter study included 25 patients with metastatic NSCLC from four tertiary oncology centers in Turkey. All patients received nivolumab monotherapy and discontinued treatment because of irAEs. Long-term survival was analyzed using Kaplan–Meier methods and compared indirectly with historical benchmarks. Results: The median overall survival (OS) was 35.73 months (95% CI: 30.06–41.40). The 2-year and 5-year OS rates were 78.9% and 27.0%, respectively. Median progression-free survival (PFS) was 16.23 months. Pneumonitis was the most frequent irAE (48%). Liver metastases significantly reduced OS (23.93 vs. 38.50 months, p = 0.005). In univariate analysis, ECOG 2 status (HR:22.07), bone metastases (HR:3.52), and subsequent systemic therapy (HR:30.19) weresignificant predictors of progression. Conclusions: Patients with metastatic NSCLC who discontinue nivolumab due to irAEs achieve notable survival outcomes, suggesting that treatment-limiting toxicity may signal a robust and durable antitumor immune response. These findings, though limited by a small cohort, highlight a distinct responder phenotype in real-world clinical practice.
Full article
(This article belongs to the Section Oncology)
►▼
Show Figures
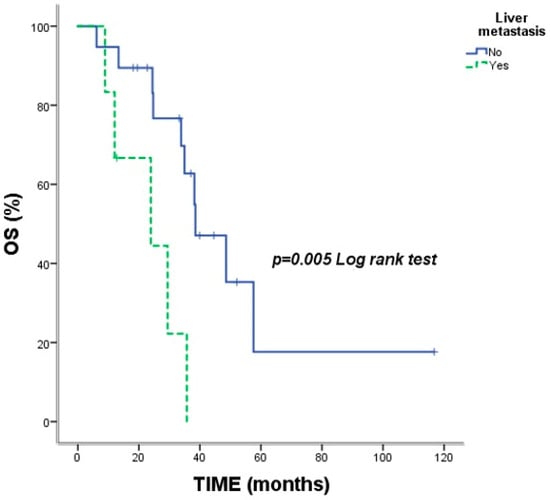
Figure 1
Open AccessSystematic Review
Factors Associated with Acute Colonic Pseudo-Obstruction After Cesarean Section: A Systematic Review and Meta-Analysis
by
Baorong Gao, Yali Miao, Hui Ye and Rui Miao
J. Clin. Med. 2026, 15(8), 2817; https://doi.org/10.3390/jcm15082817 (registering DOI) - 8 Apr 2026
Abstract
Objective: Acute colonic pseudo-obstruction (ACPO), also known as Ogilvie syndrome, is a rare but serious complication following cesarean section (CS). Identifying factors associated with its occurrence is critical for early recognition and prevention. This systematic review and meta-analysis aimed to synthesize available
[...] Read more.
Objective: Acute colonic pseudo-obstruction (ACPO), also known as Ogilvie syndrome, is a rare but serious complication following cesarean section (CS). Identifying factors associated with its occurrence is critical for early recognition and prevention. This systematic review and meta-analysis aimed to synthesize available evidence on factors associated with ACPO following CS. Methods: We performed a systematic literature search across five databases (PubMed, Embase, CNKI, Wanfang, and CBM) from inception to December 2025. Studies investigating factors associated with ACPO after CS were eligible. Quality of included studies was assessed using the Newcastle–Ottawa Scale. For factors reported in at least two studies, pooled odds ratios (ORs) or weighted mean differences (WMDs) with 95% confidence intervals (CIs) were calculated. Results: Five case-control studies comprising 484 patients (103 ACPO cases and 381 controls) were included, of which four were rated as good quality. Twenty-five potential associated factors were analyzed. Several pre-/intraoperative factors demonstrated statistically significant associations with ACPO risk, including concomitant anemia (OR = 8.94, 95% CI: 2.59–30.88), previous abdominal surgery (OR = 2.39, 95% CI: 1.28–4.47), surgery duration > 1 h (OR = 4.11, 95% CI: 2.20–7.67), and blood loss > 1000 mL (OR = 5.72, 95% CI: 2.10–15.58). Intraoperative blood loss as a continuous variable (WMD = 1.30, 95% CI: 0.14–2.46) was also significantly associated with ACPO. In contrast, emergency cesarean section, opioid use, and type of anesthesia were not significantly associated. Regarding postoperative features, bed rest > 12 h (OR = 2.66, 95% CI: 1.29–5.49), postoperative fever ≥ 38 °C (OR = 3.82, 95% CI: 1.94–7.54), elevated postoperative white blood cell count (WMD = 1.22, 95% CI: 0.30–2.14), and lower postoperative hemoglobin level (WMD = −0.50, 95% CI: −0.83 to −0.18) were significantly associated with ACPO. However, these factors may represent consequences of perioperative complications or components of the early clinical presentation of ACPO. Conclusions: This systematic review and meta-analysis identified multiple perioperative factors associated with ACPO following CS. However, the use of univariate data from a limited number of studies limits interpretability. Prospective cohort studies are needed to clarify whether these factors play a causal role in the development of ACPO.
Full article
(This article belongs to the Section Obstetrics & Gynecology)
►▼
Show Figures
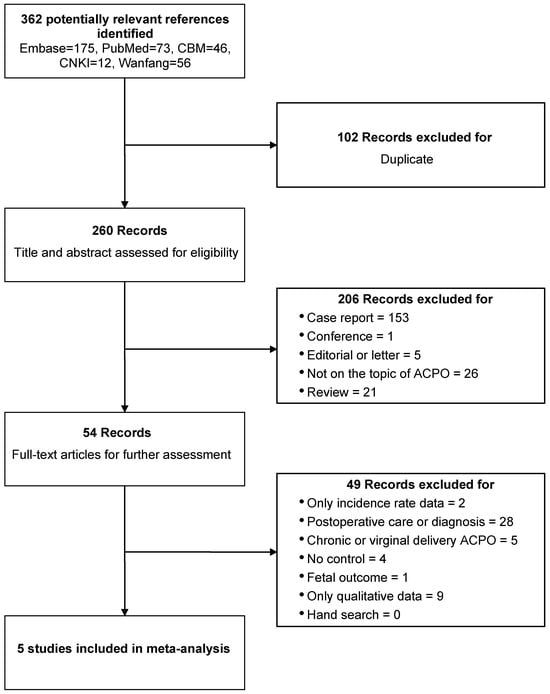
Figure 1
Open AccessArticle
The Quality of Life of Families of Children and Adolescents with Adolescent Idiopathic Scoliosis and the Adaptability and Cohesion of Families in the Patients’ Assessment
by
Barbara Cyran-Grzebyk, Gabriela Kołodziej-Lackorzyńska, Joanna Majewska, Daniel Szymczyk, Justyna Wyszyńska and Lidia Perenc
J. Clin. Med. 2026, 15(8), 2816; https://doi.org/10.3390/jcm15082816 (registering DOI) - 8 Apr 2026
Abstract
Objectives: Adolescent idiopathic scoliosis (AIS) may negatively affect both the quality of life of adolescents and the quality of life of their families (FQOL). Therefore, the analysis of objective and subjective determinants of FQOL in families of children and adolescents with AIS undergoing
[...] Read more.
Objectives: Adolescent idiopathic scoliosis (AIS) may negatively affect both the quality of life of adolescents and the quality of life of their families (FQOL). Therefore, the analysis of objective and subjective determinants of FQOL in families of children and adolescents with AIS undergoing long-term conservative treatment becomes important and will allow for a better understanding of factors that may have a significant impact on the prognosis and clinical treatment outcomes. Methods: The analysis covered a total of 200 families of children and adolescents aged 7–18 from the Podkarpackie region (Poland). The medical history chart and the original physical examination card, as well as the Family Adaptability and Cohesion Scales (FACES III) and the Family Quality of Life Scale (FQOL), were used in this study. Results: Families of adolescents without AIS demonstrated significantly higher levels of family cohesion and adaptability compared with families of adolescents with AIS (p < 0.001). The mean overall FQOL score was significantly lower in the AIS group (75.33 ± 9.18) than in the control group (86.97 ± 7.91; p < 0.001, rrb = 0.58). Multivariate analysis indicated that family adaptability was an independent predictor of FQOL in the AIS group, with higher adaptability associated with lower overall FQOL and reduced scores in parental functioning and emotional well-being domains. Conclusions: A long process of AIS treatment can cause crisis situations for patients and their families and influences both the physical and mental health of patients by changing their family’s quality of life (FQOL). Early identification of families characterized by diminished cohesion and adaptability enables the integration of psychopedagogical support and family consultations into standardized care. Such a multidimensional approach may enhance therapeutic prognosis and accelerate the rehabilitation process.
Full article
(This article belongs to the Special Issue Breakthroughs in Spine Biomechanics: Diagnostics and Treatment Approaches for Body Posture, Scoliosis and Chronic Back Pain)
Open AccessArticle
Acute Effects of High-Load Training to Failure vs. Non-Failure on Posture and Core Endurance in Collegiate Weightlifters: A Crossover Study
by
Osama R. Abdelraouf, Amr A. Abdel-Aziem, Nouf H. Alkhamees, Zizi M. Ibrahim, Ehab M. Aboelela, Reem S. Dawood and Ahmed A. Ashour
J. Clin. Med. 2026, 15(8), 2815; https://doi.org/10.3390/jcm15082815 (registering DOI) - 8 Apr 2026
Abstract
Background: Weightlifters commonly use upper-extremity high-load training, which encompasses techniques ranging from momentary failure to non-failure. However, little is known about how this training affects posture and core endurance, despite knowing that these factors are risk factors for weightlifting injuries. Therefore, this study
[...] Read more.
Background: Weightlifters commonly use upper-extremity high-load training, which encompasses techniques ranging from momentary failure to non-failure. However, little is known about how this training affects posture and core endurance, despite knowing that these factors are risk factors for weightlifting injuries. Therefore, this study aimed to determine the immediate effects of upper-extremity high-load training to momentary failure versus non-failure, using the dumbbell overhead press, on posture and core endurance in recreational collegiate weightlifters. Methods: Fifty recreational weightlifters aged 18–24 with two years of upper extremity resistance training experience were recruited for this study. The participants performed dumbbell overhead press exercises under high-load failure (HL-F) and high-load non-failure (HL-NF) conditions two days after 1RM testing and calculation of the 80% 1RM load. The study analyzed postural changes using photographic data processed in Kinovea, while core endurance was assessed during a prone plank test. Standardized warm-ups, controlled exercise execution, and pre- and post-exercise assessments were conducted to measure core endurance and postural alterations. Results: The thoracic kyphosis angle, together with scapular balance angle and lateral scapular slide distance, increased significantly after HL-F compared to the unloading state, while the craniovertebral angle and prone plank time decreased significantly (p < 0.05). The HL-NF condition showed no statistically significant differences relative to the unloading measurements (p > 0.05). The unloading measurements across testing days were consistent, indicating no carryover effect (p > 0.05). Conclusions: The findings indicate that high-load training to failure adversely affects posture and core endurance, increasing fatigue and potentially increasing the risk of acute injuries. Non-failure training maintains stability, underscoring the importance of strategic program design for achieving optimal performance while minimizing adverse effects.
Full article
(This article belongs to the Special Issue Movement Analysis in Rehabilitation)
►▼
Show Figures
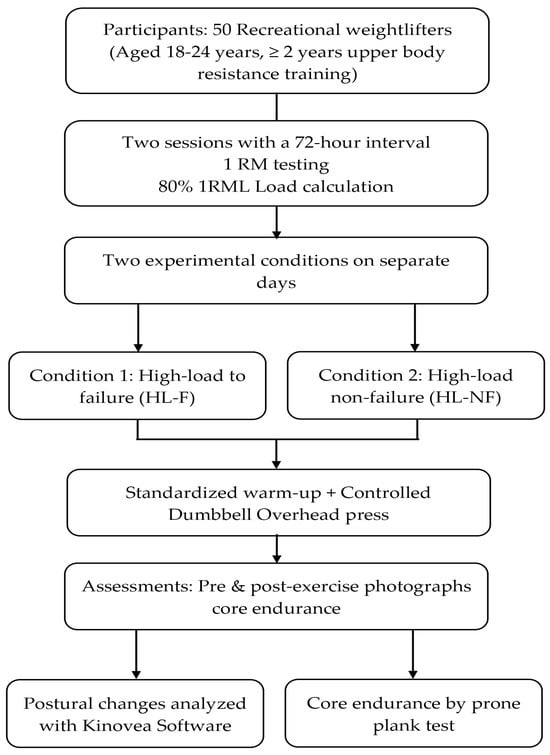
Figure 1
Open AccessArticle
Management of Hemothorax After Blunt Chest Trauma: Results from a Level II Emergency Department
by
Dania Nachira, Antonio Giulio Napolitano, Adriana Nocera, Maria Teresa Congedo, Marcello Covino, Claudia Bellettati, Claudia Leoni, Chiara Scognamiglio, Giovanni Punzo, Mariano Alberto Pennisi, Nicola Bonadia, Maria Letizia Vita, Leonardo Petracca-Ciavarella, Filippo Lococo, Elisa Meacci and Stefano Margaritora
J. Clin. Med. 2026, 15(8), 2814; https://doi.org/10.3390/jcm15082814 (registering DOI) - 8 Apr 2026
Abstract
Background: Traumatic hemothorax is a common complication of blunt chest trauma and remains associated with significant morbidity and mortality. Although contrast-enhanced computed tomography (CT) is central to diagnosis, the optimal criteria for selecting patients who require invasive management versus conservative treatment remain unclear.
[...] Read more.
Background: Traumatic hemothorax is a common complication of blunt chest trauma and remains associated with significant morbidity and mortality. Although contrast-enhanced computed tomography (CT) is central to diagnosis, the optimal criteria for selecting patients who require invasive management versus conservative treatment remain unclear. This study aimed to evaluate the management strategies and clinical outcomes of traumatic hemothorax and to identify predictors of surgical intervention and postoperative complications. Methods: We conducted a retrospective, single-center cohort study including adult patients admitted to a Level II Emergency Department with hemothorax following blunt chest trauma between January 2019 and December 2024. Primary outcomes were the need for urgent chest drainage or surgery. Secondary outcomes included postoperative complications, length of hospital stay, and intensive care unit admission. Univariable and multivariable regression analyses were performed to identify factors associated with surgical intervention and complications. Results: Seventy-two patients were included (mean age 60.0 ± 20.5 years; 80.6% male). Rib fractures were the most common cause of hemothorax (61.1%). Chest tube placement was required in 70.8% of cases, and 31.9% underwent urgent surgical intervention. Active bleeding on contrast-enhanced CT was identified in 16.7% of patients and was the only independent predictor of urgent surgery (OR 3.85, 95% CI 1.07–13.88; p = 0.039). The initial volume of blood drained after chest tube insertion did not differ between surgically and non-surgically managed patients. Conservative management was successful in 19.4% of cases. Postoperative complications occurred in five patients and were associated with a higher comorbidity burden. Overall mortality was 5.6%. Conclusions: In traumatic hemothorax following blunt chest trauma, active bleeding on contrast-enhanced CT seems to be the strongest predictor of urgent surgical intervention, whereas initial pleural drainage volume alone is not. Conservative management is safe in selected patients, while comorbidities influence postoperative outcomes. Multidisciplinary management and accurate radiological assessment are essential to guide timely and appropriate treatment.
Full article
(This article belongs to the Special Issue Clinical Update on Thoracic Trauma)
►▼
Show Figures
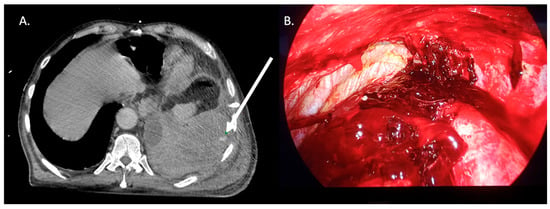
Figure 1
Open AccessSystematic Review
Timing and Outcomes of Cranioplasty After Decompressive Craniectomy: A Systematic Review of Neurological Recovery, Complications, and Predictive Factors
by
András Gati, Árpád Viola, Yousif Qais Al-Khafaji, Siran Aslan, Mustafa Qais Al-Khafaji, Yousif Asaad Taha, Murtadha Qais Al-Khafaji, Georgia Koudigkeli, Shahad Qais Al-Khafaji and Mohammad Walid Al-Smadi
J. Clin. Med. 2026, 15(8), 2813; https://doi.org/10.3390/jcm15082813 - 8 Apr 2026
Abstract
Background: The optimal timing of cranioplasty (CP) after decompressive craniectomy (DC) remains debated. Early reconstruction may enhance neurological recovery through restoration of cerebral perfusion and cerebrospinal fluid dynamics, yet concerns persist regarding postoperative complications. Objective: To evaluate the impact of early versus delayed
[...] Read more.
Background: The optimal timing of cranioplasty (CP) after decompressive craniectomy (DC) remains debated. Early reconstruction may enhance neurological recovery through restoration of cerebral perfusion and cerebrospinal fluid dynamics, yet concerns persist regarding postoperative complications. Objective: To evaluate the impact of early versus delayed cranioplasty on neurological outcomes and postoperative complications in adults following decompressive craniectomy. Methods: A systematic review was conducted in accordance with PRISMA guidelines (PROSPERO ID: CRD420251123808). PubMed, OVID, and Web of Science were searched for studies published between January 2017 and December 2025. Eligible studies compared early and delayed CP in adults and reported neurological outcomes and/or complications. Results: Twenty-one retrospective cohort studies including 8462 patients were analyzed. Neurological improvement was observed in both groups across multiple validated scales (GOSE, GOS, GCS, mRS, BI, FIM, NIHSS, MMSE). Early CP was consistently associated with superior recovery, including higher one-year Barthel Index improvement (74.1% vs. 54.8%), greater FIM gains (7.31% vs. 4.66%), and higher composite recovery rates (95.6% vs. 80.0%). No study demonstrated superior recovery with delayed CP. Infection, hydrocephalus, and seizure rates were comparable between groups. However, hematoma (21% vs. 10.4%) and hygroma (7.49% vs. 4.73%) were more frequent after early CP, although hematoma rates were influenced by a large database study. Bone flap resorption was less frequent with early CP (1.44% vs. 6.26%). Conclusions: Early cranioplasty is associated with improved neurological recovery but carries an increased risk of select complications, particularly hematoma and hygroma, representing a clinically relevant trade-off. Delayed CP does not demonstrate overall superior safety due to higher bone flap resorption. Timing should be individualized, and prospective multicenter studies with standardized definitions are needed.
Full article
(This article belongs to the Special Issue Clinical Management of Traumatic Brain Injury)
►▼
Show Figures
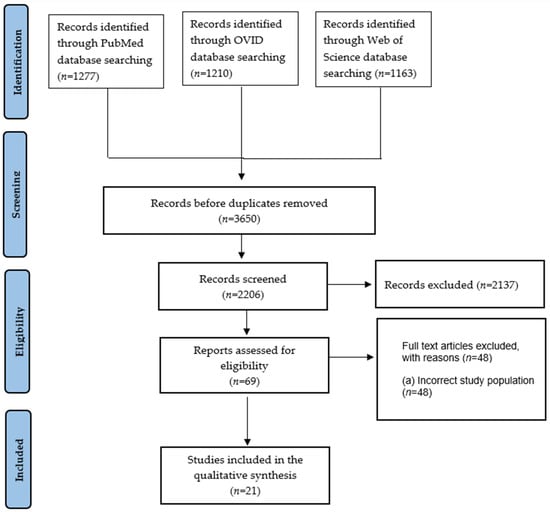
Figure 1
Open AccessArticle
Comparative Safety and Volume Trends in Gastrostomy Tube Placement: Percutaneous Endoscopic Versus Percutaneous Radiologic Approaches at a Single Center
by
Yazan Omari, Bradley Kapten, Saif Affas, Dima Sallam, Serge Sorser and Leonid Shamban
J. Clin. Med. 2026, 15(8), 2812; https://doi.org/10.3390/jcm15082812 - 8 Apr 2026
Abstract
Background: Percutaneous endoscopic gastrostomy (PEG) and percutaneous radiologic gastrostomy (PRG) are established techniques for long-term enteral access. Contemporary comparisons of complication patterns, length of stay (LOS), and utilization trends remain limited. Methods: We conducted a retrospective cohort study of adult patients undergoing initial
[...] Read more.
Background: Percutaneous endoscopic gastrostomy (PEG) and percutaneous radiologic gastrostomy (PRG) are established techniques for long-term enteral access. Contemporary comparisons of complication patterns, length of stay (LOS), and utilization trends remain limited. Methods: We conducted a retrospective cohort study of adult patients undergoing initial gastrostomy placement at a single academic center between 2021 and 2024 (n = 341). The primary outcome was any 30-day procedure-related complication. Secondary outcomes included complication subtypes, LOS, and procedural volume trends. Multivariable regression analyses were performed to adjust for potential confounders. Results: Among 341 patients, 195 underwent PEG and 146 PRG. Overall complication rates were similar (PEG 16.4% vs. PRG 14.4%, p = 0.31). Infectious complications were numerically higher with PEG (4.1% vs. 1.4%), though not statistically significant. Mean LOS was 3.2 days for PEG and 2.8 days for PRG (p = 0.12). On multivariable analysis, gastrostomy technique was not associated with complications (aOR 0.88, 95% CI 0.48–1.61) or LOS. PRG utilization increased substantially over the study period, comprising 60.7% of procedures by 2024. Conclusions: PEG and PRG demonstrated no statistically significant differences in safety outcomes, with no statistically significant differences in complications or LOS. A marked shift toward PRG utilization was observed over time. These findings support individualized, patient-centered selection of gastrostomy technique, while acknowledging limited power to detect small but clinically meaningful differences.
Full article
(This article belongs to the Section Gastroenterology & Hepatopancreatobiliary Medicine)
►▼
Show Figures
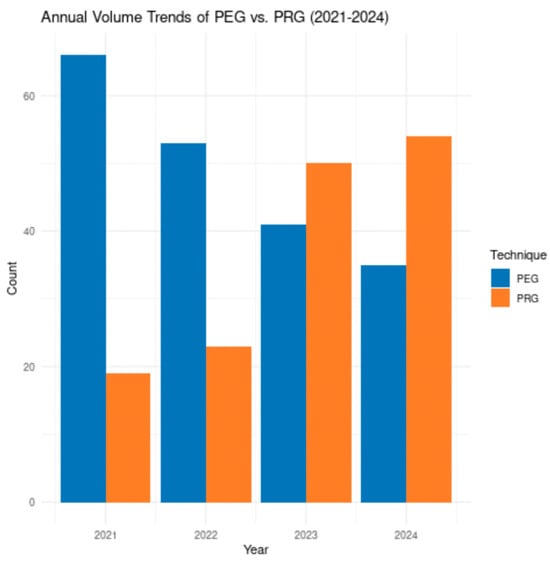
Figure 1
Open AccessReview
Thrombosis in Neuromuscular Medicine: Current Evidence, Unmet Needs, and Future Directions
by
Zhi Xuan Quak, Furene Wang, Stacey K. H. Tay, Pei Lin Koh, Eng Soo Yap and Kay Wei Ping Ng
J. Clin. Med. 2026, 15(8), 2810; https://doi.org/10.3390/jcm15082810 - 8 Apr 2026
Abstract
Venous thromboembolism (VTE), comprising deep vein thrombosis and pulmonary embolism, is an important but under-recognised complication in neuromuscular diseases. In adults, emerging epidemiological data suggests increased VTE occurrence in conditions such as Amyotrophic Lateral Sclerosis, myotonic dystrophy, myasthenia gravis, inflammatory neuropathies, inflammatory myopathies,
[...] Read more.
Venous thromboembolism (VTE), comprising deep vein thrombosis and pulmonary embolism, is an important but under-recognised complication in neuromuscular diseases. In adults, emerging epidemiological data suggests increased VTE occurrence in conditions such as Amyotrophic Lateral Sclerosis, myotonic dystrophy, myasthenia gravis, inflammatory neuropathies, inflammatory myopathies, and POEMS syndrome. This heightened risk reflects not only disease-related immobility but also disorder-specific biological mechanisms, including inflammation, endothelial dysfunction and cardiomyopathy-related stasis. Therapies such as corticosteroids, IVIG-related hyperviscosity, long-term central venous access, perioperative immobility, critical illness, and complex orthopaedic procedures have prothrombotic effects. Despite this multifactorial risk profile, disease-specific guidance for thromboprophylaxis is lacking, and current practice relies heavily on extrapolation from general medical and surgical recommendations rather than data derived from neuromuscular cohorts. In children and adolescents, the VTE burden is less well-characterised, but events have been reported in Duchenne and Becker muscular dystrophy, congenital myopathies, and spinal muscular atrophy particularly with advanced motor impairment, severe cardiomyopathy, ventilatory insufficiency, and prolonged hospitalisation. Beyond venous events, selected neuromuscular disorders also exhibit increased arterial thrombosis risk. Myotonic dystrophy and dystrophinopathies are associated with cardiomyopathy and arrhythmia that predispose to systemic embolism and stroke, while inflammatory myopathies may demonstrate arterial events related to vasculitic or endothelial processes, although overall evidence remains limited. This review summarises available empirical and epidemiological evidence on venous and arterial thrombosis across adult and paediatric neuromuscular disorders, outlines disease-specific mechanistic pathways, examines treatment-related contributors, and highlights key evidence gaps that must be addressed to guide rational and targeted prophylaxis strategies in this complex, heterogeneous population.
Full article
(This article belongs to the Special Issue Neuromuscular Diseases and Musculoskeletal Disorders)
Open AccessCorrection
Correction: Perilli et al. Early Diagnostic Markers in Crisponi Syndrome: Two Cases and Review. J. Clin. Med. 2025, 14, 7757
by
Lorenzo Perilli, Kamil Dzwilewski, Marta Pietruszka, Pasquale Striano, Giuseppe Capovilla and Maria Mazurkiewicz-Bełdzinska
J. Clin. Med. 2026, 15(8), 2809; https://doi.org/10.3390/jcm15082809 - 8 Apr 2026
Abstract
In the original publication [...]
Full article
(This article belongs to the Section Clinical Pediatrics)
►▼
Show Figures
Figure 1
Open AccessSystematic Review
Mapping the Prevalence and Risk Factors of Low Back Pain Among University Populations in Saudi Arabia: A Systematic Review and Meta-Analysis
by
Sulaiman Alanazi, Jana Alruwaili, Maysam Alruwaili, Abdulmajeed Alfayyadh, Hadeel Alsirhani, Samaher Mohammed Alowaydhah, Sultan A. Alanazi, Nesma M. Allam and Sara Elsebahy
J. Clin. Med. 2026, 15(7), 2808; https://doi.org/10.3390/jcm15072808 - 7 Apr 2026
Abstract
Background/Objectives: Low back pain (LBP) is one of the most common musculoskeletal conditions globally and a leading cause of disability. University populations may be particularly vulnerable due to prolonged sitting, academic stress, and frequently suboptimal ergonomics, especially in rapidly expanding higher education
[...] Read more.
Background/Objectives: Low back pain (LBP) is one of the most common musculoskeletal conditions globally and a leading cause of disability. University populations may be particularly vulnerable due to prolonged sitting, academic stress, and frequently suboptimal ergonomics, especially in rapidly expanding higher education systems such as those in Saudi Arabia. This systematic review and meta-analysis aimed to synthesize evidence on the prevalence of LBP among university attendants in Saudi Arabia and to quantify its associations with key demographic and environmental risk factors. Methods: We systematically reviewed observational studies reporting LBP prevalence and/or risk factors among university students and faculty in Saudi Arabia published in English, following Cochrane methodological guidance and PRISMA 2020 reporting recommendations. The protocol was prospectively registered in PROSPERO (CRD420250654048). We searched PubMed, Embase and CINAHL from inception to February 2025. Two reviewers independently screened studies, extracted data, and assessed risk of bias using the Joanna Briggs Institute checklist for analytical cross-sectional studies. Random effects meta-analyses were used to pool prevalence estimates across recall periods, regions, populations, and measurement tools, and to calculate pooled odds ratios (ORs) for age, sex, smoking, family history of LBP, and college seating conditions. Heterogeneity, subgroup, and sensitivity analyses were undertaken. Results: Thirteen cross-sectional studies were included. The overall pooled prevalence of LBP was 57% (95% confidence interval [CI] approximately 43–71), with substantial heterogeneity. Prevalence varied by recall period, region, population group, and measurement instrument; pooled prevalence was 58% among students and 50% among faculty. Increasing age (OR 1.17, 95% CI 1.01–1.34) and poor college seating conditions (OR 1.42, 95% CI 1.07–1.76) were significantly associated with LBP. Male gender, smoking, and family history showed non-significant pooled effects. These estimates are limited by substantial between-study heterogeneity, variable measurement tools, and exclusively cross-sectional designs, which restrict causal inference. Conclusions: LBP is prevalent among university attendants in Saudi Arabia, affecting both students and faculty. The consistent associations with age and seating ergonomics highlight the need for ergonomic classroom redesign and age-sensitive preventive strategies. Future work should adopt standardized LBP measures and longitudinal designs to clarify causal pathways and evaluate targeted interventions. Funding: This work was supported by the Deanship of Graduate Studies and Scientific Research at Jouf University (grant DGSSR-2026-NF-01-002).
Full article
(This article belongs to the Special Issue Evidence-Based Diagnosis and Clinical Management of Low Back Pain)
►▼
Show Figures

Figure 1
Open AccessArticle
Treatment Regret in Patients Undergoing Minimally Invasive Treatments for Benign Prostatic Hyperplasia
by
Riccardo Lombardo, Antonio Luigi Pastore, Beatrice Turchi, Antonio Franco, Matteo Romagnoli, Yazan Al Salhi, Andrea Fuschi, Cristian Fiori, Silvia Secco, Sabrina De Cillis, Alberto Olivero, Antonio Nacchia, Antonio Cicione, Luca Cindolo, Giorgia Tema, Andrea Tubaro and Cosimo De Nunzio
J. Clin. Med. 2026, 15(7), 2807; https://doi.org/10.3390/jcm15072807 - 7 Apr 2026
Abstract
Background: The aim of this study was to evaluate treatment satisfaction and decision regret in patients undergoing minimally invasive surgical therapies (MISTs) for lower urinary tract symptoms (LUTS) due to benign prostatic hyperplasia (BPH). Materials and Methods: We analyzed prospectively collected data from
[...] Read more.
Background: The aim of this study was to evaluate treatment satisfaction and decision regret in patients undergoing minimally invasive surgical therapies (MISTs) for lower urinary tract symptoms (LUTS) due to benign prostatic hyperplasia (BPH). Materials and Methods: We analyzed prospectively collected data from consecutive patients undergoing MISTs across five Italian primary care urology centers. All patients underwent a comprehensive clinical assessment, including detailed medical history and physical examination. Preoperative, perioperative, and postoperative variables were recorded. Decision regret was assessed using validated questionnaires, with significant regret defined as a score >25%. Results: A total of 155 patients were included, with a median age of 64 years (IQR 58–66) and a median IPSS of 23 (IQR 18–26). Among them, 90 patients (51%) underwent Aquablation, 21 (12%) received a temporary implantable nitinol device (iTIND), 26 (15%) underwent water vapor thermal therapy (WVTT), and 37 (21%) were treated with prostatic urethral lift (PUL). The overall median decision regret score was 0 (IQR 0–15), with 23 patients (15%) reporting significant regret (>25%). Higher regret rates were observed in patients treated with PUL and WVTT compared to those undergoing iTIND and Aquablation. None of the evaluated variables—including age, BMI, prostate volume, preoperative Qmax, or preoperative IPSS—were significantly associated with treatment regret. However, although not reaching statistical significance, a prostate volume >60 cc was associated with higher regret in patients undergoing WVTT (OR = 3.33) and PUL (OR = 4.2). Conclusions: Among patients undergoing MISTs, treatment regret is not negligible and appears higher when patient selection is suboptimal. Larger studies are warranted to better identify predictors of decision regret and optimize patient selection for these procedures.
Full article
(This article belongs to the Special Issue Emerging Surgical Techniques in the Management of Urological Diseases)
Open AccessArticle
Comparisons of Respiratory Function and Cardiorespiratory Responses Induced by the Modified Shuttle Walk Test in Children Finswimmers and Age-Matched Sedentary Non-Athletes
by
Theano Michailidou, Aspasia Mavronasou and Eleni A. Kortianou
J. Clin. Med. 2026, 15(7), 2806; https://doi.org/10.3390/jcm15072806 (registering DOI) - 7 Apr 2026
Abstract
Background: Regular aerobic exercise during childhood promotes critical physiological adaptations in the cardiovascular and respiratory system. Finswimming, a unique aquatic sport, requires high-intensity demands and specific breathing patterns. The present study aimed to compare respiratory function and cardiorespiratory responses between young male
[...] Read more.
Background: Regular aerobic exercise during childhood promotes critical physiological adaptations in the cardiovascular and respiratory system. Finswimming, a unique aquatic sport, requires high-intensity demands and specific breathing patterns. The present study aimed to compare respiratory function and cardiorespiratory responses between young male finswimmers and sedentary age-matched non-athletes. Methods: Thirty-two boys aged 8 to 12 years old were stratified into the finswimmers group (FSG, n = 16) and the non-athletes group (NAG, n = 16). Assessments included pulmonary function (spirometry) and respiratory muscle strength (Maximum Inspiratory Pressure, MIP/Maximum Expiratory Pressure, MEP). Exercise capacity was evaluated using the modified shuttle walk test (MSWT). Results: The FSG exhibited significantly higher pulmonary function (Forced Vital Capacity, Forced Expiratory Volume in 1 s, Maximum Voluntary Ventilation; p < 0.05) and superior MIP compared to the NAG (105.3 ± 24.8 versus 87.3 ± 24.7 cmH2O; p = 0.022). During the MSWT, FSG covered substantially greater distances (746.6 ± 97.2 versus 591.1 ± 86.4 m; p < 0.001) with lower levels of leg fatigue (Borg 0–10) (0.53 ± 0.39 versus 2.13 ± 1.93; p = 0.004) and demonstrated lower heart rate recovery time (4.47 ± 0.68 versus 5.75 ± 0.68 min; p < 0.001) compared to NAG. At the iso-level (8th level of MSWT), FSG scored lower levels of leg fatigue (0.13 ± 0.12 versus 2.02 ± 2.0; p = 0.001) compared to NAG, indicating better peripheral oxygen % saturation (100 ± 0.0 versus 98.14 ± 1.16; p < 0.001). Conclusions: Systematic exercise training enhances profound cardiorespiratory and peripheral muscle adaptations in children. Enhanced cardiorespiratory function allows young athletes to achieve higher workloads and recover faster than sedentary peers, highlighting the sport’s role in establishing a robust cardiorespiratory fitness.
Full article
(This article belongs to the Special Issue Insights and Innovations in Sports Cardiology)
►▼
Show Figures
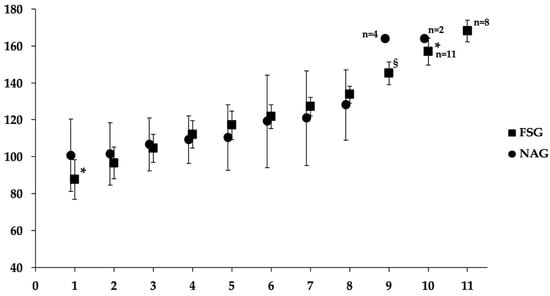
Figure 1
Open AccessArticle
Bevacizumab-Based Therapy Is Associated with Prolonged Progression-Free Survival in Patients with Peritoneal Mucinous Metastatic Colorectal Cancer
by
Süleyman Can, Veli Çakıcı, Gizem Bakır Kahveci, Şeyma Eroğlu, Burak Tok, Gökhan Uygun, Esra Özer, Yalçın Çırak and İvo Gökmen
J. Clin. Med. 2026, 15(7), 2805; https://doi.org/10.3390/jcm15072805 - 7 Apr 2026
Abstract
Objective: In metastatic colorectal cancer (mCRC), mucinous histology has been associated with poor clinical outcomes, particularly in the presence of peritoneal metastasis. However, it remains unclear whether mucinous histology exerts a context-dependent effect on treatment outcomes by modifying the efficacy of anti-vascular endothelial
[...] Read more.
Objective: In metastatic colorectal cancer (mCRC), mucinous histology has been associated with poor clinical outcomes, particularly in the presence of peritoneal metastasis. However, it remains unclear whether mucinous histology exerts a context-dependent effect on treatment outcomes by modifying the efficacy of anti-vascular endothelial growth factor (VEGF)-based therapies independently of metastatic dissemination patterns and chemotherapy backbone. Methods: We retrospectively analyzed 250 patients with mCRC treated with bevacizumab-containing systemic therapy. Tumors were classified as mucinous (n = 52) or non-mucinous (n = 198). Progression-free survival (PFS) and overall survival (OS) were estimated using the Kaplan–Meier method and compared using the log-rank test. Cox proportional hazards regression models were applied for univariate and multivariate analyses. Predefined subgroup analyses were conducted according to peritoneal metastasis status and chemotherapy backbone (oxaliplatin- or irinotecan-based). A 6-month landmark analysis was performed to reduce early progression bias. Interaction analyses evaluated potential effect modification between histology, peritoneal metastasis, and chemotherapy backbone. Results: Mucinous tumors were more frequently right-sided and strongly associated with peritoneal metastasis. In the overall cohort, mucinous histology was associated with significantly longer median PFS compared with non-mucinous histology (22.9 vs. 11.9 months; p < 0.001). This benefit was driven by patients with peritoneal metastasis, in whom mucinous histology was associated with markedly prolonged PFS (23.9 vs. 8.7 months; p < 0.001). No significant PFS difference according to histology was observed in patients without peritoneal metastasis. On multivariate analysis, mucinous histology remained independently associated with improved PFS (HR 0.44; 95% CI 0.25–0.78; p = 0.005), an effect preserved in the landmark cohort (HR 0.39; 95% CI 0.26–0.59; p < 0.001). A significant interaction between mucinous histology and peritoneal metastasis was observed (p for interaction = 0.040), indicating that the prognostic impact of histology differed according to metastatic pattern. No significant PFS difference or interaction was detected according to chemotherapy backbone within the mucinous subgroup. Conclusions: Among bevacizumab-treated patients with mCRC, mucinous histology—particularly in the presence of peritoneal metastasis—is associated with a pronounced PFS advantage independent of chemotherapy backbone. These findings suggest that mucinous peritoneal mCRC represents a biologically and clinically distinct subgroup that may derive context-specific and disproportionate benefit from anti-VEGF-based strategies, warranting prospective validation.
Full article
(This article belongs to the Special Issue Colorectal Cancer: Screening, Diagnosis and Treatment)
►▼
Show Figures
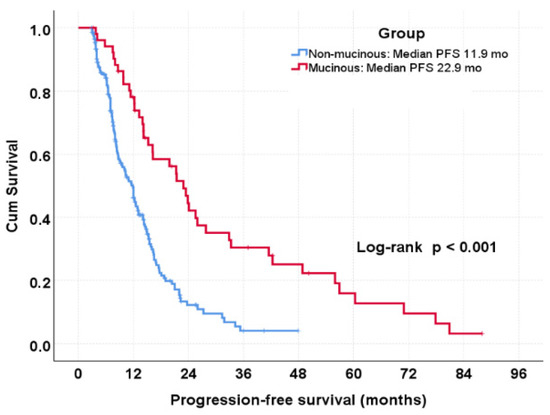
Figure 1
Open AccessArticle
Psychosocial Determinants Among Hospital and Primary Healthcare Professionals Towards Cancer and Cancer Patients in Croatia
by
Darko Kotromanovic, Ivana Kotromanovic Simic, Nika Lovrincevic Pavlovic, Marija Olujic, Sebastijan Spajic, Luka Peric, Tara Cvijic Peric, Matea Matic Licanin, Ilijan Tomas and Ivan Miskulin
J. Clin. Med. 2026, 15(7), 2804; https://doi.org/10.3390/jcm15072804 - 7 Apr 2026
Abstract
Background/Objectives: Cancer places emotional and psychosocial demands on healthcare professionals; therefore, this study aimed to examine sociodemographic and psychosocial determinants, including emotional competence, empathy, and stigma, and to assess their interrelationships with mental health, attitudes towards cancer, and cancer-related stigma among healthcare professionals
[...] Read more.
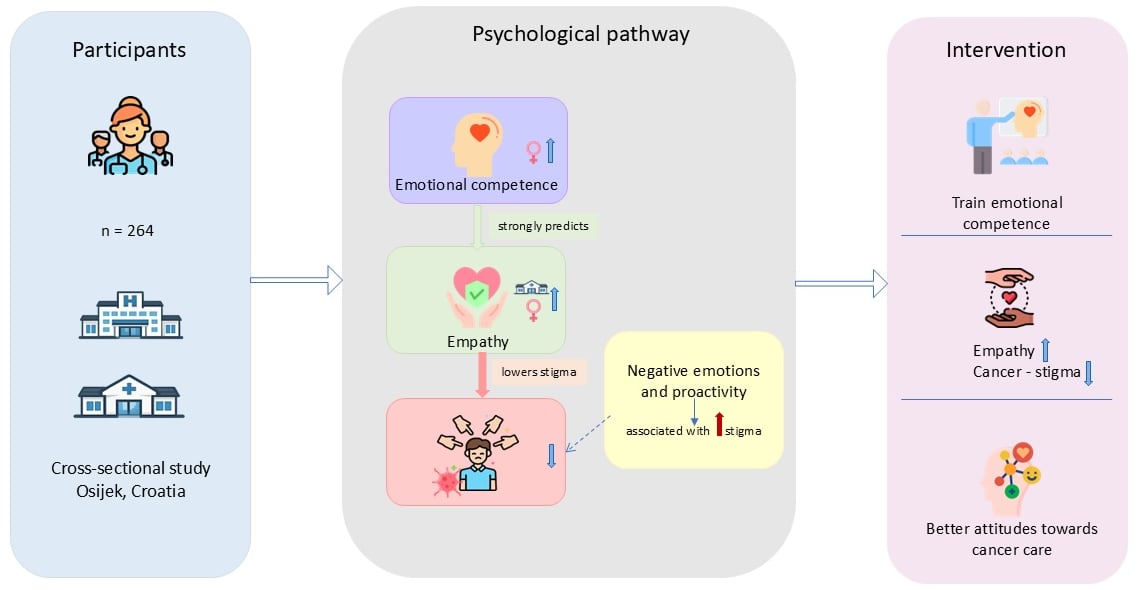
Background/Objectives: Cancer places emotional and psychosocial demands on healthcare professionals; therefore, this study aimed to examine sociodemographic and psychosocial determinants, including emotional competence, empathy, and stigma, and to assess their interrelationships with mental health, attitudes towards cancer, and cancer-related stigma among healthcare professionals involved in cancer care. Methods: This cross-sectional study was conducted from July 2025 to January 2026 via a self-administered questionnaire among 264 hospital and primary care healthcare professionals in Osijek, Croatia (69 men and 195 women; median age 37 years, IQR 31–47, age range 20–64 years), all directly involved in providing healthcare to cancer patients in Croatia. Results: Significant differences were observed by gender, age, occupation, and workplace. Men were more frequently physicians and had higher education levels and socioeconomic status, whereas women achieved higher scores in emotional competence and empathy. Physicians more often had shorter overall work experience and reported greater perceived controllability of cancer. Age-related differences were found in perceived discrimination, stigma, and controllability of cancer. Primary healthcare professionals showed a higher level of empathy and proactivity and a lower perception of cancer as an incurable disease. Higher empathy was associated with lower stigma, while negative emotions and greater proactivity were associated with higher stigma, and emotional competence was a strong predictor of empathy. Conclusions: The study identified notable sociodemographic and psychosocial differences among healthcare professionals. Emotional competence strongly predicted empathy, which was inversely associated with cancer-related stigma, suggesting potential targets for interventions to improve attitudes towards cancer care. Furthermore, women exhibited significantly higher emotional competence and empathy than men, highlighting the importance of incorporating gender-specific perspectives into developing educational and support strategies for cancer healthcare professionals.
Full article
(This article belongs to the Section Oncology)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Evaluation of Latent Tuberculosis Infection Risk in Liver Transplant Recipients
by
Miraç Öz Kahya, Serhat Erol, Dilara Kış Gökçecik, Elvan Onur Kırımker, Güle Çınar, Akın Fırat Kocaay, Deniz Balcı and Özlem Özdemir Kumbasar
J. Clin. Med. 2026, 15(7), 2803; https://doi.org/10.3390/jcm15072803 - 7 Apr 2026
Abstract
Background/Objectives: Tuberculosis remains one of the preventable causes of mortality among liver transplant recipients. The prevalence of tuberculosis in solid organ transplant recipients is higher than in the general population. The aim of this study was to evaluate the incidence of latent tuberculosis
[...] Read more.
Background/Objectives: Tuberculosis remains one of the preventable causes of mortality among liver transplant recipients. The prevalence of tuberculosis in solid organ transplant recipients is higher than in the general population. The aim of this study was to evaluate the incidence of latent tuberculosis infection (LTBI) and active tuberculosis after liver transplantation. Methods: This is a retrospective, single-center, case–control study. Adult liver transplant candidates who were evaluated between 1 January 2016 and 31 December 2022 were retrospectively assessed. Patients with pre-transplant tuberculin skin test (TST) and/or interferon-gamma release assay (IGRA) results who underwent transplantation were included in this study. Results: A total of 111 liver transplant recipients with available IGRA and/or TST results were included; 70 were men (63.1%) and 41 were women (36.9%), with a mean age of 53.5 ± 11.3 years. Demographic, clinical, and laboratory characteristics were evaluated. The most common indication for liver transplantation was viral hepatitis (33.3%), followed by cryptogenic cirrhosis (19.8%) and hepatocellular carcinoma (10.8%). All patients had a Bacillus Calmette–Guérin (BCG) vaccination scar. Ten patients received grafts from deceased donors, while 101 underwent living-donor liver transplantation. No patient received LTBI treatment before transplantation, whereas LTBI treatment was initiated in four patients after transplantation. None of the patients had a diagnosis of active tuberculosis prior to transplantation. Thoracic computed tomography revealed findings compatible with tuberculosis sequelae in 11 patients (9.9%). During a median follow-up period of 49 [27–64] months after transplantation, no cases of active tuberculosis were observed among patients with positive TST and/or IGRA results. Patients were divided into two groups according to their TST and IGRA results. Group 1 consisted of patients with IGRA positivity and/or a TST ≥5 mm, while Group 2 included patients with a TST <5 mm and negative IGRA results. The only statistically significant difference between the groups was the administration of LTBI treatment (p = 0.027); four patients in Group 1 received LTBI therapy. None of these patients were able to continue prophylaxis due to treatment-related adverse effects. Conclusions: Prophylaxis with hepatotoxic agents poses a substantial risk in liver transplant candidates. Since the hepatotoxicity may cause early cessation of LTBI treatment, the risk–benefit ratio of post-transplant LTBI therapy should be carefully assessed. In situations where LTBI treatment is deferred, close clinical monitoring is strongly recommended.
Full article
(This article belongs to the Section Respiratory Medicine)
Open AccessArticle
The Influence of Frailty on Total Hip Arthroplasty Outcomes: A Propensity-Matched Study of 90,660 Patients Using the Modified Frailty Index
by
Sri Tummala, Mehul M. Mittal, Hetsinhji Chavda, Tarun R. Sontam, Senthil N. Sambandam and Dane K. Wukich
J. Clin. Med. 2026, 15(7), 2802; https://doi.org/10.3390/jcm15072802 - 7 Apr 2026
Abstract
Background: Frailty is a key predictor of adverse surgical outcomes in older adults. However, the prognostic utility of the 5-factor modified frailty index (mFI-5) for short- and long-term outcomes following total hip arthroplasty (THA) remains inadequately defined. This study assessed the association
[...] Read more.
Background: Frailty is a key predictor of adverse surgical outcomes in older adults. However, the prognostic utility of the 5-factor modified frailty index (mFI-5) for short- and long-term outcomes following total hip arthroplasty (THA) remains inadequately defined. This study assessed the association between frailty severity, measured by the mFI-5, and postoperative complications, implant survivorship, and mortality following primary THA in a large national cohort. Methods: This retrospective cohort study included 90,660 patients aged ≥50 years undergoing primary THA for osteoarthritis from 2003 to 2020 using the TriNetX research network. Patients were stratified by frailty severity based on mFI-5 scores: non-frail (0–1), moderately frail (2), and severely frail (≥3). Cases of fractures, polytrauma, or falls were excluded. Pairwise propensity score matching was adjusted for age, sex, race, and BMI. Outcomes included 90-day medical and surgical complications, healthcare utilization, and 2- and 5-year THA revision and mortality rates. Risk ratios (RRs) with 95% confidence intervals (CIs) and Bonferroni-corrected significance thresholds (p < 0.0167) were reported. Results: Severely frail patients had significantly increased risks of 90-day mortality (RR 4.41, 95% CI 2.22–8.74), acute kidney injury (RR 2.92), myocardial infarction (RR 3.61), and periprosthetic joint infection (RR 2.02) compared to non-frail patients. At five years, severely frail patients demonstrated a 58% higher revision risk (RR 1.58) and 23.0% mortality versus 6.9% in the non-frail cohort. A dose-dependent risk gradient was observed, with moderately frail patients exhibiting intermediate risks across all outcomes. Conclusions: Frailty severity, as measured by the mFI-5, was associated with a stepwise increase in short- and long-term complications and mortality following THA. The mFI-5 may serve as a practical, scalable tool for preoperative risk stratification, counseling, and resource planning in older adults undergoing primary THA.
Full article
(This article belongs to the Special Issue New Advances in Hip and Knee Reconstructive Surgery: 2nd Edition)

Journal Menu
► ▼ Journal Menu-
- JCM Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Society Collaborations
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Applied Sciences, Children, Dentistry Journal, JCM
Preventive Dentistry and Public Health
Topic Editors: Denis Bourgeois, Elena BardelliniDeadline: 30 April 2026
Topic in
Biology, JCM, Diagnostics, Dentistry Journal
Assessment of Craniofacial Morphology: Traditional Methods and Innovative Approaches
Topic Editors: Nikolaos Gkantidis, Carlalberta VernaDeadline: 1 June 2026
Topic in
Cells, JCM, Organoids, JMP
Novel Discoveries in Oncology 2nd Edition
Topic Editors: Michela Campolo, Giovanna Casili, Alessia Filippone, Marika LanzaDeadline: 20 June 2026
Topic in
Biomedicines, IJMS, JCM, Medicina, Neurology International
Advances in Exercise-Induced Neurogenesis, Neuronal and Functional Adaptations in Neurorehabilitation
Topic Editors: Carlos Bernal-Utrera, Cleofas Rodriguez-Blanco, Maria Livia Carrascal MorenoDeadline: 29 June 2026

Conferences
Special Issues
Special Issue in
JCM
Neurosurgery and Spine Surgery: From Up-to-Date Practitioners, 2nd Edition
Guest Editor: Massimiliano VisocchiDeadline: 10 April 2026
Special Issue in
JCM
Advances in Diagnosis and Treatment for Thymic Pathology
Guest Editor: Charalambos ZisisDeadline: 10 April 2026
Special Issue in
JCM
Clinical Management of Patients with Heart Failure: 3rd Edition
Guest Editor: Cristina TudoranDeadline: 10 April 2026
Special Issue in
JCM
Oral and Maxillofacial Surgery: Recent Clinical Advances and Future Directions
Guest Editors: Funda Göker, Gianluca M. Tartaglia, Massimo Del FabbroDeadline: 10 April 2026
Topical Collections
Topical Collection in
JCM
Pediatric and Adolescent Gynecology
Collection Editor: Panagiotis Christopoulos